Клинический разбор в общей медицине №3 2023
Sechenov First Moscow State Medical University (Sechenov University), Moscow, Russia
dvoretski@mail.ru
Abstract
The paper reports the major clinical situations associated with thrombocytopenia in pregnancy. The diagnostic criteria of the most frequent disorders associated with thrombocytopenia that occur during gestation are provided. The issues related to differential diagnosis of thrombocytopenia in pregnancy are discussed.
Key words: pregnancy, thrombocytopenia, thrombotic microangiopathies, gestational thrombocytopenia, immune thrombocytopenia.
For citation: Dvoretsky L.I. Pregnant woman suffered from thrombocytopenia. Clinical review for general practice. 2023; 4 (3): 15–21.
DOI: 10.47407/kr2023.4.3.00217
 Одним из нарушений лабораторных показателей во время беременности является тромбоцитопения, определяемая при снижении количества тромбоцитов в периферической крови ниже 150×109/л [1]. Тромбоцитопения является вторым по частоте гематологическим синдромом (после анемии) при беременности и регистрируется у 7–15% беременных, причем у 1% из них количество тромбоцитов оказывается ниже 100×109/л [2, 3].
Одним из нарушений лабораторных показателей во время беременности является тромбоцитопения, определяемая при снижении количества тромбоцитов в периферической крови ниже 150×109/л [1]. Тромбоцитопения является вторым по частоте гематологическим синдромом (после анемии) при беременности и регистрируется у 7–15% беременных, причем у 1% из них количество тромбоцитов оказывается ниже 100×109/л [2, 3].
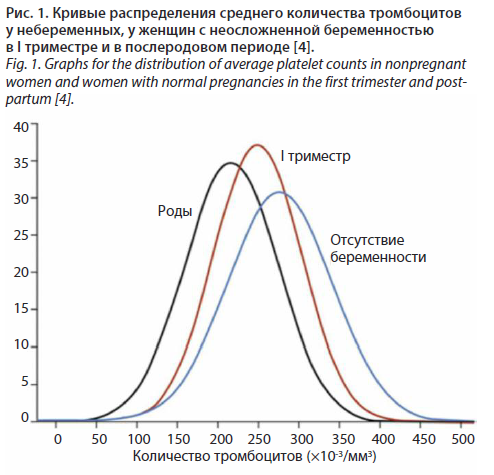
У беременных количество тромбоцитов претерпевает определенную динамику в зависимости от сроков беременности (рис. 1).
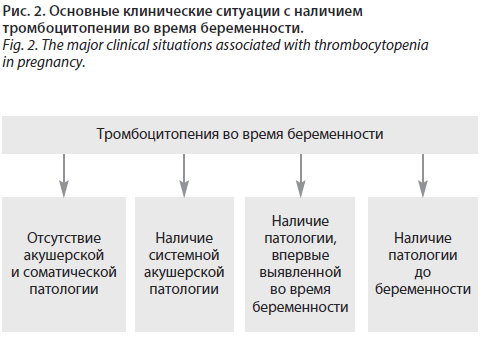
Каждый из указанных патогенетических вариантов тромбоцитопении включает определенный круг заболеваний и патологических процессов с различными причинами, клиническими проявлениями, прогнозом и методами лечения. В ряде случаев возможны комбинации механизмов развития тромбоцитопении. В акушерской практике встречаются следующие ситуации с наличием тромбоцитопении у беременных:
• тромбоцитопения при отсутствии акушерской и соматической патологии;
• тромбоцитопения при наличии системной акушерской патологии;
• тромбоцитопения как проявление патологии, впервые манифестировавшей во время беременности;
• тромбоцитопения как проявление имеющейся до беременности соматической патологии.
Диагностический поиск при тромбоцитопении у беременных должен осуществляться с учетом клинической ситуации (наличие акушерской патологии, сопутствующих заболеваний, сопровождающихся тромбоцитопенией, прием лекарственных препаратов и др.); рис. 2.
 У беременных с нормально протекающей беременностью, не отягощенных заболеваниями с наличием тромбоцитопении, может наблюдаться умеренное снижение количества тромбоцитов начиная с I триместра с дальнейшим снижением вплоть до родов [4, 5]. Данный лабораторный феномен обозначается как гестационная тромбоцитопения (ГТП). Она регистрируется у 5–10% беременных [6] и составляет около 70% всех тромбоцитопений у беременных [7]. Причинами снижения количества тромбоцитов при ГТП являются: гормональный дисбаланс, дефицит фолатов и витамина В12, ускоренный клиренс тромбоцитов, секвестрация тромбоцитов в плаценте, гемодилюция из-за увеличения объема циркулирующей крови, повышенная агрегация тромбоцитов во время беременности вследствие увеличения содержания тромбоксана А2, а также комбинация указанных факторов [8]. В большинстве случаев число тромбоцитов редко снижается ниже 100×109/л. Лишь у 1% беременных с ГТП регистрируется тромбоцитопения ≤100×109/л, в том числе у 0,1% количество тромбоцитов ниже 80×109/л [4]. В связи с этим более глубокая тромбоцитопения у беременных требует исключения другой природы данной цитопении, в частности иммунной тромбоцитопении (ИТП). В ряде случаев дифференциальный диагноз между ИТП и ГТП возможен лишь после родоразрешения [9]. Основными признаками, позволяющими заподозрить ГТП, считаются отсутствие тромбоцитопении у женщины до беременности, снижение количества тромбоцитов во время предыдущих беременностей с нормализацией после родов, отсутствие геморрагического синдрома и негативного влияния на течение беременности, спонтанная нормализация количества тромбоцитов через 1–2 мес после родов, отсутствие тромбоцитопении у новорожденного. При стабильном уровне тромбоцитов и отсутствии дальнейшего снижения их количества специального обследования и лечения, досрочного родоразрешения не требуется [10].
У беременных с нормально протекающей беременностью, не отягощенных заболеваниями с наличием тромбоцитопении, может наблюдаться умеренное снижение количества тромбоцитов начиная с I триместра с дальнейшим снижением вплоть до родов [4, 5]. Данный лабораторный феномен обозначается как гестационная тромбоцитопения (ГТП). Она регистрируется у 5–10% беременных [6] и составляет около 70% всех тромбоцитопений у беременных [7]. Причинами снижения количества тромбоцитов при ГТП являются: гормональный дисбаланс, дефицит фолатов и витамина В12, ускоренный клиренс тромбоцитов, секвестрация тромбоцитов в плаценте, гемодилюция из-за увеличения объема циркулирующей крови, повышенная агрегация тромбоцитов во время беременности вследствие увеличения содержания тромбоксана А2, а также комбинация указанных факторов [8]. В большинстве случаев число тромбоцитов редко снижается ниже 100×109/л. Лишь у 1% беременных с ГТП регистрируется тромбоцитопения ≤100×109/л, в том числе у 0,1% количество тромбоцитов ниже 80×109/л [4]. В связи с этим более глубокая тромбоцитопения у беременных требует исключения другой природы данной цитопении, в частности иммунной тромбоцитопении (ИТП). В ряде случаев дифференциальный диагноз между ИТП и ГТП возможен лишь после родоразрешения [9]. Основными признаками, позволяющими заподозрить ГТП, считаются отсутствие тромбоцитопении у женщины до беременности, снижение количества тромбоцитов во время предыдущих беременностей с нормализацией после родов, отсутствие геморрагического синдрома и негативного влияния на течение беременности, спонтанная нормализация количества тромбоцитов через 1–2 мес после родов, отсутствие тромбоцитопении у новорожденного. При стабильном уровне тромбоцитов и отсутствии дальнейшего снижения их количества специального обследования и лечения, досрочного родоразрешения не требуется [10].
В некоторых случаях HELLP-синдром развивается при тяжелой преэклампсии или эклампсии с частотой до 24% [17]. Повышение активности аланин- и аспартатаминотрансферазы может предшествовать снижению числа тромбоцитов. Максимальное снижение количества тромбоцитов наблюдается через сутки после родов с нормализацией через 6–11 дней. В 10–30% случаев HELLP-синдром манифестируется только в послеродовом периоде, в течение 72 ч после родов [18]. Тромбоцитопения у новорожденных при HELLP-синдроме не отмечается.
HELLP-синдром следует заподозрить при развитии у беременных с проявлениями преэклампсии прогрессирующей тромбоцитопении, признаков гемолиза (ретикулоцитоз, повышение активности лактатдегидрогеназы) и повышенной активности трансаминаз [6]. Умеренное повышение активности трансаминаз может наблюдаться при преэклампсии, однако высокие показатели более характерны для наличия HELLP-синдрома [19].
Клиническая симптоматика ТТП обусловлена распространенной агрегацией тромбоцитов в микроциркуляторном русле, микротромбозами и развитием органной недостаточности (почки, печень, головной мозг). Классическая пентада ТТП, включающая гемолитическую анемию, выраженную тромбоцитопению (нередко до 30×109/л и ниже), неврологическую симптоматику, лихорадку и почечную недостаточность, наблюдается менее чем в 40% случаев [25]. Диагноз ТТП может быть заподозрен при сочетании Кумбс-негативной гемолитической анемии (отсутствие неполных антиэритроцитарных иммуноглобулин – IgG-антител) с тромбоцитопенией, не связанной с другими причинами.
Дифференциальная диагностика между ТТП и НЕLLР-синдромом имеет практическое значение в связи с тактикой ведения беременных. Так, при НЕLLР-синдроме, диагностированном после 34-й недели беременности, показано срочное родоразрешение, в то время как при острой форме ТТП рекомендуется плазмаферез (плазмообмен) в первые 4–8 ч клинико-лабораторной манифестации, что значительно снижает материнскую смертность – с 90 до 10–20% [26]. В отличие от НЕLLР-синдрома, для ТТП характерны: более выраженные гемолиз и тромбоцитопения, наличие лихорадки, незначительное повышение активности трансаминаз или нормальные показатели, нормальные показатели протромбинового времени и активированного частичного тромбопластинового времени, персистенция симптомов на протяжении более 72 ч после родов [27].
Дифференцировать ТТП от HELLP-сидрома у беременных при наличии гематурии и тромбоцитопении помогает высокое соотношение (>20) показателей лактатдегидрогеназы/аспартатаминотрансферазы [28]. Диагноз ТТП подтверждается наличием выраженного дефицита активности ADAMTS 13 (<5%) [26].
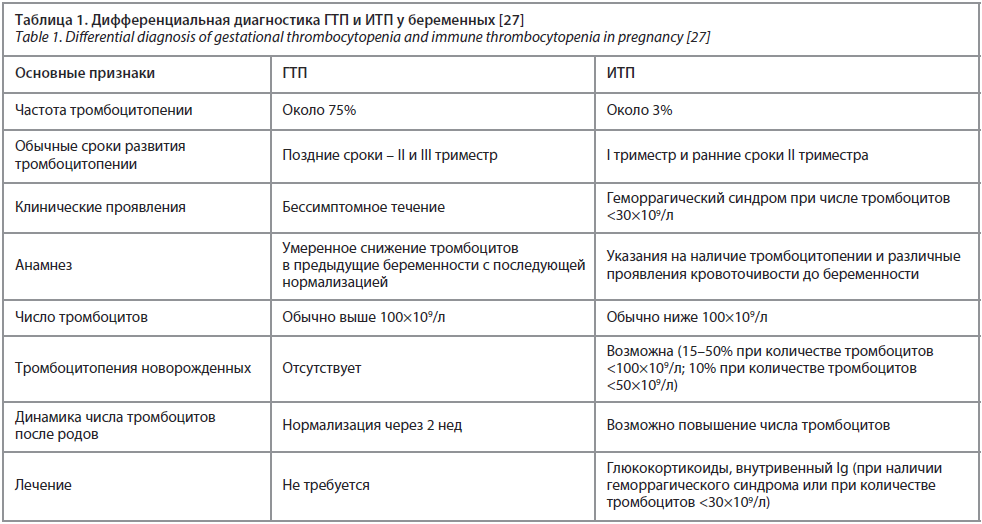
При дифференциальной диагностике ГТП и ИТП в ранние сроки беременности с количеством тромбоцитов 100×109/л и продолжающимся снижением показателей тромбоцитов по мере дальнейшего развития беременности в отсутствие указаний на ИТП до беременности более вероятным следует считать наличие у беременной ИТП. Еще более затруднительна трактовка природы тромбоцитопении в III триместре беременности, когда количество тромбоцитов колеблется между 50×109/л и 70×109/л. И хотя уточнение природы тромбоцитопении в эти сроки не может существенно изменить тактику ведения беременной, следует иметь в виду риск развития неонатальной тромбоцитопении в случае наличия у матери ИТП. При падении числа тромбоцитов ниже 50×109/л и отсутствии акушерских осложнений (преэклампсия, НЕLLР-синдром) наиболее вероятным диагнозом следует считать ИТП.
В табл. 1 представлена дифференциальная диагностика ГТП и ИТП.
β2-гликопротеину 1, волчаночный антикоагулянт), вступающих во взаимодействие с фосфолипидами или фосфолипидсвязывающими сывороточными белками. Антифосфолипидные антитела не только представляют собой серологический маркер АФС, но и обладают способностью активировать тромбоциты и нейтрофилы, что приводит к развитию тромботических осложнений [36].
Основным лабораторным признаком, заставляющим заподозрить наличие АФС, является снижение количества тромбоцитов, которое обычно колеблется от 70 до 100×109/л и не требует специального лечения. Развитие геморрагических осложнений наблюдается редко и, как правило, связано с сопутствующим нарушением в других звеньях гемостаза (плазменное звено), патологией почек или передозировкой антикоагулянтов (в случаях антикоагулянтной терапии). Клинические проявления АФС весьма разнообразны и включают патологию со стороны сердечно-сосудистой системы (тромбозы глубоких вен, рецидивирующие тромбоэмболии легочной артерии, инфаркт миокарда, внутрисердечные тромбы, клапанные поражения), поражения центральной нервной системы (острое нарушение мозгового кровообращения, транзиторные ишемические атаки), кожи (сетчатое ливедо, посттромбофлебитические язвы, гангрены пальцев рук и ног), печени (тромбозы печеночных вен). Типичными проявлениями АФС у женщин является акушерская патология, частота которой в качестве причины АФС достигает 80%.
Клинические критерии АФС [37]:
1. Сосудистые тромбозы (один и более эпизодов тромбоза, подтвержденного инструментальными методами или морфологически с отсутствием значительного воспаления сосудистой стенки).
2. Патология беременности в виде одного из трех вариантов:
• один и более случаев внутриутробной гибели морфологически нормального плода после 10 нед беременности;
• один и более эпизодов преждевременных родов морфологически нормального плода до 34 нед беременности из-за выраженной преэклампсии, или эклампсии, или выраженной плацентарной недостаточности;
• три и более последовательных случаев спонтанных абортов до 10 нед беременности (при исключении анатомических дефектов матки, гормональных нарушений, материнских и отцовских хромосомных нарушений).
Лабораторные критерии АФС:
• наличие антител к кардиолипину класса IgG или IgM в средних и высоких титрах, определенных по крайней мере дважды с интервалом не менее 12 нед;
• наличие антител к β2-гликопротеину 1, IgG и/или IgM изотип, в средних или высоких титрах по крайней мере 2 раза с интервалом 12 нед;
• наличие волчаночного антикоагулянта в плазме в двух или более исследованиях с промежутком не менее 12 нед.
Диагноз АФС считается достоверным при сочетании по крайней мере одного клинического и одного лабораторного признака. АФС исключается, если менее 12 нед или более 5 лет выявляются антифосфолипидные антитела без клинических проявлений или клинические проявления без антифосфолипидных антител.
При анализе 48 больных с СКВ, впервые диагностированной во время беременности (I и II триместры) или после родов, наиболее частыми проявлениями были тромбоцитопении и люпус-нефрит (25% и 68% соответственно). В то же время системные проявления СКВ (лихорадка, суставной синдром, алопеция, оральные язвы, гипокомплементемия) встречались значительно реже по сравнению с больными СКВ в отсутствие беременности [42]. По данным китайского исследования, включавшего 216 беременных с наличием СКВ, у 30% заболевание было впервые диагностировано во время беременности (I и II триместры) или после родов. Впервые диагностированная СКВ характеризовалась наличием тромбоцитопении и анемии, более выраженными по сравнению с беременными, ранее страдавшими СКВ [43].
Конфликт интересов. Автор заявляет об отсутствии конфликта интересов.
Сonflict of interests. The author declares that there is not conflict of interests.
Информация об авторе / Information about the author
Дворецкий Леонид Иванович – д-р мед. наук, проф. каф. госпитальной терапии №2 ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: dvoretski@mail.ru; ORCID: 0000-0003-3186-0102
Leonid I. Dvoretsky – D. Sci. (Med.), Prof., Sechenov First Moscow State Medical University (Sechenov University).
E-mail: dvoretski@mail.ru; ORCID: 0000-0003-3186-0102
Поступила в редакцию / Received: 07.03.2023
Поступила после рецензирования / Revised: 19.03.2023
Принята к публикации / Accepted: 30.03.2023
Клинический разбор в общей медицине №3 2023
У беременной тромбоцитопения
Номера страниц в выпуске:15-21
Аннотация
В статье представлены основные клинические ситуации с наличием тромбоцитопении у беременных. Приводятся диагностические критерии наиболее частых заболеваний с наличием тромбоцитопении, возникающих в гестационном периоде. Обсуждаются вопросы дифференциальной диагностики тромбоцитопений у беременных.
Ключевые слова: беременность, тромбоцитопения, тромботические микроангиопатии, гестационная тромбоцитопения, иммунная тромбоцитопения.
Для цитирования: Дворецкий Л.И. У беременной тромбоцитопения. Клинический разбор в общей медицине. 2023; 4 (3): 15–21.
DOI: 10.47407/kr2023.4.3.00217
В статье представлены основные клинические ситуации с наличием тромбоцитопении у беременных. Приводятся диагностические критерии наиболее частых заболеваний с наличием тромбоцитопении, возникающих в гестационном периоде. Обсуждаются вопросы дифференциальной диагностики тромбоцитопений у беременных.
Ключевые слова: беременность, тромбоцитопения, тромботические микроангиопатии, гестационная тромбоцитопения, иммунная тромбоцитопения.
Для цитирования: Дворецкий Л.И. У беременной тромбоцитопения. Клинический разбор в общей медицине. 2023; 4 (3): 15–21.
DOI: 10.47407/kr2023.4.3.00217
Pregnant woman suffered from thrombocytopenia
Leonid I. DvoretskySechenov First Moscow State Medical University (Sechenov University), Moscow, Russia
dvoretski@mail.ru
Abstract
The paper reports the major clinical situations associated with thrombocytopenia in pregnancy. The diagnostic criteria of the most frequent disorders associated with thrombocytopenia that occur during gestation are provided. The issues related to differential diagnosis of thrombocytopenia in pregnancy are discussed.
Key words: pregnancy, thrombocytopenia, thrombotic microangiopathies, gestational thrombocytopenia, immune thrombocytopenia.
For citation: Dvoretsky L.I. Pregnant woman suffered from thrombocytopenia. Clinical review for general practice. 2023; 4 (3): 15–21.
DOI: 10.47407/kr2023.4.3.00217
 Одним из нарушений лабораторных показателей во время беременности является тромбоцитопения, определяемая при снижении количества тромбоцитов в периферической крови ниже 150×109/л [1]. Тромбоцитопения является вторым по частоте гематологическим синдромом (после анемии) при беременности и регистрируется у 7–15% беременных, причем у 1% из них количество тромбоцитов оказывается ниже 100×109/л [2, 3].
Одним из нарушений лабораторных показателей во время беременности является тромбоцитопения, определяемая при снижении количества тромбоцитов в периферической крови ниже 150×109/л [1]. Тромбоцитопения является вторым по частоте гематологическим синдромом (после анемии) при беременности и регистрируется у 7–15% беременных, причем у 1% из них количество тромбоцитов оказывается ниже 100×109/л [2, 3].У беременных количество тромбоцитов претерпевает определенную динамику в зависимости от сроков беременности (рис. 1).
Каждый из указанных патогенетических вариантов тромбоцитопении включает определенный круг заболеваний и патологических процессов с различными причинами, клиническими проявлениями, прогнозом и методами лечения. В ряде случаев возможны комбинации механизмов развития тромбоцитопении. В акушерской практике встречаются следующие ситуации с наличием тромбоцитопении у беременных:
• тромбоцитопения при отсутствии акушерской и соматической патологии;
• тромбоцитопения при наличии системной акушерской патологии;
• тромбоцитопения как проявление патологии, впервые манифестировавшей во время беременности;
• тромбоцитопения как проявление имеющейся до беременности соматической патологии.
Диагностический поиск при тромбоцитопении у беременных должен осуществляться с учетом клинической ситуации (наличие акушерской патологии, сопутствующих заболеваний, сопровождающихся тромбоцитопенией, прием лекарственных препаратов и др.); рис. 2.
Тромбоцитопения при отсутствии акушерской и соматической патологии
 У беременных с нормально протекающей беременностью, не отягощенных заболеваниями с наличием тромбоцитопении, может наблюдаться умеренное снижение количества тромбоцитов начиная с I триместра с дальнейшим снижением вплоть до родов [4, 5]. Данный лабораторный феномен обозначается как гестационная тромбоцитопения (ГТП). Она регистрируется у 5–10% беременных [6] и составляет около 70% всех тромбоцитопений у беременных [7]. Причинами снижения количества тромбоцитов при ГТП являются: гормональный дисбаланс, дефицит фолатов и витамина В12, ускоренный клиренс тромбоцитов, секвестрация тромбоцитов в плаценте, гемодилюция из-за увеличения объема циркулирующей крови, повышенная агрегация тромбоцитов во время беременности вследствие увеличения содержания тромбоксана А2, а также комбинация указанных факторов [8]. В большинстве случаев число тромбоцитов редко снижается ниже 100×109/л. Лишь у 1% беременных с ГТП регистрируется тромбоцитопения ≤100×109/л, в том числе у 0,1% количество тромбоцитов ниже 80×109/л [4]. В связи с этим более глубокая тромбоцитопения у беременных требует исключения другой природы данной цитопении, в частности иммунной тромбоцитопении (ИТП). В ряде случаев дифференциальный диагноз между ИТП и ГТП возможен лишь после родоразрешения [9]. Основными признаками, позволяющими заподозрить ГТП, считаются отсутствие тромбоцитопении у женщины до беременности, снижение количества тромбоцитов во время предыдущих беременностей с нормализацией после родов, отсутствие геморрагического синдрома и негативного влияния на течение беременности, спонтанная нормализация количества тромбоцитов через 1–2 мес после родов, отсутствие тромбоцитопении у новорожденного. При стабильном уровне тромбоцитов и отсутствии дальнейшего снижения их количества специального обследования и лечения, досрочного родоразрешения не требуется [10].
У беременных с нормально протекающей беременностью, не отягощенных заболеваниями с наличием тромбоцитопении, может наблюдаться умеренное снижение количества тромбоцитов начиная с I триместра с дальнейшим снижением вплоть до родов [4, 5]. Данный лабораторный феномен обозначается как гестационная тромбоцитопения (ГТП). Она регистрируется у 5–10% беременных [6] и составляет около 70% всех тромбоцитопений у беременных [7]. Причинами снижения количества тромбоцитов при ГТП являются: гормональный дисбаланс, дефицит фолатов и витамина В12, ускоренный клиренс тромбоцитов, секвестрация тромбоцитов в плаценте, гемодилюция из-за увеличения объема циркулирующей крови, повышенная агрегация тромбоцитов во время беременности вследствие увеличения содержания тромбоксана А2, а также комбинация указанных факторов [8]. В большинстве случаев число тромбоцитов редко снижается ниже 100×109/л. Лишь у 1% беременных с ГТП регистрируется тромбоцитопения ≤100×109/л, в том числе у 0,1% количество тромбоцитов ниже 80×109/л [4]. В связи с этим более глубокая тромбоцитопения у беременных требует исключения другой природы данной цитопении, в частности иммунной тромбоцитопении (ИТП). В ряде случаев дифференциальный диагноз между ИТП и ГТП возможен лишь после родоразрешения [9]. Основными признаками, позволяющими заподозрить ГТП, считаются отсутствие тромбоцитопении у женщины до беременности, снижение количества тромбоцитов во время предыдущих беременностей с нормализацией после родов, отсутствие геморрагического синдрома и негативного влияния на течение беременности, спонтанная нормализация количества тромбоцитов через 1–2 мес после родов, отсутствие тромбоцитопении у новорожденного. При стабильном уровне тромбоцитов и отсутствии дальнейшего снижения их количества специального обследования и лечения, досрочного родоразрешения не требуется [10].Тромбоцитопения при наличии системной акушерской патологии
Преэклампсия
Патогенез преэклампсии принято объяснять нарушением плацентарного ангиогенеза и эндотелиальной дисфункцией с последующим развитием органных нарушений, включая тромбоцитопении [11]. Основным проявлением преэклампсии являются впервые выявленное повышение систолического (≥140 мм рт. ст.) или диастолического (≥90 мм рт. ст.) артериального давления и протеинурия после 20-й недели беременности независимо от наличия или отсутствия других органных нарушений [12]. В 15–20% случаев тромбоцитопения беременных является одним из лабораторных признаков преэклампсии различной тяжести [13, 14]. Количество тромбоцитов у беременных с преэклампсией составляет обычно не менее 100×109/л, а показатели тромбоцитов ниже 100×109/л являются одним из критериев тяжелой преэклампсии [15].НELLP-синдром
НЕLLP-синдром – аббревиатура лабораторной триады, включающей гемолиз (H – hemolys), повышение активности трансаминаз (ЕL – elevate liver transaminase) и снижение количества тромбоцитов (LP – low platelets). Этот синдром отражает цитокинопосредованную эндотелиальную дисфункцию, ведущую к активации свертывающей системы, развитию синдрома диссеминированного внутрисосудистого свертывания (ДВС-синдрома), повышенному потреблению плазменных факторов свертывания и тромбоцитов (тромбоцитопении потребления). Количество тромбоцитов обычно ниже 100×109/л, причем выраженность тромбоцитопении коррелирует с тяжестью акушерской патологии и перинатальной смертностью. Так, если при количестве тромбоцитов в интервале 100–150×109/л акушерская патология и перинатальная смертность регистрируются в 40% и 11,7%, то при более выраженной тромбоцитопении (50–100×109/л) указанные события возрастают до 54% и 14,4%, а при количестве тромбоцитов ниже 50×109/л достигают 64% и 16,4% соответственно [16].В некоторых случаях HELLP-синдром развивается при тяжелой преэклампсии или эклампсии с частотой до 24% [17]. Повышение активности аланин- и аспартатаминотрансферазы может предшествовать снижению числа тромбоцитов. Максимальное снижение количества тромбоцитов наблюдается через сутки после родов с нормализацией через 6–11 дней. В 10–30% случаев HELLP-синдром манифестируется только в послеродовом периоде, в течение 72 ч после родов [18]. Тромбоцитопения у новорожденных при HELLP-синдроме не отмечается.
HELLP-синдром следует заподозрить при развитии у беременных с проявлениями преэклампсии прогрессирующей тромбоцитопении, признаков гемолиза (ретикулоцитоз, повышение активности лактатдегидрогеназы) и повышенной активности трансаминаз [6]. Умеренное повышение активности трансаминаз может наблюдаться при преэклампсии, однако высокие показатели более характерны для наличия HELLP-синдрома [19].
Острая жировая печень беременных
В редких случаях наличие тромбоцитопении у беременных может быть проявлением острой жировой печени беременных (ОЖПБ) – тяжелого осложнения в III триместре с частотой 1 на 7–20 тыс. беременных [20]. В патогенезе развития ОЖПБ придается значение митохондриальной дисфункции, нарушению метаболизма жирных кислот, повышенному уровню эстрогенов у беременных [21]. Клинические проявления ОЖПБ включают неспецифические симптомы (боли в животе, тошнота, рвота, анорексия) в сочетании с изменениями лабораторных показателей (тромбоцитопении, гипогликемия, гиперурикемия, высокая активность трансаминаз и уровня креатинина). Количество тромбоцитов при ОЖПБ может быть значительно снижено (до 20×109/л) и обычно нормализуется через 3–4 сут после родов, достигая 100×109/л на 6-й день [13]. Гипогликемия и коагулопатия при тяжелых формах позволяют отличить ОЖПБ от других микроангиопатий.ДВС-синдром
Тромбоцитопения у беременных может быть одним из лабораторных проявлений ДВС-синдрома (тромбоцитопении потребления) в случаях различной акушерской патологии (преждевременная отслойка плаценты, эмболия околоплодными водами, послеродовые септические осложнения). При этом обращает на себя внимание наличие лабораторных признаков ДВС-синдрома (повышенная агрегация тромбоцитов, наличие комплексов фибрин-мономеров, положительный этаноловый тест) [22].Тромбоцитопения при патологии, впервые выявленной во время беременности
В ряде случаев при наступлении беременности впервые манифестируется целая группа заболеваний и синдромов, одним из проявлений которых является тромбоцитопения.Тромботическая тромбоцитопеническая пурпура
Тромботическая тромбоцитопеническая пурпура (ТТП), относящаяся к тромботическим микроангиопатиям (ТМА), была впервые описана Moshkovitz, в связи с чем указанные состояния обозначались как синдром Мошковица. В основе ТТП лежит снижение активности металлопротеиназы ADAMTS 13 (a disintegrin and metalloproteinase with thrombospondin type 1 domains, no. 13), расщепляющей в норме мультимеры фактора Виллебранда, что препятствует спонтанной адгезии и агрегации тромбоцитов, предупреждая тем самым образование микротромбов в микроциркуляторном русле [23]. При недостаточной активности протеазы происходит неконтролируемое формирование микроагрегатов тромбоцитов, блокирующих микроциркуляцию. Выделяют врожденную форму ТТП, являющуюся результатом мутации гена, регулирующего синтез ADAMTS 13, и приобретенную ТТП, связанную с антителами против фермента ADAMTS 13. Полагают, что беременность является триггером острых эпизодов как врожденной, так и приобретенной форм ТТП [24].Клиническая симптоматика ТТП обусловлена распространенной агрегацией тромбоцитов в микроциркуляторном русле, микротромбозами и развитием органной недостаточности (почки, печень, головной мозг). Классическая пентада ТТП, включающая гемолитическую анемию, выраженную тромбоцитопению (нередко до 30×109/л и ниже), неврологическую симптоматику, лихорадку и почечную недостаточность, наблюдается менее чем в 40% случаев [25]. Диагноз ТТП может быть заподозрен при сочетании Кумбс-негативной гемолитической анемии (отсутствие неполных антиэритроцитарных иммуноглобулин – IgG-антител) с тромбоцитопенией, не связанной с другими причинами.
Дифференциальная диагностика между ТТП и НЕLLР-синдромом имеет практическое значение в связи с тактикой ведения беременных. Так, при НЕLLР-синдроме, диагностированном после 34-й недели беременности, показано срочное родоразрешение, в то время как при острой форме ТТП рекомендуется плазмаферез (плазмообмен) в первые 4–8 ч клинико-лабораторной манифестации, что значительно снижает материнскую смертность – с 90 до 10–20% [26]. В отличие от НЕLLР-синдрома, для ТТП характерны: более выраженные гемолиз и тромбоцитопения, наличие лихорадки, незначительное повышение активности трансаминаз или нормальные показатели, нормальные показатели протромбинового времени и активированного частичного тромбопластинового времени, персистенция симптомов на протяжении более 72 ч после родов [27].
Дифференцировать ТТП от HELLP-сидрома у беременных при наличии гематурии и тромбоцитопении помогает высокое соотношение (>20) показателей лактатдегидрогеназы/аспартатаминотрансферазы [28]. Диагноз ТТП подтверждается наличием выраженного дефицита активности ADAMTS 13 (<5%) [26].
Атипичный гемолитико-уремический синдром
Другой редкой причиной тромбоцитопении у беременных является атипичный гемолитико-уремический синдром (аГУС), встречающийся с частотой 1 на 25 тыс. беременных [29]. По современным представлениям, аГУС возникает в результате генетически детерминированной дисрегуляции системы комплемента [30]. Неконтролируемая активация системы комплемента ведет к повреждению эндотелия и развитию ТМА, которая манифестируется главным образом со стороны почек. Существует так называемый типичный ГУС (ранее назывался постдиарейным), связанный с кишечной инфекцией и обозначающийся в настоящее время как STEC-ГУС (Shiga-toxin-продуцирующая Esherihia coli). Основными проявлениями аГУС являются тромбоцитопении, Кумбс-негативная гемолитическая анемия и острое повреждение почек, составляющие классическую триаду. Диагноз аГУС – это диагноз исключения других вариантов ТМА, в частности ТТП и HELLP-синдрома. Выраженный дефицит ADAMTS 13 при ГУС, в отличие от ТТП, отсутствует. Содержание комплемента С3 снижено почти у 1/2 больных аГУС. Дифференциальный диагноз между ТТП, НЕLLР-синдромом и ГУС имеет важное практическое значение, поскольку при ГУС может с эффектом применяться ингибитор активации комплемента экулизумаб или моноклональные антитела к комплементу С5 [31]. В большинстве случаев количество тромбоцитов повышается через 48–72 ч после назначения экулизумаба, в то время как функция почек восстанавливается в более поздние сроки вплоть до нескольких месяцев [32].Первичная иммунная тромбоцитопения
Первичная ИТП, обозначавшаяся ранее идиопатической тромбоцитопенической пурпурой, является аутоиммунным заболеванием, обусловленным выработкой антител к структурам мембраны тромбоцитов с повышенной их деструкцией. ИТП диагностируется у 1–2 на 1 тыс. беременных и составляет около 5% всех тромбоцитопений беременных [33]. Тяжелая ИТП с количеством тромбоцитов менее 50×109/л встречается у 0,83 на 10 тыс. беременных [34]. В отличие от ГТП, в 9–15% случаев ИТП беременных наблюдается неонатальная тромбоцитопении с риском внутримозговых геморрагий у 1–2% новорожденных [35].При дифференциальной диагностике ГТП и ИТП в ранние сроки беременности с количеством тромбоцитов 100×109/л и продолжающимся снижением показателей тромбоцитов по мере дальнейшего развития беременности в отсутствие указаний на ИТП до беременности более вероятным следует считать наличие у беременной ИТП. Еще более затруднительна трактовка природы тромбоцитопении в III триместре беременности, когда количество тромбоцитов колеблется между 50×109/л и 70×109/л. И хотя уточнение природы тромбоцитопении в эти сроки не может существенно изменить тактику ведения беременной, следует иметь в виду риск развития неонатальной тромбоцитопении в случае наличия у матери ИТП. При падении числа тромбоцитов ниже 50×109/л и отсутствии акушерских осложнений (преэклампсия, НЕLLР-синдром) наиболее вероятным диагнозом следует считать ИТП.
В табл. 1 представлена дифференциальная диагностика ГТП и ИТП.

Антифосфолипидный синдром
В основе антифосфолипидного синдрома (АФС), относящегося к приобретенным тромбофилиям, лежит образование антифосфолипидных антител – гетерогенной популяции аутоантител (антитела к кардиолипину иβ2-гликопротеину 1, волчаночный антикоагулянт), вступающих во взаимодействие с фосфолипидами или фосфолипидсвязывающими сывороточными белками. Антифосфолипидные антитела не только представляют собой серологический маркер АФС, но и обладают способностью активировать тромбоциты и нейтрофилы, что приводит к развитию тромботических осложнений [36].
Основным лабораторным признаком, заставляющим заподозрить наличие АФС, является снижение количества тромбоцитов, которое обычно колеблется от 70 до 100×109/л и не требует специального лечения. Развитие геморрагических осложнений наблюдается редко и, как правило, связано с сопутствующим нарушением в других звеньях гемостаза (плазменное звено), патологией почек или передозировкой антикоагулянтов (в случаях антикоагулянтной терапии). Клинические проявления АФС весьма разнообразны и включают патологию со стороны сердечно-сосудистой системы (тромбозы глубоких вен, рецидивирующие тромбоэмболии легочной артерии, инфаркт миокарда, внутрисердечные тромбы, клапанные поражения), поражения центральной нервной системы (острое нарушение мозгового кровообращения, транзиторные ишемические атаки), кожи (сетчатое ливедо, посттромбофлебитические язвы, гангрены пальцев рук и ног), печени (тромбозы печеночных вен). Типичными проявлениями АФС у женщин является акушерская патология, частота которой в качестве причины АФС достигает 80%.
Клинические критерии АФС [37]:
1. Сосудистые тромбозы (один и более эпизодов тромбоза, подтвержденного инструментальными методами или морфологически с отсутствием значительного воспаления сосудистой стенки).
2. Патология беременности в виде одного из трех вариантов:
• один и более случаев внутриутробной гибели морфологически нормального плода после 10 нед беременности;
• один и более эпизодов преждевременных родов морфологически нормального плода до 34 нед беременности из-за выраженной преэклампсии, или эклампсии, или выраженной плацентарной недостаточности;
• три и более последовательных случаев спонтанных абортов до 10 нед беременности (при исключении анатомических дефектов матки, гормональных нарушений, материнских и отцовских хромосомных нарушений).
Лабораторные критерии АФС:
• наличие антител к кардиолипину класса IgG или IgM в средних и высоких титрах, определенных по крайней мере дважды с интервалом не менее 12 нед;
• наличие антител к β2-гликопротеину 1, IgG и/или IgM изотип, в средних или высоких титрах по крайней мере 2 раза с интервалом 12 нед;
• наличие волчаночного антикоагулянта в плазме в двух или более исследованиях с промежутком не менее 12 нед.
Диагноз АФС считается достоверным при сочетании по крайней мере одного клинического и одного лабораторного признака. АФС исключается, если менее 12 нед или более 5 лет выявляются антифосфолипидные антитела без клинических проявлений или клинические проявления без антифосфолипидных антител.
Системная красная волчанка
Гематологические проявления при системной красной волчанке (СКВ) характеризуются различными цитопеническими синдромами (анемия, лейкопения, тромбоцитопения), нередко в сочетании друг с другом. В основе цитопений при СКВ лежит аутоиммунный механизм (аутоиммунная гемолитическая анемия с положительной пробой Кумбса, аутоиммунные лейко- и тромбоцитопения). Одним из критериев СКВ, согласно Американской коллегии ревматологов, является тромбоцитопения, частота которой при СКВ колеблется от 10 до 40% [38]. В процессе диагностического поиска у беременных с наличием тромбоцитопении необходимо иметь в виду, что в ряде случаев тромбоцитопения может быть дебютом СКВ и расценивается как первичная ИТП, по поводу которой назначаются глюкокортикоиды и даже описаны случаи спленэктомии [39]. В подобных ситуациях истинная природа тромбоцитопении проясняется только при появлении других системных признаков (суставной синдром, полисерозит, нефропатии и др.). ИТП предшествовала манифестации развернутой картины заболевания на протяжении до 10 лет у 16% больных СКВ [40]. По расчетам авторов, СКВ развивается у 3–15% больных с наличием ИТП. С учетом существования «гематологического» дебюта СКВ необходимо у больных с наличием неясной тромбоцитопении (особенно у молодых женщин, в том числе беременных) исключать СКВ. Частота СКВ у беременных составляет 1 случай на 1,5–3 тыс. беременностей, причем в 20% диагноз впервые устанавливается в гестационном периоде, а у 10% – после родов [41].При анализе 48 больных с СКВ, впервые диагностированной во время беременности (I и II триместры) или после родов, наиболее частыми проявлениями были тромбоцитопении и люпус-нефрит (25% и 68% соответственно). В то же время системные проявления СКВ (лихорадка, суставной синдром, алопеция, оральные язвы, гипокомплементемия) встречались значительно реже по сравнению с больными СКВ в отсутствие беременности [42]. По данным китайского исследования, включавшего 216 беременных с наличием СКВ, у 30% заболевание было впервые диагностировано во время беременности (I и II триместры) или после родов. Впервые диагностированная СКВ характеризовалась наличием тромбоцитопении и анемии, более выраженными по сравнению с беременными, ранее страдавшими СКВ [43].
Вирусные инфекции
Одной из причин тромбоцитопении, диагностированной впервые во время беременности, могут стать различные инфекции, преимущественно вирусные, играющие роль триггера. Основными инфекциями, на фоне которых возникает тромбоцитопения, являются инфекции, вызванные вирусом Эпштейна–Барр, вирусом гепатита В и С, ВИЧ и др. [27].Тромбоцитопения беременных, связанная с предшествующими заболеваниями
Очевидно, что беременная женщина может оказаться в поле зрения акушера-гинеколога, будучи еще до наступления беременности «обладательницей» каких-то заболеваний, при которых встречается тромбоцитопения (ИТП, гепатиты и циррозы печени, СКВ, гемобластозы и др.). При этом каждое из этих заболеваний может быть диагностировано впервые на основании догестационного анамнеза и имеющихся результатов клинико-лабораторного обследования, либо оно уже диагностировалось ранее и проводилось соответствующее лечение. Нередко при наступлении беременности возникает декомпенсация имеющихся заболеваний, в частности усугубление выраженности тромбоцитопении. В подобных ситуациях диагностическая проблема трансформируется в терапевтическую и заключается в тактике ведения беременной с конкретным соматическим заболеванием, что требует взаимодействия акушера со специалистами соответствующего профиля.Заключение
Расшифровка природы тромбоцитопении у беременных представляет непростую клиническую задачу для акушера-гинеколога и требует компетентности в вопросах патологии, гематологии, иммунологии и ряда других дисциплин. Прежде всего необходимо решить вопрос о необходимости проведения диагностического поиска с учетом количества тромбоцитов, клинической ситуации (данные анамнеза, в том числе и акушерского, наличие геморрагического синдрома, состояние других ростков кроветворения и т.д.). С учетом междисциплинарного характера проблемы тромбоцитопении у беременных необходимо конструктивное взаимодействие акушеров-гинекологов со смежными специалистами.Конфликт интересов. Автор заявляет об отсутствии конфликта интересов.
Сonflict of interests. The author declares that there is not conflict of interests.
Информация об авторе / Information about the author
Дворецкий Леонид Иванович – д-р мед. наук, проф. каф. госпитальной терапии №2 ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: dvoretski@mail.ru; ORCID: 0000-0003-3186-0102
Leonid I. Dvoretsky – D. Sci. (Med.), Prof., Sechenov First Moscow State Medical University (Sechenov University).
E-mail: dvoretski@mail.ru; ORCID: 0000-0003-3186-0102
Поступила в редакцию / Received: 07.03.2023
Поступила после рецензирования / Revised: 19.03.2023
Принята к публикации / Accepted: 30.03.2023
Список исп. литературыСкрыть список1. Cheng CK, Chan J, Cembrowski GS, van Assendelft OW. Complete blood count reference interval diagrams derived from NHANES III: stratification by age, sex, and race. Lab Hematol 2004; 10 (1): 42–53. DOI: 10.1532/lh96.04010
2. Boehlen F, Hohlfeld P, Extermann P et al. Platelet count at term pregnancy: a reappraisal of the threshold. Obstet Gynecol 2000; 95 (1): 29–33. DOI: 10.1016/s0029-7844(99)00537-2
3. Perepu U, Rosenstein L. Maternal thrombocytopenia in pregnancy. Proceed Obstet Gynecol 2013; 3: 6.
4. Reese JA, Peck JD, Deschamps DR et al. Platelet counts during pregnancy. N Engl J Med 2018; 379: 32–43. DOI: 10.1056/NEJMoa 1802897
5. Valera MC, Parant O, Vayssiere C et al. Physiologic and pathologic changes of platelets in pregnancy. Platelets 2010; 21: 587–95. DOI: 10.3109/09537104.2010.509828
6. Cines DB, Levine LD. Thrombocytopenia in pregnancy. Blood 2017; 130: 2271–7. DOI: 10.1182/blood-2017-05-781971
7. Bockenstedt PL. Thrombocytopenia in pregnancy. Hematol Oncol Clin North Am 2011; 25 (2): 293–310. DOI: 10.1016/j.hoc.2011.01.004
8. Reese JA, Peck JD, McIntosh JJ et al. Platelet counts in women with normal pregnancies: A systematic review. Am J Hematol 2017; 92 (11): 1224–32. DOI: 10.1002/ajh.24829. PMID: 28631317.
9. Kasai J, Aoki S, Kamiya N et al. Clinical features of gestational thrombocytopenia difficult to differentiate from immune thrombocytopenia diagnosed during pregnancy. J Obstet Gynaecol Res 2015; 41: 44–9. DOI:10.1111/jog.12496
10. Rottenstreich A, Israeli N, Levin G et al. Clinical characteristics, neonatal risk and recurrence rate of gestational thrombocytopenia with platelet count <100×109/L. Eur J Obstet Gynecol Reprod Biol 2018; 231: 75–9. DOI: 10.1016/j.ejogrb.2018.10.026
11. Kohli S, Ranjan S, Hoffmann J et al. Maternal extracellular vesicles and platelets promote preeclampsia via inflammasome activation in trophoblasts. Blood 2016; 12 (17): 2153–64. DOI: 10.1182/blood-2016-03-705434
12. Gestational hypertension and preeclampsia ACOG Practice Bulletin Summary, Number 222. Obstet Gynecol 2020; 135 (6): 1492–5. DOI: 10.1097/aog.0000000000003892
13. Gernsheimer T, James AH, Stasi R. How I treat thrombocytopenia in pregnancy. Blood 2013; 121: 38–47.
14. Myers B. Diagnosis and management of maternal thrombocytopenia in pregnancy. Br J Haematol 2012; 158: 3–15. DOI: 10.1111/j.1365-2141.2012.09135.x
15. Mol BWJ, Roberts CT, Thangaratinam S et al. Pre-eclampsia. Lancet 2016; 387: 999–1011. DOI: 10.1016/S0140-6736(15)00070-7
16. Martin JN, Rinehart BK, May WL et al. the spectrum of severe preeclampsia: comparative analysis by HELLP syndrome classification. Am J Obstet Gynecol 1999; 180: 1373–84. DOI: 10.1016/s0002-9378(99)70022-0
17. Fitzpatrick KE, Hinshaw K, Kurinczuk JJ, Knight M. Risk factors, management, and outcomes of hemolysis, elevated liver enzymes, and low platelets syndrome and elevated liver enzymes, low platelets syndrome. Obstet Gynecol 2014; 123: 618–27. DOI: 10.1097/AOG. 0000000000000140
18. Rath W, Faridi A, Dudenhausen JW. HELLP syndrome. J Perinat Med 2000; 28: 249–60. DOI: 10.1515/JPM.2000.033
19. Phipps E, Prasanna D, Brima W, Jim B. Preeclampsia: updates in pathogenesis, definitions, and guidelines. Clin J Am Soc Nephrol 2016; 11: 1102–13. DOI: 10.2215/CJN.12081115
20. Lee NM, Brady CW. Liver disease in pregnancy. World J Gastroenterol 2009; 15 (8): 897–906. DOI: 10.3748/wjg.15.897
21. Ding J, Han LP, Lou XP et al. Effectiveness of combining plasma exchange with plasma perfusion in acute fatty liver of pregnancy: a retrospective analysis. Gynecol Obstet Invest 2015; 79: 97–100. DOI: 10.1159/000368752
22. Макацария А.Д., Панфилова О.Ю. К вопросу о ДВС-синдроме в акушерстве: новое о старом. Практическая медицина. 2010; 4 (43): 25.
[Makatsariia A.D., Panfilova O.Iu. K voprosu o DVS-sindrome v akusherstve: novoe o starom. Prakticheskaia meditsina. 2010; 4 (43): 25 (in Russian).]
23. Mariotte E, Azoulay E, Galicier L et al. Epidemiology and pathophysiology of adulthood-onset thrombotic microangiopathy with severe ADAMTS13 deficiency (thrombotic thrombo-cytopenic purpura): a cross-sectional analysis of the French national registry for thrombotic microangiopathy. Lancet Haematol 2016; 3: e237–45. DOI: 10.1016/S2352-3026(16)30018-7
24. Von Auer C, von Krogh AS, Kremer Hovinga JA, Lämmle B. Current insights into thrombotic microangiopathies: Thrombotic thrombocytopenic purpura and pregnancy. Thromb Res 2015; 135 (Suppl. 1): 30–3. DOI: 10.1016/S0049-3848(15)50437-4
25. Kappler S, Ronan-Bentle S, Graham A. Thrombotic microangiopathies (TTP, HUS, HELLP). Emerg Med Clin N Am 2014; 32: 649–71. DOI: 10.1016/j.emc.2014.04.008
26. George JN, Nester CM. Syndrome of thrombotic microangiopathy. N Engl J Med 2014; 371: 654–66. DOI: 10.1056/NEJMra1312353
27. Bergmann F, Rath W. The Differential Diagnosis of Thrombocytopenia in Pregnancy. An interdisciplinary challenge. Dtsch Arztebl Int 2015; 112 (47): 795–802. DOI: 10.3238/arztebl.2015.0795
28. Keiser SD, Boyd KW, Rehberg JF et al. A high LDH to AST ratio helps to differentiate pregnancy-associated thrombotic thrombocytopenic purpura (TTP) from HELLP syndrome. J Matern-Fetal Neonatal Med 2012; 25: 1059–63. DOI: 10.3109/14767058.2011.619603
29. Jokiranta TS. HUS and atypical HUS. Blood 2017; 129: 2847–56. DOI: 10.1182/blood-2016-11-709865
30. Thomas MR, Robinson S, Scully MA. How we manage thrombotic microangiopathies in pregnancy. Br J Haematol 2016; 173: 821–30. DOI: 10.1111/bjh.14045
31. Legendre C.M., Licht C., Muus P. et al. Terminal complement inhibitor ecuzulimab in atypical hemolytic-uremic syndrome. N Engl J Med. 2013;368:2169–2181 DOI: 10.1056/NEJMoa1208981
32. Sarno L, Tufano A, Maruotti GM et al. Eculizumab in pregnancy: a narrative overview. J Nephrol 2019; 32: 17–25. DOI: 10.1007/s40620-018-0517-z
33. Park YH. Diagnosis and management of thrombocytopenia in pregnancy. Blood Res 2022; 57 (S1): 79–85. DOI: 10.5045/br.2022. 2022068. PMID: 35483931; PMCID: PMC9057658
34. Care A, Pavord S, Knight M, Alfirevic Z. Severe primary autoimmune thrombocytopenia in pregnancy: a national cohort study. BJOG 2018; 125 (5): 604–12. DOI: 10.1111/1471-0528.14697. PMID: 28432736
35. Gill KK, Kelton JG. Management of idiopathic thrombocytopenic purpura in pregnancy. Semin Hematol 2000; 37 (3): 275–89. DOI: 10.1016/s0037-1963(00)90106-9
36. Антифосфолипидный синдром. Под ред. Е.Л. Насонова. М.: Литтера, 2004.
[Antifosfolipidnyi sindrom. Pod red. E.L. Nasonova. M.: Littera, 2004 (in Russian).]
37. Miyakis S, Lockshin M, Atsumi T et al. International consensus statement on an update of the classifi cation criteria for defi nite antiphospholipid syndrome (APS). J Thromb Haemost 2006; 4: 295–306. DOI: 10.1111/j.1538-7836.2006.01753.x
38. Fayyaz A, Igoe A, Kurien B et al. Haematological manifestations of lupus. Lupus Sci Med 2015; 2: e000078. DOI: 10.1136/lupus-2014-000078
39. Bashal F. Hematological disorders in patients with systemic lupus erythematosus. Open Rheumatol J 2013; 7: 87–95. DOI: 10.2174/ 18743129013 07010087
40. Hepburn AL, Narat S, Mason JC. The management of peripheral blood cytopenias in systemic lupus erythematosus. Rheumatology 2010; 49 (12): 2243–54. DOI: 10.1093/rheumatology/keq269
41. Clowse ME, Jamison M, Myers E, James AH. A national study of the complications of lupus in pregnancy. Am J Obstet Gynecol 2008; 199 (2): 127. e1–6. DOI: 10.1016/j.ajog.2008.03.012
42. Zhao C, Zhao J, Huang Y et al. New-onset systemic lupus erythematosus during pregnancy. Clin Rheumatol 2013; 32 (6): 815–22. DOI: 10.1007/s10067-013-2180-z. PMID: 23358829
43. He X, Jiang D, Wang Z et al. Clinical features of new-onset systemic lupus erythematosus during pregnancy in Central China: a retrospective study of 68 pregnancies. Clin Rheumatol 2021; 40 (6): 2121–31. DOI: 10.1007/s10067-020-05452-2. PMID: 33064224.
28 июня 2023
Количество просмотров: 1277
