Клинический разбор в общей медицине №5 2024
Egor A. Borisenko1, Beatrice A. Volel1,5
1 Sechenov First Moscow State Medical University (Sechenov University), Moscow, Russia;
2 National Research University Higher School of Economics, Moscow, Russia;
3 Research center of neurology, Moscow, Russia;
4 Kazan Federal University, Kazan, Russia;
5 Mental health research center, Moscow, Russia;
petelin_d_s@staff.sechenov.ru
Abstract
Functional neurological disorders are widely represented in clinical practice, but their etiology, pathogenesis, as well as approaches to diagnosis and therapy have not been sufficiently studied. This article provides an overview of the taxonomy and clinical manifestations of functional neurological disorders. Modern data on the diagnosis of the discussed group of disorders are also presented, with an emphasis on instrumental methods – electroencephalography, transcranial magnetic stimulation, functional magnetic resonance imaging. The available data on evidence-based approaches to the treatment of functional neurological disorders are summarized. The main points of the literature review are illustrated by clinical observation.
Keywords: functional neurological disorders, electroencephalography, transcranial magnetic stimulation, functional magnetic resonance imaging.
For citation: Petelin D.S., Ragimova A.A., Gizetdinova K.R., Viazmin A.O., Borisenko E.A., Volel B.A. Modern approaches to the diagnosis and treatment of functional neurological disorders: clinical case and literature review. Clinical review for general practice. 2024; 5 (5): 49–56 (In Russ.). DOI: 10.47407/kr2024.5.5.00406
С современной точки зрения патогенез ФНР представляется комплексным, в их формировании могут быть задействованы различные факторы – генетические, психологические и клинические. В недавнем систематическом обзоре на модели функциональных
неэпилептических судорог было показано наличие генетических маркеров данного расстройства, преимущественно кодирующих различные белки в серотонинергических, адренергических и опиатергических путях головного мозга [7]. Значительную роль в формировании ФНР также играют перенесенные в детском возрасте травматические события, такие как физическое и сексуальное насилие, а также эмоциональная изоляция ребенка [8]. Накапливающиеся данные, кроме того, свидетельствуют в пользу широкого спектра нарушений в функционировании нейрональных контуров, которые задействованы в обработке сенсорной информации и формировании образа тела пациента [9]. Наконец, заслуживает упоминания тот факт, что ФНР могут формироваться после перенесенной коронавирусной инфекции, что может быть аргументом в пользу вклада нейровоспаления в развитие данной группы расстройств [10].
 Несмотря на наличие утвержденных и общепринятых операциональных критериев установления диагноза ФНР (например, критерии DSM-V в табл. 1), диагностика ФНР остается предметом для научной и практической дискуссии, однако имеет смысл остановиться на ряде консенсусных положений, которые разделяются большинством специалистов в этой области.
Несмотря на наличие утвержденных и общепринятых операциональных критериев установления диагноза ФНР (например, критерии DSM-V в табл. 1), диагностика ФНР остается предметом для научной и практической дискуссии, однако имеет смысл остановиться на ряде консенсусных положений, которые разделяются большинством специалистов в этой области.
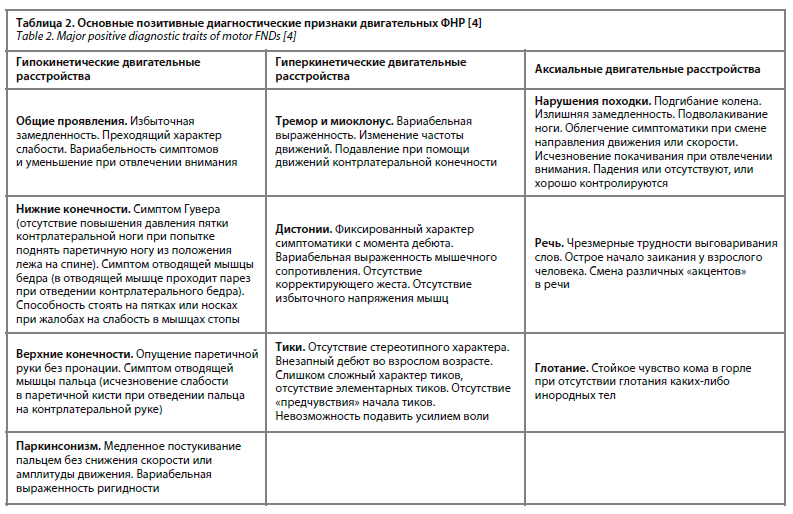
Так, важнейшим в диагностике ФНР является установление «позитивного» диагноза, под которым подразумевается выявление у пациента специфических патогномоничных симптомов ФНР, а не квалификации данного диагноза на основании непохожести наблюдаемых симптомов на какое-либо другое неврологическое заболевание [4]. Спектр патогномоничных симптомов ФНР исключительно широк, и они выявлены для большинства типов ФНР. Перечень основных позитивных диагностических свидетельств двигательных ФНР представлен в табл. 2.
Вторым важнейшим аспектом диагностики ФНР является необходимость психиатрического обследования пациентов. Несмотря на то что ФНР в настоящее время не рассматривается как чисто психиатрическое расстройство, у таких пациентов исключительно часто (около 75% всех наблюдений) отмечаются сопутствующие психические расстройства, преимущественно тревожного и депрессивного спектра, а также самоповреждающее поведение и расстройства пищевого поведения [11]. Несмотря на то что использование основных классов психофармакологических препаратов (антидепрессанты, антипсихотики и др.) не ассоциировано с достоверным улучшением самих ФНР, коррекция коморбидных расстройств может приводить к существенной положительной динамике и повышению качества жизни пациентов [12]. Третьим важным аспектом диагностики ФНР является нарастающее использование инструментальных методов обследования, которые демонстрируют все более обнадеживающие результаты. В частности, в последние десятилетия нейробиологические и нейрофизиологические исследования позволили выявить целый ряд маркеров ФНР при проведении электроэнцефалографии (ЭЭГ), анализе вызванных моторных потенциалов при проведении транкраниальной магнитной стимуляции (ТМС) и функциональной магнитно-резонансной томографии (фМРТ). Согласно недавнему метаанализу накопленные в этой области данные уже в ближайшие годы позволят разработать инструментальные диагностические маркеры, способствующие объективизации диагноза ФНР [13]. В связи с этим, представим краткий обзор выявленных в исследованиях биологических маркеров ФНР.
ЭЭГ-маркеры. Одним из наиболее известных биомаркеров ФНР является потенциал Берейтшафта (ПБ) – это медленно нарастающий потенциал, начинающийся примерно за секунду до самостоятельного движения [14]. В исследованиях было показано, что ПБ присутствует у 25–85% пациентов с функциональным миоклонусом (ФМ) непосредственно перед подергиванием [15–20]. Примечательно то, что отсутствие ПБ перед произвольным движением (разгибанием запястья) наблюдалось более чем у 1/2 пациентов с ФМ [17]. Также у пациентов с ФМ наблюдалось ослабление ритмов в бета- и гамма-диапазоне – связанная с событиями десинхронизация (ССД) [15, 16]. Оба биомаркера – ПБ и ССД позволяют различить ФМ от органического мио-клонуса со специфичностью в 100% и чувствительностью 75–80% [21]. Условная негативная вариация (CNV) – это негативная кортикальная волна, которая предшествует заранее заданному императивному стимулу, требующему быстрой двигательной реакции.
Подавление амплитуды CNV наблюдается у пациентов с ФМР в сравнении со здоровыми испытуемыми [22] и испытуемыми, имитирующими парез [23]. Наконец, в одном из исследований продемонстрировано недостаточное ослабление сенсорных вызванных потенциалов (СВП) при стимуляции срединного нерва у пациентов с ФНР в сравнении со здоровым контролем [24].
ТМС (МВП) маркеры. Моторные вызванные потенциалы, индуцированные ТМС во время произвольных мышечных сокращений у здоровых испытуемых имели меньшую задержку (латентность), более высокие амплитуды и большую длительность, чем у пациентов с ФНР [25]. В исследовании МВП во время моторного воображения (МВ) [26] было показано, что амплитуда МВП во время МВ у здоровых испытуемых увеличивалась на 200%, в то время как у пациентов с функциональным парезом воображение движения «паретичным» пальцем ассоциировалось со снижением средней амплитуды МВП на 37%. Воображение движения здоровым пальцем у тех же пациентов с парезом увеличило МВП всего на 63% в сравнении с МВП, записанными в состоянии покоя. Также у пациентов с функциональным парезом наблюдалось уменьшение кортикоспинальной проводимости во время воображения движения их собственных «пораженных» частей тела, что выражалось в снижении амплитуды МВП в сравнении со здоровыми испытуемыми [27, 28].
фМРТ-биомаркеры. Исследования, в которых пациенты выполняли эмоционально окрашенные задания, в целом характеризовали повышенную лимбическую/паралимбическую активность у пациентов с ФНР по сравнению с контрольной группой [29]. Например, было сообщено об ухудшении способности миндалевидного тела к быстрому снижению чувствительности при повторном предъявлении стимулов и повышенной сенсибилизации наряду с повышенной функциональной связанностью между миндалевидным телом и областями, отвечающими за контроль движений [30–35]. Однако есть исследования, показывающие нормальные или сниженные реакции миндалевидного тела [36–38]. Были описаны изменения в работе островковой доли мозга, поясной извилины и вентромедиальной префронтальной коры (вмПК) при обработке эмоций и управлении движениями. В исследовании S. Aybek и соавт., 2015 пациентам с ФНР и здоровым испытуемым предъявлялись эмоциональные стимулы в виде грустных и испуганных лиц с последующим заданием. В результате у пациентов с ФНР наблюдалась повышенная активация в областях, отвечающих за «реакцию замирания» на страх (околоводопроводное серое вещество), и областях, отвечающих за самосознание и двигательный контроль (поясная извилина и дополнительная двигательная область). В еще одной работе анализировали МРТ-снимки пациентки с функциональным параличом левой руки во время выполнения тестирования Go/No-Go с использованием обеих рук в сравнении с контрольной группой (здоровые испытуемые и испытуемые, имитирующие паралич). Подготовительная активация в правой моторной коре сопровождалась увеличением активности вмПК, а также наблюдалась увеличенная функциональная связанность между этими регионами [39]. У пациентов с функциональной дистонией [38] наблюдалась пониженная активность левой островковой доли во время выполнения заданий с интенсивными эмоциями. Напротив, пациенты с функциональной слабостью [40] и другими ФНР [41] демонстрировали повышенную активность левой островковой доли во время выполнения движений или задания с выбором действия. Другие исследования подтверждают роль областей мозга, участвующих в моторной концептуализации, ингибирующем контроле, внимании, метапознании, вере/ожиданиях, контроле эмоций и защитном поведении, связанном с угрозой, в патофизиологии ФНР [31–46].
• искренне и полно доносить до пациента информацию о диагнозе;
• открыто демонстрировать пациенту позитивные диагностические признаки функционального характера расстройства;
• объяснять сущность и природу имеющегося у пациента расстройства;
• выявлять и корректировать дисфункциональные представления пациента о диагнозе;
• использовать мотивационное интервью, для того чтобы простимулировать пациента на выздоровление;
• поддерживать независимое функционирование пациента и убежденность в возможности излечения;
• вовлекать семью и близких пациента в процесс диагностики и терапии.
Основными методиками помощи пациентам с ФНР являются психотерапия и физическая реабилитация (физиотерапия), данные по эффективности лекарственной терапии ограничены [49]. Среди психотерапевтических методик интенсивному изучению при ФНР подвергались когнитивно-поведенческая терапия (КПТ), терапия осознанности, диалектическая терапия и психотерапия, основанная на психоаналитических подходах. Наиболее убедительная доказательная база была получена в отношение КПТ, которая по некоторым данным позволяет достичь ремиссии у приблизительно 75% пациентов с ФНР. По некоторым данным, диалектическая поведенческая терапия позволяют достичь сопоставимых результатов, однако они были получены на менее масштабных выборках. Тем не менее в одном исследовании на модели неэпилептических функциональных судорог было показано, что присоединение КПТ к рутинному ведению пациентов не приводило к, собственно, урежению числа припадков, хотя и улучшало качество жизни и общий уровень функционирования [48].
С другой стороны, физическая реабилитация пациентов (поведенческая активация, выполнение физических упражнений, выработка навыков по преодолению ФНР) также демонстрировала достоверное положительное влияние не только на качество жизни, но и на выраженность самих ФНР [49]. В последние годы для усиления процесса реабилитации широко используются различные инновационные методики, в числе которых терапия виртуальной реальности, биологическая обратная связь и неинвазивные методики стимуляции головного мозга [4].
Данные по лекарственной терапии ограничены преимущественно описаниями отдельных клинических кейсов и в доступной литературе существуют лишь два рандомизированных клинических исследования. В одном из них при ФНР сравнивали бензодиазепиновый транквилизатор мидазолам с галоперидолом, а в другом галоперидол с кветиапном. В целом галоперидол продемонстрировал сопоставимую с кветиапном эффективность и был достоверно эффективнее мидазолама, однако как объемы выборок, так и размер эффекта в обоих исследованиях были достаточно небольшими, что затрудняет генерализацию полученных данных [49].
С целью проиллюстрировать некоторые из представленных данных, приводим клиническое наблюдение.
Пациентка А.Е.М., 34 лет. Обратилась на консультацию в психотерапевтическое отделение по рекомендации невролога с жалобами на приступообразно формирующуюся слабость в мышцах нижних конечностей, которые сменяются приступами мышечных спазмов, затрудняющих ходьбу.
Анамнез. Наследственность развернутыми психопатологическими состояниями не отягощена, родственницы по линии матери (мать, тетка, бабка) по характеру были выраженно тревожными, склонными опасаться за свое здоровье и здоровье окружающих.
Родилась от нормально протекавшей беременности, роды в срок, развивалась по возрасту. С малых лет была крайне впечатлительной, боязливой, отмечались страхи темноты, грозы, не переносила нахождения в одиночестве длительное время, часто плакала. Детские дошкольные учреждения посещала, однако была там капризной, с трудом соглашалась оставлять родителей. В возрасте
6 лет была свидетелем ограбления квартиры соседей, после чего в течение нескольких месяцев выраженно заикалась, боялась куда-либо выходить без сопровождения родителей. Затем состояние редуцировалось.
В школу пошла в возрасте 7 лет, адаптировалась к нахождению в школе лучше, чем в детском дошкольном учреждении, сумела завести несколько подруг. Училась на хорошо и удовлетворительно, после школы окончила техникум, работала.
В 23 года вышла замуж, отношения в браке были стабильными, родила в браке двух детей, роды в 25 и 28 лет. Период беременности и послеродовый период проходил спокойно, аффективных колебаний не отмечалось.
Заболела остро в возрасте 32 лет – без видимой провокации во время прогулки с ребенком во дворе отметила появление выраженной слабости в ногах, стала ощущать в них выраженное онемение. С того момента оказалась ограничена в передвижениях, стала пользоваться палкой при ходьбе. В дальнейшем клинические проявления расстройства усложнились за счет появления приступообразных гиперкинезов – в состоянии покоя периодически стала отмечать спазм и напряжение мышц нижних конечностей, приводившее к насильственному разгибанию бедра. Выраженность симптоматики была плавающей – более выраженная на улице, в домашних условиях она, по словам родственников, то возникала, то исчезала.
Вместе с тем стала отмечать появление выраженной немотивированной приступообразной тревоги с массивной соматовегетативной симптоматикой (одышка, учащенное сердцебиение, головокружение, чувство нереальности происходящего). Иногда приступы обходились самостоятельно, иногда усложнялись за счет присоединения гиперкинезов в мышцах ног.
Сформировала ограничительное поведение – в связи с симптомами ушла с работы, стала просить родственников сопровождать ее во время прогулок с детьми, сама никуда не выходила. При этом существенного снижения настроения не отмечала, в отсутствие приступов паники радовалась жизни, справлялась с уходом за детьми в домашних условиях.
В течение последующих двух лет 6 раз госпитализировалась в стационары психиатрического и неврологического профиля. Динамика состояния в условиях стационара была стереотипной – формировалось быстрое улучшение состояния с почти полной редукцией тревоги и неврологической симптоматики, особенно после внутривенных инфузий лекарственных препаратов как транквилизаторов, так и ноотропных препаратов. После выписки из стационара каждый раз отмечала полное возобновление симптоматики, несмотря на прием предписанной поддерживающей терапии (получала рекомендации по приему после выписки габапентина, амитриптилина, пароксетина, сертралина, тофизопама). В связи с этим быстро отменяла поддерживающую психофармакотерпию. Обратилась на консультацию в Клинику нервных болезней.
Психический статус. Выглядит на свой возраст, аккуратно одета, декоративной косметикой не пользуется. При ходьбе опирается на трость, подволакивает последовательно обе ноги при ходьбе. На прием приходит в сопровождении матери, стремится говорить с врачом в ее присутствии. Жалуется на выраженную слабость в обеих нижних конечностях. В связи со слабостью ограничивает перемещения в отсутствие сопровождающих лиц из страха упасть и остаться беспомощной. Также беспокоят жалобы на приступы паники с массивной соматовегетативной симптоматикой, страхом смерти, на высоте которых отмечает спазм мышц нижних конечностей. На фоне обсуждения вопросов здоровья несколько раз отмечают эпизоды насильственного разгибания мышц бедра, во время которых плачет и быстро успокаивается. Фон настроения ровный. Сон и аппетит не нарушены. Суицидальные мысли отрицает. Настроена на госпитализацию.
Неврологический статус. Менингеальной симптоматики нет. Лицо симметрично. Зрачки правильной формы, обычного размера, реакция на свет, конвергенцию, аккомодацию сохранна. Глазные щели симметричны. Острота слуха в пределах нормы (различает шепотную речь с расстояния 6 м). Вестибулярной атаксии и нистагма нет. Язык по средней линии, глотание не нарушено. Мышечный тонус в норме, D=S. Сухожильные рефлексы в норме в верхних и нижних конечностях. Сила в верхних конечностях достаточная, с нижних – снижение до 3–4 баллов во всех группах мышц. При неврологическом обследовании выявляются симптомы Гувера и симптом отводящей мышцы бедра. Несколько раз в процессе неврологического обследования отмечаются сокращения передней группы бедренных мышц, приводящие к формированному разгибанию ноги. Сокращение прекращается при отвлечении внимания пациентки. В позе Ромберга пошатывается. Пальценосовую пробу выполняет. Тазовые функции сохранены.
В результатах лабораторных (общий анализ крови и мочи, расширенная биохимия крови) и инструментальных (МРТ головного мозга, электронейромиография мышц нижних конечностей) методов обследования – без патологии.
Пациентке установлен двойной диагноз – ФНР и паническое расстройство с агорафобией. Пациентка в полной мере соответствует клиническим критериям диагностики ФНР (см. табл. 1), кроме того, в неврологическом статусе выявляются позитивные диагностические симптомы диагностики ФНР, такие как симптом Гувера, симптом отводящей мышцы бедра и вариабельность симптоматики (см. табл. 2).
С пациенткой и ее родственниками была проведена разъяснительная беседа о характере имеющихся у нее симптомов и отсутствии необходимости в госпитализации с учетом прошлого нестойкого эффекта от стационарного лечения. Рекомендован прием пароксетина в дозе до 40 мг/сут амбулаторно, бромдигидрохлорфенилбензодиазепин по 0,5 мг при тревоге, а также курс КПТ. Основными направлениями работы в ходе КПТ были коррекция представлений пациентки о своем заболевании, как о жизнеугрожающем или инвалидизирующим, поиск и коррекция автоматических мыслей, провоцирующих формирование приступов паники и гиперкинезов. Пациентке даны рекомендации по ведению дневника эмоций, постепенному повышению экспозиции к ситуациям, вызывающим страх (в первую очередь, нахождение на улице).
Катамнез через 6 мес. На фоне продолжающейся психофармакотерапии и психотерапии отметила существенное улучшение самочувствия – полностью прошли приступы паники, а также сокращения мышц нижних конечностей. Слабость в ногах сохранилась без существенной динамики, однако в существенной степени скорректировалось связанное с ней ограничительное поведение – начала самостоятельно выходить на улицу, в полной мере справляется с уходом за детьми. В неврологическом статусе было выявлено незначительное повышение мышечной силы в нижних конечностях до 4 баллов.
Разбор. В представленном клиническом наблюдении состояние пациентки определяется сосуществованием двух расстройств – ФНР с двигательными симптомами как по типу парезов, так и по типу гиперкинезов, а также паническое расстройство с формированием агорафобии. При этом отмечается взаимное влияние двух расстройств – функциональная неврологическая симптоматика в значительной степени определяет развитие агорафобии, а на высоте приступов паники в части случаев происходит усложнение картины ФНР.
Представленное клиническое наблюдение ярко иллюстрирует некоторые литературные данные из представленных в настоящем обзоре. У обсуждаемой пациентки в анамнезе было выявлено выраженное психотравмирующее событие детского возраста (стала свидетелем ограбления), выраженность которого оказалась достаточна, чтобы вызывать преходящее заикание. Также динамика пациентки в условиях стационаров хорошо соотносятся с литературными данными о выраженном эффекте плацебо, который свойственен для пациентов с ФНР.
Успех в терапии пациентки был достигнут за счет использования методик коммуникации, предложенных S. Kola и соавт. – с пациенткой проведена детальная разъяснительная беседа о сути ее расстройства, были продемонстрированы объективные свидетельства функционального характера неврологической симптоматики, в процесс реабилитации были включены родственники пациентки [4]. Корректировка дисфункциональных представлений о болезни была произведена в том числе и за счет борьбы с нарастающими признаками госпитализма – пациентке разъяснена необходимость адаптации во внебольничных условиях и бессмысленность дальнейшего стационарного лечения. При этом динамика обсуждаемых расстройств сопоставима с данными литературы об относительно быстрой редукции тревожных расстройств на фоне психотерапии и психофармакотерапии, но крайне медленном изменении выраженности ФНР.
Конфликт интересов. Авторы заявляют об отсутствии конфликта интересов.
Conflict of interests. The authors declare that there is not conflict of interests.
Финансирование: Данная работа/статья является результатом исследовательского проекта, реализованного в рамках Программы фундаментальных исследований Национального исследовательского университета «Высшая школа экономики» (НИУ ВШЭ)
Financing: This work/article is an output of a research project implemented as part of the Basic Research Program at the National Research University Higher School of Economics (HSE University)
Информация об авторах
Information about the authors
Петелин Дмитрий Сергеевич – канд. мед. наук, ассистент каф. психиатрии и психосоматики ИКМ им. Н.В. Склифосовского, ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: petelin_d_s@staff.sechenov.ru; ORCID: 0000-0002-2228-6316
Dmitry S. Petelin – Cand. Sci. (Med.), Sechenov First Moscow State Medical University (Sechenov University).
E-mail: petelin_d_s@staff.sechenov.ru;
ORCID: 0000-0002-2228-6316
Рагимова Айнур Алигейдаровна – канд. мед. наук, науч. сотр. Института когнитивных нейронаук Центра нейроэкономики и когнитивных исследований Национального исследовательского института «Высшая школа экономики»; врач-психиатр, ФГБНУ «Научный центр неврологии». ORCID: 0000-0002-4370-4249
Aynur A. Ragimova – Cand. Sci. (Med.), Institute for Cognitive Neuroscience / Centre for Cognition & Decision Makin, HSE University; Psychiatrist, Research Center
of Neurology. ORCID: 0000-0002-4370-4249
Гизетдинова Камиля Рафаэлевна – студентка, ФГАОУ ВО «Казанский (Приволжский) Федеральный Университет».
ORCID: 0009-0004-7682-4396
Kamilya R. Gizetdinova – Student, Kazan Federal University. ORCID: 0009-0004-7682-4396
Вязьмин Александр Олегович – аспирант, Национальный исследовательский институт «Высшая школа экономики».
ORCID: 0000-0003-2346-4222
Alexandr O. Viazmin – Graduate Student, HSE University. ORCID: 0000-0003-2346-4222
Борисенко Егор Артемович – студент, ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет).
ORCID: 0009-0009-4657-3924
Egor A. Borisenko – Student, Sechenov First Moscow State Medical University (Sechenov University).
ORCID: 0009-0009-4657-3924
Волель Беатриса Альбертовна – д-р мед. наук, директор
ИКМ им. Н.В. Склифосовского, ФГАОУ ВО «Первый МГМУ
им. И.М. Сеченова» (Сеченовский Университет), вед. науч. сотр. отдела по изучению пограничной психической патологии
и психосоматических расстройств, ФГБНУ «Научный центр психического здоровья. ORCID: 0000-0003-1667-5355
Beatrice A. Volel – Dr. Sci. (Med.), Head of N.V. Sklifosovsky Institution for Clinical Medicine, Sechenov First Moscow State Medical University (Sechenov University); Federal state budgetary scientific institution mental health research center. ORCID: 0009-0009-4657-3924
Поступила в редакцию: 06.05.2024
Поступила после рецензирования: 15.05.2024
Принята к публикации: 23.04.2024
Received: 06.05.2024
Revised: 15.05.2024
Accepted: 23.04.2024
Клинический разбор в общей медицине №5 2024
Современные подходы к диагностике и терапии функциональных неврологических расстройств: клиническое наблюдение и обзор литературы
Номера страниц в выпуске:49-56
Аннотация
Функциональные неврологические расстройства широко представлены в клинической практике, однако их этиология, патогенезы, а также подходы к диагностике и терапии изучены недостаточно. В настоящей статье представлен обзор систематики и клинических проявлений функциональный неврологических расстройств. Также представлены современные данные о диагностике обсуждаемой группы расстройств с акцентом на инструментальных методах – электроэнцефалографии, транскраниальной магнитной стимуляции, функциональной магнитной резонансной томографии. Обобщены доступные данные о доказательных подходах к терапии функциональных неврологических расстройств. Основные положения обзора литературы проиллюстрированы клиническим наблюдением.
Ключевые слова: функциональные неврологические расстройства, электроэнцефалография, транскраниальная магнитная стимуляция, функциональная магнитно-резонансная томография
Для цитирования: Петелин Д.С., Рагимова А.А., Гизетдинова К.Р., Вязьмин А.О., Борисенко Е.А., Волель Б.А. Современные подходы к диагностике и терапии функциональных неврологических расстройств: клиническое наблюдение и обзор литературы. Клинический разбор в общей медицине. 2024; 5 (5): 49–56. DOI: 10.47407/kr2024.5.5.00406
Функциональные неврологические расстройства широко представлены в клинической практике, однако их этиология, патогенезы, а также подходы к диагностике и терапии изучены недостаточно. В настоящей статье представлен обзор систематики и клинических проявлений функциональный неврологических расстройств. Также представлены современные данные о диагностике обсуждаемой группы расстройств с акцентом на инструментальных методах – электроэнцефалографии, транскраниальной магнитной стимуляции, функциональной магнитной резонансной томографии. Обобщены доступные данные о доказательных подходах к терапии функциональных неврологических расстройств. Основные положения обзора литературы проиллюстрированы клиническим наблюдением.
Ключевые слова: функциональные неврологические расстройства, электроэнцефалография, транскраниальная магнитная стимуляция, функциональная магнитно-резонансная томография
Для цитирования: Петелин Д.С., Рагимова А.А., Гизетдинова К.Р., Вязьмин А.О., Борисенко Е.А., Волель Б.А. Современные подходы к диагностике и терапии функциональных неврологических расстройств: клиническое наблюдение и обзор литературы. Клинический разбор в общей медицине. 2024; 5 (5): 49–56. DOI: 10.47407/kr2024.5.5.00406
Modern approaches to the diagnosis and treatment of functional neurological disorders: clinical case and literature review
Dmitry S. Petelin1, Aynur A. Ragimova2,3, Kamilya R. Gizetdinova4, Alexandr O. Viazmin2,Egor A. Borisenko1, Beatrice A. Volel1,5
1 Sechenov First Moscow State Medical University (Sechenov University), Moscow, Russia;
2 National Research University Higher School of Economics, Moscow, Russia;
3 Research center of neurology, Moscow, Russia;
4 Kazan Federal University, Kazan, Russia;
5 Mental health research center, Moscow, Russia;
petelin_d_s@staff.sechenov.ru
Abstract
Functional neurological disorders are widely represented in clinical practice, but their etiology, pathogenesis, as well as approaches to diagnosis and therapy have not been sufficiently studied. This article provides an overview of the taxonomy and clinical manifestations of functional neurological disorders. Modern data on the diagnosis of the discussed group of disorders are also presented, with an emphasis on instrumental methods – electroencephalography, transcranial magnetic stimulation, functional magnetic resonance imaging. The available data on evidence-based approaches to the treatment of functional neurological disorders are summarized. The main points of the literature review are illustrated by clinical observation.
Keywords: functional neurological disorders, electroencephalography, transcranial magnetic stimulation, functional magnetic resonance imaging.
For citation: Petelin D.S., Ragimova A.A., Gizetdinova K.R., Viazmin A.O., Borisenko E.A., Volel B.A. Modern approaches to the diagnosis and treatment of functional neurological disorders: clinical case and literature review. Clinical review for general practice. 2024; 5 (5): 49–56 (In Russ.). DOI: 10.47407/kr2024.5.5.00406
Введение
Функциональные неврологические расстройства (ФНР) представляют собой группу широко распространенных и клинически значимых патологических состояний, характеризующихся формированием неврологической симптоматики, которая не соотносится с объективно выявляемым повреждением нейрональной ткани [1]. Спектр клинических проявлений ФНР крайне широк и включает такие расстройства, как двигательные нарушения, выпадение сенсорных функций, а также неэпилептические судороги [2]. Распространенность, согласно современным исследованиям, представляется значительно более высокой, чем предполагалось ранее. Так, представленность ФНР в популяции составляет от 4 до 12 случаев на 100 тыс. населения, в то время как в специализированных неврологических стационарах на долю ФНР приходится до 6–16% всех обращений [1, 3]. Дополнительно проблема ФНР актуализируется в связи с тем, что диагностика и терапия данного расстройства до настоящего времени остается предметом научных и практических дискуссий, а основанные на принципах доказательной медицины протоколы до настоящего времени не разработаны [4].Этиология и патогенез
Первоначальная клиническая и психопатологическая концептуализация ФНР была сформирована в рамках психоаналитической концепции и предполагала трактовать данные расстройства как «конверсионные», что подразумевает трансформацию несознаваемых психических конфликтов и травматических переживаний в телесную сферу [5]. Подобная концептуализация ФНР подразумевала их манифестацию по психогенным механизмам и вероятно высокую эффективность психотерапии, в том числе психодинамической. Однако реальная клиническая практика и результаты недавних исследований свидетельствуют в пользу преимущественно хронического и безремиссионного течения ФНР у значительной части пациентов. Так, согласно систематическому обзору J. Gelauf, при катамнестическом наблюдении (средний срок 7 лет) у 39% (10–90% по разным данным) пациентов симптомы сохраняются несмотря на любые медицинские вмешательства [6]. Данные факты наряду с накапливающимися нейробиологическими данными заставляют рассматривать патогенез ФНР как более комплексный и задействующий целый ряд факторов, помимо психологических.С современной точки зрения патогенез ФНР представляется комплексным, в их формировании могут быть задействованы различные факторы – генетические, психологические и клинические. В недавнем систематическом обзоре на модели функциональных
неэпилептических судорог было показано наличие генетических маркеров данного расстройства, преимущественно кодирующих различные белки в серотонинергических, адренергических и опиатергических путях головного мозга [7]. Значительную роль в формировании ФНР также играют перенесенные в детском возрасте травматические события, такие как физическое и сексуальное насилие, а также эмоциональная изоляция ребенка [8]. Накапливающиеся данные, кроме того, свидетельствуют в пользу широкого спектра нарушений в функционировании нейрональных контуров, которые задействованы в обработке сенсорной информации и формировании образа тела пациента [9]. Наконец, заслуживает упоминания тот факт, что ФНР могут формироваться после перенесенной коронавирусной инфекции, что может быть аргументом в пользу вклада нейровоспаления в развитие данной группы расстройств [10].
Подходы к диагностике
 Несмотря на наличие утвержденных и общепринятых операциональных критериев установления диагноза ФНР (например, критерии DSM-V в табл. 1), диагностика ФНР остается предметом для научной и практической дискуссии, однако имеет смысл остановиться на ряде консенсусных положений, которые разделяются большинством специалистов в этой области.
Несмотря на наличие утвержденных и общепринятых операциональных критериев установления диагноза ФНР (например, критерии DSM-V в табл. 1), диагностика ФНР остается предметом для научной и практической дискуссии, однако имеет смысл остановиться на ряде консенсусных положений, которые разделяются большинством специалистов в этой области.Так, важнейшим в диагностике ФНР является установление «позитивного» диагноза, под которым подразумевается выявление у пациента специфических патогномоничных симптомов ФНР, а не квалификации данного диагноза на основании непохожести наблюдаемых симптомов на какое-либо другое неврологическое заболевание [4]. Спектр патогномоничных симптомов ФНР исключительно широк, и они выявлены для большинства типов ФНР. Перечень основных позитивных диагностических свидетельств двигательных ФНР представлен в табл. 2.

Вторым важнейшим аспектом диагностики ФНР является необходимость психиатрического обследования пациентов. Несмотря на то что ФНР в настоящее время не рассматривается как чисто психиатрическое расстройство, у таких пациентов исключительно часто (около 75% всех наблюдений) отмечаются сопутствующие психические расстройства, преимущественно тревожного и депрессивного спектра, а также самоповреждающее поведение и расстройства пищевого поведения [11]. Несмотря на то что использование основных классов психофармакологических препаратов (антидепрессанты, антипсихотики и др.) не ассоциировано с достоверным улучшением самих ФНР, коррекция коморбидных расстройств может приводить к существенной положительной динамике и повышению качества жизни пациентов [12]. Третьим важным аспектом диагностики ФНР является нарастающее использование инструментальных методов обследования, которые демонстрируют все более обнадеживающие результаты. В частности, в последние десятилетия нейробиологические и нейрофизиологические исследования позволили выявить целый ряд маркеров ФНР при проведении электроэнцефалографии (ЭЭГ), анализе вызванных моторных потенциалов при проведении транкраниальной магнитной стимуляции (ТМС) и функциональной магнитно-резонансной томографии (фМРТ). Согласно недавнему метаанализу накопленные в этой области данные уже в ближайшие годы позволят разработать инструментальные диагностические маркеры, способствующие объективизации диагноза ФНР [13]. В связи с этим, представим краткий обзор выявленных в исследованиях биологических маркеров ФНР.
ЭЭГ-маркеры. Одним из наиболее известных биомаркеров ФНР является потенциал Берейтшафта (ПБ) – это медленно нарастающий потенциал, начинающийся примерно за секунду до самостоятельного движения [14]. В исследованиях было показано, что ПБ присутствует у 25–85% пациентов с функциональным миоклонусом (ФМ) непосредственно перед подергиванием [15–20]. Примечательно то, что отсутствие ПБ перед произвольным движением (разгибанием запястья) наблюдалось более чем у 1/2 пациентов с ФМ [17]. Также у пациентов с ФМ наблюдалось ослабление ритмов в бета- и гамма-диапазоне – связанная с событиями десинхронизация (ССД) [15, 16]. Оба биомаркера – ПБ и ССД позволяют различить ФМ от органического мио-клонуса со специфичностью в 100% и чувствительностью 75–80% [21]. Условная негативная вариация (CNV) – это негативная кортикальная волна, которая предшествует заранее заданному императивному стимулу, требующему быстрой двигательной реакции.
Подавление амплитуды CNV наблюдается у пациентов с ФМР в сравнении со здоровыми испытуемыми [22] и испытуемыми, имитирующими парез [23]. Наконец, в одном из исследований продемонстрировано недостаточное ослабление сенсорных вызванных потенциалов (СВП) при стимуляции срединного нерва у пациентов с ФНР в сравнении со здоровым контролем [24].
ТМС (МВП) маркеры. Моторные вызванные потенциалы, индуцированные ТМС во время произвольных мышечных сокращений у здоровых испытуемых имели меньшую задержку (латентность), более высокие амплитуды и большую длительность, чем у пациентов с ФНР [25]. В исследовании МВП во время моторного воображения (МВ) [26] было показано, что амплитуда МВП во время МВ у здоровых испытуемых увеличивалась на 200%, в то время как у пациентов с функциональным парезом воображение движения «паретичным» пальцем ассоциировалось со снижением средней амплитуды МВП на 37%. Воображение движения здоровым пальцем у тех же пациентов с парезом увеличило МВП всего на 63% в сравнении с МВП, записанными в состоянии покоя. Также у пациентов с функциональным парезом наблюдалось уменьшение кортикоспинальной проводимости во время воображения движения их собственных «пораженных» частей тела, что выражалось в снижении амплитуды МВП в сравнении со здоровыми испытуемыми [27, 28].
фМРТ-биомаркеры. Исследования, в которых пациенты выполняли эмоционально окрашенные задания, в целом характеризовали повышенную лимбическую/паралимбическую активность у пациентов с ФНР по сравнению с контрольной группой [29]. Например, было сообщено об ухудшении способности миндалевидного тела к быстрому снижению чувствительности при повторном предъявлении стимулов и повышенной сенсибилизации наряду с повышенной функциональной связанностью между миндалевидным телом и областями, отвечающими за контроль движений [30–35]. Однако есть исследования, показывающие нормальные или сниженные реакции миндалевидного тела [36–38]. Были описаны изменения в работе островковой доли мозга, поясной извилины и вентромедиальной префронтальной коры (вмПК) при обработке эмоций и управлении движениями. В исследовании S. Aybek и соавт., 2015 пациентам с ФНР и здоровым испытуемым предъявлялись эмоциональные стимулы в виде грустных и испуганных лиц с последующим заданием. В результате у пациентов с ФНР наблюдалась повышенная активация в областях, отвечающих за «реакцию замирания» на страх (околоводопроводное серое вещество), и областях, отвечающих за самосознание и двигательный контроль (поясная извилина и дополнительная двигательная область). В еще одной работе анализировали МРТ-снимки пациентки с функциональным параличом левой руки во время выполнения тестирования Go/No-Go с использованием обеих рук в сравнении с контрольной группой (здоровые испытуемые и испытуемые, имитирующие паралич). Подготовительная активация в правой моторной коре сопровождалась увеличением активности вмПК, а также наблюдалась увеличенная функциональная связанность между этими регионами [39]. У пациентов с функциональной дистонией [38] наблюдалась пониженная активность левой островковой доли во время выполнения заданий с интенсивными эмоциями. Напротив, пациенты с функциональной слабостью [40] и другими ФНР [41] демонстрировали повышенную активность левой островковой доли во время выполнения движений или задания с выбором действия. Другие исследования подтверждают роль областей мозга, участвующих в моторной концептуализации, ингибирующем контроле, внимании, метапознании, вере/ожиданиях, контроле эмоций и защитном поведении, связанном с угрозой, в патофизиологии ФНР [31–46].
Терапия ФНР
Считается, что эффективное ведение пациентов с ФНР должно начинаться с должного информирования пациентов и детального разъяснения им характера расстройства, от которого они страдают. Несмотря на исключительно высокий ответ на плацебо у обсуждаемой категории пациентов, использование методик, основанных на эффекте плацебо, считается некорректной клинической практикой в связи с формированием у пациента ошибочного представления о характере имеющегося заболевания [47]. S. Kola и соавт. предложили следующие основные подходы к коммуницированию с пациентом, страдающим от ФНР [4]:• искренне и полно доносить до пациента информацию о диагнозе;
• открыто демонстрировать пациенту позитивные диагностические признаки функционального характера расстройства;
• объяснять сущность и природу имеющегося у пациента расстройства;
• выявлять и корректировать дисфункциональные представления пациента о диагнозе;
• использовать мотивационное интервью, для того чтобы простимулировать пациента на выздоровление;
• поддерживать независимое функционирование пациента и убежденность в возможности излечения;
• вовлекать семью и близких пациента в процесс диагностики и терапии.
Основными методиками помощи пациентам с ФНР являются психотерапия и физическая реабилитация (физиотерапия), данные по эффективности лекарственной терапии ограничены [49]. Среди психотерапевтических методик интенсивному изучению при ФНР подвергались когнитивно-поведенческая терапия (КПТ), терапия осознанности, диалектическая терапия и психотерапия, основанная на психоаналитических подходах. Наиболее убедительная доказательная база была получена в отношение КПТ, которая по некоторым данным позволяет достичь ремиссии у приблизительно 75% пациентов с ФНР. По некоторым данным, диалектическая поведенческая терапия позволяют достичь сопоставимых результатов, однако они были получены на менее масштабных выборках. Тем не менее в одном исследовании на модели неэпилептических функциональных судорог было показано, что присоединение КПТ к рутинному ведению пациентов не приводило к, собственно, урежению числа припадков, хотя и улучшало качество жизни и общий уровень функционирования [48].
С другой стороны, физическая реабилитация пациентов (поведенческая активация, выполнение физических упражнений, выработка навыков по преодолению ФНР) также демонстрировала достоверное положительное влияние не только на качество жизни, но и на выраженность самих ФНР [49]. В последние годы для усиления процесса реабилитации широко используются различные инновационные методики, в числе которых терапия виртуальной реальности, биологическая обратная связь и неинвазивные методики стимуляции головного мозга [4].
Данные по лекарственной терапии ограничены преимущественно описаниями отдельных клинических кейсов и в доступной литературе существуют лишь два рандомизированных клинических исследования. В одном из них при ФНР сравнивали бензодиазепиновый транквилизатор мидазолам с галоперидолом, а в другом галоперидол с кветиапном. В целом галоперидол продемонстрировал сопоставимую с кветиапном эффективность и был достоверно эффективнее мидазолама, однако как объемы выборок, так и размер эффекта в обоих исследованиях были достаточно небольшими, что затрудняет генерализацию полученных данных [49].
С целью проиллюстрировать некоторые из представленных данных, приводим клиническое наблюдение.
Пациентка А.Е.М., 34 лет. Обратилась на консультацию в психотерапевтическое отделение по рекомендации невролога с жалобами на приступообразно формирующуюся слабость в мышцах нижних конечностей, которые сменяются приступами мышечных спазмов, затрудняющих ходьбу.
Анамнез. Наследственность развернутыми психопатологическими состояниями не отягощена, родственницы по линии матери (мать, тетка, бабка) по характеру были выраженно тревожными, склонными опасаться за свое здоровье и здоровье окружающих.
Родилась от нормально протекавшей беременности, роды в срок, развивалась по возрасту. С малых лет была крайне впечатлительной, боязливой, отмечались страхи темноты, грозы, не переносила нахождения в одиночестве длительное время, часто плакала. Детские дошкольные учреждения посещала, однако была там капризной, с трудом соглашалась оставлять родителей. В возрасте
6 лет была свидетелем ограбления квартиры соседей, после чего в течение нескольких месяцев выраженно заикалась, боялась куда-либо выходить без сопровождения родителей. Затем состояние редуцировалось.
В школу пошла в возрасте 7 лет, адаптировалась к нахождению в школе лучше, чем в детском дошкольном учреждении, сумела завести несколько подруг. Училась на хорошо и удовлетворительно, после школы окончила техникум, работала.
В 23 года вышла замуж, отношения в браке были стабильными, родила в браке двух детей, роды в 25 и 28 лет. Период беременности и послеродовый период проходил спокойно, аффективных колебаний не отмечалось.
Заболела остро в возрасте 32 лет – без видимой провокации во время прогулки с ребенком во дворе отметила появление выраженной слабости в ногах, стала ощущать в них выраженное онемение. С того момента оказалась ограничена в передвижениях, стала пользоваться палкой при ходьбе. В дальнейшем клинические проявления расстройства усложнились за счет появления приступообразных гиперкинезов – в состоянии покоя периодически стала отмечать спазм и напряжение мышц нижних конечностей, приводившее к насильственному разгибанию бедра. Выраженность симптоматики была плавающей – более выраженная на улице, в домашних условиях она, по словам родственников, то возникала, то исчезала.
Вместе с тем стала отмечать появление выраженной немотивированной приступообразной тревоги с массивной соматовегетативной симптоматикой (одышка, учащенное сердцебиение, головокружение, чувство нереальности происходящего). Иногда приступы обходились самостоятельно, иногда усложнялись за счет присоединения гиперкинезов в мышцах ног.
Сформировала ограничительное поведение – в связи с симптомами ушла с работы, стала просить родственников сопровождать ее во время прогулок с детьми, сама никуда не выходила. При этом существенного снижения настроения не отмечала, в отсутствие приступов паники радовалась жизни, справлялась с уходом за детьми в домашних условиях.
В течение последующих двух лет 6 раз госпитализировалась в стационары психиатрического и неврологического профиля. Динамика состояния в условиях стационара была стереотипной – формировалось быстрое улучшение состояния с почти полной редукцией тревоги и неврологической симптоматики, особенно после внутривенных инфузий лекарственных препаратов как транквилизаторов, так и ноотропных препаратов. После выписки из стационара каждый раз отмечала полное возобновление симптоматики, несмотря на прием предписанной поддерживающей терапии (получала рекомендации по приему после выписки габапентина, амитриптилина, пароксетина, сертралина, тофизопама). В связи с этим быстро отменяла поддерживающую психофармакотерпию. Обратилась на консультацию в Клинику нервных болезней.
Психический статус. Выглядит на свой возраст, аккуратно одета, декоративной косметикой не пользуется. При ходьбе опирается на трость, подволакивает последовательно обе ноги при ходьбе. На прием приходит в сопровождении матери, стремится говорить с врачом в ее присутствии. Жалуется на выраженную слабость в обеих нижних конечностях. В связи со слабостью ограничивает перемещения в отсутствие сопровождающих лиц из страха упасть и остаться беспомощной. Также беспокоят жалобы на приступы паники с массивной соматовегетативной симптоматикой, страхом смерти, на высоте которых отмечает спазм мышц нижних конечностей. На фоне обсуждения вопросов здоровья несколько раз отмечают эпизоды насильственного разгибания мышц бедра, во время которых плачет и быстро успокаивается. Фон настроения ровный. Сон и аппетит не нарушены. Суицидальные мысли отрицает. Настроена на госпитализацию.
Неврологический статус. Менингеальной симптоматики нет. Лицо симметрично. Зрачки правильной формы, обычного размера, реакция на свет, конвергенцию, аккомодацию сохранна. Глазные щели симметричны. Острота слуха в пределах нормы (различает шепотную речь с расстояния 6 м). Вестибулярной атаксии и нистагма нет. Язык по средней линии, глотание не нарушено. Мышечный тонус в норме, D=S. Сухожильные рефлексы в норме в верхних и нижних конечностях. Сила в верхних конечностях достаточная, с нижних – снижение до 3–4 баллов во всех группах мышц. При неврологическом обследовании выявляются симптомы Гувера и симптом отводящей мышцы бедра. Несколько раз в процессе неврологического обследования отмечаются сокращения передней группы бедренных мышц, приводящие к формированному разгибанию ноги. Сокращение прекращается при отвлечении внимания пациентки. В позе Ромберга пошатывается. Пальценосовую пробу выполняет. Тазовые функции сохранены.
В результатах лабораторных (общий анализ крови и мочи, расширенная биохимия крови) и инструментальных (МРТ головного мозга, электронейромиография мышц нижних конечностей) методов обследования – без патологии.
Пациентке установлен двойной диагноз – ФНР и паническое расстройство с агорафобией. Пациентка в полной мере соответствует клиническим критериям диагностики ФНР (см. табл. 1), кроме того, в неврологическом статусе выявляются позитивные диагностические симптомы диагностики ФНР, такие как симптом Гувера, симптом отводящей мышцы бедра и вариабельность симптоматики (см. табл. 2).
С пациенткой и ее родственниками была проведена разъяснительная беседа о характере имеющихся у нее симптомов и отсутствии необходимости в госпитализации с учетом прошлого нестойкого эффекта от стационарного лечения. Рекомендован прием пароксетина в дозе до 40 мг/сут амбулаторно, бромдигидрохлорфенилбензодиазепин по 0,5 мг при тревоге, а также курс КПТ. Основными направлениями работы в ходе КПТ были коррекция представлений пациентки о своем заболевании, как о жизнеугрожающем или инвалидизирующим, поиск и коррекция автоматических мыслей, провоцирующих формирование приступов паники и гиперкинезов. Пациентке даны рекомендации по ведению дневника эмоций, постепенному повышению экспозиции к ситуациям, вызывающим страх (в первую очередь, нахождение на улице).
Катамнез через 6 мес. На фоне продолжающейся психофармакотерапии и психотерапии отметила существенное улучшение самочувствия – полностью прошли приступы паники, а также сокращения мышц нижних конечностей. Слабость в ногах сохранилась без существенной динамики, однако в существенной степени скорректировалось связанное с ней ограничительное поведение – начала самостоятельно выходить на улицу, в полной мере справляется с уходом за детьми. В неврологическом статусе было выявлено незначительное повышение мышечной силы в нижних конечностях до 4 баллов.
Разбор. В представленном клиническом наблюдении состояние пациентки определяется сосуществованием двух расстройств – ФНР с двигательными симптомами как по типу парезов, так и по типу гиперкинезов, а также паническое расстройство с формированием агорафобии. При этом отмечается взаимное влияние двух расстройств – функциональная неврологическая симптоматика в значительной степени определяет развитие агорафобии, а на высоте приступов паники в части случаев происходит усложнение картины ФНР.
Представленное клиническое наблюдение ярко иллюстрирует некоторые литературные данные из представленных в настоящем обзоре. У обсуждаемой пациентки в анамнезе было выявлено выраженное психотравмирующее событие детского возраста (стала свидетелем ограбления), выраженность которого оказалась достаточна, чтобы вызывать преходящее заикание. Также динамика пациентки в условиях стационаров хорошо соотносятся с литературными данными о выраженном эффекте плацебо, который свойственен для пациентов с ФНР.
Успех в терапии пациентки был достигнут за счет использования методик коммуникации, предложенных S. Kola и соавт. – с пациенткой проведена детальная разъяснительная беседа о сути ее расстройства, были продемонстрированы объективные свидетельства функционального характера неврологической симптоматики, в процесс реабилитации были включены родственники пациентки [4]. Корректировка дисфункциональных представлений о болезни была произведена в том числе и за счет борьбы с нарастающими признаками госпитализма – пациентке разъяснена необходимость адаптации во внебольничных условиях и бессмысленность дальнейшего стационарного лечения. При этом динамика обсуждаемых расстройств сопоставима с данными литературы об относительно быстрой редукции тревожных расстройств на фоне психотерапии и психофармакотерапии, но крайне медленном изменении выраженности ФНР.
Заключение
ФНР широко представлены в популяции и среди неврологических пациентов. Патогенез данной группы расстройств является комплексным и включает генетические, психологические и нейробиологические факторы риска. Диагностика ФНР основана на выявлении позитивных диагностических признаков при неврологическом осмотре, а также на консультации психиатра, необходимой для выявления часто встречающихся при ФНР коморбидных психических расстройств. Накапливающиеся данные о биологических маркерах ФНР в ближайшие годы позволят сформировать объективизированные подходы к подтверждению диагноза. Несмотря на свойственное ФНР хроническое течение и малую эффективность медикаментозной терапии, комплексная психообразовательная, психотерапевтическая и реабилитационная помощь позволяет достичь улучшения у большинства пациентов с ФНР.Конфликт интересов. Авторы заявляют об отсутствии конфликта интересов.
Conflict of interests. The authors declare that there is not conflict of interests.
Финансирование: Данная работа/статья является результатом исследовательского проекта, реализованного в рамках Программы фундаментальных исследований Национального исследовательского университета «Высшая школа экономики» (НИУ ВШЭ)
Financing: This work/article is an output of a research project implemented as part of the Basic Research Program at the National Research University Higher School of Economics (HSE University)
Информация об авторах
Information about the authors
Петелин Дмитрий Сергеевич – канд. мед. наук, ассистент каф. психиатрии и психосоматики ИКМ им. Н.В. Склифосовского, ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: petelin_d_s@staff.sechenov.ru; ORCID: 0000-0002-2228-6316
Dmitry S. Petelin – Cand. Sci. (Med.), Sechenov First Moscow State Medical University (Sechenov University).
E-mail: petelin_d_s@staff.sechenov.ru;
ORCID: 0000-0002-2228-6316
Рагимова Айнур Алигейдаровна – канд. мед. наук, науч. сотр. Института когнитивных нейронаук Центра нейроэкономики и когнитивных исследований Национального исследовательского института «Высшая школа экономики»; врач-психиатр, ФГБНУ «Научный центр неврологии». ORCID: 0000-0002-4370-4249
Aynur A. Ragimova – Cand. Sci. (Med.), Institute for Cognitive Neuroscience / Centre for Cognition & Decision Makin, HSE University; Psychiatrist, Research Center
of Neurology. ORCID: 0000-0002-4370-4249
Гизетдинова Камиля Рафаэлевна – студентка, ФГАОУ ВО «Казанский (Приволжский) Федеральный Университет».
ORCID: 0009-0004-7682-4396
Kamilya R. Gizetdinova – Student, Kazan Federal University. ORCID: 0009-0004-7682-4396
Вязьмин Александр Олегович – аспирант, Национальный исследовательский институт «Высшая школа экономики».
ORCID: 0000-0003-2346-4222
Alexandr O. Viazmin – Graduate Student, HSE University. ORCID: 0000-0003-2346-4222
Борисенко Егор Артемович – студент, ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет).
ORCID: 0009-0009-4657-3924
Egor A. Borisenko – Student, Sechenov First Moscow State Medical University (Sechenov University).
ORCID: 0009-0009-4657-3924
Волель Беатриса Альбертовна – д-р мед. наук, директор
ИКМ им. Н.В. Склифосовского, ФГАОУ ВО «Первый МГМУ
им. И.М. Сеченова» (Сеченовский Университет), вед. науч. сотр. отдела по изучению пограничной психической патологии
и психосоматических расстройств, ФГБНУ «Научный центр психического здоровья. ORCID: 0000-0003-1667-5355
Beatrice A. Volel – Dr. Sci. (Med.), Head of N.V. Sklifosovsky Institution for Clinical Medicine, Sechenov First Moscow State Medical University (Sechenov University); Federal state budgetary scientific institution mental health research center. ORCID: 0009-0009-4657-3924
Поступила в редакцию: 06.05.2024
Поступила после рецензирования: 15.05.2024
Принята к публикации: 23.04.2024
Received: 06.05.2024
Revised: 15.05.2024
Accepted: 23.04.2024
Список исп. литературыСкрыть список1. Mishra A, Pandey S. Functional Neurological Disorders: Clinical Spectrum, Diagnosis, and Treatment. Neurologist. 2022;27(5):276-89. DOI: 10.1097/NRL.0000000000000453
2. Bennett K, Diamond C, Hoeritzauer I et al. A practical review of functional neurological disorder (FND) for the general physician. Clin Med (Lond). 2021;21(1):28-36. DOI: 10.7861/clinmed.2020-0987
3. O’Mahony B, Nielsen G, Baxendale S et al. Economic Cost of Functional Neurologic Disorders: A Systematic Review. Neurology. 2023;101(2): 202-14. DOI: 10.1212/WNL.0000000000207388
4. Kola S, LaFaver K. Updates in Functional Movement Disorders: from Pathophysiology to Treatment Advances. Curr Neurol Neurosci Rep. 2022;22(5):305-11. DOI: 10.1007/s11910-022-01192-9
5. Sharma VD, Jones R, Factor SA. Psychodynamic Psychotherapy for Functional (Psychogenic) Movement Disorders. J Mov Disord. 2017;10(1):40-4. DOI: 10.14802/jmd.16038
6. Gelauff J, Stone J, Edwards M et al. The prognosis of functional (psychogenic) motor symptoms: a systematic review. J Neurol, Neurosurge, Psychiatry. 2014;85(2):220-6. DOI: 10.1136/jnnp-2013-305321
7. Asadi-Pooya AA, Hallett M, Mirzaei Damabi N, Fazelian Dehkordi K. Genetics of Functional Seizures; A Scoping Systematic Review. Genes (Basel). 2023;14(8), 1537. DOI: 10.3390/genes14081537
8. Ludwig L, Pasman JA, Nicholson T et al. Stressful life events and maltreatment in conversion (functional neurological) disorder: systematic review and meta-analysis of case-control studies. Lancet Psychiatry. 2018;5(4):307–320. DOI: 10.1016/S2215-0366(18)30051-8
9. Drane DL, Fani N, Hallett M et al. A framework for understanding the pathophysiology of functional neurological disorder. CNS Spectr. 2020;4:1-7. DOI: 10.1017/S1092852920001789
10. Shishorin R, Gamirova A, Tolmacheva V et al. The onset of functional movement disorders after COVID-19: A case series. Indian J Psychiatry. 2022;64(5):529-32. DOI: 10.4103/indianjpsychiatry.indianjpsychiatry_327_22
11. Macchi ZA, Kletenik I, Olvera C et al. Psychiatric Comorbidities in Functional Movement Disorders: A Retrospective Cohort Study. Mov Disord Clin Pract. 2021;8(5):725-32. DOI:10.1002/mdc3.13226
12. O’Connell N, Nicholson T, Blackman G et al. Medication prescriptions in 322 motor functional neurological disorder patients in a large UK mental health service: A case control study. Gen Hosp Psychiatry. 2019;58:94-102. DOI:10.1016/j.genhosppsych.2019.04.004
13. Patwal R, Jolly AJ, Kumar A et al. Diagnostic accuracy of clinical signs and investigations for functional weakness, sensory and movement disorders: A systematic review. J Psychosom Res. 2023;168:111196. DOI: 10.1016/j.jpsychores.2023.111196
14. Deecke L. Bereitschaftspotential as an indicator of movement preparation in supplementary motor area and motor cortex. Ciba Found Symp. 1987;132:231-50. DOI: 10.1002/9780470513545.ch14
15. Beudel M, Zutt R, Meppelink AM et al. Improving neurophysiological biomarkers for functional myoclonic movements. Parkinsonism Relat Disord. 2018;51:3-8. DOI: 10.1016/j.parkreldis.2018.03.029
16. Meppelink AM, Little S, Oswal A s et al. Event related desynchronisation predicts functional propriospinal myoclonus. Parkinsonism Relat Disord. 2016;31:116-8. DOI: 10.1016/j.parkreldis.2016.07.010
17. van der Salm SMA, Tijssen MAJ, Koelman JHTM et al. The bereitschaftspotential in jerky movement disorders. J Neurol Neurosurg Psychiatry. 2012; 83(12):1162-7. DOI: 10.1136/jnnp-2012-303081
18. Terada K, Ikeda A, Van Ness PC et al. Presence of Bereitschaftspotential preceding psychogenic myoclonus: clinical application of jerk-locked back averaging. J Neurol Neurosurg Psychiatry. 1995; 58(6):745-7. DOI: 10.1136/jnnp.58.6.745
19. Erro R, Bhatia KP, Edwards MJ et al. Clinical diagnosis of propriospinal myoclonus is unreliable: an electrophysiologic study. Mov Disord. 2013;28(13):1868-73. DOI:10.1002/mds.25627
20. Esposito M, Edwards MJ, Bhatia KP et al. Idiopathic spinal myoclonus: a clinical and neurophysiological assessment of a movement disorder of uncertain origin. Mov Disord. 2009; 24(16):2344–2349. DOI: 10.1002/mds.22812
21. Thomsen BLC, Teodoro T, Edwards MJ. Biomarkers in functional movement disorders: a systematic review. J Neurol Neurosurg Psychiatry. 2020;91(12):1261-9. DOI: 10.1136/jnnp-2020-323141
22. Teodoro T, Koreki A, Meppelink AM et al. Contingent negative variation: a biomarker of abnormal attention in functional movement disorders. Eur J Neurol. 2020;27:985-94. DOI: 10.1111/ene.14189
23. Blakemore RL, Hyland BI, Hammond-Tooke GD et al. Deficit in late-stage contingent negative variation provides evidence for disrupted movement preparation in patients with conversion paresis. Biol Psychol. 2015;109:73-85. DOI: 10.1016/j.biopsycho.2015.04.009
24. Macerollo A, Chen J-C, Pareés I et al. Sensory attenuation assessed by sensory evoked potentials in functional movement disorders. PLoS One. 2015;10(6):e0129507. DOI: 10.1371/journal.pone.0129507
25. Brum M, Cabib C, Valls-Solé J. Clinical value of the assessment of changes in MEP duration with voluntary contraction. Front Neurosci. 2015;9:505. DOI: 10.3389/fnins.2015.00505
26. Liepert J, Hassa T, Tüscher O et al. Abnormal motor excitability in patients with psychogenic paresis. A TMS study. J Neurol. 2009;256(1):121-6. DOI: 10.1007/s00415-009-0090-4
27. Liepert J, Hassa T, Tüscher O et al. Electrophysiological correlates of motor conversion disorder. Mov Disord. 2008;23(15):2171-6. DOI: 10.1002/mds.21994
28. Liepert J, Hassa T, Tüscher O et al. Motor excitability during movement imagination and movement observation in psychogenic lower limb paresis. J Psychosom Res. 2011;70(1):59-65. DOI: 10.1016/j.jpsychores.2010.06.004
29. Pick S, Goldstein LH, Perez DL et al. Emotional processing in functional neurological disorder: a review, biopsychosocial model and research agenda. J Neurol Neurosurg Psychiatry. 2019;90:704-11. DOI:10.1136/jnnp-2018-319201
30. Aybek S, Nicholson TR, Zelaya F et al. Neural Correlates of Recall of Life Events in Conversion Disorder. JAMA Psychiatry. 2014;71(1):52–60. DOI:10.1001/jamapsychiatry.2013.2842
31. Aybek S, Nicholson TR, O’Daly O. Emotion-Motion Interactions in Conversion Disorder: An fMRI Study. PLoS ONE. 2015;10(4): e0123273. DOI: 10.1371/journal.pone.0123273
32. Espay AJ, Maloney T, Vannest J et al. Impaired emotion processing in functional (psychogenic) tremor: A functional magnetic resonance imaging study. Neuroimage Clin. 2018;17:179-87. DOI:10.1016/j. nicl.2017.10.020
33. Hassa T, Sebastian A, Liepert J et al. Symptom-specific amygdala hyperactivity modulates motor control network in conversion disorder. NeuroImage Clin. 2017;15:143-50. DOI: 10.1016/j.nicl.2017.04.004
34. Morris LS, To B, Baek K et al. Disrupted avoidance learning in functional neurological disorder: Implications for harm avoidance theories. Neuroimage Clin. 2017;16:286-94. DOI: 10.1016/j.nicl.2017.08.007
35. Voon V, Brezing C, Gallea C et al. Emotional stimuli and motor conversion disorder. Brain. 2010;33:1526-36. DOI: 10.1093/brain/awq054
36. Allendorfer JB, Nenert R, Hernando KA et al. FMRI response to acute psychological stress differentiates patients with psychogenic non-epileptic seizures from healthy controls. A biochemical and neuroimaging biomarker study. Neuroimage Clin. 2019;24:101967. DOI: 10.1016/j.nicl.2019.101967
37. Balachandran N, Goodman AM, Allendorfer JB et al. Relationship between neural responses to stress and mental health symptoms in psychogenic nonepileptic seizures after traumatic brain injury. Epilepsia. 2021;62:107-19. DOI: 10.1111/epi.16758
38. Espay AJ, Maloney T, Vannest J et al. Dysfunction in emotion processing underlies functional (psychogenic) dystonia. Mov Disord. 2018;33(1):136-45. DOI:10.1002/mds.27217
39. Cojan Y, Waber L, Carruzzo A et al. Motor inhibition in hysterical conversion paralysis. Neuroimage. 2019;47:1026-37. DOI: 10.1016/j.neuroimage.2009.05.023
40. Stone J, Zeman A, Simonotto E et al. Sharpe FMRI in patients with motor conversion symptoms and controls with simulated weakness. Psychosom Med. 2007;69(9):961-9. DOI: 10.1097/PSY.0b013e31815b6c14
41. Voon V, Brezing C, Gallea C et al. Aberrant supplementary motor complex and limbic activity during motor preparation in motor conversion disorder. Mov Disord. 2011;26(13):2396-403. DOI: 10.1002/mds. 23890
42. Bègue I, Blakemore R, Klug J et al. Metacognition of visuomotor decisions in conversion disorder. Neuropsychologia. 2018;114:251-65. DOI: 10.1016/j.neuropsychologia.2018.04.018
43. Deeley Q, Oakley DA, Toone B et al. Halligan The functional anatomy of suggested limb paralysis. Cortex. 2013;49(2):411-22. DOI: 10.1016/j.cortex.2012.09.016
44. Edwards MJ, Adams RA, Brown H et al. A Bayesian account of ‚hysteria‘. Brain. 2012;135(11):3495-512. DOI: 10.1093/brain/aws129
45. Schrag AE, Mehta AR, Bhatia KP et al. The functional neuroimaging correlates of psychogenic versus organic dystonia. Brain. 2013;136:770-81. DOI: 10.1093/brain/awt008
46. Voon V, Cavanna AE, Coburn K et al. Functional neuroanatomy and neurophysiology of functional neurological disorders (Conversion Disorder). J Neuropsychiatry Clin Neurosci. 2016;28(3):168-90. DOI: 10.1176/appi.neuropsych.14090217
47. Fiorio M, Braga M, Marotta A et al. (2022). Functional neurological disorder and placebo and nocebo effects: shared mechanisms. Nat Rev Neurol. 2022;18(10):624-35. DOI: 10.1038/s41582-022-00711-z
48. Goldstein LH, Robinson EJ, Mellers JDC et al. Cognitive behavioural therapy for adults with dissociative seizures (CODES): a pragmatic, multicentre, randomised controlled trial. Lancet Psychiatry. 2020;7(6):491-505. DOI: 10.1016/S2215-0366(20)30128-0
49. Varley D, Sweetman J, Brabyn S et al. The clinical management of functional neurological disorder: A scoping review of the literature. J Psychosom Res. 2023;165:111121. DOI: 10.1016/j.jpsychores.2022.
111121
50. Alberto J. Espay, Thomas Maloney, Jennifer Vannest et al.Impaired emotion processing in functional (psychogenic) tremor. A functional magnetic resonance imaging study. NeuroImage: Clinical. 2018;17:179-87. DOI: 10.1016/j.nicl.2017.10.020


