Психиатрия Всемирная психиатрия
Психиатрия Всемирная психиатрия
№03 2021
Клиническая характеристика взрослых пациентов с тревогой и связанными расстройствами, направленная на персонализированное ведение №03 2021
Номера страниц в выпуске:336-356
Резюме
Клинический конструкт “тревожные неврозы” был широким и плохо определенным понятием, так что описание и разграничение специфичных тревожных расстройств в DSM-III были важной задачей. Однако тревога и связанные расстройства не только часто коморбидны, но также очень гетерогенны. Таким образом, диагностические руководства обеспечивают только первый шаг к формированию плана ведения пациента, и требуется разработка вспомогательных методов лечения тревожных состояний. Эта статья направлена на систематическое описание важных факторов (доменов) персонализированного ведения взрослых пациентов с тревогой и связанными расстройствами. Мы собрали результаты доступных исследований и рассмотрели релевантные диагностические методы, уделяя особое внимание возможности их использования в рутинной клинической практике. Мы выделили области, где имеющиеся данные позволяют клиницистам персонализировать ведение тревожных состояний, и определили, где таких данных недостаточно. В целом исследования показывают, что мы приближаемся к переходу от стандартных рекомендаций по терапии тревоги и связанных расстройств селективными ингибиторами обратного захвата серотонина, когнитивно-поведенческой терапией или их комбинацией, к более комплексному подходу, показывающему, что у клинициста есть более широкий спектр доступных методов лечения, и что лечение тревожных состояний может быть персонализировано уже сейчас в некоторых важных аспектах.
Ключевые слова: тревога, тревога и связанные расстройства, обсессивно-компульсивное расстройство, посттравматическое стрессовое расстройство, персонализация лечения, профиль симптомов, клинические субтипы, тяжесть, нейрокогниция, функционирование, качество жизни, личностные черты, психиатрические антецеденты, психиатрическая коморбидность, соматическая коморбидность, семейная история, раннее средовое воздействие, недавние средовые факторы, защитные факторы, дисфункциональные когнитивные схемы.
Клинический конструкт “тревожные неврозы” был широким и плохо определенным понятием, так что описание и разграничение специфичных тревожных расстройств в DSM-III были важной задачей. Однако тревога и связанные расстройства не только часто коморбидны, но также очень гетерогенны. Таким образом, диагностические руководства обеспечивают только первый шаг к формированию плана ведения пациента, и требуется разработка вспомогательных методов лечения тревожных состояний. Эта статья направлена на систематическое описание важных факторов (доменов) персонализированного ведения взрослых пациентов с тревогой и связанными расстройствами. Мы собрали результаты доступных исследований и рассмотрели релевантные диагностические методы, уделяя особое внимание возможности их использования в рутинной клинической практике. Мы выделили области, где имеющиеся данные позволяют клиницистам персонализировать ведение тревожных состояний, и определили, где таких данных недостаточно. В целом исследования показывают, что мы приближаемся к переходу от стандартных рекомендаций по терапии тревоги и связанных расстройств селективными ингибиторами обратного захвата серотонина, когнитивно-поведенческой терапией или их комбинацией, к более комплексному подходу, показывающему, что у клинициста есть более широкий спектр доступных методов лечения, и что лечение тревожных состояний может быть персонализировано уже сейчас в некоторых важных аспектах.
Ключевые слова: тревога, тревога и связанные расстройства, обсессивно-компульсивное расстройство, посттравматическое стрессовое расстройство, персонализация лечения, профиль симптомов, клинические субтипы, тяжесть, нейрокогниция, функционирование, качество жизни, личностные черты, психиатрические антецеденты, психиатрическая коморбидность, соматическая коморбидность, семейная история, раннее средовое воздействие, недавние средовые факторы, защитные факторы, дисфункциональные когнитивные схемы.
Тревожные расстройства – самые распространенные психические расстройства, их распространенность в общей популяции достигает 7,3% 1 . Дифференцировка специфичных тревожных расстройств в DSM-III была важным шагом к разработке более персонализированного лечения пациентов с тревогой 2 . Например, раньше считали, что пациенты с тревожными расстройствами реагируют преимущественно на ингибиторы моноаминоксидазы (МАО) 3 . В то же время тревожные расстройства характеризуются значительной коморбидностью и гетерогенны по своей феноменологии и психобиологии. Так, например, социальное тревожное расстройство часто сопровождается генерализованным тревожным расстройством (ГТР) 4 . Хотя существует множество данных об эффективности селективных ингибиторов обратного захвата серотонина и когнитивно-поведенческой терапии в лечении тревожных расстройств, эта гетерогенность может объяснить, почему некоторые пациенты не реагируют на первую линию терапии 5 .
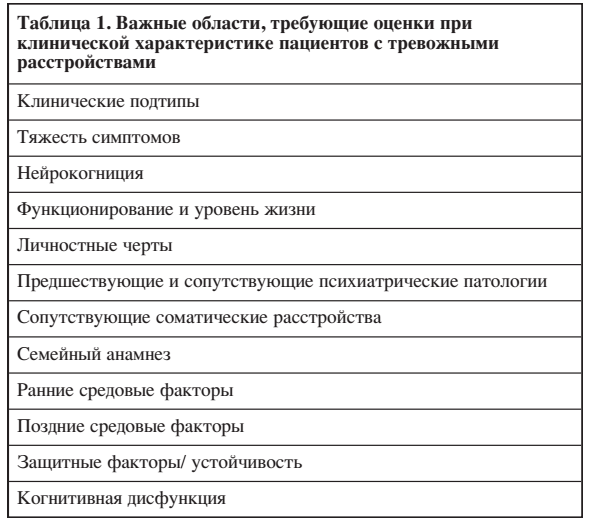
Хотя современные диагностические системы, безусловно, полезны для составления первоначального плана лечения, приходится разрабатывать вспомогательные диагностические методы. Они помогают отойти от гайдлайнов, которые делают упор на СИОЗС и КПТ как первую линию терапии, к более детальной диагностике, которая предоставляет клиницистам больше конкретных рекомендаций и способствует более персонализированному подходу к терапии пациента. Эта статья направлена на систематическое описание важных факторов (доменов), релевантных для персонализированного ведения пациентов с тревожными расстройствами и связанными состояниями, такими как обсессивно-компульсивное расстройство (ОКР) и посттравматическое стрессовое расстройство (ПТСР) (Таблица 1). Для каждого фактора (домена) мы собрали результаты актуальных исследований и рассмотрели релевантные диагностические инструменты, уделяя особое внимание возможности использовать их в рутинной клинической практике. Мы выделили области, где имеющиеся данные позволяют клиницистам персонализировать ведение тревожных состояний, и определили, где таких данных недостаточно. Научная литература, посвященная тревоге, имеет много пересечений с работами о депрессии, поэтому неудивительно, что факторы, описанные в этой работе, сходны с факторами, описанными в предыдущей статье по депрессии.
В соответствии с принципами доказательной медицины, значительные усилия были приложены к поиску биомаркеров тревожного расстройства и связанных состояний. Примечательно, что возникновение и уменьшение страха – это парадигма, лежащая в основе симптомов всех тревожных расстройств, а также концептуализации подходов к лечению. Другие специфические конструкции, такие как когнитивная гибкость и ингибиторный контроль, могут быть более актуальными для конкретных заболеваний, таких как ОКР 8 . Эти концепты были отмечены в классификации психических расстройств Национального института психического здоровья США (NIMH) Исследовательских критериев доменов (RDoC) 9 , и способствовали разделению тревожных расстройств в DSM-5 и МКБ-11 на тревожное или связанные со страхом расстройства, обсессивно-компульсивное и связанные расстройства и расстройства, специфически связанные со стрессом (эти термины использованы в МКБ-11).
Несмотря на обилие серьезных работ по нейробиологии тревоги и связанных расстройств, на сегодняшний день не существует достаточно чувствительных и специфических биомаркеров, которые можно использовать в клинической практике. Поэтому мы не рассматриваем подробно биомаркеры в нашей статье. Однако мы предполагаем, что более персонализированный подход к пациентам с тревогой, может быть полезен в поиске биомаркеров, а также для работы над нейробиологией тревоги в целом, учитывая потенциальную ценность более тонких клинических методов оценки гетерогенности расстройства способами, которые могут быть нейробиологически информативными и предсказать реакцию на лечение.
Статья фокусируется на тревоге и связанных расстройствах у взрослых пациентов. Данные заболевания часто имеют раннее начало, и изучение тревоги у детей важно, как с клинической точки зрения, так и с точки зрения общественного здравоохранения, поэтому необходимы дополнительные исследования тревожных расстройств у детей и подростков. Мы также не рассматриваем подробно тревогу, возникающую вторично по отношению к другим психическим расстройствам, таким как депрессивное расстройство, психотические расстройства, тревогу, связанную с другими медицинскими состояниями, или тревогу, связанную с приемом препаратов, несмотря на их клиническое значение. Также мы не рассматриваем подпороговый уровень тревоги и связанных расстройств. Там, где это уместно, рассматриваются культуральные и гендерные вопросы.
ПРОФИЛЬ СИМПТОМОВ
Тревожные расстройства проявляются тревогой, страхом и/или паническими атаками, часто сопровождаются избегающим поведением или чрезмерной осторожностью по отношению к предполагаемым угрозам. В DSM-5 и
МКБ-11 тревожные расстройства включают: агорафобию, генерализованное тревожное расстройство (ГТР), паническое расстройство, элективный мутизм, тревожное расстройство, вызванное разлукой, специфические фобии и социальное тревожное расстройство. ОКР и ПТСР выносят в отдельную, но тесно связанную группу. В обоих нозологиях диагностика тревожных расстройств предполагает наличие у пациента выраженного или существенного уровня страха или тревоги, которые отличаются от стресс-индуцированной тревоги стойкостью (т.е. длятся несколько месяцев и больше) и уровнем приносимого дискомфорта.
В МКБ-10 и DSM-5 тревожные расстройства в первую очередь дифференцируют по предполагаемой угрозе и объектам и ситуациям, вызывающим тревогу или страх. Предполагаемая угроза и связанные стимулы варьируются от жестко ограниченных (например, при специфических фобиях) и ситуативных (агорафобия, тревожное расстройство при разлуке, паническое расстройство и социальное тревожное расстройство) к распространенным на все области жизни (при генерализованном тревожном расстройстве). Таким образом, при малой специфичности тревоги, как симптома, тревожные расстройства могут быть дифференцированы при тщательном изучении ситуаций, при которых возникают тревога и избегающее поведение.
Например, паническое расстройство возникает из-за интероцептивных сигналов, которые ошибочно оцениваются как вредные, тогда как социальная тревога характеризуется страхом социальных взаимодействий и публичных выступлений, вследствие боязни негативной оценки окружающими. Дифференциальная диагностика тревожных расстройств имеет важное значение для ведения пациента и подбора терапии, поскольку большинство научно обоснованных фармакологических и психологических методов лечения эффективны только при определенных расстройствах.
Наиболее значимые отличия в диагностических критериях между МКБ-11 и DSM-5 у ПТСР. В DSM-5 критерии были существенно расширены, чтобы включить двадцать симптомов в 4 кластера, в попытке охватить весь спектр хронических посттравматических расстройств. В отличие от этого, МКБ-11 упростил диагностические требования к ПТСР до трех основных симптомов, которые наиболее четко отличают это расстройство от других состояний: повторное переживание травмирующего события или событий в настоящем, попытки избежать напоминания о событии и ощущения постоянной угрозы. Данные исследований показывают, что упрощенные критерии МКБ-11 эффективнее помогают диагностировать ПТСР, чем критерии DSM-5. МКБ-11 определяет, что “комплекс ПТСР” состоит из 3 основных симптомов, описанных выше, которые сопровождаются нарушением регуляции аффекта, пониженной самооценкой и трудностями в отношениях с окружающими. Анализ скрытого класса и анализ скрытого профиля подтвердили различия между ПТСР и “комплексом ПТСР”, а также обнаружили связь между сложным ПТСР и травмой в детстве в некоторых исследованиях.
Тревожные расстройства проявляются чувством страха или тревогой. Страх – это эмоциональная реакция на воспринимаемую предсказуемую или неминуемую угрозу, когда мало или совсем нет времени для сознательной разработки стратегии побега, в то время как тревога – это ориентированное на будущее состояние ожидания неопределенных, длительных или отдаленных угроз, когда есть время понять и прочувствовать природу ситуации. Оба состояния предназначены для активации когнитивных, аффективных, физиологических и поведенческих процессов, повышающих безопасность. В случае страха быстрые, непроизвольные физиологические реакции облегчают выбор и выработку соответствующей реакции (борьба или бегство). В то время как тревога активирует физиологическую и когнитивную стратегическую подготовку к борьбе или бегству, если это необходимо. Этот взгляд на страх и тревогу подтверждается моделями континуума неизбежности хищничества животных, которые предполагают различные режимы (от потенциальной угрозы до обнаружения угрозы, до атаки хищника при нападении), каждый из которых приводит к различным четко определенным моделям защитного поведения.
Эти канонические модели универсальны (хотя ответы зависят от вида) и применимы не только к приматам, но и к людям. Оптогенетические исследования у не приматов показывают, что стимулы, аналогичные угрозам до и после столкновения, вызывают активацию вентромедиальной префронтальной коры, гиппокампа и базолатеральной миндалины – областей, участвующих в запоминании угроз, поиске и предотвращении. В цикле режима атаки активируются средняя поясная кора, центральная миндалина, гипоталамус и периакведуктальное серое вещество – области, участвующие в быстром реагировании на угрозу (например, бегство). Аналогичные защитные схемы существуют и у людей: снимки функциональной магнитно-резонансной томографии (МРТ) показывают, что отдаленная угроза связана с повышенной активностью в вентромедиальной префронтальной коре, и по мере приближения угрозы наблюдается большая активация в периакведуктальном сером веществе среднего мозга. RDoС, в котором используется комплексный подход к психопатологии, опирается на эти модели и предполагает, что “ответы на угрозы с низкой вероятностью качественно отличаются от поведения при высокой вероятности угрозы, которые характеризуют страх”.
В то время как прототипы страха и тревоги находятся в разных “местах” в континууме реагирования, клинические проявления более подвижны. Например, восприятие угрозы может быстро измениться с отдаленного на неизбежное с помощью одних только оценок и образов, без изменения внешних обстоятельств. Примером может служить человек с посттравматическим расстройством, который испытывает страшное воспоминание о травме (т.е. о неминуемой угрозе) в разгар тревоги в незнакомой обстановке (т.е. отдаленная угроза). Тревога и страх проявляются в нескольких сферах: поведенческой, физиологической и субъективных ощущениях. Состояния тревоги обычно сопровождаются бдительным, осторожным и избегающим поведением, физиологической готовностью к серьезной опасности (реакция испуга, мышечное напряжение), заявлениями о беспокойстве или озабоченности, а также ощущением надвигающейся или неопределенной угрозы (например, “Что, если я неправильно произнесу слово на званом обеде на следующей неделе – мне будет так неловко” или “Что, если я упаду в обморок в кинотеатре”). Состояния страха сопровождаются поведением побега (или сражения), возбуждением автономной нервной системы, заявлениями о страхе и испуге и ощущением серьезной угрозы (например, «Я умираю» или «Мне нужно выбираться отсюда»).
Примечательно, что эти способы ответа не всегда совпадают 30 . Например, люди могут сообщать о тревоге или страхе при отсутствии физиологических или поведенческих изменений или могут избегать ситуаций, не испытывая чувств тревоги или страха. Даже во время панических атак люди иногда сообщают о страхе без признаков физиологических изменений 31 . Такое несоответствие может быть информативным для выбора лечения. Например, субъективный дистресс при отсутствии физиологических изменений может указывать на ценность когнитивно-ориентированного подхода к лечению, а не биологически ориентированного (такого как регуляция дыхания или фармакотерапия), а избегающее поведение при отсутствии физиологических изменений может указывать на особую ценность экспозиционной терапии. Однако доказательства такого подбора лечения еще только появляются, поскольку клинические исследования были сосредоточены в первую очередь на конкретных диагнозах и клинических подтипах, а не на детальной оценке конкретного поведения, физиологических параметров или когнитивных оценок.
В клинической практике первым и ключевым шагом в оценке тревоги является постановка диагноза тревожного расстройства на основе профиля симптомов. Диагноз тревожных расстройств у взрослых может быть установлен с помощью клинических интервью. Примерами таких интервью служат: структурированное клиническое интервью для диагностики для DSM-5 (SCID-5) 32 , мини-международное нейропсихиатрическое интервью (MINI) 33 , комплексное международное диагностическое интервью (CIDI) 34 . Интервью по тревоге и связанным расстройствам для DSM-5 (ADIS-5) особенно ориентировано на дифференциальную диагностику тревожных расстройств 35 . Структурированное диагностическое интервью для обсессивно-компульсивных и связанных с ними расстройств может быть полезным для диагностики этих часто упускаемых из виду состояний 36 .
Важно определить, является ли тревожная симптоматика (например, панические атаки) проявлениями другого психического расстройства (например, депрессии или биполярного расстройства). Употребление психоактивных веществ или интоксикация (например, употребление кофеина, стимуляторы) и абстинентный синдром (например, от употребления алкоголя) могут привести к развитию выраженной тревоги. Некоторые медицинские состояния, такие как сердечно-легочные (например, астма), эндокринные (например, заболевание щитовидной железы) и неврологические (например, сложные парциальные припадки) заболевания, также вызывают развитие тревожной симптоматики.
Для выявления тревоги, связанной с заболеваниями, необходимо подробно изучить историю болезни и провести физическое обследование, проанализировать анализы крови (например, уровень тиреотропного гормона) и результаты инструментальных методов диагностики (например, электрокардиография или электроэнцефалография). Хотя структурные (например, воксель-базированная морфометрия) и функциональная МРТ использовались для изучения патофизиологии тревожных расстройств, в настоящее время они не используются в диагностических целях 11,12 .
Данные о недостаточной эффективности диагностики и лечении тревожных расстройства подчеркивают важность скрининга симптомов тревоги 37 . Опросник генерализованного тревожного расстройства-7 (GAD-7) 38 – это опросник, состоящий из 7 пунктов, который был разработан специально для ГТР, но оказался полезен для выявления любого тревожного расстройства с адекватной чувствительностью и специфичностью 39 . Другие инструменты скрининга включают больничную шкалу тревоги и депрессии 40 и шкалу общей степени тяжести тревоги (OASIS) 41 , которая включает измерение выраженности избегающего поведения (важная особенность, поскольку уровни тревожности могут быть замаскированы без такого измерения). Шкала Перинатального Скрининга Тревожности подходит в качестве неспецифического скринера для женщин в перинатальном периоде 42 .
Если присутствует тревога или связанное с ней расстройство, можно использовать несколько показателей для оценки профиля тревожной симптоматики. Интервью для определения симптомов настроения и тревоги оценивает все симптомы эмоциональных расстройств по DSM и МКБ, а также другие проявления интернализующей психопатологии 43 . Каждый пункт оценивается от явно отсутствующего до частично присутствующего (субклинический, подпороговый) и четко присутствующего, что позволяет оценить баллы профиля симптомов. Помимо интервью, существуют анкеты самооценки для каждого тревожного и родственного расстройства, которые предоставляют более подробные профили симптомов. К ним относятся шкалы DSM-5, разработанные для агорафобии, ГТР, ОКР, ПТСР, социального тревожного расстройства и специфической фобии, каждая из которых включает элементы для аффективных состояний страха и тревоги, физиологических, когнитивных и поведенческих симптомов 44 . Было показано, что, за исключением специфической фобии, эти шкалы обладают адекватными сильными психометрическими свойствами 45-52 .
Существует ряд других хорошо проверенных стандартизированных опросников по симптомам. Они включают Пенсильванский опросник для оценки уровня беспокойства 53 для ГТР; обсессивно-компульсивную шкалу Йеля-Брауна (Y-BOCS) 54 для ОКР; опросник паники и фобии Олбани для агорафобии 55 ; опросник мобильности для агорафобии 56 ; шкалу тяжести панического расстройства 57 и шкалу паники и агорафобии 58 для панического расстройства и агорафобии; Опросник посттравматического стресса для DSM-5 (PCL-5) 59 и Шкалу клинической оценки посттравматического стрессового расстройства для DSM-5 (CAPS-5) 60 для посттравматического стрессового расстройства; и «Опросник социальной фобии и тревоги» 61 и «Шкалу социальной тревожности Либовица 62 » для определения социальной фобии. Не существует шкал для каждого типа конкретной фобии, но в этом случае можно использовать Шкалу Оценки Страхов (FSS)63, анкету из 51 пункта, в которой респондентам предлагается указать свой дискомфорт или чувство тревоги по каждому из 51 стимула.
Дифференциальная диагностика тревожных расстройств может помочь клиницисту подобрать более эффективную терапию. Конкретные варианты когнитивно-поведенческой терапии (КПТ) ориентированы на конкретные тревожные расстройства. Имеются существенные доказательства эффективности таких целевых методов лечения 64-66 , и они рекомендуются в качестве психологических методов лечения тревоги и связанных с ней расстройств первой линии в нескольких руководящих организациях, в том числе в Национальном институте здравоохранения и передового опыта Великобритании (NICE) 67 . Например, КПТ для панического расстройства включает в себя интероцептивное воздействие на телесные ощущения, вызывающие страх; КПТ для социального тревожного расстройства включает когнитивную реструктуризацию вокруг размышлений после события; КПТ для генерализованного тревожного расстройства рассматривает метаубеждения о беспокойстве; КПТ для ОКР включает воздействие специфических сигналов, которые вызывают дистресс и побуждение выполнять навязчивые ритуалы, а также профилактику реагирования, направленную на устранение навязчивых состояний; и КПТ для ПТСР включает воздействие воображения или когнитивную переработку в отношении воспоминаний о травме. Таким образом, дифференциальная диагностика облегчает выбор наиболее подходящей формы психотерапии. Даже при использовании трансдиагностической КПТ, многообещающего подхода, ориентированного на конкретные расстройства 68 , клиницисту все равно потребуется реализовывать терапевтические стратегии таким образом, чтобы они учитывали направленность страхов и фобий каждого человека.
С точки зрения фармакотерапии СИОЗС продемонстрировали эффективность при всех основных тревожных и связанных с ними расстройствах. Тем не менее важно дифференцировать различные расстройства по нескольким причинам. Во-первых, рекомендации по фармакотерапии СИОЗС различаются в зависимости от различных тревожных и связанных с ними состояний 69 . Так, например, особенно важно начинать с более низких доз СИОЗС при паническом расстройстве (поскольку стандартные дозы могут быть непереносимы), в то время как более высокая доза и более длительная продолжительность лечения требуются при ОКР. Во-вторых, препараты, отличные от СИОЗС, обладают разной эффективностью при различных тревожных состояниях и связанных с ними расстройствах 69 . Так, например, трициклический антидепрессант имипрамин эффективен при некоторых тревожных и связанных с ними расстройствах (например, ГТР, паническое расстройство, ПТСР), но не при других (ОКР, социальное тревожное расстройство). Бензодиазепин алпразолам эффективен при различных тревожных расстройствах (ГТР, паническое расстройство, социальное тревожное расстройство), но не при расстройствах, связанных с тревогой (ОКР и ПТСР). Буспирон эффективен при ГТР, но не при других тревожных и связанных с ними расстройствах, в то время как ОКР представляется уникальным среди этих состояний, поскольку он более чувствителен к серотонинергическим, чем к норадренергическим ингибиторам обратного захвата 69 .
Повысить эффективность лечения может помочь сопоставление терапии с кластерами симптомов, учитывая неоднородность, существующую в диагностических метках. Действительно, есть свидетельства того, что клиницисты уже рассматривают кластеры симптомов как более информативные для выбора фармакотерапии в сравнении с диагностическими категориями 70,71 . Например, в выборке из 318 пациентов диагноз ПТСР не был связан с назначением какого-либо конкретного класса лекарств, препараты подбирались по кластеру симптомов: назначение противосудорожных средств было связано с симптомами избегания, назначение антидепрессантов связано с состоянием оцепенения, назначению анксиолитиков при тревоге и назначение стабилизаторов настроения при гипервозбуждении 71 . Аналогичным образом, при паническом расстройстве анксиолитики чаще назначались при физических симптомах реакции страха, тогда как антидепрессанты и противосудорожные средства назначались при психологических симптомах. Аналогичное соответствие класса лекарств с кластерами симптомов было найдено для агорафобии, ОКР, социального тревожного расстройства и специфической фобии. Очевидно, что профиль симптомов определяет текущий выбор фармакотерапии врачами, и область персонализированной медицины будет расширена за счет рандомизированных контролируемых исследований для подтверждения (или нет) такого соответствия профиля симптомов лекарственным средствам.
Тот же аргумент справедлив и для психотерапии, которая была поставлена в тупик использованием методик КПТ (например, дыхательные техники, когнитивная реструктуризация, экспозиционная терапия, профилактика ответных реакций) без учета кластеров симптомов. Были призывы сопоставить основные активные методы терапии с конкретными профилями симптомов (например, дыхательные техники для регуляции возбуждения, когнитивная реструктуризация для когнитивных искажений, терапия воздействия для предотвращения) 72,73 . Это остается важной областью будущих исследований. Тем не менее вполне возможно, что практикующие клиницисты уже адаптируют основные компоненты КПТ к проявлениям симптомов точно так же, как это наблюдается при фармакотерапии.
КЛИНИЧЕСКИЕ ПОДТИПЫ
Каждое из тревожных и связанных расстройств характеризуется значительной неоднородностью, из-за чего и были выделены несколько клинических подтипов. Содержание страха или беспокойства (когнитивный компонент), физиологических реакций (таких как паническая атака) и поведенческой реакции (которая часто включает избегающее поведение и может включать опасливое поведение) может быть полезным при определении наличия или отсутствия определенного клинического подтипа. Кроме того, был принят ряд других подходов к подтипам, в том числе в зависимости от возраста начала и сопутствующих симптомов. Здесь мы рассматриваем основные клинические подтипы ключевых тревожных расстройств.
При ГТР полезно оценить как природу беспокойства, так и диапазон психических (психологических) и соматических (физические) симптомов. Беспокойство может быть сосредоточено на смерти (например, кто-то не звонит, когда он сказал, что предпочел бы умереть), болезни (например, «головная боль означает, что у меня опухоль мозга»), разрушении (например, «протечка в потолке означает, что нужна новая крыша, и если я не сделаю ее вовремя, мой дом будет разрушен»), а иногда на нищете (например, «Если я одолжу сестре деньги, она никогда не перестанет просить, и я разорюсь»). Такие инструменты, как Пенсильванский опросник для оценки уровня беспокойства 53 , оценивают направленность беспокойства у пациентов ГТР, в то время как психические и соматические подшкалы шкалы оценки тревожности Гамильтона (HAM-A) 74 полезны для оценки спектра симптомов.
Понимание точной природы страха важно для КПТ, которая может сосредоточиться на когнитивной реструктуризации конкретных беспокойств или подверженности определенным видам страхов. С точки зрения фармакотерапии ранее считалось, что трициклические антидепрессанты более полезны при психических симптомах, в то время как бензодиазепины более полезны при соматических симптомах 75 . Тем не менее было относительно мало последующих доказательств, подтверждающих избирательную реакцию психических и соматических симптомов на различные методы фармакотерапии. Ряд лекарств, эффективных при ГТР, влияют как на психические, так и на соматические симптомы 76-79 .
Что касается ОКР, в значительной части литературы подчеркивается, что навязчивые идеи и компульсии, как правило, имеют несколько симптомов, включая мытье, проверку безопасности, упорядочивание предметов и накопительство 80 . Хотя у многих пациентов есть симптомы, которые лежат в разных измерениях, или они испытывают целый ряд симптомов, меняющихся с течением времени, есть некоторые свидетельства того, что плоскость проявления симптомов связана с конкретными психобиологическими характеристиками и может влиять на результаты лечения. В частности, симптомы накопления с меньшей вероятностью будут реагировать на СИОЗС. Необходима дальнейшая работа, чтобы определить, могут ли пациенты с патологическим накопительством, которые не реагируют на СИОЗС, реагировать на дополнение терапии антагонистами дофамина 81 .
Диагноз ОКР может быть установлен на основании опроса пациента о последствиях отказа от навязчивых действий и оценки вероятности того, что ожидаемые последствия действительно произойдут. Возможно, будет полезно спросить пациента, могут ли возникнуть последствия, которых он опасается, для кого-то другого, чтобы оценить их мыслительный процесс без влияния их собственного беспокойства по поводу невыполнения принуждений. ОКР может быть формально оценено с помощью шкалы оценки убеждений Брауна 82 . Пациенты с ОКР с формальной критикой к своему состоянию реже обращаются к психиатру, и могут хуже реагировать на фармакотерапию и психотерапию 83 . Таким пациентам могут потребоваться дополнительные вмешательства, такие как семейная психотерапия 84 и антагонисты дофамина 85 .
Если у пациентов с ОКР есть текущие или прошлые тики, важно определить, являются ли компульсии похожими на тики (например, прочищение горла) или направлены на снижение тревоги (например, мытье рук после ощущения загрязнения). ОКР, связанное с тиками, характеризуется рядом особенностей, включая раннее начало, чаще возникает у мужчин, семейный анамнез тиков и чаще наличие симптомов, связанных с реакцией на раздражитель (или предчувствие сенсорных симптомов) или перфекционизмом. Тяжесть тика может быть формально оценена с помощью ряда мер 86 . Тикоподобные компульсии плохо реагируют на стандартную терапию и могут лучше реагировать на аугментацию антагонистами дофамина 83 .
Был предложен ряд других подтипов ОКР, включая ОКР с ранним началом 83 . Хотя такая работа была полезна для лучшего понимания гетерогенности ОКР, нет достаточных доказательств того, что такое подтипирование имеет клиническую ценность.
Что касается панического расстройства, было обнаружено, что различные панические симптомы могут объединяются в несколько кластеров, включая респираторные, ночные, когнитивные и вестибулярные симптомы 31 . Исследование физиологии дыхания при паническом расстройстве было особенно полезно для углубления понимания нейробиологии этого состояния 87 . Тем не менее нет убедительных доказательств того, что какой-либо из этих подтипов обладает особой психобиологией, равно как и нет убедительных доказательств того, что какой-либо из них обладает избирательным ответом на лечение 88 . Однако возможно, что более обширное исследование приведет к более конкретным рекомендациям по лечению подтипов панического расстройства.
ПТСР диагностируется в DSM-5 с использованием двадцати симптомов, которые делятся на 4 подгруппы, а именно: навязчивое повторное переживание события (5 симптомов), избегающее поведение (два симптома), нарушения когнитивных процессов и эмоционального состояния (7 симптомов) и изменения в возбуждении и реактивности нервной системы (6 симптомов). Хотя уже давно было высказано предположение, что различные проявления ПТСР подкрепляются различными нейробиологическими механизмами 89,90 , похоже, что существуют сильные генетические корреляции между группами симптомов ПТСР и что эффективная фармакотерапия ПТСР уменьшает выраженность симптомов из различных групп 91 . Как отмечалось ранее, назначение противосудорожных препаратов было связано с избегающим поведением, антидепрессантов – с симптомами оцепенения, анксиолитиков – с интрузиями, а стабилизаторов настроения – с гипервозбуждением 71 , но необходима дальнейшая работа для наработки доказательной базы для принятия таких решений.
Была выдвинута гипотеза о существовании диссоциативного подтипа ПТСР с характерной нейробиологией 92 . Этот подтип может характеризоваться чрезмерной модуляцией аффекта, а не его демодуляцией с повторным переживанием и симптомами гипервозбуждения. Большинство клиницистов оценивают диссоциацию по психиатрическому анамнезу, но может быть полезно использовать формальный инструмент, такой как Шкала диссоциативных переживаний (DES) 93 . DES-II – это самоопросник по 28 пунктам, который оценивает частоту диссоциативных переживаний в повседневной жизни, при этом баллы выше 30 считаются высокими 94 .
Запись сеансов лечения для последующего просмотра может быть полезна для пациентов с симптомами диссоциации, а также частые приостановки, перерывы, более медленное продвижение к содержанию психотравмирующего события, чтобы не перегружать пациента. Кроме того, в соответствии с гипотезой о том, что диссоциация связана с избеганием, есть доказательства того, что при наличии диссоциации когнитивная процессинговая терапия должна включать компонент экспозиции 95 . Конструкция "комплексного ПТСР" по МКБ-11 характеризуется повышенным уровнем ранней детской травмы и диссоциативных симптомов, но необходима дальнейшая работа, чтобы определить, какие конкретные вмешательства улучшат результаты при этом состоянии 96 .
В DSM-IV диагноз социальное тревожное расстройство ставился на основании более обобщенных критериев, относящихся к пациентам с более широким спектром социальных страхов. В DSM-5 был введен диагноз социофобия, для которого характерен страх преимущественно перед публичными выступлениями. Существует мнение, что социальное тревожное расстройство варьируется от страха перед конкретной ситуаций до обширного спектра ситуаций, вызывающих страх, и что болезнь у пациентов с большим спектром страхов протекает тяжелее, и что такие пациенты хуже реагируют на терапию 97 . Предварительные результаты исследований показывают, что пациенты с социальным тревожным расстройством могут реагировать на бета-адреноблокаторы (такие как пропранолол или атенолол) 98 .
С другой стороны, СИОЗС могут быть полезны пациентам с любой степенью тяжести социального тревожного расстройства 99 . Когнитивно-поведенческая терапия, по-видимому, эффективна при всех типах социальной тревожности.
Специфические фобии включают тип “животные” (например, пауки, насекомые, собаки), тип "кровь-инъекция-травма" (например, иглы, инвазивные медицинские процедуры), тип “естественная среда” (например, высота, шторм, вода), ситуационный тип (например, самолеты, лифты, закрытые помещения) и «прочие» типы (например, фобическое избегание ситуаций, которые могут привести к удушью, рвоте или заражению болезнью). Экспозиционные техники (техники воздействия?), адаптированные к конкретным фобиям, полезны для этого диапазона типов специфических фобий.
В отличие от других фобий, которые приводят к стойкой тахикардии в ответ на пугающие сигналы, при типе "кровь-инъекция-травма" у некоторых пациентов может наблюдаться дифазная реакция с начальным повышением частоты сердечных сокращений, за которым следует вазовагальная брадикардия и, в некоторых случаях, обморок 100,101 . Если пациенты теряют сознание при воздействии сигналов, экспозиционную терапию можно проводить в положении пациента лежа. Может быть полезно обучение пациентов технике изометрического напряжения мышц, которая может помочь повысить артериальное давление во время воздействия на них сигналов, которых они опасаются 102 .
Ситуативный тип специфической фобии часто пересекается с агорафобией и/или паническим расстройством и поэтому обычно требует когнитивных методов в дополнение к воздействию.
ТЯЖЕСТЬ
Оценка тяжести симптомов тревоги является важным компонентом обследования пациентов с тревогой или связанными с ней состояниями.
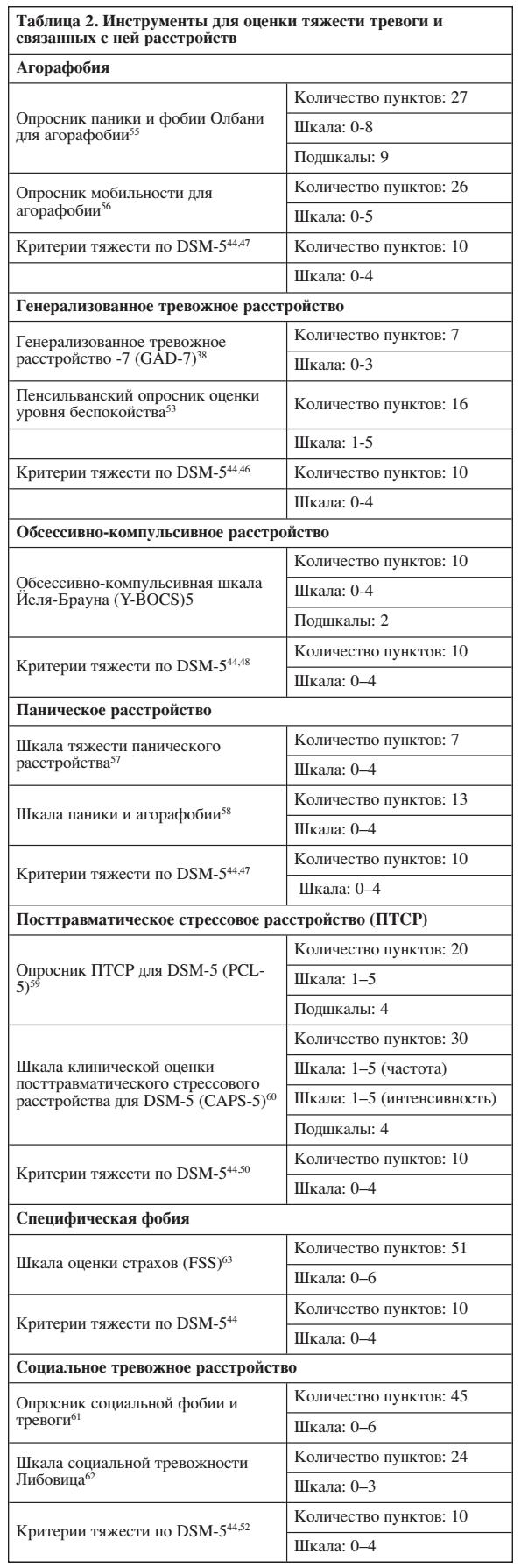
В DSM-5 включены критерии тяжести симптомов для каждого из тревожных и связанных с ними расстройств, а некоторые стандартизированные показатели симптомов широко используются в клинической практике и исследованиях. К ним относятся GAD-7 38 и Пенсильванский опросник оценки уровня беспокойства 53 для ГТР; Y-BOCS54 для ОКР (Обсессивно-компульсивная шкала Йеля-Брауна); шкала тяжести панического расстройства 57 и шкала паники и агорафобии 58 для панического расстройства; опросник мобильности для агорафобии 56 и Олбанский опросник паники и фобии 55 для агорафобии; PCL-5 59 и CAPS-5 60 для ПТСР; программа обследования страхов 63 для специфических фобий; опросник социальной тревоги и социофобии 61 и шкала социальной тревожности Либовица 62 для социофобии (Таблица 2).

Измерение тяжести симптомов тревоги полезно по ряду причин. Во-первых, учет всего спектра тяжести симптомов актуален для моделей предоставления лечения, основанных на ступенчатом подходе. Стратифицированная ступенчатая помощь предлагает менее интенсивное лечение (например, цифровую терапию) тем, у кого симптомы менее выражены, в то время как тем, у кого симптомы более выражены, предлагается более интенсивное лечение 103-105 . Интенсивные подходы, включая посещение на дому или госпитализацию, могут быть необходимы при агорафобии, когда пациенты не могут покинуть свой дом, для пациентов с ОКР, когда ритуалы делают их дома небезопасными или препятствуют посещению клиники, или когда они страдают тяжелым пренебрежением к себе в результате своих симптомов, или для пациентов с ПТСР, у которых настолько тяжелые симптомы, что они не могут посещать сеансы амбулаторного лечения.
Во-вторых, определение тяжести симптомов во время лечебных визитов помогает направлять врача и пациента, позволяя им реагировать на утяжеление симптомов и положительно влиять на результаты лечения 106,107 . Были внедрены практические подходы к лечению тревоги как у взрослых, так и у детей на основе шкал, и это обещает способствовать улучшению персонализированного ухода и повышению эффективности лечения 108,109 .
В-третьих, клинические рекомендации по лечению тревожных расстройств могут рекомендовать выбор лечения в зависимости от тяжести симптомов. Это согласуется с высказанным выше замечанием о том, что легкие симптомы могут поддаваться менее интенсивному лечению, в то время как более тяжелые симптомы могут потребовать более интенсивной терапии, включая использование более одного метода лечения.
Тяжесть ГТР может быть оценена с помощью GAD-7 (самоопросник) и оценочной шкалы тревоги Гамильтона (интервью). В GAD-7 баллы 5, 10 и 15 могут быть интерпретированы как обозначающие легкий, умеренный и тяжелый уровни тревоги: увеличение баллов по шкале тесно связано с ухудшением функциональных нарушений и увеличением числа дней нетрудоспособности 39 . В шкале Гамильтона баллы 9, 15 и 24 могут быть интерпретированы как представляющие нижние границы пограничного, легкого и умеренного уровня тревоги соответственно 110 . Увеличение тяжести симптомов линейно связано с увеличением функциональных нарушений в трех областях шкалы инвалидности Шихана (см. ниже) 111 .
Гайдлайн Национального института здравоохранения и совершенствования медицинской помощи Великобритании (NICE) по ведению пациентов с ГТР рекомендует при легкой степени тяжести тревоги первоначально провести период активного мониторинга, так как симптомы часто проходят без необходимости вмешательства. Если симптомы не исчезли после периода активного наблюдения, следует предложить низкоинтенсивные психологические вмешательства (по существу, самопомощь или психолого-педагогические подходы). При наличии выраженных функциональных нарушений или когда симптомы не устраняются с помощью низкоинтенсивных психологических вмешательств, следует предлагать либо высокоинтенсивные психологические вмешательства (КПТ или прикладная релаксация), либо медикаментозное лечение (обычно СИОЗС), в зависимости от пожеланий человека 112 .
При ОКР тяжесть симптомов может быть оценена с помощью Y-BOCS: у взрослых баллы 14, 26 и 35 могут указывать на нижние пределы умеренной, среднетяжелой и тяжелой интенсивности симптомов соответственно 113 . Увеличение тяжести симптомов, как правило, связано с увеличением уровня инвалидности. Тяжесть симптомов является одним из нескольких важных клинических факторов, которые следует учитывать при выборе лечения 69 . Некоторые гайдлайны указывают, что тяжесть влияет на выбор между фармакотерапией и психотерапией (например, психотерапия является первой линией вмешательства при легкой форме ОКР, а фармакотерапия применяется, когда КПТ не эффективна) 114 , другие гайдлайны указывают, что фармакотерапия и психотерапия могут использоваться независимо от уровня тяжести симптомов при ОКР 69 .
При посттравматическом расстройстве оценка тяжести симптомов может быть сложной, так как требуется комплексно оценить расстройства различных отделов организма. Наиболее широко используемым показателем тяжести симптомов является Шкала клинической оценки посттравматического стрессового расстройства для DSM-5 60 , которая включает 30 пунктов, оценивающих тяжесть симптомов за предыдущую неделю. Пациенты с ПТСР с тяжелыми симптомами могут испытывать больше трудностей во время когнитивно-поведенческой терапии. Однако интенсивные амбулаторные программы, в которых ежедневно участвуют пациенты с ПТСР, могут увеличить показатели удержания до 90% 115,116 , с соответствующим уменьшением как симптомов ПТСР, так и суицидальных мыслей 117 .
НЕЙРОКОГНИЦИЯ
Нейрокогниция представляет собой один из ключевых механизмов, с помощью которого изменения в структуре и функциях мозга в конечном итоге приводят к появлению клинических признаков и симптомов. Находясь ближе к предполагаемому биологическому субстрату и будучи измеримыми с помощью объективных тестов, нейрокогнитивные маркеры могут быть более надежными, последовательными и устойчивыми, чем изменчивая симптоматика расстройства 118-120 . Нейрокогнитивное тестирование у пациентов с ОКР и связанными с ним расстройствами, например, использовалось для характеристики аномалий лобно-височных долей 121 , а также для выявления предполагаемых подтипов с различной структурой мозга, функциями 122 .
Клиническая оценка нейрокогнитивных способностей при тревоге и связанных с ней расстройствах получила импульс благодаря разработке более надежных нейрокогнитивных тестов с адекватной специфичностью и чувствительностью для областей, имеющих отношение к этим состояниям, а также благодаря технологическим достижениям, использование компактных компьютеризированных батарей, которые относительно дешевы и просты в применении с небольшой нагрузкой на пациентов и персонал. Такое тестирование может способствовать оценке и диагностике, а также может использоваться для мониторинга эффективности лечения (хотя некоторые нейрокогнитивные нарушения, по-видимому, не изменяются, когда симптомы реагируют на вмешательство, представляя собой маркеры уязвимости кандидатов, которые также встречаются у бессимптомных родственников первой степени у таких пациентов) 8,123 .
Когнитивные тесты чаще используются при ОКР, чем при других тревожных расстройствах. В систематическом обзоре и метаанализе статей о биомаркерах-кандидатах для ОКР только когнитивные показатели показали убедительные или весьма убедительные подтверждающие результаты (доказательства класса 1 или 2) 124 . Кроме того, оценка с использованием стандартизированных инструментов самоотчета, таких как Инструмент когнитивной оценки навязчивых идей и компульсий (CAIOC-13) 125 , шкала из 13 пунктов, показывает широкий спектр функциональных нарушений при ОКР, которые, как считается, являются следствием когнитивных трудностей, которые мешают многим аспектам повседневной жизни. Поскольку эти недостатки легко упускаются из виду, недавнее экспертное исследование рекомендовало рутинную когнитивно-функциональную оценку с использованием таких шкал, как CAIOC-13, в клинической оценке для пациентов с ОКР 126 .
В будущем есть надежда, что нейрокогнитивное тестирование может быть использовано для выявления тревожных расстройств даже до появления симптомов 126 и для априорного прогнозирования реакции на лечение, улучшения эффективности терапии 124 . Оценка когнитивной негибкости, вероятно, будет иметь особое значение для прогнозирования результатов лечения ОКР. Тем не менее доказательства остаются весьма предварительными, и лишь в нескольких небольших исследованиях ОКР показан общий или дифференциальный ответ на фармакотерапию или КПТ в зависимости от степени когнитивной гибкости при выполнении задач по смене заданий 127 .
ФУНКЦИОНИРОВАНИЕ И УРОВЕНЬ ЖИЗНИ
Оценка функционирования и качества жизни пациентов с тревожными расстройства важна по нескольким причинам, рассмотренным в предыдущем разделе о тяжести симптомов. Во-первых, влияние расстройства на эти области помогает определить, следует ли использовать стандартное амбулаторное лечение или требуются более интенсивные подходы. Во-вторых, оценка функционирования и качества жизни является частью медицинской помощи, основанной на измерениях. Имеются убедительные доказательства того, что лечение тревоги и связанных с ней расстройств позитивно влияет на функционирование и повышает уровень жизни 128 . В-третьих, рекомендации по лечению тревожных расстройств могут частично основываться на степени функциональных нарушений. Хотя тяжесть симптомов, функциональные нарушения и качество жизни демонстрируют значительные корреляции, важно отметить, что у любого конкретного пациента они могут быть не полностью согласованы, и, следовательно, каждая конструкция нуждается в независимой оценке 129,130 .
Согласно Всемирной организации здравоохранения, качество жизни – это восприятие индивидом своего положения в жизни в контексте культуры и систем ценностей, в которых он живет, и в соответствии с его целями, ожиданиями и проблемами. Таким образом, оценку качества жизни можно отличить от измерения функциональных нарушений и инвалидности, связанной с симптомами, по ее направленности на субъективное переживание удовлетворенности текущим функционированием и сопутствующее чувство общего благополучия.
Оценка качества жизни в идеале должна охватывать как общие, так и конкретные показатели, чтобы обеспечить максимальную чувствительность и обобщаемость. Однако исследования тревожных расстройств, ПТСР и ОКР в основном использовали общие инструменты. Наиболее часто использовались шкала инвалидности Шиэна 131 , Опросник качества жизни и удовлетворенности (Q-LES-Q) 132 и Исследование медицинских результатов по 36 пунктам Краткой формы обследования здоровья (SF-36) 133 , при этом также использовались EuroQol (EQ-5D) 134 и Инвентаризация качества жизни (QOLI) 135 . Шкалы, специфичные для расстройств, включают CAIOC-13 125 для ОКР и обследование здоровья ветеранов Rand 12 (VR-12) для ПТСР 136 .
Некоторые клинические рекомендации по лечению тревоги и связанных с ней расстройств были сосредоточены на функциональных нарушениях. В рекомендациях NICE по ОКР, например, предлагается психологическое лечение низкой интенсивности для пациентов с легкими функциональными нарушениями (или когда пациент предпочитает этот вид лечения), в то время как СИОЗС или более интенсивная КПТ предлагаются в случае умеренных функциональных нарушений 137 .
ЛИЧНОСТНЫЕ ЧЕРТЫ
Среди “классических” черт пятифакторной (Большой пятерки) модели личности, нейротизм, который относится к негативной эмоциональности или стойкой склонности к готовности испытать сильные негативные эмоции, показал наиболее устойчивую связь с тревожностью 138 . Невротизм был связан с усилением симптомов общей тревоги, а также симптомов ОКР, панического расстройства, фобий, ПТСР и социального тревожного расстройства. Согласно трехсторонней модели Clark и Watson 139 , нейротизм является основным фактором риска, общим для тревожных и депрессивных расстройств, при этом дополнительный компонент тревожного возбуждения более специфичен для тревожных состояний, а ангедония более характерна для депрессии 140 .
В клиническом контексте понимание степени и истории негативной эмоциональности пациента как фактора уязвимости может помочь контекстуализировать начальное возникновение и поддержание симптомов тревоги. Если нейротизм влияет на текущее преодоление и функционирование, например, усиливая тревогу и связанные с ней расстройства, его уровни могут быть снижены с помощью психологических методов лечения, основанных на принятии и когнитивно-поведенческих подходах, которые специально нацелены на реакцию на негативные эмоции 141 .
Еще одна черта личности из Большой пятерки, экстраверсия, которая относится к общительности и склонности черпать энергию из взаимодействия с другими, имеет клиническое значение для понимания некоторых тревожных расстройств, включая агорафобию, специфическую фобию и социальное тревожное расстройство 138 . Было обнаружено, что социальная тревожность генетически коррелирует со снижением экстраверсии, но не с нейротизмом 142 . Знание уровня экстраверсии пациента может быть особенно полезным при информировании о лечении социальной тревожности, например, при выборе иерархии социальных воздействий.
Пациенты с генерализованной тревожностью, как правило, имеют более высокий уровень ответственности в сравнении со средним 143 . Высокая ответственность может создать как возможности, так и проблемы для соблюдения режима лечения в ходе психотерапии тревожного или связанного с ним расстройства. Это может привести к более высокому уровню выполнения терапевтических домашних заданий, но также к большему беспокойству и озабоченности по поводу назначенных практик или задач. В последнем случае клинические рассуждения предполагают, что может быть полезно четкое обсуждение реалистичных ожиданий и нормализации постепенного прогресса. Высокий уровень ответственности также может указывать на возможность наличия в основе обсессивно-компульсивного расстройства личности и потенциальную ценность методов лечения, разработанных для этого состояния 144 .
В некоторой литературе указывается, что Пять основных личностных черт лучше всего рассматривать в сочетании, когда дело касается тревожных расстройств, при этом более высокие уровни экстраверсии и сознательности связаны с более низким риском развития тревожных расстройств среди лиц с высоким уровнем нейротизма 145 . В соответствии с этим, более высокие уровни ответственности были связаны с более быстрым восстановлением от негативных эмоций у взрослых 146 , возможно, смягчая последствия невротизма.
Таким образом, клиницист должен обращать внимание на различные комбинации Пяти личностных черт. Если пациент демонстрирует высокий невротизм, но низкую ответственность, он/она может подвергаться особому риску возникновения трудностей с регулированием эмоций и, таким образом, эффективнее могут быть стратегии, направленные на улучшение регуляции эмоций, например, диалектическую поведенческую терапию. Напротив, пациент с высоким нейротизмом, но также с высокой экстраверсией и ответственностью может извлечь выгоду из стандартных стратегий, таких как когнитивная реструктуризация или воздействие. Однако необходимы дальнейшие исследования, чтобы установить, могут ли рекомендации по лечению основываться на оценке Пяти основных признаков.
С точки зрения того, как клиницист должен оценивать личностные черты у тревожного пациента, оценка Пяти основных черт характера была предметом растущего внимания, и доступен ряд проверенных шкал, таких как Инвентаризация личности NEO-3 147 и Инвентаризация Большой пятерки-2 148 . Однако, поскольку эти шкалы являются относительно длинными, клиницисты могут счесть полезным выбрать наиболее релевантные поддомены – такие как нейротизм – для оценки или использовать краткие шкалы личностных качеств (например, Десятибалльный показатель Личности 149 ). При оценке личности клиницисты должны учитывать потенциальные двунаправленные влияния между личностными чертами и тревогой, поскольку наличие тревоги или связанного с ней расстройства может повлиять на переживание и сообщения о невротизме с течением времени 150 .
Важно отметить, что каждая из Пяти основных личностных черт, как предполагается, состоит из “аспектов”, которые в дальнейшем могут оказаться полезными для понимания развития и поддержания симптомов у пациентов с тревожностью. Например, недавние усилия по изучению аспектов личности в рамках нейротизма выявили 5 потенциальных поддоменов, включая тревогу, депрессию, склонность к гневу, соматические жалобы и зависть 151 . Детальная оценка личностных аспектов может указывать на конкретные цели вмешательства, которые могут быть продуктивными в ходе психотерапии, такие как решение соматических проблем с помощью стратегий "разум-тело" или снижение уровня тревоги с помощью когнитивно-поведенческих методов.
Наконец, личностные черты могут проявляться в форме расстройств личности, как описано в DSM-5. В частности, расстройства личности кластера С могут быть чрезмерно представлены у пациентов с тревожными расстройствами: они включают избегающее расстройство личности (характеризующееся социальным торможением и чувствительностью к отвержению); зависимое расстройство личности (характеризуется тревогой разлуки и пассивным поведением); и обсессивно-компульсивное расстройство личности (характеризуется сильной потребностью в порядке и контролем). Расстройства личности кластера С, которые сочетаются с тревогой и связанными с ней расстройствами, могут усложнить лечение, например, мешая проведению лечения в случае избегающего расстройства личности или приводя к чрезмерной зависимости в случае зависимой личности. Эти расстройства личности могут быть оценены с помощью Описи личности для DSM-5 (PID-5) 152 .
ПРЕДШЕСТВУЮЩИЕ И СОПУТСТВУЮЩИЕ ПСИХИАТРИЧЕСКИЕ НАРУШЕНИЯ
Многие люди, страдающие тревожными расстройствами, имеют сопутствующие психические заболевания 153 . Тревожные расстройства занимают относительно центральное место в многомерной области психопатологии 154 , и имеются данные о наличии связи между этими расстройствами и другими психическими расстройствами, особенно с депрессией. Как отмечалось ранее, некоторые рассматривают тревожные и депрессивные расстройства как проявления общей интернализующей психопатологии, которую можно далее разделить на расстройства страха (например, паника, фобия) и дистресса (например, ГТР, ПТСР, депрессия) 155 .
Некоторые авторы выразили озабоченность по поводу того, что сопутствующая патология может быть артефактом наших современных диагностических систем 156 , которую лучше рассматривать как отражение тяжести и/или масштабов основной проблемы, а не как коморбидное возникновение заболеваний. Такая перспектива может подчеркнуть необходимость измерения трансдиагностических конструктов, таких как нейротизм. Примечательно, что в DSM-5 наличие панических атак теперь используется в качестве общего спецификатора (например, социальная тревога с паническими атаками или без них) и может быть полезно для сигнализации тяжести различных расстройств.
Средний возраст начала тревожных расстройств наступает раньше, чем у многих других психических расстройств, что приводит к вопросу о том, как часто тревожные расстройства предшествуют сопутствующим заболеваниям. В Всемирном Исследовании психического здоровья (World Mental Health Survey) был выявлен очень ранний средний возраст начала (7–14 лет) для тревоги сепарации и специфической фобии, в то время как ГТР, паническое расстройство и ПТСР имели гораздо более поздний возраст начала (24–50 лет). Тем не менее в большинстве пар сопутствующих заболеваний тревожные расстройства либо сопутствуют, либо предшествуют другому расстройству. Наиболее четкая картина наблюдается в отношении специфической фобии: она возникает первой в 75% пар сопутствующих заболеваний 153 . С этой точки зрения раннее распознавание и лечение тревожных расстройств могут быть ключевыми для предотвращения развития последующих психических заболеваний 157 . Необходимы дальнейшие исследования, чтобы определить, предотвращает ли лечение специфической фобии возникновение более поздних психиатрических состояний 158 .
Для оценки сопутствующей патологии можно использовать несколько диагностических интервью. SCID-5 полезен, но его проведение занимает около 90 минут и требует значительной подготовки. MINI проводится быстрее, но имеет недостаток в том, что он полностью структурирован. DSM-5 включает “сквозные” показатели симптомов, которые могут быть полезны при скрининге на целый ряд сопутствующих заболеваний. Опросник психиатрического диагностического скрининга (PDSQ) 159 охватывает многочисленные психические расстройства, включая настроение, тревогу, злоупотребление психоактивными веществами, пищевые и соматоформные расстройства.
У людей с тревожным расстройством выявление других психических состояний является ключевым фактором в персонализации ведения. Если эти два состояния считаются независимыми, то оба, скорее всего, потребуют независимого лечения. Если они взаимозависимы, то в игру вступают 5 основных моделей 6 .
Во-первых, последовательная модель: например, у пациента с социальным тревожным расстройством и расстройством, связанным с употреблением психоактивных веществ, стабилизация расстройства, связанного с употреблением психоактивных веществ, может быть приоритетом перед коррекцией тревожного расстройства. Во-вторых, иерархически взвешенная модель (одно лечение может устранить основной фактор, такой как нейротизм, и, таким образом, улучшить сопутствующие заболевания): например, СИОЗС и/или КПТ могут быть полезны при сопутствующих состояниях тревоги и депрессии. В-третьих, модель, взвешенная по степени тяжести (лечение первичного тревожного состояния может исправить любые вторичные состояния или последствия): например, если панические атаки приводят к агорафобии, то лечение, направленное на панические атаки, может быть первым шагом к терапии агорафобии. В-четвертых, модель “мотивационного обхода”: например, человек с пограничным расстройством личности, приводящим к сильной тревоге, может быть не мотивирован проходить психотерапию, но может быть готов принимать лекарства от тревоги, что также может оказать положительное влияние на импульсивные черты личности. В-пятых, модель управления рисками: например, если у человека с ПТСР развилось расстройство, связанное с употреблением психоактивных веществ, и он проявляет сильную агрессию, то госпитализация и другие соответствующие стратегии, нацеленные на безопасность пациента и семьи, могут быть первоочередной задачей.
Несмотря на наличие существенной доказательной базы по лечению тревожных расстройств, а также растущей доказательной базы по ведению пациентов с сопутствующей патологией, любому конкретному пациенту требуется индивидуальная оценка, взвешивание возможных причинно-следственных моделей для оптимального решения этих проблем.
СОПУТСТВУЮЩИЕ СОМАТИЧЕСКИЕ НАРУШЕНИЯ
Тревожные расстройства могут возникать как следствие физического расстройства, предшествовать физическому расстройству или быть сопутствующим явлением.
Широкий спектр физических расстройств может привести к симптомам тревоги или усугубить их, с некоторыми признаками специфичности для тревоги и связанных с ней расстройств. Так, например, существуют важные причинно-следственные связи между респираторными заболеваниями и паническим расстройством 87 . Было высказано предположение (хотя оспариваемое), что существуют причинно-следственные связи между паническим расстройством и целым рядом физических состояний, включая пролапс митрального клапана 160 и гипермобильность суставов 161 . Кроме того, особое внимание уделялось роли черепно-мозговой травмы при ПТСР 162 и роли некоторых инфекций при ОКР 163 .
Большинство исследований, посвященных физической сопутствующей патологии при тревожных расстройствах, сосредоточены на сердечно-сосудистых заболеваниях. Метаанализ показал, что у людей с пожизненным диагнозом тревожного расстройства на 60% повышен риск возникновения сердечно-сосудистых заболеваний 164 . Примечательно, что риск тревожного состояния существенно возрастает после острого заболевания, например острого инфаркта миокарда. Осведомленность о событии болезни может сыграть важную роль, поскольку “тихий” инфаркт миокарда (при котором человек не знает о сердечном событии 165 ) не сопровождается повышенным риском развития тревожных состояний, в отличие от явного инфаркта. Тревога после инфаркта миокарда, в свою очередь, связана с негативными сердечно-сосудистыми последствиями 166 .
Несмотря на значительное внимание к связи между тревожными расстройствами и сердечно-сосудистыми заболеваниями, наличие причинно-следственной связи еще предстоит доказать. Возможно, что еще более важно, эта ассоциация не является специфичной, поскольку тревожные расстройства связаны с целым рядом физических расстройств, с коэффициентами риска в диапазоне 1,17–1,73 для 10 групп состояний и между 1,13 и 2,40 для отдельных состояний 167 . Связь тревожных расстройств с сердечно-сосудистыми заболеваниями находится только в середине этого диапазона. Другими словами, чрезмерное внимание к сопутствующей патологии тревожных расстройств с сердечно-сосудистыми заболеваниями не оправдано, и внимание следует распространить на другие физические состояния.
Учитывая отсутствие специфичности в ассоциациях тревожных расстройств с физическими заболеваниями, мы подчеркиваем важность скрининга и оценки физических расстройств у всех пациентов с тревогой и связанными с ней расстройствами, а также уделения особого внимания возможности того, что физические условия играют причинную роль в развитии тревожных расстройств, особенно у пациентов с необычными или рефрактерными проявлениями 168 . Более конкретные рекомендации относительно оценки физического состояния были даны при депрессии, которая часто сопровождается тревогой и связанными с ней расстройствами 6 . Эти рекомендации согласуются с общим акцентом на интеграцию психического здоровья в лечение неинфекционных заболеваний, включая выявление и устранение поддающихся изменению факторов риска, таких как употребление табака, нездоровое питание, отсутствие физической активности и вредное употребление алкоголя 169,170 .
Клиницисты должны учитывать, как конкретные симптомы тревоги пациента могут повлиять на взаимодействие с медицинскими учреждениями. Например, беспокойство может привести к тому, что пациенты не обратятся за помощью по поводу симптомов физического здоровья, или затруднить посещение ими медицинских осмотров. С другой стороны, определенные тревожные опасения (например, беспокойство по поводу здоровья) могут привести к многочисленным обращениям к врачу, где чрезмерная диагностика может привести к усилению основных проблем, связанных с тревогой. В этих обстоятельствах могут быть уместны такие меры, как опросник Краткий перечень проблем со здоровьем 171 , и адекватный подбор методов лечения 172 .
Когда педиатрический острый нейропсихический синдром (PANS) подозревается в качестве причины возникновения симптомов ОКР, требуется провести всестороннее психиатрическое и физическое обследование 163 , и в дополнение к стандартным методам лечения ОКР может быть рассмотрена специфическая иммунотерапия 173 . Учитывая высокие показатели совместного возникновения ПТСР и черепно-мозговой травмы, может быть рекомендован скрининг на это состояние у пациентов с ПТСР: появляется все больше литературы, демонстрирующей, что существующие методы лечения ПТСР эффективны в этой популяции 174 , но может потребоваться дополнительное выявление симптомов травмы головного мозга. Оценка и лечение обструктивного апноэ во сне может улучшить лечение ПТСР.
В целом наличие сопутствующих физических заболеваний требует целенаправленного лечения. Это может включать мероприятия, ориентированные на конкретные заболевания, а также на формирование здорового образа жизни. Примечательно, что появляется все больше свидетельств того, что занятия физической активностью защищают от тревожных симптомов и расстройств 175 . Однако доказательства эффективности аэробных упражнений, а также ряда подходов к дополнительной и альтернативной медицине в лечении тревоги и связанных с ней расстройств остаются предварительными 176,177 .
СЕМЕЙНЫЙ АНАМНЕЗ
Известно, что тревога и связанные с ней расстройства возникают в семьях, и повышенный риск развития тревожных состояний среди родственных лиц, начиная от ГТР и заканчивая ОКР, фобиями и паническим расстройством, хорошо задокументирован в клинических и популяционных выборках 178 .
Знание семейного анамнеза – где это возможно, включая конкретных пострадавших родственников, их отношения к пациенту, возраст начала и течение расстройства – может помочь клиницисту понять текущее состояние пациента и помочь пациенту контекстуализировать его/ее текущие и прошлые проблемы с тревогой.
Метааналитические данные показывают, что наличие родственника первой степени с любым тревожным расстройством может увеличить развития тревожного расстройства в 4–6 раз. Этот риск может быть аналогичным образом повышен независимо от того, является ли родственник первой степени родителем, братом или сестрой или ребенком, что позволяет предположить, что систематический опрос о ряде членов семьи может быть наиболее информативным. Это семейное накопление тревожных расстройств было в значительной степени обусловлено генетическими факторами, причем исследования близнецов показали, что наследуемость тревожных состояний составляет от 30 до 40% 178 .
Исследования показали, что специфические для расстройств паттерны семейной передачи, при которых семейная история определенного тревожного расстройства более тесно связана с повышенным риском возникновения этого же расстройства, а также других тревожных расстройств или психопатологий. Там, где это уместно, специфичность этого расстройства может быть информативной для дифференциальной диагностики тревожных состояний, поскольку сообщенная история нескольких членов семьи с данным расстройством может указывать на аналогичный диагноз, который следует учитывать. Эта специфичность была продемонстрирована для ОКР, панического расстройства, социального тревожного расстройства и в некоторых случаях ГТР 179 .
Сбор семейного анализа у самих взрослых пациентов является наиболее простым подходом, но такую информацию также можно получить от членов семьи. Исследование, сравнивающее прямое интервью с отчетами членов семьи, показало удовлетворительное согласие между информантами. Данные свидетельствуют о том, что, когда люди положительно подтверждают семейную историю тревожного или связанного с ним расстройства у одного или нескольких своих родственников, эту информацию можно считать достоверной; однако клиницисты должны иметь в виду, что люди могут не знать о тревоге и других психических состояниях у своих родственников, и сообщения могут быть предвзятыми из-за различных характеристик пациентов 180 .
Для повышения точности исследования было рекомендовано использовать несколько информантов, но это может быть сложно в стандартных клинических обследованиях. Относительно короткие инструменты скрининга для семейной психиатрической истории, такие как Скрининг Семейной Истории 181 , занимают от 5 до 20 мин и могут быть более осуществимыми в клинической практике.
Важно отметить, что положительный семейный анамнез был связан не только с развитием тревоги или связанного с ней расстройства в течение всей жизни, но и со значимыми клиническими изменениями в болезни. Например, проспективное когортное исследование показало, что семейный анамнез тревожного расстройства был связан с большей повторяемостью тревоги и ухудшением функционирования, а также с большим количеством посещений врача в течение взрослой жизни 182 . Таким образом, оценка семейного анамнеза может поспособствовать лучшему прогнозированию и помочь с подбором терапии.
РАННИЕ СРЕДОВЫЕ ФАКТОРЫ
Широкий спектр ранних воздействий окружающей среды был изучен в связи с тревожными расстройствами. К ним относятся перинатальные осложнения, сезон рождения, социально-экономический статус, методы воспитания родителей, инфекции и черепно-мозговая травма. Исследования характеризовались методологическими ограничениями, и выводы остаются предварительными 183-185 . Тем не менее следует особо оценить ряд ранних воздействий на окружающую среду, поскольку они могут повлиять на планирование лечения.
Во-первых, появляется все больше свидетельств того, что острое начало обсессивно-компульсивных симптомов в детском возрасте иногда может быть вызвано стрептококковыми инфекциями (т.е. аутоиммунными психоневрологическими расстройствами, связанными со стрептококковыми инфекциями, PANDAS) или широким спектром других заболеваний (например, PANS). Как отмечалось ранее, при подозрении на PANS требуется всестороннее психиатрическое и физическое обследование 163 , и в таких случаях имеет смысл рассмотреть дополнение стандартного лечения специфической иммунотерапией 173 .
Во-вторых, растущая база фактических данных подтверждает связь между трудностями в раннем детстве и последующим развитием тревожных расстройств. Примеры включают физическое и сексуальное надругательство 186,187 , разлуку с родителями 188 и эмоциональное жестокое обращение 189 . Большее количество серьезных невзгод в детстве и подростковом возрасте предсказывало последующее возникновение тревожных расстройств в течение следующих нескольких лет в выборке поздних подростков 190 . Данные Всемирных обследований психического здоровья показывают, что снижение уровня насилия над детьми приводит к снижению распространенности тревожных расстройств на 31% 191 . В литературе по-прежнему изучается ряд вопросов, включая ассоциации различных типов ранних психологических травм с тревогой, возрастом, когда была нанесена психотравма, причинно-следственные связи между такими травмами и развитием тревоги, а также ассоциации детских травм с различными клиническими особенностями тревоги.
Учитывая важность этой связи, оценка истории детских травм должна быть частью комплексной диагностики пациентов с тревожными расстройствами. Как обсуждалось в связи с депрессией, при оценке ранних психологических травм у пациента с тревожностью 6 необходимо учитывать ряд ключевых вопросов. Во-первых, сообщения о неблагоприятных обстоятельствах в значительной степени субъективны, и существует вероятность предвзятого отзыва. Во-вторых, важно исследовать не только произошедшие события, но и ключевые аспекты субъективного опыта и присвоенный смысл. В-третьих, личность и социокультурный фон могут влиять как на опыт, так и на сообщения о детских травмах. Анализ истории детских психотравм, который акцентируется на преодолении трудностей и устойчивости, может быть полезен для решения этих проблем.
Детский опыт заботы и жестокого обращения (CECA) 192 представляет собой комплексный опрос для оценки наличия неблагоприятных условий в детстве. Он позволяет подробно собрать информацию, но для его проведения требуется много времени, подготовка интервьюера, а информация о его клинической полезности ограничена. Несколько более коротких анкет для самоотчета были использованы в исследовательских целях и могут быть рассмотрены в клинической практике. К ним относятся более короткий опросник для самоотчета, основанный на CECA (CECA.Q) 193 , и Опросник детской травмы (CTQ) 194 . Краткая форма CTQ содержит 28 пунктов, оценивающих 5 причин возникновения детских психотравм: эмоциональная холодность, недостаток физических контактов, эмоциональное насилие, физическое насилие и сексуальное насилие.
Существует ряд мер для оценки моделей поведения молодых родителей. Опросник молодых родителей (YPI) используется в схемной терапии и служит полезным способом оценки стилей воспитания и того, как они могут быть связаны с ранними неадаптивными схемами индивидуума 195 .
В опроснике содержится 72 пункта, которые ретроспективно оценивают воспринимаемый опыт воспитания в отношении каждого воспитателя. Этот показатель предназначен для использования в сочетании со схематическим опросником молодых родителей (YSQ) 196 , в котором оценивается восемнадцать ранних неадаптивных схем воспитания.
Хотя большая часть потенциально значимой доказательной базы базируется на данных работы, посвященной депрессиям 6 , наличие ранних неблагоприятных факторов может повлиять на планирование лечения тревожных расстройств несколькими способами. Во-первых, наличие ранних неблагоприятных последствий может быть связано с преждевременным прекращением лечения, возможно, из-за слабого терапевтического альянса. В таких случаях представляется целесообразным уделять особое внимание совместному принятию решений. Во-вторых, можно рассмотреть конкретные основанные на фактических данных методы психотерапии, разработанные для пациентов с детскими психотравмами, такими как, например, проработка детских травм. В-третьих, возможно, что ранние неблагоприятные условия приводят к снижению реакции на лечение, что указывает на необходимость смены тактики.
ПОЗДНИЕ СРЕДОВЫЕ ФАКТОРЫ
Широкий спектр факторов, вызывающих стресс в окружающей среде, связан с повышением уровня тревожности 197 . К ним относятся статус меньшинства (особенно связанный с риском развития ПТСР, который был обусловлен опытом дискриминации и изоляции), нестабильность доходов, безработица, бездомность, стихийные бедствия, вооруженные конфликты, преступность и переселение.
Люди, имеющие детские психотравмы, больше подвержены тревожным состояниям, развивающимся от более слабых стрессоров (т.е. сенсибилизация к стрессу). Например, данные Национального эпидемиологического обследования по алкоголю и связанным с ним состояниям (NE-SARC) показали, что степень влияния стрессовых жизненных событий прошлого года на риск развития тревожных расстройств и ПТСР была усилена наличием детских травм, особенно трех или более 198 . На степень влияния так же влияет пол, поскольку для повышения чувствительности к стрессу у женщин по сравнению с мужчинами требовалось меньше основных жизненных стрессоров.
Данные близнецовых исследований показывают, что почти все виды средового влияния подвержены генетическому влиянию (например, генетическая склонность к рисковому поведению может привести к увеличению воздействия опасных сред) 199 . Доказательства влияния генетики на стресс до сих пор слабы, а данные близнецовых исследований указывают на отсутствие умеренных эффектов взаимодействия 200,201 . Полногеномные методы дали многообещающие начальные результаты: например, было обнаружено, что полигенный показатель эмоциональной отзывчивости к окружающей среде взаимодействует с негативным воспитанием, вызывая более выраженную тревожную симптоматику 202 .
Учет непосредственных жизненных стрессоров важен при оценке тревожных расстройств. Полуструктурированные интервью включают в себя Шкалу жизненных событий и трудностей (LEDS) 203 , которая оценивает объективные аспекты жизненных событий и воздействие хронических стрессоров, а также субъективный опыт человека о том, насколько угрожающими или разрушительными они были. Другим полезным инструментом является Интервью Жизненного Стресса Калифорнийского Универститета 204 , в котором оценивается как хронический, так и эпизодический стресс, а также оценивается их степень влияния в контексте других жизненных обстоятельств. Для обоих вариантов интервью требуется подготовка.
Ряд самоопросников для оценки жизненных событий и воздействия хронических стрессоров может быть пригоден для использования в клинической практике. К ним относятся Психиатрическая Эпидемиологическая Исследовательская Шкала (PERI-LES) 205 , Опросник по угрожающим переживаниям (LTE) 206 и Опросник стрессовых жизненных событий (QSLE) 207 . Все они обладают хорошими или сильными психометрическими свойствами. В PERI-LES перечислены 102 события, и он широко использовался в эпидемиологических исследованиях. LTE был специально разработан кратким. Он оценивает всего двенадцать недавних событий в жизни, которые связаны с долгосрочной угрозой. QSLE был разработан, чтобы охватить все периоды жизни, в нем оценивается восемнадцать жизненных событий, которые происходят в детстве, подростковом возрасте и взрослой жизни, и их влияние. Дискриминацию можно оценить с помощью самоопросника Шкала повседневной дискриминации 208 .
Стрессовые жизненные события и хронические стрессоры могут влиять на клиническое ведение несколькими способами. Во-первых, они могут препятствовать самообслуживанию и приверженности/реагированию на медицинскую помощь, особенно в сочетании с высокими личными требованиями (такими как высокие школьные или должностные обязанности) 209 . Например, практика выполнения домашних заданий КПТ может выполняться реже в зависимости от жизненных стрессоров, и, хотя практика когнитивных и поведенческих навыков важна для общих показателей успеха, учет препятствий для выполнения практик необходим для адекватного лечения.
Во-вторых, высокий уровень хронического стресса может привести к стойкой сенсибилизации гипофизарно-надпочечниковой оси и вегетативной нервной системы 210 , тем самым способствуя усилению физиологических и когнитивных нарушений, уже присутствующих у лиц с тревожными расстройствами. Сочетание высокого возбуждения и дефицита внимания может снизить восприятие информации, относящейся к лечению, будь то информация о лекарствах или когнитивных и поведенческих навыках. Стратегии регулирования возбуждения (например, переподготовка дыхания, расслабление мышц, тренировка осознанности) могут иметь особую ценность для человека, сталкивающегося со значительными жизненными стрессорами.
В-третьих, для некоторых людей травматический опыт может потребовать терапии, сфокусированной на травму, нацеленной на навязчивые и тревожные воспоминания, а также на поведенческие и физиологические последствия.
С другой стороны, понимание контекстуальных факторов, таких как соседское насилие, может смягчить терапевтический подход к травматизации; например, воздействие in vivo на области, которые напоминают о травме, будет противопоказано всякий раз, когда существует вероятность повторной травмы.
В-четвертых, знание о недавних жизненных стрессорах может помочь в подборе психологического лечения. Например, пациенты с паническим расстройством иногда сообщают о медицинских травмах у себя или других членов семьи, которые вызывают у них боязливую реакцию на телесные ощущения. Понимание этих медицинских травм может помочь клиницисту наиболее эффективно адаптировать когнитивную перестройку в отношении личного риска или спроектировать воздействия 211 . Аналогичным образом, пациенты с социальным тревожным расстройством, которые недавно были уволены с работы, могут испытывать повышенное восприятие отвержения, и эта информация может способствовать адаптации практики когнитивных навыков.
ЗАЩИТНЫЕ ФАКТОРЫ/УСТОЙЧИВОСТЬ
Факторы защиты и устойчивости, как правило, могут быть сгруппированы на индивидуальные личностные черты и на поддерживающие факторы окружающей среды, хотя эти два фактора, вероятно, будут взаимосвязаны, поскольку люди с устойчивыми чертами характера могут самостоятельно выбирать благоприятную среду и вести свою жизнь таким образом, чтобы увеличить устойчивость к стрессу.
Экстраверсия – это индивидуальная черта, которая, как показано, действует как защитный фактор при тревожных расстройствах (см. выше). Одним из аспектов экстраверсии являются положительные эмоции, такие как счастье, радость, заинтересованность, уверенность. Было показано, что они способствуют гибкости мышления и решению проблем, уменьшают физиологические последствия негативных эмоций, создают устойчивые социальные ресурсы, способствуют эффективным стратегиям преодоления и создают условия улучшения эмоционального благополучия 212 .
Высокий уровень позитивного влияния черт характера действовал как защитный фактор в смягчении клинической картины тревожных расстройств в перспективе и как защитный фактор, уменьшая последствия стрессовых жизненных событий и риска развития социального тревожного расстройства 213 . Черты характера, которые, как было показано, снижают риск тревожных расстройств у подростков, включают оптимизм, воспринимаемую компетентность и адекватную самооценку 214 .
В обзоре защитных факторов тревожных расстройств среди взрослых в общей популяции также были выделены уровни физической активности и стили преодоления стрессовых событий (способы реагирования на воспринимаемые стрессоры) 215 .
Благоприятная межличностная среда может выступать в качестве защитного фактора от стрессовых воздействий. Предполагается, что гармоничные межличностные отношения способствуют благополучию за счет расширения социальных контактов и связей, а также доступа к ресурсам. Защитная функция социальной поддержки была продемонстрирована в различных контекстах риска, включая испытанное насилие в детстве 216 . Социальная поддержка также связана со снижением риска развития тревожных расстройств в перспективе 214,217 и может смягчить развитие ПТСР после воздействия травмы. Учитывая роль низкого финансового благополучия в развитии тревожности 197 , неудивительно, что наличие работы коррелирует с уменьшением симптомов депрессии и тревоги и снижением риска самоубийств, особенно среди мужчин 218-220 .
Всестороннее клиническое интервью для пациентов с тревожностью и связанными с ней расстройствами должно охватывать защитные факторы и устойчивость. Как описано в случае с депрессией 6 , аббревиатура SOCIAL помогает выделить основные защитные факторы: Социальные ресурсы, включая друзей, группы и социальное влияние (S); Место работы (оплачиваемое или нет) (O); Детей и семью (С); Доходы и источники материальных ресурсов (I); Способности, внешность, здоровье, свободное время и другие личные ресурсы (A); а также Любовь и секс в интимных отношениях (L) 221 . Более углубленные расспросы по этим темам могут оценить сильные стороны, которые можно использовать на протяжении всего процесса лечения (например, привлечение поддерживающего партнера в аспектах практики когнитивно-поведенческих навыков), а также слабые области, которые необходимо укрепить.
Существует ряд стандартизированных шкал для определения факторов защиты. Положительное влияние признака может быть измерено с помощью Шкалы положительного и отрицательного воздействия (PANAS) 222 , широко используемого инструмента, состоящего из 20 пунктов. Самооценку можно оценить с помощью шкалы самооценки Розенберга 223 , десятибалльной шкалы общей самооценки или самопринятия. Альтернативой им может быть Информационная система измерения результатов (PROMIS) 224 , состоящая из пунктов шкалы для определения чувства смысла и цели (ощущение того, что в жизни есть цель и есть веские причины для жизни, включая надежду, оптимизм, целеустремленность и чувства, что жизнь достойна), положительного влияния (чувства, которые отражают уровень приятного взаимодействия с окружающей средой, такие как счастье, радость, волнение, энтузиазм и удовлетворенность) и самоэффективности (уверенность в способности эффективно справляться с различными стрессовыми ситуациями).
Был разработан ряд шкал самоотчета воспринимаемой устойчивости 225 , которые рекомендованы для использования в клиническом лечении депрессии. К ним относится шкала устойчивости Коннора-Дэвидсона 226 , 25-балльная шкала личной компетентности, упорства, доверия к своим инстинктам, терпимости к негативным влияниям, принятия изменений, безопасных отношений и духовных влияний, которая чувствительна к изменениям в лечении. Укороченная версия этой шкалы из 10 пунктов может быть более практичной 227 . Краткая шкала устойчивости включает всего 6 пунктов и измеряет способность оправляться от жизненных стрессоров 228 .
Большое количество шкал измеряет социальную поддержку. Например, Многомерная Шкала Воспринимаемой Социальной Поддержки 229 , которая состоит из 12 пунктов и определяет воспринимаемую поддержку со стороны семьи, друзей и значимых других. Другим вариантом является Медицинское Обследование Социальной Поддержки 230 , которое измеряет эмоциональную/информационную поддержку, материальную поддержку и социальное взаимодействие. Кроме того, шкалы PROMIS 224 включают показатели дружеского общения, эмоциональной поддержки, ин формационной поддержки и инструментальной поддержки.
Навыки преодоления можно измерить с помощью Контрольного списка 231 "Способы преодоления". Несмотря на объем (66 пунктов), эта шкала измеряет мысли и действия, которые люди используют для удовлетворения внутренних или внешних потребностей в конкретных стрессовых ситуациях. Более короткой альтернативой является Краткая ориентация на преодоление проблем, с которыми сталкивался опись 232 (28 пунктов), в которой оценивается проблемно-ориентированное преодоление (например, активное преодоление, планирование, подавление конкурирующих действий, сдерживание и поиск инструментальной социальной поддержки) и эмоционально-ориентированное преодоление (например, поиск эмоциональной социальной поддержки, позитивное переосмысление, принятие, отрицание и обращение к религии). Эти шкалы дают представление о типе навыков преодоления, некоторые из которых являются адаптивными и могут быть усилены, в то время как другие являются неадаптивными (например, принятие желаемого за действительное, отрицание) и могут быть объектом вмешательства.
Наличие защитных факторов или их отсутствие может менять клиническое ведение несколькими способами. Во-первых, те защитные факторы, которые уже присутствуют, могут быть усилены, поощрены и использованы в лечении. Например, поддерживающие близкие люди могут быть включены в процесс лечения, например, когда родные совместно осваивают когнитивно-поведенческие навыки и облегчают практику воздействия in vivo для пациентов с агорафобией 233 . Поддерживающие члены семьи могут быть аналогично полезными партнерами для пациентов с ОКР или ПТСР, поскольку они участвуют в предотвращении воздействия стрессорных факторов, заботясь о том, чтобы исправить чрезмерную тревогу со стороны члена семьи (например, выполнение просьб пациента о чрезмерном мытье из-за опасений загрязнения), поскольку выполнение таких действий непреднамеренно усиливает избегающее поведение 234 . Позитивный аффект может способствовать экспозиционной терапии фобий 235 .
При отсутствии защитных факторов, влияния на эти области могут быть перспективны. По сути, КПТ обеспечивает большую защиту за счет обучения навыкам борьбы со внутренними (т.е. симптомами тревоги) и внешними стрессорами. Создание надежных сетей социальной поддержки может стать целью вмешательства, особенно когда тревога приводит к избегающему поведению и ослабляет социальные связи и поддержку. Новые методы психологических влияний, направленных на повышение чувствительности к вознаграждению, могут быть эффективны у пациентов со сниженным настроением 236,237 , при этом первоначальные результаты показывают эффективность как у тревожных, так и у депрессивных пациентов. Практики, основанные на осознанности, также улучшают положительное влияние 238 .
КОГНИТИВНАЯ ДИСФУНКЦИЯ
Тревожные люди проявляют повышенную чувствительность при распознавании, обработке и реагировании на информацию, связанную с угрозой, даже в отсутствие реальной угрозы.
Переоценка угрозы возникает в процессах внимания. Смещение внимания означает, что тревожные люди склонны легко отвлекаться на потенциальные угрозы за счет внимания к другим, возможно, более важным особенностям окружающей среды 239 . В клинически тревожных группах смещение внимания часто зависит от их фокуса внимания (например, социально тревожные люди проявляют смещение внимания для выявления социальных опасностей, в то время как люди с ГТР проявляют более широкое смещение внимания к физическим и социальным угрозам). Смещения внимания включают в себя ряд компонентов, начиная от сенсорно-перцептивных процессов (ранняя обработка и обнаружение стимулов), до внимания (способность обращать внимание на одни стимулы и игнорировать другие), памяти (поддержание и извлечение информации) и исполнительной функции (сложные интегративные процессы и процессы принятия решений).
Кроме того, тревожные люди, как правило, демонстрируют замедленное отвлечение от стимулов, связанных с угрозой. Особый тип смещения в процессе внимания возникает в отношении интероцептивных сигналов. Интероцептивная осведомленность (или осведомленность о внутренних состояниях организма) изучалась в основном у пациентов с паническим расстройством, но интероцептивная чувствительность может повышаться и при других тревожных расстройствах 240,241 . Примечательно, что повышенная интероцетивная чувствительность не приводит к более точной оценке состояния, что может приводить к ошибкам в сообщении о симптомах и неправильной оценке угрозы.
У людей с тревожными расстройствами могут возникать различные смещения внимания, некоторые проявляют большую предвзятость на этапе первоначального обнаружения, у других смещения внимания проявляются на этапе переключения внимания, а у третьих смещения внимания проявляются игнорированием важных стимулов 242,243 . Такие смещения внимания, вероятно, лежат в основе распространенных жалоб на отвлекаемость и плохую концентрацию у людей с ГТР и у лиц, страдающих фобией, когда они сталкиваются со своими опасными ситуациями.
Наряду с концентрированием внимания на угрозе, тревожные индивидуумы также интерпретируют неоднозначные стимулы как угрожающие 244,245 . Смещения внимания, вероятно, влияют на интерпретацию угрозы, которая, в свою очередь, предположительно влияет на внимание к угрозе. Неправильная интерпретация часто наблюдается в ответ на неоднозначные стимулы, например, значения двусмысленных предложений.
Как и в случае с “тревожным” вниманием, “тревожная” интерпретация, как правило, специфично проявляется при разных тревожных расстройствах. Таким образом, люди с паническим расстройством более склонны интерпретировать как угрозу неоднозначные стимулы, связанные с физическими ощущениями, в то время как люди с социальным тревожным расстройством склонны интерпретировать неоднозначные социальные события как более негативные, а умеренно негативные социальные события как более катастрофические в сравнении с другими тревожными пациентами или контрольной группой. Люди с ГТР склонны интерпретировать любые неоднозначные события в целом как угрожающие 20 .
Повышенная чувствительность к тревоге характерна для большинства тревожных расстройств, хотя особенно выражена у пациентов с паническим расстройством 246 . Было показано, что повышенная чувствительность к тревоге является как предиктором развития симптоматики тревоги, так и фактором, способствующим сохранению тревожной симптоматики. Она реагирует на когнитивные, поведенческие и фармакологические вмешательства 246 .
Многие исследовательские инструменты для оценки смещения внимания не подходят для клинической практики. Онлайн- или веб-программы для изменения смещения внимания (описанные ниже) обычно включают тесты на смещение внимания. Более практичными являются стандартизированные шкалы самоотчета, которые измеряют аспекты взаимодействия со стимулами, связанными с угрозой.
Одним из примеров является шкала контроля внимания из 20 пунктов 247 , оценивающая фокусировку и переключение внимания.
Опросник Интерпретации 248 оценивает взаимодействие индивидов с неоднозначными социальными сценариями. Этот опросник включает двадцать два неоднозначных сценария (например, “Вы видите, как группа друзей обедает, они замолкают, когда вы приближаетесь”) и 3 интерпретации каждого сценария (т.е. положительная: “Они собираются попросить вас присоединиться”; отрицательная: “Они говорили о вас негативные вещи”; и нейтральная: “Они только что закончили свой разговор”). Участников просят оценить, насколько вероятно, что каждая интерпретация пришла бы им в голову, если бы они оказались в аналогичной ситуации.
Для ОКР Опросник навязчивых убеждений 249 представляет собой опросник по когнитивным предубеждениям, состоящий из 44 пунктов, которые приводят к неправильной интерпретации обычно возникающих навязчивых мыслей как угрожающих. Многомерная оценка интероцептивной осведомленности-2 (МАЙЯ-2) 250 представляет собой опросник по состояниям с тридцатью семью пунктами для измерения нескольких аспектов интероцепции путем самоотчета. Индекс чувствительности к тревоге – 3 251 представляет собой шкалу из 18 пунктов с тремя подшкалами, представляющими физические проблемы (например, смерть, обморок), когнитивные проблемы (например, потеря контроля) и социальные проблемы (например, смущение), связанные с тревогой и связанными с ней симптомами.
КПТ при ОКР направлена на когнитивные предубеждения в отношении угрозы. Психообразование, начальная терапевтическая стратегия, обычно включает информацию, предназначенную для исправления ошибочных представлений, особенно о симптомах тревоги. Когнитивная реструктуризация обучает навыкам выявления завышенных оценок опасности и способам балансирования оценок с более обоснованными интерпретациями. Экспозиционная терапия нацелена на исправление ошибок прогнозирования (т.е. нарушение негативных ожиданий) посредством непосредственного опыта. Высокий уровень неправильной оценки угрозы может указывать на необходимость проведения КПТ, хотя нет достаточных доказательств соответствия подхода к лечению (медикаментозное лечение против КПТ по сравнению с другими психотерапиями) к таким когнитивным предубеждениям. Фактически только одно исследование показало, что более высокие баллы по чувствительности к тревоге предсказывали более слабую реакцию как на КПТ, так и на медикаментозную терапию 252 .
Программы модификации предубеждений появились как более целенаправленное лечение когнитивных предубеждений. Методика тренировки внимания 253 состоит из упражнений на слуховое внимание, которые требуют от людей овладения навыками исполнительного контроля, включая избирательное внимание, разделенное внимание и переключение внимания, чтобы уменьшить негибкое сосредоточенное на себе внимание, предвзятое внимание, ориентированное на угрозу, беспокойство и размышления. Эта методика продемонстрировала эффективность при тревожных расстройствах 254 . Тренировка смещения внимания (т.е. тренировка смещения внимания от стимулов, связанных с угрозой, к нейтральным или позитивным стимулам путем усиления выбора точечного воздействия) и тренировка смещения интерпретации (т.е. Обучение нейтральной или позитивной интерпретации неоднозначных сценариев путем усиления выбора слов) также имеют доказательную базу. Однако, хотя такое обучение оказывает сильное влияние на смещение внимания или интерпретации как таковое, исследования, как правило, показывают небольшие размеры влияния на симптомы тревоги 255,256 .
Понимание когнитивных предубеждений также имеет отношение к подходам фармакотерапии, особенно когда пациенты считают, что их телесные ощущения указывают на травму или опасность, что может привести к чрезмерному страху перед лекарствами и их побочными эффектами.
В этих сценариях могут быть рекомендованы дифференцированные подходы к лечению.
Когнитивные предубеждения, связанные с угрозой, могут незаметно влиять на способы получения и кодирования информации, так что то, что является благоприятными комментариями врача, может быть легко неверно истолковано как угроза пациенту. Осторожность в представлении информации с учетом предубеждений пациента может быть полезной.
Есть некоторые доказательства того, что изменение когнитивных предубеждений улучшает терапевтические результаты, особенно при расстройствах социальной тревожности 257-259 и паническом расстройстве 64 . Следовательно, отсутствие изменений в когнитивных процессах может быть показателем плохой реакции на лечение и необходимости переоценки подхода к лечению. Данные о влиянии фармакотерапии тревожных расстройств на когнитивную сферу по-прежнему находятся в стадии ранних исследований.
ОБСУЖДЕНИЕ
Цель этой статьи – описать систематически важные области, которые имеют отношение к персонализации лечения тревожных расстройств. Тщательная оценка симптомов тревоги для обеспечения надлежащего клинического диагноза имеет ключевое значение, учитывая, что большинство доказательств в этой области основано на исследованиях конкретных расстройств. Тем не менее растет число работ, подтверждающих мнение о том, что оценка других областей также полезна при принятии клинических решений.
Данные приведенных в этой статье исследований свидетельствуют о том, что мы начинаем переходить от простых рекомендаций лечить тревогу и связанные с ней расстройства с помощью СИОЗС, КПТ или их комбинации к более сложному подходу, который подчеркивает, что у врача есть все более широкий спектр доступных методов лечения и что лечение тревоги и связанных с ней расстройств может быть персонализировано в ряде важных аспектов.
Этот обзор того, что известно в настоящее время, а также ключевых областей для будущих исследований, представляется своевременным и ценным по ряду причин. Во-первых, он согласуется с растущим возрождением интереса к созданию персонализированной психиатрии и с аналогичными обзорами в других важных областях психиатрии 6,260 . Во-вторых, он согласуется с систематической работой по определению результатов лечения и может помочь определить переменные для потенциального включения в сложные прогностические модели, включая машинные подходы к обучению 261,262 . В-третьих, в литературе предлагается ряд клинически осуществимых мер, включая шкалы самоотчета, которые потенциально могут быть включены в будущие наблюдательные или интервенционные исследования.
В-четвертых, в обзоре определен ряд шкал, которые могут начать использоваться клиницистами на практике, поскольку они пытаются персонализировать лечение тревоги и связанных с ней расстройств, признавая, что для подтверждения их использования необходимы дополнительные исследования.
Ряд потенциальных критических замечаний в отношении нашего подхода здесь заслуживают обсуждения. Во-первых, можно утверждать, что клиницисты уже осведомлены о неоднородности тревоги и связанных с ней состояний. Хотя это, безусловно, верно, систематических усилий по предоставлению клиницисту практических способов оценки такой неоднородности не предпринимается. Во-вторых, можно утверждать, что использование формальных оценок не является практичным или эффективным в стандартной клинической практике. Однако, даже если клиницисты не всегда формально полагаются на диагностические критерии, внедрение надежной нозологической системы благотворно повлияет на подход клиницистов к оценке, и существует растущая доказательная база, свидетельствующая о ценности регулярного мониторинга исходов тревожных расстройств 106,107 . В-третьих, можно утверждать, что в конечном счете для оптимальной персонализации управления тревогой и связанными с ней расстройствами необходим трансляционный нейробиологический подход. Наша цель, безусловно, состоит не в том, чтобы преуменьшить важность такой работы, а скорее в том, чтобы утверждать, что уточнение клинической оценки может внести полезный вклад как в нейробиологическую, так и в интервенционную работу в будущем.
Ключевым вопросом, который возникает в результате этого и аналогичных обзоров, является обилие и сложность имеющихся соответствующих мер. Это изобилие создает ряд важных проблем для диагностики 263 . Во-первых, даже если клиницисты согласны с важностью оценки конкретной конструкции, использование различных инструментов может привести к разногласиям в выводах. Во-вторых, меры могут дать информацию, которую клиницистам трудно интерпретировать, и поэтому могут укрепить мнение о том, что клиническое суждение более полезно, чем клинические меры. В-третьих, использование ряда показателей может затруднить общение между врачами и пациентами, что затруднит совместное принятие решений. Приведенный здесь обзор согласуется с призывами разработать общие показатели 264 , согласовать основные наборы результатов 265,266 и согласовать результаты измерений 263 .
Возможно, будет полезно сравнить существующие работы по индивидуальным подходам к депрессии и тревожности 6 . На первый взгляд, похоже, что область депрессии гораздо более развита, с большим количеством имеющихся данных по целому ряду важных областей и о том, как их можно использовать для персонализации лечения. Напротив, тяжелая депрессия является чрезвычайно гетерогенным состоянием, в то время как некоторые тревожные и связанные с ними расстройства кажутся более однородными. Хотя ни одному конкретному тревожному или связанному с ним состоянию не уделялось столько внимания, как депрессии, распознавание специфической тревожности и связанных с ней состояний создало возможность для более детальной работы над каждым из этих расстройств, а подтипирование конкретных состояний способствовало персонализированному подходу к терапии пациента.
Очевидно, что необходимо проделать большую дальнейшую работу для разработки подробного и основанного на фактических данных подхода к персонализации терапии тревожных расстройств.
Иерархические модели симптомов, такие как модель иерархической таксономии психопатологии (HiTOP) 155 или трехуровневая модель депрессии и тревожности 267,268 , обеспечивают полезную основу для понимания генетических, нейробиологических и экологических факторов риска и моделей ковариации симптомов. В будущем было бы полезно, чтобы клинические испытания включали не только диагностику тревоги и определение тяжести симптомов, а также более подробную оценку симптоматики (например, оценку специфического поведения, физиологических параметров и когнитивных оценок), а также ряда других областей, рассмотренных здесь. Мы надеемся, что такая работа поспособствует персонализации лечения тревоги и связанных с ней состояний.
Перевод: Викторов А.А. (г. Санкт-Петербург)
Редактура: к.м.н. Рукавишников Г.В. (г. Санкт-Петербург)
Stein DJ, Craske MG, Rothbaum BO et al. The clinical characterization of the adult patient with an anxiety or related disorder aimed at personal-ization of management. World Psychiatry. 2021;20(3):336-356.
DOI:10.1002/wps.20919
Хотя современные диагностические системы, безусловно, полезны для составления первоначального плана лечения, приходится разрабатывать вспомогательные диагностические методы. Они помогают отойти от гайдлайнов, которые делают упор на СИОЗС и КПТ как первую линию терапии, к более детальной диагностике, которая предоставляет клиницистам больше конкретных рекомендаций и способствует более персонализированному подходу к терапии пациента. Эта статья направлена на систематическое описание важных факторов (доменов), релевантных для персонализированного ведения пациентов с тревожными расстройствами и связанными состояниями, такими как обсессивно-компульсивное расстройство (ОКР) и посттравматическое стрессовое расстройство (ПТСР) (Таблица 1). Для каждого фактора (домена) мы собрали результаты актуальных исследований и рассмотрели релевантные диагностические инструменты, уделяя особое внимание возможности использовать их в рутинной клинической практике. Мы выделили области, где имеющиеся данные позволяют клиницистам персонализировать ведение тревожных состояний, и определили, где таких данных недостаточно. Научная литература, посвященная тревоге, имеет много пересечений с работами о депрессии, поэтому неудивительно, что факторы, описанные в этой работе, сходны с факторами, описанными в предыдущей статье по депрессии.
В соответствии с принципами доказательной медицины, значительные усилия были приложены к поиску биомаркеров тревожного расстройства и связанных состояний. Примечательно, что возникновение и уменьшение страха – это парадигма, лежащая в основе симптомов всех тревожных расстройств, а также концептуализации подходов к лечению. Другие специфические конструкции, такие как когнитивная гибкость и ингибиторный контроль, могут быть более актуальными для конкретных заболеваний, таких как ОКР 8 . Эти концепты были отмечены в классификации психических расстройств Национального института психического здоровья США (NIMH) Исследовательских критериев доменов (RDoC) 9 , и способствовали разделению тревожных расстройств в DSM-5 и МКБ-11 на тревожное или связанные со страхом расстройства, обсессивно-компульсивное и связанные расстройства и расстройства, специфически связанные со стрессом (эти термины использованы в МКБ-11).
Несмотря на обилие серьезных работ по нейробиологии тревоги и связанных расстройств, на сегодняшний день не существует достаточно чувствительных и специфических биомаркеров, которые можно использовать в клинической практике. Поэтому мы не рассматриваем подробно биомаркеры в нашей статье. Однако мы предполагаем, что более персонализированный подход к пациентам с тревогой, может быть полезен в поиске биомаркеров, а также для работы над нейробиологией тревоги в целом, учитывая потенциальную ценность более тонких клинических методов оценки гетерогенности расстройства способами, которые могут быть нейробиологически информативными и предсказать реакцию на лечение.
Статья фокусируется на тревоге и связанных расстройствах у взрослых пациентов. Данные заболевания часто имеют раннее начало, и изучение тревоги у детей важно, как с клинической точки зрения, так и с точки зрения общественного здравоохранения, поэтому необходимы дополнительные исследования тревожных расстройств у детей и подростков. Мы также не рассматриваем подробно тревогу, возникающую вторично по отношению к другим психическим расстройствам, таким как депрессивное расстройство, психотические расстройства, тревогу, связанную с другими медицинскими состояниями, или тревогу, связанную с приемом препаратов, несмотря на их клиническое значение. Также мы не рассматриваем подпороговый уровень тревоги и связанных расстройств. Там, где это уместно, рассматриваются культуральные и гендерные вопросы.
ПРОФИЛЬ СИМПТОМОВ
Тревожные расстройства проявляются тревогой, страхом и/или паническими атаками, часто сопровождаются избегающим поведением или чрезмерной осторожностью по отношению к предполагаемым угрозам. В DSM-5 и
МКБ-11 тревожные расстройства включают: агорафобию, генерализованное тревожное расстройство (ГТР), паническое расстройство, элективный мутизм, тревожное расстройство, вызванное разлукой, специфические фобии и социальное тревожное расстройство. ОКР и ПТСР выносят в отдельную, но тесно связанную группу. В обоих нозологиях диагностика тревожных расстройств предполагает наличие у пациента выраженного или существенного уровня страха или тревоги, которые отличаются от стресс-индуцированной тревоги стойкостью (т.е. длятся несколько месяцев и больше) и уровнем приносимого дискомфорта.
В МКБ-10 и DSM-5 тревожные расстройства в первую очередь дифференцируют по предполагаемой угрозе и объектам и ситуациям, вызывающим тревогу или страх. Предполагаемая угроза и связанные стимулы варьируются от жестко ограниченных (например, при специфических фобиях) и ситуативных (агорафобия, тревожное расстройство при разлуке, паническое расстройство и социальное тревожное расстройство) к распространенным на все области жизни (при генерализованном тревожном расстройстве). Таким образом, при малой специфичности тревоги, как симптома, тревожные расстройства могут быть дифференцированы при тщательном изучении ситуаций, при которых возникают тревога и избегающее поведение.

Например, паническое расстройство возникает из-за интероцептивных сигналов, которые ошибочно оцениваются как вредные, тогда как социальная тревога характеризуется страхом социальных взаимодействий и публичных выступлений, вследствие боязни негативной оценки окружающими. Дифференциальная диагностика тревожных расстройств имеет важное значение для ведения пациента и подбора терапии, поскольку большинство научно обоснованных фармакологических и психологических методов лечения эффективны только при определенных расстройствах.
Наиболее значимые отличия в диагностических критериях между МКБ-11 и DSM-5 у ПТСР. В DSM-5 критерии были существенно расширены, чтобы включить двадцать симптомов в 4 кластера, в попытке охватить весь спектр хронических посттравматических расстройств. В отличие от этого, МКБ-11 упростил диагностические требования к ПТСР до трех основных симптомов, которые наиболее четко отличают это расстройство от других состояний: повторное переживание травмирующего события или событий в настоящем, попытки избежать напоминания о событии и ощущения постоянной угрозы. Данные исследований показывают, что упрощенные критерии МКБ-11 эффективнее помогают диагностировать ПТСР, чем критерии DSM-5. МКБ-11 определяет, что “комплекс ПТСР” состоит из 3 основных симптомов, описанных выше, которые сопровождаются нарушением регуляции аффекта, пониженной самооценкой и трудностями в отношениях с окружающими. Анализ скрытого класса и анализ скрытого профиля подтвердили различия между ПТСР и “комплексом ПТСР”, а также обнаружили связь между сложным ПТСР и травмой в детстве в некоторых исследованиях.
Тревожные расстройства проявляются чувством страха или тревогой. Страх – это эмоциональная реакция на воспринимаемую предсказуемую или неминуемую угрозу, когда мало или совсем нет времени для сознательной разработки стратегии побега, в то время как тревога – это ориентированное на будущее состояние ожидания неопределенных, длительных или отдаленных угроз, когда есть время понять и прочувствовать природу ситуации. Оба состояния предназначены для активации когнитивных, аффективных, физиологических и поведенческих процессов, повышающих безопасность. В случае страха быстрые, непроизвольные физиологические реакции облегчают выбор и выработку соответствующей реакции (борьба или бегство). В то время как тревога активирует физиологическую и когнитивную стратегическую подготовку к борьбе или бегству, если это необходимо. Этот взгляд на страх и тревогу подтверждается моделями континуума неизбежности хищничества животных, которые предполагают различные режимы (от потенциальной угрозы до обнаружения угрозы, до атаки хищника при нападении), каждый из которых приводит к различным четко определенным моделям защитного поведения.
Эти канонические модели универсальны (хотя ответы зависят от вида) и применимы не только к приматам, но и к людям. Оптогенетические исследования у не приматов показывают, что стимулы, аналогичные угрозам до и после столкновения, вызывают активацию вентромедиальной префронтальной коры, гиппокампа и базолатеральной миндалины – областей, участвующих в запоминании угроз, поиске и предотвращении. В цикле режима атаки активируются средняя поясная кора, центральная миндалина, гипоталамус и периакведуктальное серое вещество – области, участвующие в быстром реагировании на угрозу (например, бегство). Аналогичные защитные схемы существуют и у людей: снимки функциональной магнитно-резонансной томографии (МРТ) показывают, что отдаленная угроза связана с повышенной активностью в вентромедиальной префронтальной коре, и по мере приближения угрозы наблюдается большая активация в периакведуктальном сером веществе среднего мозга. RDoС, в котором используется комплексный подход к психопатологии, опирается на эти модели и предполагает, что “ответы на угрозы с низкой вероятностью качественно отличаются от поведения при высокой вероятности угрозы, которые характеризуют страх”.
В то время как прототипы страха и тревоги находятся в разных “местах” в континууме реагирования, клинические проявления более подвижны. Например, восприятие угрозы может быстро измениться с отдаленного на неизбежное с помощью одних только оценок и образов, без изменения внешних обстоятельств. Примером может служить человек с посттравматическим расстройством, который испытывает страшное воспоминание о травме (т.е. о неминуемой угрозе) в разгар тревоги в незнакомой обстановке (т.е. отдаленная угроза). Тревога и страх проявляются в нескольких сферах: поведенческой, физиологической и субъективных ощущениях. Состояния тревоги обычно сопровождаются бдительным, осторожным и избегающим поведением, физиологической готовностью к серьезной опасности (реакция испуга, мышечное напряжение), заявлениями о беспокойстве или озабоченности, а также ощущением надвигающейся или неопределенной угрозы (например, “Что, если я неправильно произнесу слово на званом обеде на следующей неделе – мне будет так неловко” или “Что, если я упаду в обморок в кинотеатре”). Состояния страха сопровождаются поведением побега (или сражения), возбуждением автономной нервной системы, заявлениями о страхе и испуге и ощущением серьезной угрозы (например, «Я умираю» или «Мне нужно выбираться отсюда»).
Примечательно, что эти способы ответа не всегда совпадают 30 . Например, люди могут сообщать о тревоге или страхе при отсутствии физиологических или поведенческих изменений или могут избегать ситуаций, не испытывая чувств тревоги или страха. Даже во время панических атак люди иногда сообщают о страхе без признаков физиологических изменений 31 . Такое несоответствие может быть информативным для выбора лечения. Например, субъективный дистресс при отсутствии физиологических изменений может указывать на ценность когнитивно-ориентированного подхода к лечению, а не биологически ориентированного (такого как регуляция дыхания или фармакотерапия), а избегающее поведение при отсутствии физиологических изменений может указывать на особую ценность экспозиционной терапии. Однако доказательства такого подбора лечения еще только появляются, поскольку клинические исследования были сосредоточены в первую очередь на конкретных диагнозах и клинических подтипах, а не на детальной оценке конкретного поведения, физиологических параметров или когнитивных оценок.
В клинической практике первым и ключевым шагом в оценке тревоги является постановка диагноза тревожного расстройства на основе профиля симптомов. Диагноз тревожных расстройств у взрослых может быть установлен с помощью клинических интервью. Примерами таких интервью служат: структурированное клиническое интервью для диагностики для DSM-5 (SCID-5) 32 , мини-международное нейропсихиатрическое интервью (MINI) 33 , комплексное международное диагностическое интервью (CIDI) 34 . Интервью по тревоге и связанным расстройствам для DSM-5 (ADIS-5) особенно ориентировано на дифференциальную диагностику тревожных расстройств 35 . Структурированное диагностическое интервью для обсессивно-компульсивных и связанных с ними расстройств может быть полезным для диагностики этих часто упускаемых из виду состояний 36 .
Важно определить, является ли тревожная симптоматика (например, панические атаки) проявлениями другого психического расстройства (например, депрессии или биполярного расстройства). Употребление психоактивных веществ или интоксикация (например, употребление кофеина, стимуляторы) и абстинентный синдром (например, от употребления алкоголя) могут привести к развитию выраженной тревоги. Некоторые медицинские состояния, такие как сердечно-легочные (например, астма), эндокринные (например, заболевание щитовидной железы) и неврологические (например, сложные парциальные припадки) заболевания, также вызывают развитие тревожной симптоматики.
Для выявления тревоги, связанной с заболеваниями, необходимо подробно изучить историю болезни и провести физическое обследование, проанализировать анализы крови (например, уровень тиреотропного гормона) и результаты инструментальных методов диагностики (например, электрокардиография или электроэнцефалография). Хотя структурные (например, воксель-базированная морфометрия) и функциональная МРТ использовались для изучения патофизиологии тревожных расстройств, в настоящее время они не используются в диагностических целях 11,12 .
Данные о недостаточной эффективности диагностики и лечении тревожных расстройства подчеркивают важность скрининга симптомов тревоги 37 . Опросник генерализованного тревожного расстройства-7 (GAD-7) 38 – это опросник, состоящий из 7 пунктов, который был разработан специально для ГТР, но оказался полезен для выявления любого тревожного расстройства с адекватной чувствительностью и специфичностью 39 . Другие инструменты скрининга включают больничную шкалу тревоги и депрессии 40 и шкалу общей степени тяжести тревоги (OASIS) 41 , которая включает измерение выраженности избегающего поведения (важная особенность, поскольку уровни тревожности могут быть замаскированы без такого измерения). Шкала Перинатального Скрининга Тревожности подходит в качестве неспецифического скринера для женщин в перинатальном периоде 42 .
Если присутствует тревога или связанное с ней расстройство, можно использовать несколько показателей для оценки профиля тревожной симптоматики. Интервью для определения симптомов настроения и тревоги оценивает все симптомы эмоциональных расстройств по DSM и МКБ, а также другие проявления интернализующей психопатологии 43 . Каждый пункт оценивается от явно отсутствующего до частично присутствующего (субклинический, подпороговый) и четко присутствующего, что позволяет оценить баллы профиля симптомов. Помимо интервью, существуют анкеты самооценки для каждого тревожного и родственного расстройства, которые предоставляют более подробные профили симптомов. К ним относятся шкалы DSM-5, разработанные для агорафобии, ГТР, ОКР, ПТСР, социального тревожного расстройства и специфической фобии, каждая из которых включает элементы для аффективных состояний страха и тревоги, физиологических, когнитивных и поведенческих симптомов 44 . Было показано, что, за исключением специфической фобии, эти шкалы обладают адекватными сильными психометрическими свойствами 45-52 .
Существует ряд других хорошо проверенных стандартизированных опросников по симптомам. Они включают Пенсильванский опросник для оценки уровня беспокойства 53 для ГТР; обсессивно-компульсивную шкалу Йеля-Брауна (Y-BOCS) 54 для ОКР; опросник паники и фобии Олбани для агорафобии 55 ; опросник мобильности для агорафобии 56 ; шкалу тяжести панического расстройства 57 и шкалу паники и агорафобии 58 для панического расстройства и агорафобии; Опросник посттравматического стресса для DSM-5 (PCL-5) 59 и Шкалу клинической оценки посттравматического стрессового расстройства для DSM-5 (CAPS-5) 60 для посттравматического стрессового расстройства; и «Опросник социальной фобии и тревоги» 61 и «Шкалу социальной тревожности Либовица 62 » для определения социальной фобии. Не существует шкал для каждого типа конкретной фобии, но в этом случае можно использовать Шкалу Оценки Страхов (FSS)63, анкету из 51 пункта, в которой респондентам предлагается указать свой дискомфорт или чувство тревоги по каждому из 51 стимула.
Дифференциальная диагностика тревожных расстройств может помочь клиницисту подобрать более эффективную терапию. Конкретные варианты когнитивно-поведенческой терапии (КПТ) ориентированы на конкретные тревожные расстройства. Имеются существенные доказательства эффективности таких целевых методов лечения 64-66 , и они рекомендуются в качестве психологических методов лечения тревоги и связанных с ней расстройств первой линии в нескольких руководящих организациях, в том числе в Национальном институте здравоохранения и передового опыта Великобритании (NICE) 67 . Например, КПТ для панического расстройства включает в себя интероцептивное воздействие на телесные ощущения, вызывающие страх; КПТ для социального тревожного расстройства включает когнитивную реструктуризацию вокруг размышлений после события; КПТ для генерализованного тревожного расстройства рассматривает метаубеждения о беспокойстве; КПТ для ОКР включает воздействие специфических сигналов, которые вызывают дистресс и побуждение выполнять навязчивые ритуалы, а также профилактику реагирования, направленную на устранение навязчивых состояний; и КПТ для ПТСР включает воздействие воображения или когнитивную переработку в отношении воспоминаний о травме. Таким образом, дифференциальная диагностика облегчает выбор наиболее подходящей формы психотерапии. Даже при использовании трансдиагностической КПТ, многообещающего подхода, ориентированного на конкретные расстройства 68 , клиницисту все равно потребуется реализовывать терапевтические стратегии таким образом, чтобы они учитывали направленность страхов и фобий каждого человека.
С точки зрения фармакотерапии СИОЗС продемонстрировали эффективность при всех основных тревожных и связанных с ними расстройствах. Тем не менее важно дифференцировать различные расстройства по нескольким причинам. Во-первых, рекомендации по фармакотерапии СИОЗС различаются в зависимости от различных тревожных и связанных с ними состояний 69 . Так, например, особенно важно начинать с более низких доз СИОЗС при паническом расстройстве (поскольку стандартные дозы могут быть непереносимы), в то время как более высокая доза и более длительная продолжительность лечения требуются при ОКР. Во-вторых, препараты, отличные от СИОЗС, обладают разной эффективностью при различных тревожных состояниях и связанных с ними расстройствах 69 . Так, например, трициклический антидепрессант имипрамин эффективен при некоторых тревожных и связанных с ними расстройствах (например, ГТР, паническое расстройство, ПТСР), но не при других (ОКР, социальное тревожное расстройство). Бензодиазепин алпразолам эффективен при различных тревожных расстройствах (ГТР, паническое расстройство, социальное тревожное расстройство), но не при расстройствах, связанных с тревогой (ОКР и ПТСР). Буспирон эффективен при ГТР, но не при других тревожных и связанных с ними расстройствах, в то время как ОКР представляется уникальным среди этих состояний, поскольку он более чувствителен к серотонинергическим, чем к норадренергическим ингибиторам обратного захвата 69 .
Повысить эффективность лечения может помочь сопоставление терапии с кластерами симптомов, учитывая неоднородность, существующую в диагностических метках. Действительно, есть свидетельства того, что клиницисты уже рассматривают кластеры симптомов как более информативные для выбора фармакотерапии в сравнении с диагностическими категориями 70,71 . Например, в выборке из 318 пациентов диагноз ПТСР не был связан с назначением какого-либо конкретного класса лекарств, препараты подбирались по кластеру симптомов: назначение противосудорожных средств было связано с симптомами избегания, назначение антидепрессантов связано с состоянием оцепенения, назначению анксиолитиков при тревоге и назначение стабилизаторов настроения при гипервозбуждении 71 . Аналогичным образом, при паническом расстройстве анксиолитики чаще назначались при физических симптомах реакции страха, тогда как антидепрессанты и противосудорожные средства назначались при психологических симптомах. Аналогичное соответствие класса лекарств с кластерами симптомов было найдено для агорафобии, ОКР, социального тревожного расстройства и специфической фобии. Очевидно, что профиль симптомов определяет текущий выбор фармакотерапии врачами, и область персонализированной медицины будет расширена за счет рандомизированных контролируемых исследований для подтверждения (или нет) такого соответствия профиля симптомов лекарственным средствам.
Тот же аргумент справедлив и для психотерапии, которая была поставлена в тупик использованием методик КПТ (например, дыхательные техники, когнитивная реструктуризация, экспозиционная терапия, профилактика ответных реакций) без учета кластеров симптомов. Были призывы сопоставить основные активные методы терапии с конкретными профилями симптомов (например, дыхательные техники для регуляции возбуждения, когнитивная реструктуризация для когнитивных искажений, терапия воздействия для предотвращения) 72,73 . Это остается важной областью будущих исследований. Тем не менее вполне возможно, что практикующие клиницисты уже адаптируют основные компоненты КПТ к проявлениям симптомов точно так же, как это наблюдается при фармакотерапии.
КЛИНИЧЕСКИЕ ПОДТИПЫ
Каждое из тревожных и связанных расстройств характеризуется значительной неоднородностью, из-за чего и были выделены несколько клинических подтипов. Содержание страха или беспокойства (когнитивный компонент), физиологических реакций (таких как паническая атака) и поведенческой реакции (которая часто включает избегающее поведение и может включать опасливое поведение) может быть полезным при определении наличия или отсутствия определенного клинического подтипа. Кроме того, был принят ряд других подходов к подтипам, в том числе в зависимости от возраста начала и сопутствующих симптомов. Здесь мы рассматриваем основные клинические подтипы ключевых тревожных расстройств.
При ГТР полезно оценить как природу беспокойства, так и диапазон психических (психологических) и соматических (физические) симптомов. Беспокойство может быть сосредоточено на смерти (например, кто-то не звонит, когда он сказал, что предпочел бы умереть), болезни (например, «головная боль означает, что у меня опухоль мозга»), разрушении (например, «протечка в потолке означает, что нужна новая крыша, и если я не сделаю ее вовремя, мой дом будет разрушен»), а иногда на нищете (например, «Если я одолжу сестре деньги, она никогда не перестанет просить, и я разорюсь»). Такие инструменты, как Пенсильванский опросник для оценки уровня беспокойства 53 , оценивают направленность беспокойства у пациентов ГТР, в то время как психические и соматические подшкалы шкалы оценки тревожности Гамильтона (HAM-A) 74 полезны для оценки спектра симптомов.
Понимание точной природы страха важно для КПТ, которая может сосредоточиться на когнитивной реструктуризации конкретных беспокойств или подверженности определенным видам страхов. С точки зрения фармакотерапии ранее считалось, что трициклические антидепрессанты более полезны при психических симптомах, в то время как бензодиазепины более полезны при соматических симптомах 75 . Тем не менее было относительно мало последующих доказательств, подтверждающих избирательную реакцию психических и соматических симптомов на различные методы фармакотерапии. Ряд лекарств, эффективных при ГТР, влияют как на психические, так и на соматические симптомы 76-79 .
Что касается ОКР, в значительной части литературы подчеркивается, что навязчивые идеи и компульсии, как правило, имеют несколько симптомов, включая мытье, проверку безопасности, упорядочивание предметов и накопительство 80 . Хотя у многих пациентов есть симптомы, которые лежат в разных измерениях, или они испытывают целый ряд симптомов, меняющихся с течением времени, есть некоторые свидетельства того, что плоскость проявления симптомов связана с конкретными психобиологическими характеристиками и может влиять на результаты лечения. В частности, симптомы накопления с меньшей вероятностью будут реагировать на СИОЗС. Необходима дальнейшая работа, чтобы определить, могут ли пациенты с патологическим накопительством, которые не реагируют на СИОЗС, реагировать на дополнение терапии антагонистами дофамина 81 .
Диагноз ОКР может быть установлен на основании опроса пациента о последствиях отказа от навязчивых действий и оценки вероятности того, что ожидаемые последствия действительно произойдут. Возможно, будет полезно спросить пациента, могут ли возникнуть последствия, которых он опасается, для кого-то другого, чтобы оценить их мыслительный процесс без влияния их собственного беспокойства по поводу невыполнения принуждений. ОКР может быть формально оценено с помощью шкалы оценки убеждений Брауна 82 . Пациенты с ОКР с формальной критикой к своему состоянию реже обращаются к психиатру, и могут хуже реагировать на фармакотерапию и психотерапию 83 . Таким пациентам могут потребоваться дополнительные вмешательства, такие как семейная психотерапия 84 и антагонисты дофамина 85 .
Если у пациентов с ОКР есть текущие или прошлые тики, важно определить, являются ли компульсии похожими на тики (например, прочищение горла) или направлены на снижение тревоги (например, мытье рук после ощущения загрязнения). ОКР, связанное с тиками, характеризуется рядом особенностей, включая раннее начало, чаще возникает у мужчин, семейный анамнез тиков и чаще наличие симптомов, связанных с реакцией на раздражитель (или предчувствие сенсорных симптомов) или перфекционизмом. Тяжесть тика может быть формально оценена с помощью ряда мер 86 . Тикоподобные компульсии плохо реагируют на стандартную терапию и могут лучше реагировать на аугментацию антагонистами дофамина 83 .
Был предложен ряд других подтипов ОКР, включая ОКР с ранним началом 83 . Хотя такая работа была полезна для лучшего понимания гетерогенности ОКР, нет достаточных доказательств того, что такое подтипирование имеет клиническую ценность.
Что касается панического расстройства, было обнаружено, что различные панические симптомы могут объединяются в несколько кластеров, включая респираторные, ночные, когнитивные и вестибулярные симптомы 31 . Исследование физиологии дыхания при паническом расстройстве было особенно полезно для углубления понимания нейробиологии этого состояния 87 . Тем не менее нет убедительных доказательств того, что какой-либо из этих подтипов обладает особой психобиологией, равно как и нет убедительных доказательств того, что какой-либо из них обладает избирательным ответом на лечение 88 . Однако возможно, что более обширное исследование приведет к более конкретным рекомендациям по лечению подтипов панического расстройства.
ПТСР диагностируется в DSM-5 с использованием двадцати симптомов, которые делятся на 4 подгруппы, а именно: навязчивое повторное переживание события (5 симптомов), избегающее поведение (два симптома), нарушения когнитивных процессов и эмоционального состояния (7 симптомов) и изменения в возбуждении и реактивности нервной системы (6 симптомов). Хотя уже давно было высказано предположение, что различные проявления ПТСР подкрепляются различными нейробиологическими механизмами 89,90 , похоже, что существуют сильные генетические корреляции между группами симптомов ПТСР и что эффективная фармакотерапия ПТСР уменьшает выраженность симптомов из различных групп 91 . Как отмечалось ранее, назначение противосудорожных препаратов было связано с избегающим поведением, антидепрессантов – с симптомами оцепенения, анксиолитиков – с интрузиями, а стабилизаторов настроения – с гипервозбуждением 71 , но необходима дальнейшая работа для наработки доказательной базы для принятия таких решений.
Была выдвинута гипотеза о существовании диссоциативного подтипа ПТСР с характерной нейробиологией 92 . Этот подтип может характеризоваться чрезмерной модуляцией аффекта, а не его демодуляцией с повторным переживанием и симптомами гипервозбуждения. Большинство клиницистов оценивают диссоциацию по психиатрическому анамнезу, но может быть полезно использовать формальный инструмент, такой как Шкала диссоциативных переживаний (DES) 93 . DES-II – это самоопросник по 28 пунктам, который оценивает частоту диссоциативных переживаний в повседневной жизни, при этом баллы выше 30 считаются высокими 94 .
Запись сеансов лечения для последующего просмотра может быть полезна для пациентов с симптомами диссоциации, а также частые приостановки, перерывы, более медленное продвижение к содержанию психотравмирующего события, чтобы не перегружать пациента. Кроме того, в соответствии с гипотезой о том, что диссоциация связана с избеганием, есть доказательства того, что при наличии диссоциации когнитивная процессинговая терапия должна включать компонент экспозиции 95 . Конструкция "комплексного ПТСР" по МКБ-11 характеризуется повышенным уровнем ранней детской травмы и диссоциативных симптомов, но необходима дальнейшая работа, чтобы определить, какие конкретные вмешательства улучшат результаты при этом состоянии 96 .
В DSM-IV диагноз социальное тревожное расстройство ставился на основании более обобщенных критериев, относящихся к пациентам с более широким спектром социальных страхов. В DSM-5 был введен диагноз социофобия, для которого характерен страх преимущественно перед публичными выступлениями. Существует мнение, что социальное тревожное расстройство варьируется от страха перед конкретной ситуаций до обширного спектра ситуаций, вызывающих страх, и что болезнь у пациентов с большим спектром страхов протекает тяжелее, и что такие пациенты хуже реагируют на терапию 97 . Предварительные результаты исследований показывают, что пациенты с социальным тревожным расстройством могут реагировать на бета-адреноблокаторы (такие как пропранолол или атенолол) 98 .
С другой стороны, СИОЗС могут быть полезны пациентам с любой степенью тяжести социального тревожного расстройства 99 . Когнитивно-поведенческая терапия, по-видимому, эффективна при всех типах социальной тревожности.
Специфические фобии включают тип “животные” (например, пауки, насекомые, собаки), тип "кровь-инъекция-травма" (например, иглы, инвазивные медицинские процедуры), тип “естественная среда” (например, высота, шторм, вода), ситуационный тип (например, самолеты, лифты, закрытые помещения) и «прочие» типы (например, фобическое избегание ситуаций, которые могут привести к удушью, рвоте или заражению болезнью). Экспозиционные техники (техники воздействия?), адаптированные к конкретным фобиям, полезны для этого диапазона типов специфических фобий.
В отличие от других фобий, которые приводят к стойкой тахикардии в ответ на пугающие сигналы, при типе "кровь-инъекция-травма" у некоторых пациентов может наблюдаться дифазная реакция с начальным повышением частоты сердечных сокращений, за которым следует вазовагальная брадикардия и, в некоторых случаях, обморок 100,101 . Если пациенты теряют сознание при воздействии сигналов, экспозиционную терапию можно проводить в положении пациента лежа. Может быть полезно обучение пациентов технике изометрического напряжения мышц, которая может помочь повысить артериальное давление во время воздействия на них сигналов, которых они опасаются 102 .
Ситуативный тип специфической фобии часто пересекается с агорафобией и/или паническим расстройством и поэтому обычно требует когнитивных методов в дополнение к воздействию.
ТЯЖЕСТЬ
Оценка тяжести симптомов тревоги является важным компонентом обследования пациентов с тревогой или связанными с ней состояниями.
В DSM-5 включены критерии тяжести симптомов для каждого из тревожных и связанных с ними расстройств, а некоторые стандартизированные показатели симптомов широко используются в клинической практике и исследованиях. К ним относятся GAD-7 38 и Пенсильванский опросник оценки уровня беспокойства 53 для ГТР; Y-BOCS54 для ОКР (Обсессивно-компульсивная шкала Йеля-Брауна); шкала тяжести панического расстройства 57 и шкала паники и агорафобии 58 для панического расстройства; опросник мобильности для агорафобии 56 и Олбанский опросник паники и фобии 55 для агорафобии; PCL-5 59 и CAPS-5 60 для ПТСР; программа обследования страхов 63 для специфических фобий; опросник социальной тревоги и социофобии 61 и шкала социальной тревожности Либовица 62 для социофобии (Таблица 2).

Измерение тяжести симптомов тревоги полезно по ряду причин. Во-первых, учет всего спектра тяжести симптомов актуален для моделей предоставления лечения, основанных на ступенчатом подходе. Стратифицированная ступенчатая помощь предлагает менее интенсивное лечение (например, цифровую терапию) тем, у кого симптомы менее выражены, в то время как тем, у кого симптомы более выражены, предлагается более интенсивное лечение 103-105 . Интенсивные подходы, включая посещение на дому или госпитализацию, могут быть необходимы при агорафобии, когда пациенты не могут покинуть свой дом, для пациентов с ОКР, когда ритуалы делают их дома небезопасными или препятствуют посещению клиники, или когда они страдают тяжелым пренебрежением к себе в результате своих симптомов, или для пациентов с ПТСР, у которых настолько тяжелые симптомы, что они не могут посещать сеансы амбулаторного лечения.
Во-вторых, определение тяжести симптомов во время лечебных визитов помогает направлять врача и пациента, позволяя им реагировать на утяжеление симптомов и положительно влиять на результаты лечения 106,107 . Были внедрены практические подходы к лечению тревоги как у взрослых, так и у детей на основе шкал, и это обещает способствовать улучшению персонализированного ухода и повышению эффективности лечения 108,109 .
В-третьих, клинические рекомендации по лечению тревожных расстройств могут рекомендовать выбор лечения в зависимости от тяжести симптомов. Это согласуется с высказанным выше замечанием о том, что легкие симптомы могут поддаваться менее интенсивному лечению, в то время как более тяжелые симптомы могут потребовать более интенсивной терапии, включая использование более одного метода лечения.
Тяжесть ГТР может быть оценена с помощью GAD-7 (самоопросник) и оценочной шкалы тревоги Гамильтона (интервью). В GAD-7 баллы 5, 10 и 15 могут быть интерпретированы как обозначающие легкий, умеренный и тяжелый уровни тревоги: увеличение баллов по шкале тесно связано с ухудшением функциональных нарушений и увеличением числа дней нетрудоспособности 39 . В шкале Гамильтона баллы 9, 15 и 24 могут быть интерпретированы как представляющие нижние границы пограничного, легкого и умеренного уровня тревоги соответственно 110 . Увеличение тяжести симптомов линейно связано с увеличением функциональных нарушений в трех областях шкалы инвалидности Шихана (см. ниже) 111 .
Гайдлайн Национального института здравоохранения и совершенствования медицинской помощи Великобритании (NICE) по ведению пациентов с ГТР рекомендует при легкой степени тяжести тревоги первоначально провести период активного мониторинга, так как симптомы часто проходят без необходимости вмешательства. Если симптомы не исчезли после периода активного наблюдения, следует предложить низкоинтенсивные психологические вмешательства (по существу, самопомощь или психолого-педагогические подходы). При наличии выраженных функциональных нарушений или когда симптомы не устраняются с помощью низкоинтенсивных психологических вмешательств, следует предлагать либо высокоинтенсивные психологические вмешательства (КПТ или прикладная релаксация), либо медикаментозное лечение (обычно СИОЗС), в зависимости от пожеланий человека 112 .
При ОКР тяжесть симптомов может быть оценена с помощью Y-BOCS: у взрослых баллы 14, 26 и 35 могут указывать на нижние пределы умеренной, среднетяжелой и тяжелой интенсивности симптомов соответственно 113 . Увеличение тяжести симптомов, как правило, связано с увеличением уровня инвалидности. Тяжесть симптомов является одним из нескольких важных клинических факторов, которые следует учитывать при выборе лечения 69 . Некоторые гайдлайны указывают, что тяжесть влияет на выбор между фармакотерапией и психотерапией (например, психотерапия является первой линией вмешательства при легкой форме ОКР, а фармакотерапия применяется, когда КПТ не эффективна) 114 , другие гайдлайны указывают, что фармакотерапия и психотерапия могут использоваться независимо от уровня тяжести симптомов при ОКР 69 .
При посттравматическом расстройстве оценка тяжести симптомов может быть сложной, так как требуется комплексно оценить расстройства различных отделов организма. Наиболее широко используемым показателем тяжести симптомов является Шкала клинической оценки посттравматического стрессового расстройства для DSM-5 60 , которая включает 30 пунктов, оценивающих тяжесть симптомов за предыдущую неделю. Пациенты с ПТСР с тяжелыми симптомами могут испытывать больше трудностей во время когнитивно-поведенческой терапии. Однако интенсивные амбулаторные программы, в которых ежедневно участвуют пациенты с ПТСР, могут увеличить показатели удержания до 90% 115,116 , с соответствующим уменьшением как симптомов ПТСР, так и суицидальных мыслей 117 .
НЕЙРОКОГНИЦИЯ
Нейрокогниция представляет собой один из ключевых механизмов, с помощью которого изменения в структуре и функциях мозга в конечном итоге приводят к появлению клинических признаков и симптомов. Находясь ближе к предполагаемому биологическому субстрату и будучи измеримыми с помощью объективных тестов, нейрокогнитивные маркеры могут быть более надежными, последовательными и устойчивыми, чем изменчивая симптоматика расстройства 118-120 . Нейрокогнитивное тестирование у пациентов с ОКР и связанными с ним расстройствами, например, использовалось для характеристики аномалий лобно-височных долей 121 , а также для выявления предполагаемых подтипов с различной структурой мозга, функциями 122 .
Клиническая оценка нейрокогнитивных способностей при тревоге и связанных с ней расстройствах получила импульс благодаря разработке более надежных нейрокогнитивных тестов с адекватной специфичностью и чувствительностью для областей, имеющих отношение к этим состояниям, а также благодаря технологическим достижениям, использование компактных компьютеризированных батарей, которые относительно дешевы и просты в применении с небольшой нагрузкой на пациентов и персонал. Такое тестирование может способствовать оценке и диагностике, а также может использоваться для мониторинга эффективности лечения (хотя некоторые нейрокогнитивные нарушения, по-видимому, не изменяются, когда симптомы реагируют на вмешательство, представляя собой маркеры уязвимости кандидатов, которые также встречаются у бессимптомных родственников первой степени у таких пациентов) 8,123 .
Когнитивные тесты чаще используются при ОКР, чем при других тревожных расстройствах. В систематическом обзоре и метаанализе статей о биомаркерах-кандидатах для ОКР только когнитивные показатели показали убедительные или весьма убедительные подтверждающие результаты (доказательства класса 1 или 2) 124 . Кроме того, оценка с использованием стандартизированных инструментов самоотчета, таких как Инструмент когнитивной оценки навязчивых идей и компульсий (CAIOC-13) 125 , шкала из 13 пунктов, показывает широкий спектр функциональных нарушений при ОКР, которые, как считается, являются следствием когнитивных трудностей, которые мешают многим аспектам повседневной жизни. Поскольку эти недостатки легко упускаются из виду, недавнее экспертное исследование рекомендовало рутинную когнитивно-функциональную оценку с использованием таких шкал, как CAIOC-13, в клинической оценке для пациентов с ОКР 126 .
В будущем есть надежда, что нейрокогнитивное тестирование может быть использовано для выявления тревожных расстройств даже до появления симптомов 126 и для априорного прогнозирования реакции на лечение, улучшения эффективности терапии 124 . Оценка когнитивной негибкости, вероятно, будет иметь особое значение для прогнозирования результатов лечения ОКР. Тем не менее доказательства остаются весьма предварительными, и лишь в нескольких небольших исследованиях ОКР показан общий или дифференциальный ответ на фармакотерапию или КПТ в зависимости от степени когнитивной гибкости при выполнении задач по смене заданий 127 .
ФУНКЦИОНИРОВАНИЕ И УРОВЕНЬ ЖИЗНИ
Оценка функционирования и качества жизни пациентов с тревожными расстройства важна по нескольким причинам, рассмотренным в предыдущем разделе о тяжести симптомов. Во-первых, влияние расстройства на эти области помогает определить, следует ли использовать стандартное амбулаторное лечение или требуются более интенсивные подходы. Во-вторых, оценка функционирования и качества жизни является частью медицинской помощи, основанной на измерениях. Имеются убедительные доказательства того, что лечение тревоги и связанных с ней расстройств позитивно влияет на функционирование и повышает уровень жизни 128 . В-третьих, рекомендации по лечению тревожных расстройств могут частично основываться на степени функциональных нарушений. Хотя тяжесть симптомов, функциональные нарушения и качество жизни демонстрируют значительные корреляции, важно отметить, что у любого конкретного пациента они могут быть не полностью согласованы, и, следовательно, каждая конструкция нуждается в независимой оценке 129,130 .
Согласно Всемирной организации здравоохранения, качество жизни – это восприятие индивидом своего положения в жизни в контексте культуры и систем ценностей, в которых он живет, и в соответствии с его целями, ожиданиями и проблемами. Таким образом, оценку качества жизни можно отличить от измерения функциональных нарушений и инвалидности, связанной с симптомами, по ее направленности на субъективное переживание удовлетворенности текущим функционированием и сопутствующее чувство общего благополучия.
Оценка качества жизни в идеале должна охватывать как общие, так и конкретные показатели, чтобы обеспечить максимальную чувствительность и обобщаемость. Однако исследования тревожных расстройств, ПТСР и ОКР в основном использовали общие инструменты. Наиболее часто использовались шкала инвалидности Шиэна 131 , Опросник качества жизни и удовлетворенности (Q-LES-Q) 132 и Исследование медицинских результатов по 36 пунктам Краткой формы обследования здоровья (SF-36) 133 , при этом также использовались EuroQol (EQ-5D) 134 и Инвентаризация качества жизни (QOLI) 135 . Шкалы, специфичные для расстройств, включают CAIOC-13 125 для ОКР и обследование здоровья ветеранов Rand 12 (VR-12) для ПТСР 136 .
Некоторые клинические рекомендации по лечению тревоги и связанных с ней расстройств были сосредоточены на функциональных нарушениях. В рекомендациях NICE по ОКР, например, предлагается психологическое лечение низкой интенсивности для пациентов с легкими функциональными нарушениями (или когда пациент предпочитает этот вид лечения), в то время как СИОЗС или более интенсивная КПТ предлагаются в случае умеренных функциональных нарушений 137 .
ЛИЧНОСТНЫЕ ЧЕРТЫ
Среди “классических” черт пятифакторной (Большой пятерки) модели личности, нейротизм, который относится к негативной эмоциональности или стойкой склонности к готовности испытать сильные негативные эмоции, показал наиболее устойчивую связь с тревожностью 138 . Невротизм был связан с усилением симптомов общей тревоги, а также симптомов ОКР, панического расстройства, фобий, ПТСР и социального тревожного расстройства. Согласно трехсторонней модели Clark и Watson 139 , нейротизм является основным фактором риска, общим для тревожных и депрессивных расстройств, при этом дополнительный компонент тревожного возбуждения более специфичен для тревожных состояний, а ангедония более характерна для депрессии 140 .
В клиническом контексте понимание степени и истории негативной эмоциональности пациента как фактора уязвимости может помочь контекстуализировать начальное возникновение и поддержание симптомов тревоги. Если нейротизм влияет на текущее преодоление и функционирование, например, усиливая тревогу и связанные с ней расстройства, его уровни могут быть снижены с помощью психологических методов лечения, основанных на принятии и когнитивно-поведенческих подходах, которые специально нацелены на реакцию на негативные эмоции 141 .
Еще одна черта личности из Большой пятерки, экстраверсия, которая относится к общительности и склонности черпать энергию из взаимодействия с другими, имеет клиническое значение для понимания некоторых тревожных расстройств, включая агорафобию, специфическую фобию и социальное тревожное расстройство 138 . Было обнаружено, что социальная тревожность генетически коррелирует со снижением экстраверсии, но не с нейротизмом 142 . Знание уровня экстраверсии пациента может быть особенно полезным при информировании о лечении социальной тревожности, например, при выборе иерархии социальных воздействий.
Пациенты с генерализованной тревожностью, как правило, имеют более высокий уровень ответственности в сравнении со средним 143 . Высокая ответственность может создать как возможности, так и проблемы для соблюдения режима лечения в ходе психотерапии тревожного или связанного с ним расстройства. Это может привести к более высокому уровню выполнения терапевтических домашних заданий, но также к большему беспокойству и озабоченности по поводу назначенных практик или задач. В последнем случае клинические рассуждения предполагают, что может быть полезно четкое обсуждение реалистичных ожиданий и нормализации постепенного прогресса. Высокий уровень ответственности также может указывать на возможность наличия в основе обсессивно-компульсивного расстройства личности и потенциальную ценность методов лечения, разработанных для этого состояния 144 .
В некоторой литературе указывается, что Пять основных личностных черт лучше всего рассматривать в сочетании, когда дело касается тревожных расстройств, при этом более высокие уровни экстраверсии и сознательности связаны с более низким риском развития тревожных расстройств среди лиц с высоким уровнем нейротизма 145 . В соответствии с этим, более высокие уровни ответственности были связаны с более быстрым восстановлением от негативных эмоций у взрослых 146 , возможно, смягчая последствия невротизма.
Таким образом, клиницист должен обращать внимание на различные комбинации Пяти личностных черт. Если пациент демонстрирует высокий невротизм, но низкую ответственность, он/она может подвергаться особому риску возникновения трудностей с регулированием эмоций и, таким образом, эффективнее могут быть стратегии, направленные на улучшение регуляции эмоций, например, диалектическую поведенческую терапию. Напротив, пациент с высоким нейротизмом, но также с высокой экстраверсией и ответственностью может извлечь выгоду из стандартных стратегий, таких как когнитивная реструктуризация или воздействие. Однако необходимы дальнейшие исследования, чтобы установить, могут ли рекомендации по лечению основываться на оценке Пяти основных признаков.
С точки зрения того, как клиницист должен оценивать личностные черты у тревожного пациента, оценка Пяти основных черт характера была предметом растущего внимания, и доступен ряд проверенных шкал, таких как Инвентаризация личности NEO-3 147 и Инвентаризация Большой пятерки-2 148 . Однако, поскольку эти шкалы являются относительно длинными, клиницисты могут счесть полезным выбрать наиболее релевантные поддомены – такие как нейротизм – для оценки или использовать краткие шкалы личностных качеств (например, Десятибалльный показатель Личности 149 ). При оценке личности клиницисты должны учитывать потенциальные двунаправленные влияния между личностными чертами и тревогой, поскольку наличие тревоги или связанного с ней расстройства может повлиять на переживание и сообщения о невротизме с течением времени 150 .
Важно отметить, что каждая из Пяти основных личностных черт, как предполагается, состоит из “аспектов”, которые в дальнейшем могут оказаться полезными для понимания развития и поддержания симптомов у пациентов с тревожностью. Например, недавние усилия по изучению аспектов личности в рамках нейротизма выявили 5 потенциальных поддоменов, включая тревогу, депрессию, склонность к гневу, соматические жалобы и зависть 151 . Детальная оценка личностных аспектов может указывать на конкретные цели вмешательства, которые могут быть продуктивными в ходе психотерапии, такие как решение соматических проблем с помощью стратегий "разум-тело" или снижение уровня тревоги с помощью когнитивно-поведенческих методов.
Наконец, личностные черты могут проявляться в форме расстройств личности, как описано в DSM-5. В частности, расстройства личности кластера С могут быть чрезмерно представлены у пациентов с тревожными расстройствами: они включают избегающее расстройство личности (характеризующееся социальным торможением и чувствительностью к отвержению); зависимое расстройство личности (характеризуется тревогой разлуки и пассивным поведением); и обсессивно-компульсивное расстройство личности (характеризуется сильной потребностью в порядке и контролем). Расстройства личности кластера С, которые сочетаются с тревогой и связанными с ней расстройствами, могут усложнить лечение, например, мешая проведению лечения в случае избегающего расстройства личности или приводя к чрезмерной зависимости в случае зависимой личности. Эти расстройства личности могут быть оценены с помощью Описи личности для DSM-5 (PID-5) 152 .
ПРЕДШЕСТВУЮЩИЕ И СОПУТСТВУЮЩИЕ ПСИХИАТРИЧЕСКИЕ НАРУШЕНИЯ
Многие люди, страдающие тревожными расстройствами, имеют сопутствующие психические заболевания 153 . Тревожные расстройства занимают относительно центральное место в многомерной области психопатологии 154 , и имеются данные о наличии связи между этими расстройствами и другими психическими расстройствами, особенно с депрессией. Как отмечалось ранее, некоторые рассматривают тревожные и депрессивные расстройства как проявления общей интернализующей психопатологии, которую можно далее разделить на расстройства страха (например, паника, фобия) и дистресса (например, ГТР, ПТСР, депрессия) 155 .
Некоторые авторы выразили озабоченность по поводу того, что сопутствующая патология может быть артефактом наших современных диагностических систем 156 , которую лучше рассматривать как отражение тяжести и/или масштабов основной проблемы, а не как коморбидное возникновение заболеваний. Такая перспектива может подчеркнуть необходимость измерения трансдиагностических конструктов, таких как нейротизм. Примечательно, что в DSM-5 наличие панических атак теперь используется в качестве общего спецификатора (например, социальная тревога с паническими атаками или без них) и может быть полезно для сигнализации тяжести различных расстройств.
Средний возраст начала тревожных расстройств наступает раньше, чем у многих других психических расстройств, что приводит к вопросу о том, как часто тревожные расстройства предшествуют сопутствующим заболеваниям. В Всемирном Исследовании психического здоровья (World Mental Health Survey) был выявлен очень ранний средний возраст начала (7–14 лет) для тревоги сепарации и специфической фобии, в то время как ГТР, паническое расстройство и ПТСР имели гораздо более поздний возраст начала (24–50 лет). Тем не менее в большинстве пар сопутствующих заболеваний тревожные расстройства либо сопутствуют, либо предшествуют другому расстройству. Наиболее четкая картина наблюдается в отношении специфической фобии: она возникает первой в 75% пар сопутствующих заболеваний 153 . С этой точки зрения раннее распознавание и лечение тревожных расстройств могут быть ключевыми для предотвращения развития последующих психических заболеваний 157 . Необходимы дальнейшие исследования, чтобы определить, предотвращает ли лечение специфической фобии возникновение более поздних психиатрических состояний 158 .
Для оценки сопутствующей патологии можно использовать несколько диагностических интервью. SCID-5 полезен, но его проведение занимает около 90 минут и требует значительной подготовки. MINI проводится быстрее, но имеет недостаток в том, что он полностью структурирован. DSM-5 включает “сквозные” показатели симптомов, которые могут быть полезны при скрининге на целый ряд сопутствующих заболеваний. Опросник психиатрического диагностического скрининга (PDSQ) 159 охватывает многочисленные психические расстройства, включая настроение, тревогу, злоупотребление психоактивными веществами, пищевые и соматоформные расстройства.
У людей с тревожным расстройством выявление других психических состояний является ключевым фактором в персонализации ведения. Если эти два состояния считаются независимыми, то оба, скорее всего, потребуют независимого лечения. Если они взаимозависимы, то в игру вступают 5 основных моделей 6 .
Во-первых, последовательная модель: например, у пациента с социальным тревожным расстройством и расстройством, связанным с употреблением психоактивных веществ, стабилизация расстройства, связанного с употреблением психоактивных веществ, может быть приоритетом перед коррекцией тревожного расстройства. Во-вторых, иерархически взвешенная модель (одно лечение может устранить основной фактор, такой как нейротизм, и, таким образом, улучшить сопутствующие заболевания): например, СИОЗС и/или КПТ могут быть полезны при сопутствующих состояниях тревоги и депрессии. В-третьих, модель, взвешенная по степени тяжести (лечение первичного тревожного состояния может исправить любые вторичные состояния или последствия): например, если панические атаки приводят к агорафобии, то лечение, направленное на панические атаки, может быть первым шагом к терапии агорафобии. В-четвертых, модель “мотивационного обхода”: например, человек с пограничным расстройством личности, приводящим к сильной тревоге, может быть не мотивирован проходить психотерапию, но может быть готов принимать лекарства от тревоги, что также может оказать положительное влияние на импульсивные черты личности. В-пятых, модель управления рисками: например, если у человека с ПТСР развилось расстройство, связанное с употреблением психоактивных веществ, и он проявляет сильную агрессию, то госпитализация и другие соответствующие стратегии, нацеленные на безопасность пациента и семьи, могут быть первоочередной задачей.
Несмотря на наличие существенной доказательной базы по лечению тревожных расстройств, а также растущей доказательной базы по ведению пациентов с сопутствующей патологией, любому конкретному пациенту требуется индивидуальная оценка, взвешивание возможных причинно-следственных моделей для оптимального решения этих проблем.
СОПУТСТВУЮЩИЕ СОМАТИЧЕСКИЕ НАРУШЕНИЯ
Тревожные расстройства могут возникать как следствие физического расстройства, предшествовать физическому расстройству или быть сопутствующим явлением.
Широкий спектр физических расстройств может привести к симптомам тревоги или усугубить их, с некоторыми признаками специфичности для тревоги и связанных с ней расстройств. Так, например, существуют важные причинно-следственные связи между респираторными заболеваниями и паническим расстройством 87 . Было высказано предположение (хотя оспариваемое), что существуют причинно-следственные связи между паническим расстройством и целым рядом физических состояний, включая пролапс митрального клапана 160 и гипермобильность суставов 161 . Кроме того, особое внимание уделялось роли черепно-мозговой травмы при ПТСР 162 и роли некоторых инфекций при ОКР 163 .
Большинство исследований, посвященных физической сопутствующей патологии при тревожных расстройствах, сосредоточены на сердечно-сосудистых заболеваниях. Метаанализ показал, что у людей с пожизненным диагнозом тревожного расстройства на 60% повышен риск возникновения сердечно-сосудистых заболеваний 164 . Примечательно, что риск тревожного состояния существенно возрастает после острого заболевания, например острого инфаркта миокарда. Осведомленность о событии болезни может сыграть важную роль, поскольку “тихий” инфаркт миокарда (при котором человек не знает о сердечном событии 165 ) не сопровождается повышенным риском развития тревожных состояний, в отличие от явного инфаркта. Тревога после инфаркта миокарда, в свою очередь, связана с негативными сердечно-сосудистыми последствиями 166 .
Несмотря на значительное внимание к связи между тревожными расстройствами и сердечно-сосудистыми заболеваниями, наличие причинно-следственной связи еще предстоит доказать. Возможно, что еще более важно, эта ассоциация не является специфичной, поскольку тревожные расстройства связаны с целым рядом физических расстройств, с коэффициентами риска в диапазоне 1,17–1,73 для 10 групп состояний и между 1,13 и 2,40 для отдельных состояний 167 . Связь тревожных расстройств с сердечно-сосудистыми заболеваниями находится только в середине этого диапазона. Другими словами, чрезмерное внимание к сопутствующей патологии тревожных расстройств с сердечно-сосудистыми заболеваниями не оправдано, и внимание следует распространить на другие физические состояния.
Учитывая отсутствие специфичности в ассоциациях тревожных расстройств с физическими заболеваниями, мы подчеркиваем важность скрининга и оценки физических расстройств у всех пациентов с тревогой и связанными с ней расстройствами, а также уделения особого внимания возможности того, что физические условия играют причинную роль в развитии тревожных расстройств, особенно у пациентов с необычными или рефрактерными проявлениями 168 . Более конкретные рекомендации относительно оценки физического состояния были даны при депрессии, которая часто сопровождается тревогой и связанными с ней расстройствами 6 . Эти рекомендации согласуются с общим акцентом на интеграцию психического здоровья в лечение неинфекционных заболеваний, включая выявление и устранение поддающихся изменению факторов риска, таких как употребление табака, нездоровое питание, отсутствие физической активности и вредное употребление алкоголя 169,170 .
Клиницисты должны учитывать, как конкретные симптомы тревоги пациента могут повлиять на взаимодействие с медицинскими учреждениями. Например, беспокойство может привести к тому, что пациенты не обратятся за помощью по поводу симптомов физического здоровья, или затруднить посещение ими медицинских осмотров. С другой стороны, определенные тревожные опасения (например, беспокойство по поводу здоровья) могут привести к многочисленным обращениям к врачу, где чрезмерная диагностика может привести к усилению основных проблем, связанных с тревогой. В этих обстоятельствах могут быть уместны такие меры, как опросник Краткий перечень проблем со здоровьем 171 , и адекватный подбор методов лечения 172 .
Когда педиатрический острый нейропсихический синдром (PANS) подозревается в качестве причины возникновения симптомов ОКР, требуется провести всестороннее психиатрическое и физическое обследование 163 , и в дополнение к стандартным методам лечения ОКР может быть рассмотрена специфическая иммунотерапия 173 . Учитывая высокие показатели совместного возникновения ПТСР и черепно-мозговой травмы, может быть рекомендован скрининг на это состояние у пациентов с ПТСР: появляется все больше литературы, демонстрирующей, что существующие методы лечения ПТСР эффективны в этой популяции 174 , но может потребоваться дополнительное выявление симптомов травмы головного мозга. Оценка и лечение обструктивного апноэ во сне может улучшить лечение ПТСР.
В целом наличие сопутствующих физических заболеваний требует целенаправленного лечения. Это может включать мероприятия, ориентированные на конкретные заболевания, а также на формирование здорового образа жизни. Примечательно, что появляется все больше свидетельств того, что занятия физической активностью защищают от тревожных симптомов и расстройств 175 . Однако доказательства эффективности аэробных упражнений, а также ряда подходов к дополнительной и альтернативной медицине в лечении тревоги и связанных с ней расстройств остаются предварительными 176,177 .
СЕМЕЙНЫЙ АНАМНЕЗ
Известно, что тревога и связанные с ней расстройства возникают в семьях, и повышенный риск развития тревожных состояний среди родственных лиц, начиная от ГТР и заканчивая ОКР, фобиями и паническим расстройством, хорошо задокументирован в клинических и популяционных выборках 178 .
Знание семейного анамнеза – где это возможно, включая конкретных пострадавших родственников, их отношения к пациенту, возраст начала и течение расстройства – может помочь клиницисту понять текущее состояние пациента и помочь пациенту контекстуализировать его/ее текущие и прошлые проблемы с тревогой.
Метааналитические данные показывают, что наличие родственника первой степени с любым тревожным расстройством может увеличить развития тревожного расстройства в 4–6 раз. Этот риск может быть аналогичным образом повышен независимо от того, является ли родственник первой степени родителем, братом или сестрой или ребенком, что позволяет предположить, что систематический опрос о ряде членов семьи может быть наиболее информативным. Это семейное накопление тревожных расстройств было в значительной степени обусловлено генетическими факторами, причем исследования близнецов показали, что наследуемость тревожных состояний составляет от 30 до 40% 178 .
Исследования показали, что специфические для расстройств паттерны семейной передачи, при которых семейная история определенного тревожного расстройства более тесно связана с повышенным риском возникновения этого же расстройства, а также других тревожных расстройств или психопатологий. Там, где это уместно, специфичность этого расстройства может быть информативной для дифференциальной диагностики тревожных состояний, поскольку сообщенная история нескольких членов семьи с данным расстройством может указывать на аналогичный диагноз, который следует учитывать. Эта специфичность была продемонстрирована для ОКР, панического расстройства, социального тревожного расстройства и в некоторых случаях ГТР 179 .
Сбор семейного анализа у самих взрослых пациентов является наиболее простым подходом, но такую информацию также можно получить от членов семьи. Исследование, сравнивающее прямое интервью с отчетами членов семьи, показало удовлетворительное согласие между информантами. Данные свидетельствуют о том, что, когда люди положительно подтверждают семейную историю тревожного или связанного с ним расстройства у одного или нескольких своих родственников, эту информацию можно считать достоверной; однако клиницисты должны иметь в виду, что люди могут не знать о тревоге и других психических состояниях у своих родственников, и сообщения могут быть предвзятыми из-за различных характеристик пациентов 180 .
Для повышения точности исследования было рекомендовано использовать несколько информантов, но это может быть сложно в стандартных клинических обследованиях. Относительно короткие инструменты скрининга для семейной психиатрической истории, такие как Скрининг Семейной Истории 181 , занимают от 5 до 20 мин и могут быть более осуществимыми в клинической практике.
Важно отметить, что положительный семейный анамнез был связан не только с развитием тревоги или связанного с ней расстройства в течение всей жизни, но и со значимыми клиническими изменениями в болезни. Например, проспективное когортное исследование показало, что семейный анамнез тревожного расстройства был связан с большей повторяемостью тревоги и ухудшением функционирования, а также с большим количеством посещений врача в течение взрослой жизни 182 . Таким образом, оценка семейного анамнеза может поспособствовать лучшему прогнозированию и помочь с подбором терапии.
РАННИЕ СРЕДОВЫЕ ФАКТОРЫ
Широкий спектр ранних воздействий окружающей среды был изучен в связи с тревожными расстройствами. К ним относятся перинатальные осложнения, сезон рождения, социально-экономический статус, методы воспитания родителей, инфекции и черепно-мозговая травма. Исследования характеризовались методологическими ограничениями, и выводы остаются предварительными 183-185 . Тем не менее следует особо оценить ряд ранних воздействий на окружающую среду, поскольку они могут повлиять на планирование лечения.
Во-первых, появляется все больше свидетельств того, что острое начало обсессивно-компульсивных симптомов в детском возрасте иногда может быть вызвано стрептококковыми инфекциями (т.е. аутоиммунными психоневрологическими расстройствами, связанными со стрептококковыми инфекциями, PANDAS) или широким спектром других заболеваний (например, PANS). Как отмечалось ранее, при подозрении на PANS требуется всестороннее психиатрическое и физическое обследование 163 , и в таких случаях имеет смысл рассмотреть дополнение стандартного лечения специфической иммунотерапией 173 .
Во-вторых, растущая база фактических данных подтверждает связь между трудностями в раннем детстве и последующим развитием тревожных расстройств. Примеры включают физическое и сексуальное надругательство 186,187 , разлуку с родителями 188 и эмоциональное жестокое обращение 189 . Большее количество серьезных невзгод в детстве и подростковом возрасте предсказывало последующее возникновение тревожных расстройств в течение следующих нескольких лет в выборке поздних подростков 190 . Данные Всемирных обследований психического здоровья показывают, что снижение уровня насилия над детьми приводит к снижению распространенности тревожных расстройств на 31% 191 . В литературе по-прежнему изучается ряд вопросов, включая ассоциации различных типов ранних психологических травм с тревогой, возрастом, когда была нанесена психотравма, причинно-следственные связи между такими травмами и развитием тревоги, а также ассоциации детских травм с различными клиническими особенностями тревоги.
Учитывая важность этой связи, оценка истории детских травм должна быть частью комплексной диагностики пациентов с тревожными расстройствами. Как обсуждалось в связи с депрессией, при оценке ранних психологических травм у пациента с тревожностью 6 необходимо учитывать ряд ключевых вопросов. Во-первых, сообщения о неблагоприятных обстоятельствах в значительной степени субъективны, и существует вероятность предвзятого отзыва. Во-вторых, важно исследовать не только произошедшие события, но и ключевые аспекты субъективного опыта и присвоенный смысл. В-третьих, личность и социокультурный фон могут влиять как на опыт, так и на сообщения о детских травмах. Анализ истории детских психотравм, который акцентируется на преодолении трудностей и устойчивости, может быть полезен для решения этих проблем.
Детский опыт заботы и жестокого обращения (CECA) 192 представляет собой комплексный опрос для оценки наличия неблагоприятных условий в детстве. Он позволяет подробно собрать информацию, но для его проведения требуется много времени, подготовка интервьюера, а информация о его клинической полезности ограничена. Несколько более коротких анкет для самоотчета были использованы в исследовательских целях и могут быть рассмотрены в клинической практике. К ним относятся более короткий опросник для самоотчета, основанный на CECA (CECA.Q) 193 , и Опросник детской травмы (CTQ) 194 . Краткая форма CTQ содержит 28 пунктов, оценивающих 5 причин возникновения детских психотравм: эмоциональная холодность, недостаток физических контактов, эмоциональное насилие, физическое насилие и сексуальное насилие.
Существует ряд мер для оценки моделей поведения молодых родителей. Опросник молодых родителей (YPI) используется в схемной терапии и служит полезным способом оценки стилей воспитания и того, как они могут быть связаны с ранними неадаптивными схемами индивидуума 195 .
В опроснике содержится 72 пункта, которые ретроспективно оценивают воспринимаемый опыт воспитания в отношении каждого воспитателя. Этот показатель предназначен для использования в сочетании со схематическим опросником молодых родителей (YSQ) 196 , в котором оценивается восемнадцать ранних неадаптивных схем воспитания.
Хотя большая часть потенциально значимой доказательной базы базируется на данных работы, посвященной депрессиям 6 , наличие ранних неблагоприятных факторов может повлиять на планирование лечения тревожных расстройств несколькими способами. Во-первых, наличие ранних неблагоприятных последствий может быть связано с преждевременным прекращением лечения, возможно, из-за слабого терапевтического альянса. В таких случаях представляется целесообразным уделять особое внимание совместному принятию решений. Во-вторых, можно рассмотреть конкретные основанные на фактических данных методы психотерапии, разработанные для пациентов с детскими психотравмами, такими как, например, проработка детских травм. В-третьих, возможно, что ранние неблагоприятные условия приводят к снижению реакции на лечение, что указывает на необходимость смены тактики.
ПОЗДНИЕ СРЕДОВЫЕ ФАКТОРЫ
Широкий спектр факторов, вызывающих стресс в окружающей среде, связан с повышением уровня тревожности 197 . К ним относятся статус меньшинства (особенно связанный с риском развития ПТСР, который был обусловлен опытом дискриминации и изоляции), нестабильность доходов, безработица, бездомность, стихийные бедствия, вооруженные конфликты, преступность и переселение.
Люди, имеющие детские психотравмы, больше подвержены тревожным состояниям, развивающимся от более слабых стрессоров (т.е. сенсибилизация к стрессу). Например, данные Национального эпидемиологического обследования по алкоголю и связанным с ним состояниям (NE-SARC) показали, что степень влияния стрессовых жизненных событий прошлого года на риск развития тревожных расстройств и ПТСР была усилена наличием детских травм, особенно трех или более 198 . На степень влияния так же влияет пол, поскольку для повышения чувствительности к стрессу у женщин по сравнению с мужчинами требовалось меньше основных жизненных стрессоров.
Данные близнецовых исследований показывают, что почти все виды средового влияния подвержены генетическому влиянию (например, генетическая склонность к рисковому поведению может привести к увеличению воздействия опасных сред) 199 . Доказательства влияния генетики на стресс до сих пор слабы, а данные близнецовых исследований указывают на отсутствие умеренных эффектов взаимодействия 200,201 . Полногеномные методы дали многообещающие начальные результаты: например, было обнаружено, что полигенный показатель эмоциональной отзывчивости к окружающей среде взаимодействует с негативным воспитанием, вызывая более выраженную тревожную симптоматику 202 .
Учет непосредственных жизненных стрессоров важен при оценке тревожных расстройств. Полуструктурированные интервью включают в себя Шкалу жизненных событий и трудностей (LEDS) 203 , которая оценивает объективные аспекты жизненных событий и воздействие хронических стрессоров, а также субъективный опыт человека о том, насколько угрожающими или разрушительными они были. Другим полезным инструментом является Интервью Жизненного Стресса Калифорнийского Универститета 204 , в котором оценивается как хронический, так и эпизодический стресс, а также оценивается их степень влияния в контексте других жизненных обстоятельств. Для обоих вариантов интервью требуется подготовка.
Ряд самоопросников для оценки жизненных событий и воздействия хронических стрессоров может быть пригоден для использования в клинической практике. К ним относятся Психиатрическая Эпидемиологическая Исследовательская Шкала (PERI-LES) 205 , Опросник по угрожающим переживаниям (LTE) 206 и Опросник стрессовых жизненных событий (QSLE) 207 . Все они обладают хорошими или сильными психометрическими свойствами. В PERI-LES перечислены 102 события, и он широко использовался в эпидемиологических исследованиях. LTE был специально разработан кратким. Он оценивает всего двенадцать недавних событий в жизни, которые связаны с долгосрочной угрозой. QSLE был разработан, чтобы охватить все периоды жизни, в нем оценивается восемнадцать жизненных событий, которые происходят в детстве, подростковом возрасте и взрослой жизни, и их влияние. Дискриминацию можно оценить с помощью самоопросника Шкала повседневной дискриминации 208 .
Стрессовые жизненные события и хронические стрессоры могут влиять на клиническое ведение несколькими способами. Во-первых, они могут препятствовать самообслуживанию и приверженности/реагированию на медицинскую помощь, особенно в сочетании с высокими личными требованиями (такими как высокие школьные или должностные обязанности) 209 . Например, практика выполнения домашних заданий КПТ может выполняться реже в зависимости от жизненных стрессоров, и, хотя практика когнитивных и поведенческих навыков важна для общих показателей успеха, учет препятствий для выполнения практик необходим для адекватного лечения.
Во-вторых, высокий уровень хронического стресса может привести к стойкой сенсибилизации гипофизарно-надпочечниковой оси и вегетативной нервной системы 210 , тем самым способствуя усилению физиологических и когнитивных нарушений, уже присутствующих у лиц с тревожными расстройствами. Сочетание высокого возбуждения и дефицита внимания может снизить восприятие информации, относящейся к лечению, будь то информация о лекарствах или когнитивных и поведенческих навыках. Стратегии регулирования возбуждения (например, переподготовка дыхания, расслабление мышц, тренировка осознанности) могут иметь особую ценность для человека, сталкивающегося со значительными жизненными стрессорами.
В-третьих, для некоторых людей травматический опыт может потребовать терапии, сфокусированной на травму, нацеленной на навязчивые и тревожные воспоминания, а также на поведенческие и физиологические последствия.
С другой стороны, понимание контекстуальных факторов, таких как соседское насилие, может смягчить терапевтический подход к травматизации; например, воздействие in vivo на области, которые напоминают о травме, будет противопоказано всякий раз, когда существует вероятность повторной травмы.
В-четвертых, знание о недавних жизненных стрессорах может помочь в подборе психологического лечения. Например, пациенты с паническим расстройством иногда сообщают о медицинских травмах у себя или других членов семьи, которые вызывают у них боязливую реакцию на телесные ощущения. Понимание этих медицинских травм может помочь клиницисту наиболее эффективно адаптировать когнитивную перестройку в отношении личного риска или спроектировать воздействия 211 . Аналогичным образом, пациенты с социальным тревожным расстройством, которые недавно были уволены с работы, могут испытывать повышенное восприятие отвержения, и эта информация может способствовать адаптации практики когнитивных навыков.
ЗАЩИТНЫЕ ФАКТОРЫ/УСТОЙЧИВОСТЬ
Факторы защиты и устойчивости, как правило, могут быть сгруппированы на индивидуальные личностные черты и на поддерживающие факторы окружающей среды, хотя эти два фактора, вероятно, будут взаимосвязаны, поскольку люди с устойчивыми чертами характера могут самостоятельно выбирать благоприятную среду и вести свою жизнь таким образом, чтобы увеличить устойчивость к стрессу.
Экстраверсия – это индивидуальная черта, которая, как показано, действует как защитный фактор при тревожных расстройствах (см. выше). Одним из аспектов экстраверсии являются положительные эмоции, такие как счастье, радость, заинтересованность, уверенность. Было показано, что они способствуют гибкости мышления и решению проблем, уменьшают физиологические последствия негативных эмоций, создают устойчивые социальные ресурсы, способствуют эффективным стратегиям преодоления и создают условия улучшения эмоционального благополучия 212 .
Высокий уровень позитивного влияния черт характера действовал как защитный фактор в смягчении клинической картины тревожных расстройств в перспективе и как защитный фактор, уменьшая последствия стрессовых жизненных событий и риска развития социального тревожного расстройства 213 . Черты характера, которые, как было показано, снижают риск тревожных расстройств у подростков, включают оптимизм, воспринимаемую компетентность и адекватную самооценку 214 .
В обзоре защитных факторов тревожных расстройств среди взрослых в общей популяции также были выделены уровни физической активности и стили преодоления стрессовых событий (способы реагирования на воспринимаемые стрессоры) 215 .
Благоприятная межличностная среда может выступать в качестве защитного фактора от стрессовых воздействий. Предполагается, что гармоничные межличностные отношения способствуют благополучию за счет расширения социальных контактов и связей, а также доступа к ресурсам. Защитная функция социальной поддержки была продемонстрирована в различных контекстах риска, включая испытанное насилие в детстве 216 . Социальная поддержка также связана со снижением риска развития тревожных расстройств в перспективе 214,217 и может смягчить развитие ПТСР после воздействия травмы. Учитывая роль низкого финансового благополучия в развитии тревожности 197 , неудивительно, что наличие работы коррелирует с уменьшением симптомов депрессии и тревоги и снижением риска самоубийств, особенно среди мужчин 218-220 .
Всестороннее клиническое интервью для пациентов с тревожностью и связанными с ней расстройствами должно охватывать защитные факторы и устойчивость. Как описано в случае с депрессией 6 , аббревиатура SOCIAL помогает выделить основные защитные факторы: Социальные ресурсы, включая друзей, группы и социальное влияние (S); Место работы (оплачиваемое или нет) (O); Детей и семью (С); Доходы и источники материальных ресурсов (I); Способности, внешность, здоровье, свободное время и другие личные ресурсы (A); а также Любовь и секс в интимных отношениях (L) 221 . Более углубленные расспросы по этим темам могут оценить сильные стороны, которые можно использовать на протяжении всего процесса лечения (например, привлечение поддерживающего партнера в аспектах практики когнитивно-поведенческих навыков), а также слабые области, которые необходимо укрепить.
Существует ряд стандартизированных шкал для определения факторов защиты. Положительное влияние признака может быть измерено с помощью Шкалы положительного и отрицательного воздействия (PANAS) 222 , широко используемого инструмента, состоящего из 20 пунктов. Самооценку можно оценить с помощью шкалы самооценки Розенберга 223 , десятибалльной шкалы общей самооценки или самопринятия. Альтернативой им может быть Информационная система измерения результатов (PROMIS) 224 , состоящая из пунктов шкалы для определения чувства смысла и цели (ощущение того, что в жизни есть цель и есть веские причины для жизни, включая надежду, оптимизм, целеустремленность и чувства, что жизнь достойна), положительного влияния (чувства, которые отражают уровень приятного взаимодействия с окружающей средой, такие как счастье, радость, волнение, энтузиазм и удовлетворенность) и самоэффективности (уверенность в способности эффективно справляться с различными стрессовыми ситуациями).
Был разработан ряд шкал самоотчета воспринимаемой устойчивости 225 , которые рекомендованы для использования в клиническом лечении депрессии. К ним относится шкала устойчивости Коннора-Дэвидсона 226 , 25-балльная шкала личной компетентности, упорства, доверия к своим инстинктам, терпимости к негативным влияниям, принятия изменений, безопасных отношений и духовных влияний, которая чувствительна к изменениям в лечении. Укороченная версия этой шкалы из 10 пунктов может быть более практичной 227 . Краткая шкала устойчивости включает всего 6 пунктов и измеряет способность оправляться от жизненных стрессоров 228 .
Большое количество шкал измеряет социальную поддержку. Например, Многомерная Шкала Воспринимаемой Социальной Поддержки 229 , которая состоит из 12 пунктов и определяет воспринимаемую поддержку со стороны семьи, друзей и значимых других. Другим вариантом является Медицинское Обследование Социальной Поддержки 230 , которое измеряет эмоциональную/информационную поддержку, материальную поддержку и социальное взаимодействие. Кроме того, шкалы PROMIS 224 включают показатели дружеского общения, эмоциональной поддержки, ин формационной поддержки и инструментальной поддержки.
Навыки преодоления можно измерить с помощью Контрольного списка 231 "Способы преодоления". Несмотря на объем (66 пунктов), эта шкала измеряет мысли и действия, которые люди используют для удовлетворения внутренних или внешних потребностей в конкретных стрессовых ситуациях. Более короткой альтернативой является Краткая ориентация на преодоление проблем, с которыми сталкивался опись 232 (28 пунктов), в которой оценивается проблемно-ориентированное преодоление (например, активное преодоление, планирование, подавление конкурирующих действий, сдерживание и поиск инструментальной социальной поддержки) и эмоционально-ориентированное преодоление (например, поиск эмоциональной социальной поддержки, позитивное переосмысление, принятие, отрицание и обращение к религии). Эти шкалы дают представление о типе навыков преодоления, некоторые из которых являются адаптивными и могут быть усилены, в то время как другие являются неадаптивными (например, принятие желаемого за действительное, отрицание) и могут быть объектом вмешательства.
Наличие защитных факторов или их отсутствие может менять клиническое ведение несколькими способами. Во-первых, те защитные факторы, которые уже присутствуют, могут быть усилены, поощрены и использованы в лечении. Например, поддерживающие близкие люди могут быть включены в процесс лечения, например, когда родные совместно осваивают когнитивно-поведенческие навыки и облегчают практику воздействия in vivo для пациентов с агорафобией 233 . Поддерживающие члены семьи могут быть аналогично полезными партнерами для пациентов с ОКР или ПТСР, поскольку они участвуют в предотвращении воздействия стрессорных факторов, заботясь о том, чтобы исправить чрезмерную тревогу со стороны члена семьи (например, выполнение просьб пациента о чрезмерном мытье из-за опасений загрязнения), поскольку выполнение таких действий непреднамеренно усиливает избегающее поведение 234 . Позитивный аффект может способствовать экспозиционной терапии фобий 235 .
При отсутствии защитных факторов, влияния на эти области могут быть перспективны. По сути, КПТ обеспечивает большую защиту за счет обучения навыкам борьбы со внутренними (т.е. симптомами тревоги) и внешними стрессорами. Создание надежных сетей социальной поддержки может стать целью вмешательства, особенно когда тревога приводит к избегающему поведению и ослабляет социальные связи и поддержку. Новые методы психологических влияний, направленных на повышение чувствительности к вознаграждению, могут быть эффективны у пациентов со сниженным настроением 236,237 , при этом первоначальные результаты показывают эффективность как у тревожных, так и у депрессивных пациентов. Практики, основанные на осознанности, также улучшают положительное влияние 238 .
КОГНИТИВНАЯ ДИСФУНКЦИЯ
Тревожные люди проявляют повышенную чувствительность при распознавании, обработке и реагировании на информацию, связанную с угрозой, даже в отсутствие реальной угрозы.
Переоценка угрозы возникает в процессах внимания. Смещение внимания означает, что тревожные люди склонны легко отвлекаться на потенциальные угрозы за счет внимания к другим, возможно, более важным особенностям окружающей среды 239 . В клинически тревожных группах смещение внимания часто зависит от их фокуса внимания (например, социально тревожные люди проявляют смещение внимания для выявления социальных опасностей, в то время как люди с ГТР проявляют более широкое смещение внимания к физическим и социальным угрозам). Смещения внимания включают в себя ряд компонентов, начиная от сенсорно-перцептивных процессов (ранняя обработка и обнаружение стимулов), до внимания (способность обращать внимание на одни стимулы и игнорировать другие), памяти (поддержание и извлечение информации) и исполнительной функции (сложные интегративные процессы и процессы принятия решений).
Кроме того, тревожные люди, как правило, демонстрируют замедленное отвлечение от стимулов, связанных с угрозой. Особый тип смещения в процессе внимания возникает в отношении интероцептивных сигналов. Интероцептивная осведомленность (или осведомленность о внутренних состояниях организма) изучалась в основном у пациентов с паническим расстройством, но интероцептивная чувствительность может повышаться и при других тревожных расстройствах 240,241 . Примечательно, что повышенная интероцетивная чувствительность не приводит к более точной оценке состояния, что может приводить к ошибкам в сообщении о симптомах и неправильной оценке угрозы.
У людей с тревожными расстройствами могут возникать различные смещения внимания, некоторые проявляют большую предвзятость на этапе первоначального обнаружения, у других смещения внимания проявляются на этапе переключения внимания, а у третьих смещения внимания проявляются игнорированием важных стимулов 242,243 . Такие смещения внимания, вероятно, лежат в основе распространенных жалоб на отвлекаемость и плохую концентрацию у людей с ГТР и у лиц, страдающих фобией, когда они сталкиваются со своими опасными ситуациями.
Наряду с концентрированием внимания на угрозе, тревожные индивидуумы также интерпретируют неоднозначные стимулы как угрожающие 244,245 . Смещения внимания, вероятно, влияют на интерпретацию угрозы, которая, в свою очередь, предположительно влияет на внимание к угрозе. Неправильная интерпретация часто наблюдается в ответ на неоднозначные стимулы, например, значения двусмысленных предложений.
Как и в случае с “тревожным” вниманием, “тревожная” интерпретация, как правило, специфично проявляется при разных тревожных расстройствах. Таким образом, люди с паническим расстройством более склонны интерпретировать как угрозу неоднозначные стимулы, связанные с физическими ощущениями, в то время как люди с социальным тревожным расстройством склонны интерпретировать неоднозначные социальные события как более негативные, а умеренно негативные социальные события как более катастрофические в сравнении с другими тревожными пациентами или контрольной группой. Люди с ГТР склонны интерпретировать любые неоднозначные события в целом как угрожающие 20 .
Повышенная чувствительность к тревоге характерна для большинства тревожных расстройств, хотя особенно выражена у пациентов с паническим расстройством 246 . Было показано, что повышенная чувствительность к тревоге является как предиктором развития симптоматики тревоги, так и фактором, способствующим сохранению тревожной симптоматики. Она реагирует на когнитивные, поведенческие и фармакологические вмешательства 246 .
Многие исследовательские инструменты для оценки смещения внимания не подходят для клинической практики. Онлайн- или веб-программы для изменения смещения внимания (описанные ниже) обычно включают тесты на смещение внимания. Более практичными являются стандартизированные шкалы самоотчета, которые измеряют аспекты взаимодействия со стимулами, связанными с угрозой.
Одним из примеров является шкала контроля внимания из 20 пунктов 247 , оценивающая фокусировку и переключение внимания.
Опросник Интерпретации 248 оценивает взаимодействие индивидов с неоднозначными социальными сценариями. Этот опросник включает двадцать два неоднозначных сценария (например, “Вы видите, как группа друзей обедает, они замолкают, когда вы приближаетесь”) и 3 интерпретации каждого сценария (т.е. положительная: “Они собираются попросить вас присоединиться”; отрицательная: “Они говорили о вас негативные вещи”; и нейтральная: “Они только что закончили свой разговор”). Участников просят оценить, насколько вероятно, что каждая интерпретация пришла бы им в голову, если бы они оказались в аналогичной ситуации.
Для ОКР Опросник навязчивых убеждений 249 представляет собой опросник по когнитивным предубеждениям, состоящий из 44 пунктов, которые приводят к неправильной интерпретации обычно возникающих навязчивых мыслей как угрожающих. Многомерная оценка интероцептивной осведомленности-2 (МАЙЯ-2) 250 представляет собой опросник по состояниям с тридцатью семью пунктами для измерения нескольких аспектов интероцепции путем самоотчета. Индекс чувствительности к тревоге – 3 251 представляет собой шкалу из 18 пунктов с тремя подшкалами, представляющими физические проблемы (например, смерть, обморок), когнитивные проблемы (например, потеря контроля) и социальные проблемы (например, смущение), связанные с тревогой и связанными с ней симптомами.
КПТ при ОКР направлена на когнитивные предубеждения в отношении угрозы. Психообразование, начальная терапевтическая стратегия, обычно включает информацию, предназначенную для исправления ошибочных представлений, особенно о симптомах тревоги. Когнитивная реструктуризация обучает навыкам выявления завышенных оценок опасности и способам балансирования оценок с более обоснованными интерпретациями. Экспозиционная терапия нацелена на исправление ошибок прогнозирования (т.е. нарушение негативных ожиданий) посредством непосредственного опыта. Высокий уровень неправильной оценки угрозы может указывать на необходимость проведения КПТ, хотя нет достаточных доказательств соответствия подхода к лечению (медикаментозное лечение против КПТ по сравнению с другими психотерапиями) к таким когнитивным предубеждениям. Фактически только одно исследование показало, что более высокие баллы по чувствительности к тревоге предсказывали более слабую реакцию как на КПТ, так и на медикаментозную терапию 252 .
Программы модификации предубеждений появились как более целенаправленное лечение когнитивных предубеждений. Методика тренировки внимания 253 состоит из упражнений на слуховое внимание, которые требуют от людей овладения навыками исполнительного контроля, включая избирательное внимание, разделенное внимание и переключение внимания, чтобы уменьшить негибкое сосредоточенное на себе внимание, предвзятое внимание, ориентированное на угрозу, беспокойство и размышления. Эта методика продемонстрировала эффективность при тревожных расстройствах 254 . Тренировка смещения внимания (т.е. тренировка смещения внимания от стимулов, связанных с угрозой, к нейтральным или позитивным стимулам путем усиления выбора точечного воздействия) и тренировка смещения интерпретации (т.е. Обучение нейтральной или позитивной интерпретации неоднозначных сценариев путем усиления выбора слов) также имеют доказательную базу. Однако, хотя такое обучение оказывает сильное влияние на смещение внимания или интерпретации как таковое, исследования, как правило, показывают небольшие размеры влияния на симптомы тревоги 255,256 .
Понимание когнитивных предубеждений также имеет отношение к подходам фармакотерапии, особенно когда пациенты считают, что их телесные ощущения указывают на травму или опасность, что может привести к чрезмерному страху перед лекарствами и их побочными эффектами.
В этих сценариях могут быть рекомендованы дифференцированные подходы к лечению.
Когнитивные предубеждения, связанные с угрозой, могут незаметно влиять на способы получения и кодирования информации, так что то, что является благоприятными комментариями врача, может быть легко неверно истолковано как угроза пациенту. Осторожность в представлении информации с учетом предубеждений пациента может быть полезной.
Есть некоторые доказательства того, что изменение когнитивных предубеждений улучшает терапевтические результаты, особенно при расстройствах социальной тревожности 257-259 и паническом расстройстве 64 . Следовательно, отсутствие изменений в когнитивных процессах может быть показателем плохой реакции на лечение и необходимости переоценки подхода к лечению. Данные о влиянии фармакотерапии тревожных расстройств на когнитивную сферу по-прежнему находятся в стадии ранних исследований.
ОБСУЖДЕНИЕ
Цель этой статьи – описать систематически важные области, которые имеют отношение к персонализации лечения тревожных расстройств. Тщательная оценка симптомов тревоги для обеспечения надлежащего клинического диагноза имеет ключевое значение, учитывая, что большинство доказательств в этой области основано на исследованиях конкретных расстройств. Тем не менее растет число работ, подтверждающих мнение о том, что оценка других областей также полезна при принятии клинических решений.
Данные приведенных в этой статье исследований свидетельствуют о том, что мы начинаем переходить от простых рекомендаций лечить тревогу и связанные с ней расстройства с помощью СИОЗС, КПТ или их комбинации к более сложному подходу, который подчеркивает, что у врача есть все более широкий спектр доступных методов лечения и что лечение тревоги и связанных с ней расстройств может быть персонализировано в ряде важных аспектов.
Этот обзор того, что известно в настоящее время, а также ключевых областей для будущих исследований, представляется своевременным и ценным по ряду причин. Во-первых, он согласуется с растущим возрождением интереса к созданию персонализированной психиатрии и с аналогичными обзорами в других важных областях психиатрии 6,260 . Во-вторых, он согласуется с систематической работой по определению результатов лечения и может помочь определить переменные для потенциального включения в сложные прогностические модели, включая машинные подходы к обучению 261,262 . В-третьих, в литературе предлагается ряд клинически осуществимых мер, включая шкалы самоотчета, которые потенциально могут быть включены в будущие наблюдательные или интервенционные исследования.
В-четвертых, в обзоре определен ряд шкал, которые могут начать использоваться клиницистами на практике, поскольку они пытаются персонализировать лечение тревоги и связанных с ней расстройств, признавая, что для подтверждения их использования необходимы дополнительные исследования.
Ряд потенциальных критических замечаний в отношении нашего подхода здесь заслуживают обсуждения. Во-первых, можно утверждать, что клиницисты уже осведомлены о неоднородности тревоги и связанных с ней состояний. Хотя это, безусловно, верно, систематических усилий по предоставлению клиницисту практических способов оценки такой неоднородности не предпринимается. Во-вторых, можно утверждать, что использование формальных оценок не является практичным или эффективным в стандартной клинической практике. Однако, даже если клиницисты не всегда формально полагаются на диагностические критерии, внедрение надежной нозологической системы благотворно повлияет на подход клиницистов к оценке, и существует растущая доказательная база, свидетельствующая о ценности регулярного мониторинга исходов тревожных расстройств 106,107 . В-третьих, можно утверждать, что в конечном счете для оптимальной персонализации управления тревогой и связанными с ней расстройствами необходим трансляционный нейробиологический подход. Наша цель, безусловно, состоит не в том, чтобы преуменьшить важность такой работы, а скорее в том, чтобы утверждать, что уточнение клинической оценки может внести полезный вклад как в нейробиологическую, так и в интервенционную работу в будущем.
Ключевым вопросом, который возникает в результате этого и аналогичных обзоров, является обилие и сложность имеющихся соответствующих мер. Это изобилие создает ряд важных проблем для диагностики 263 . Во-первых, даже если клиницисты согласны с важностью оценки конкретной конструкции, использование различных инструментов может привести к разногласиям в выводах. Во-вторых, меры могут дать информацию, которую клиницистам трудно интерпретировать, и поэтому могут укрепить мнение о том, что клиническое суждение более полезно, чем клинические меры. В-третьих, использование ряда показателей может затруднить общение между врачами и пациентами, что затруднит совместное принятие решений. Приведенный здесь обзор согласуется с призывами разработать общие показатели 264 , согласовать основные наборы результатов 265,266 и согласовать результаты измерений 263 .
Возможно, будет полезно сравнить существующие работы по индивидуальным подходам к депрессии и тревожности 6 . На первый взгляд, похоже, что область депрессии гораздо более развита, с большим количеством имеющихся данных по целому ряду важных областей и о том, как их можно использовать для персонализации лечения. Напротив, тяжелая депрессия является чрезвычайно гетерогенным состоянием, в то время как некоторые тревожные и связанные с ними расстройства кажутся более однородными. Хотя ни одному конкретному тревожному или связанному с ним состоянию не уделялось столько внимания, как депрессии, распознавание специфической тревожности и связанных с ней состояний создало возможность для более детальной работы над каждым из этих расстройств, а подтипирование конкретных состояний способствовало персонализированному подходу к терапии пациента.
Очевидно, что необходимо проделать большую дальнейшую работу для разработки подробного и основанного на фактических данных подхода к персонализации терапии тревожных расстройств.
Иерархические модели симптомов, такие как модель иерархической таксономии психопатологии (HiTOP) 155 или трехуровневая модель депрессии и тревожности 267,268 , обеспечивают полезную основу для понимания генетических, нейробиологических и экологических факторов риска и моделей ковариации симптомов. В будущем было бы полезно, чтобы клинические испытания включали не только диагностику тревоги и определение тяжести симптомов, а также более подробную оценку симптоматики (например, оценку специфического поведения, физиологических параметров и когнитивных оценок), а также ряда других областей, рассмотренных здесь. Мы надеемся, что такая работа поспособствует персонализации лечения тревоги и связанных с ней состояний.
Перевод: Викторов А.А. (г. Санкт-Петербург)
Редактура: к.м.н. Рукавишников Г.В. (г. Санкт-Петербург)
Stein DJ, Craske MG, Rothbaum BO et al. The clinical characterization of the adult patient with an anxiety or related disorder aimed at personal-ization of management. World Psychiatry. 2021;20(3):336-356.
DOI:10.1002/wps.20919
1 октября 2021
Количество просмотров: 2135
