Психиатрия Всемирная психиатрия
Психиатрия Всемирная психиатрия
№03 2019
Эффективность и безопасность пищевых добавок в лечении психических расстройств: мета-обзор мета-анализов рандомизированных контролируемых исследований №03 2019
Номера страниц в выпуске:317-332
Роль питания в психическом здоровье становится все более признанной. Наряду с обычным приемом пищи, рацион питания также может включать «пищевые добавки», среди которых полиненасыщенные жирные кислоты (ПНЖК), витамины, минералы, антиоксиданты, аминокислоты и пре/пробиотики. В последнее время появилось большое количество мета-анализов изучения пищевых добавок при лечении психических расстройств. Чтобы подготовить мета-обзор этих важнейших данных, мы собрали и оценили все мета-анализы рандомизированных контролируемых исследований (РКТ), в которых сообщается об эффективности и безопасности пищевых добавок при частых и тяжелых психических расстройствах. Наш системный поиск выявил 33 мета-анализа плацебо-контролируемых РКТ с первичным анализом, включающих данные о результатах о 10951 человек. Наиболее убедительные доказательства были найдены в отношении ПНЖК (особенно эйкозапентаеновой кислоты) при использовании в качестве дополнительного средства в лечении депрессии. Более новые данные свидетельствуют о том, что ПНЖК также могут быть полезны при синдроме дефицита внимания/гиперактивности, в то время как доказательств эффективности при лечении шизофрении не получено. Добавки на основе фолата широко исследовались как адъювантная терапия при лечении депрессии и шизофрении, с положительным эффектом при высоких дозах метилфолата в РКТ при лечении большого депрессивного расстройства. Появились новые данные в пользу того, что N-ацетилцистеин является полезным вспомогательным средством при расстройствах настроения и шизофрении. Все пищевые добавки имели хорошие профили безопасности, без признаков серьезных побочных эффектов или противопоказаний к применению вместе с психиатрическими препаратами. В заключении, врачи должны быть проинформированы о пищевых добавках с установленной эффективностью для лечения определенных состояний (таких как эйкозапентаеновая кислота при депрессии), но также должны быть осведомлены о тех пищевых добавках, которые пока не имеют должной доказательной базы. Будущие исследования должны быть направлены на изучение основных механизмов действия, а также на то, какие лица могут извлечь наибольшую пользу из этих пищевых добавок.
Ключевые слова: пищевые добавки, полиненасыщенные жирные кислоты, омега-3, эйкозапентаеновая кислота, метилфолат, витамин D, N-ацетилцистеин, депрессия, шизофрения, синдром дефицита внимания/гиперактивности, адъювантное лечение.
Ключевые слова: пищевые добавки, полиненасыщенные жирные кислоты, омега-3, эйкозапентаеновая кислота, метилфолат, витамин D, N-ацетилцистеин, депрессия, шизофрения, синдром дефицита внимания/гиперактивности, адъювантное лечение.
Перевод: Симонов Р.В. (Санкт-Петербург)
Редактура: к.м.н. Чумаков Е.М. (Санкт-Петербург)
Firth J, Teasdale SB, Allott K. The efficacy and safety of nutrient supplements in the treatment of mental disorders: a meta-review of meta-analyses of randomized controlled trials. World Psychiatry. 2019;18(3):308–24.
Роль питания в психическом здоровье становится все более признанной. Наряду с обычным приемом пищи, рацион питания также может включать «пищевые добавки», среди которых полиненасыщенные жирные кислоты (ПНЖК), витамины, минералы, антиоксиданты, аминокислоты и пре/пробиотики. В последнее время появилось большое количество мета-анализов изучения пищевых добавок при лечении психических расстройств. Чтобы подготовить мета-обзор этих важнейших данных, мы собрали и оценили все мета-анализы рандомизированных контролируемых исследований (РКТ), в которых сообщается об эффективности и безопасности пищевых добавок при частых и тяжелых психических расстройствах. Наш системный поиск выявил 33 мета-анализа плацебо-контролируемых РКТ с первичным анализом, включающих данные о результатах о 10951 человек. Наиболее убедительные доказательства были найдены в отношении ПНЖК (особенно эйкозапентаеновой кислоты) при использовании в качестве дополнительного средства в лечении депрессии. Более новые данные свидетельствуют о том, что ПНЖК также могут быть полезны при синдроме дефицита внимания/гиперактивности, в то время как доказательств эффективности при лечении шизофрении не получено. Добавки на основе фолата широко исследовались как адъювантная терапия при лечении депрессии и шизофрении, с положительным эффектом при высоких дозах метилфолата в РКТ при лечении большого депрессивного расстройства. Появились новые данные в пользу того, что N-ацетилцистеин является полезным вспомогательным средством при расстройствах настроения и шизофрении. Все пищевые добавки имели хорошие профили безопасности, без признаков серьезных побочных эффектов или противопоказаний к применению вместе с психиатрическими препаратами. В заключении, врачи должны быть проинформированы о пищевых добавках с установленной эффективностью для лечения определенных состояний (таких как эйкозапентаеновая кислота при депрессии), но также должны быть осведомлены о тех пищевых добавках, которые пока не имеют должной доказательной базы. Будущие исследования должны быть направлены на изучение основных механизмов действия, а также на то, какие лица могут извлечь наибольшую пользу из этих пищевых добавок.
Ключевые слова: пищевые добавки, полиненасыщенные жирные кислоты, омега-3, эйкозапентаеновая кислота, метилфолат, витамин D, N-ацетилцистеин, депрессия, шизофрения, синдром дефицита внимания/гиперактивности, адъювантное лечение.
В настоящее время имеются многочисленные данные, свидетельствующие о том, что люди с психическими расстройствами обычно потребляют избыточное количество продуктов с высоким содержанием жира и сахара, при недостаточном потреблении продуктов с высоким содержанием питательных веществ по сравнению с населением в целом1-5. Связь между неправильным питанием и психическими заболеваниями, по-видимому, сохраняется даже при учете других факторов, которые могли бы объяснить эту связь, таких как социальная депривация или ожирение, и не объясняется обратной причинно-следственной связью1,6.
Кроме того, хотя метаболические и гормональные побочные эффекты психотропных препаратов могут влиять на прием пищи7,8, неправильное питание, по-видимому, присутствует даже до постановки психиатрических диагнозов. Например, при депрессии, плохое питание предшествует и действует как фактор риска для развития расстройства6,9,10. Аналогично при психотических расстройствах, различные дефициты питания проявляются еще до начала антипсихотического лечения11.
В настоящее время ясна роль диеты для поддержания физического здоровья, так как изучено влияние питания на развитие кардиометаболических заболеваний, рака и преждевременной смертности12,13. Параллельно все больше признается потенциальное влияние диеты на психические расстройства14,15. Однако, питательные вещества могут потребляться в пищу не только при обычных приемах пищи, но и в виде пищевых добавок16. Добавки, как правило, используют для: а) коррекции недостаточного питания (или при низком уровне питательных веществ в плазме); б) приема специфических питательных веществ в больших чем обычно дозах, для достижения определенных физиологических целей; в) обеспечения питательных веществ в более биодосутпной форме, что важно для людей с генетическими особенностями или при проблемах со здоровьем, при которых усвоение питательных веществ может быть нарушено. Эти добавки могут быть получены как синтетическим путем, так и естественным, непосредственно из пищи. Как правило, речь идет о витаминах (например, фолиевая кислота, витамин D), минералах (например, цинк, магний), пре- и пробиотиках (из конкретных штаммов кишечных бактерий), полиненасыщенных жирных кислотах (ПНЖК) (обычно омега-3 рыбные масла) или аминокислотах (например, N-ацетилцистеин, глицин).
Питательные добавки широко используются в популяции. Например, в США более половины взрослого населения принимают те или иные пищевые добавки17. Но доказательств того, что такое широкое применение снижает заболеваемость или преждевременную смертность, нет (даже наиболее качественные исследования, например витамина D18 и E19,20, были отрицательными). Тем не менее, некоторые конкретные питательные добавки связаны с пользой для здоровья у конкретных групп населения или клинических состояний (например беременным женщинам рекомендуется добавить в рацион фолиевую кислоту, для снижения риска развития дефицита нервной трубки у плода21; при тяжелой анемии рекомендуется назначается витамин B1222; пероральный прием препаратов цинка – терапия первой линии при болезни Вильсона23; и национальная медицинская ассоциация рекомендует омега-3 жирные кислоты пациентам с перенесенным инфарктом миокарда24).
В настоящее время наблюдается повышенный академический и клинический интерес к роли питательных добавок для лечения различных психических расстройств14-16. Этот рост исследований частично объясняется нашим развивающимся пониманием нейробиологических основ психических заболеваний, которые подразумевают использование определенных питательных веществ в качестве вспомогательного лечения по целому ряду причин25.
Во-первых, недавние клинические исследования показали, что многие психические расстройства сопряжены с повышением уровня маркеров окислительного стресса и воспаления26-29, а также была отмечена связь между эффективностью фармакологических препаратов и коррекцией образа жизни при психических расстройствах с изменением этих биомаркеров30,31. Таким образом, антиоксидантные и противовоспалительные свойства некоторых пищевых добавок (таких как N-ацетилцистеин32 и омега-3 жирные кислоты33) указывают на то, что они могут быть полезны при лечении психических расстройств, вызванных воспалением и окислительным стрессом.
Во-вторых, в настоящее время имеются данные крупных исследований, показывающие, что психотические расстройства и расстройства настроения связаны со снижением сывороточного уровня основных питательных веществ, таких как цинк34,35, фолат36,37 и витамин D38,39. Поскольку эти дефициты, вероятно, связаны со степенью ответа на лечение и клиническим исходом в этих популяциях11,34,40, существует возможность того, что добавление питательных веществ может улучшить результаты лечения.
В-третьих, появляются некоторые данные о том, что психические расстройства могут быть связаны с дисфункцией кишечного микробиома41,42. Поскольку кишечные бактерии могут быть модифицированы с помощью микронутриентов и пре/пробиотиков43,44, это позволяет предположить, что некоторые пре/пробиотические добавки могут быть потенциально полезными новыми терапевтическими вариантами, заслуживающими дальнейшего исследования45,46.
Наряду с теоретическим потенциалом пищевых добавок, нацеленных на определенные аспекты психических расстройств, существует также огромное количество клинических испытаний и мета-анализов, изучающих их использование в психиатрическом лечении в качестве профилактики47,48. Тем не менее, их роль все еще остается неясной. Это, вероятно, связано с отсутствием четкого и современного руководства для врачей и исследователей в отношении их: а) относительной эффективности для улучшения клинических исходов у людей с психическими заболеваниями; и б) безопасности для использования, особенно в сочетании с препаратами психиатрического профиля.
Цель настоящего мета-обзора состоит в том, чтобы обобщить и оценить данные высшего уровня об эффективности и безопасности пищевых добавок при лечении психических расстройств, а также изучить условия, при которых они могут быть эффективными. Для этого мы идентифицировали, синтезировали и оценили все доступные данные из мета-анализов рандомизированных контролируемых исследований (РКТ), изучающих качество доказательств для всех пищевых добавок при различных психических расстройствах. Наряду с предоставлением четкого обзора эффективности конкретных питательных добавок при различных расстройствах, мы также стремились изучить, какие дозы и симптоматические цели являются наиболее подходящими, в то же время дополнительно сообщая о безопасности и переносимости.
Систематический поиск
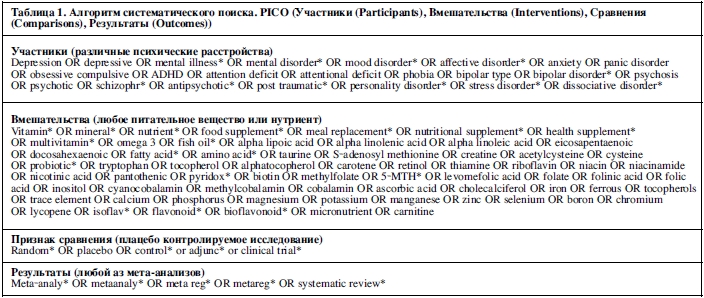
Алгоритм поиска заголовков и ключевых слов представлен в Таблице 1. Систематический поиск проводился с использованием Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, Health Technology Assessment Database, Allied и Complementary Medicine (AMED), PsycINFO и Ovid MEDLINE(R) по состоянию на 1 февраля 2019 года.
Поиск Google Scholar был проведен с использованием тех же ключевых слов, чтобы выявить любые дополнительные соответствующие статьи. Также был проведен поиск по спискам литературы включенных в обзор статей.
Критерии отбора
Критерии отбора были организованы в соответствии со структурой отчетности PICO (Участники (Participants), Вмешательства (Interventions), Сравнения (Comparisons), Результаты (Outcomes)), как описано ниже.
Все исследования вышеуказанных состояний были отобраны при условии, что по меньшей мере 75% выборки имели подтвержденное психическое заболевание или состояние риска, подтвержденное либо клиническим анамнезом, либо достижением установленных пороговых значений при достоверных скрининговых исследованиях. Исследования, изучающие влияние пищевых добавок на психическое здоровье в общей популяции, включались только в том случае, если имелись данные из подгруппы людей с психическими заболеваниями (при этом 75% выборки соответствовали вышеуказанным критериям). Исследования, изучающие пищевые добавки только для улучшения дефицита питания, связанного с расстройствами пищевого поведения или злоупотребления психоактивными веществами, были исключены. Исследования, изучающие нарушения развития центральной нервной системы (например, аутизм, умственная отсталость) или нейродегенеративные расстройства (например, деменция), также не включались.
Вмешательства
Все питательные добавки, рассмотренные для этого мета-обзора, использовались или как дополнительная терапия, или в качестве монотерапии. Питательные добавки были определены как витамины, минералы, макроэлементы, жирные кислоты или аминокислоты (включая пероральные формы), обычно встречающиеся в рационе человека. Метаанализ модификации диеты и травяных добавок включен не был.
Сравнения
Поскольку это исследование было направлено на предоставление доказательств высшего уровня, были включены только мета-анализы РКТ.
Там, где перекрещивались данные о пищевой добавке для конкретного результата/расстройства, использовался самый последний обновленный мета-анализ, если он охватывал более 75% испытаний в более ранней версии. В тех случаях, когда более ранние мета-анализы представляли уникальные результаты, путем включения большего числа исследований или использования отдельных анализов подгрупп, эти данные использовались в качестве дополнительных анализов для нашего мета-обзора.
AMSTAR-2 оценивает 16 пунктов, которые отражают качество систематического обзора/мета-анализа. Семь из них были определены как “критические», которые использовались для определения общей уверенности в результатах обзора50. Для целей нашего мета-обзора включенные мета-анализы были оценены по всем 16 пунктам AMSTAR-2, и также получили отдельную оценку за количество “критических” пунктов.
В соответствии с общепринятыми трактовками, SMD были классифицированы как незначительные (<0,2), малые (0,2-0,4), умеренные (0,4-0,8) или большие (>0,8). В тех случаях, когда мета-анализы давали размеры эффекта, скорректированные на системную ошибку, это сообщались вместе с основными наблюдаемыми эффектами и интерпретировались как первичные результаты анализа. В тех случаях, когда непрерывные результаты были представлены в виде взвешенных средних различий или необработанных средних различий, они были пересчитаны в SMD (Hedges’ g) с использованием комплексного мета-анализа 3.0. В тех случаях, когда оригинальные мета-анализы сообщали о положительном влиянии питательных веществ в виде отрицательных величин эффекта (чтобы представить уменьшение симптомов), они были перекодированы в положительные, так что все представленные здесь величины эффекта являются положительными значениями, которые непосредственно указывают на пользу от использования питательных веществ по сравнению с плацебо, или отрицательными значениями, когда плацебо было связано с лучшими результатами, чем влияние питательных веществ. В тех случаях, когда мета-анализ применял модели фиксированных эффектов для расчета размеров эффекта пищевых добавок по сравнению с плацебо, они также пересчитывались с использованием модели случайных эффектов, так что SMD между добавками/расстройствами подлежали сравнению.
Результаты вторичных анализов, фокусирующихся на безопасности и переносимости, как правило, сообщались как категориальные исходы (относительные частоты нежелательных эффектов или прекращения лечения в сравнениях применения препаратов с плацебо). Они были извлечены в виде коэффициентов шансов (OR) или коэффициентов риска (RR) в соответствии с первоначальными результатами.
Как для первичного, так и для вторичного анализа мы также извлекли число участников (N), а также количество исследований/сравнений (n), из которых был получен размер объединенного эффекта. Кроме того, гетерогенность была количественно определена с использованием статистики I2 и классифицирована как низкая (I2<25%), умеренная (I2=25-50%) или высокая (I2>50%).
Там, где сообщалось, были также извлечены все дополнительные характеристики исследования, особенно в отношении используемой пищевой добавки (включая тип, дозу и остальные факторы), образец и диагностические детали, а также любые соответствующие выполненные анализы подгрупп (например, разделение испытаний высокого/низкого качества, конкретных подвыборок пациентов или уровней дозировки).
Потенциальное влияние системной ошибки публикации оценивалось везде, где имелись достаточные данные для соответствующего анализа, и скорректированные размеры эффекта (при контроле за небольшим системной ошибкой исследования) представлены вместе с основными выводами.
 Результаты систематического поиска
Результаты систематического поиска
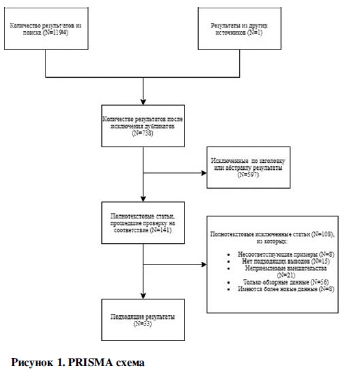
Поиск обнаружил 1194 результатов, которые были уменьшены до 737 после удаления дубликатов. Еще одна потенциально приемлемая статья была получена из дополнительного поиска Google Scholar. Оценка заголовков и абстрактов отсеяла еще 597 статей, в то время как 141 статья была извлечена и рассмотрена в полном объеме. Из них 108 не подходили для участия. Таким образом, в общей сложности для этого мета-обзора были включены приемлемые данные из 33 независимых мета-анализов РКТ пищевых добавок при психических расстройствах (см. Рисунок 1).
Мета-анализы изучали РКТ полиненасыщенных жирных кислот, витаминов, минералов, аминокислотных добавок и пре/пробиотиков, с первичным анализом, включавшим результаты в общей сложности от 10951 человека. Все мета-анализы основывались на питательных добавках, вводимых в сочетании с “обычным лечением” (без указания схем лечения) или в качестве дополнительного лечения к определенному классу психотропных препаратов (например, селективные ингибиторы обратного захвата серотонина (СИОЗС) при депрессии или антипсихотики при шизофрении). Только один из мета-анализов сообщил о питательной добавке в качестве монотерапии для психического расстройства (т.е. омега-3 жирные кислоты для депрессии), в то время как другие специально не исключали пациентов, принимающих лекарства. Никакие мета-анализы напрямую не сравнивали пищевые добавки с психотропными препаратами. Все исследования51-82 были плацебо-контролируемыми.
Конкретные психические состояния (и отмеченные результаты лечения), рассматриваемые в этом мета-обзоре, включают: шизофрению (изучение общих симптомов наряду с позитивными, негативными, общими и депрессивными симптомами и позднюю дискинезию)52-59; состояния риска развития психоза (изучение ослабленных симптомов психоза, негативных симптомов, перехода к психозу и функционирования)60-63; депрессивные расстройства (включая любую клиническую депрессию, диагностированное большое депрессивное расстройство (БДР), депрессию во время беременности, в пожилом возрасте или как сопутствующую патологию к хроническим состояниям здоровья)51,59,64-73; состояния, связанные с тревогой и стрессом (включая генерализованное тревожное расстройство, обсессивно-компульсивное расстройство (ОКР) и трихотилломанию)68,72,74; биполярное аффективное расстройство I и II типов (изучение общих симптомов, биполярной мании, биполярной депрессии, функциональных нарушений и качества жизни)56,68,72,75,76; и СДВГ (включая сложные симптомы, гиперактивность-импульсивность, невнимательность, поведенческие сопутствующие нарушения, такие как агрессия, и когнитивное функционирование)77-82.


Наиболее широко оцененной витаминной добавкой для лечения психических расстройств был витамин В9, который также называют “фолат». Его можно вводить как добавку в виде фолиевой кислоты, фолиниевой кислоты или метилфолата (который также известен как l-метилфолат, левомефоловая кислота или 5-метилтетрагидрофолат).
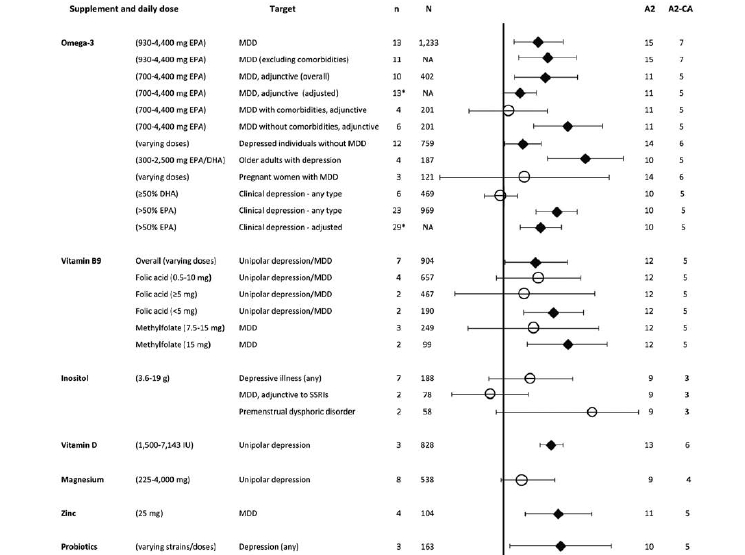
В качестве дополнения к СИОЗС у 904 лиц с униполярной депрессией (в основном БДР), добавки на основе фолатов (включая фолиевую кислоту и метилфолат, вводимые в различных дозах) были связаны со значительным снижением депрессивных симптомов по сравнению с плацебо, хотя между исследованиями была большая гетерогенность (n=7, SMD=0,37, 95% CI: 0,01-0,72, p=0,04, I2=79%)67.
При введении витамина В9 в виде фолиевой кислоты (0,5-10 мг/сут) достоверного влияния на депрессивные симптомы не наблюдалось (N=657, n=4, SMD=0,4, 95% CI: -0,08– 0,88, p=0,1, I2=83%). Значительные эффекты наблюдались в двух испытаниях с использованием низкой дозы (<5 мг/сут) фолиевой кислоты (N=190, SMD=0,57, 95% CI: 0,23-0,91, p<0,001, I2=25%), в то время как не наблюдалось существенных преимуществ от доз ≥5 мг/сут (N=467, n=2, SMD=0,24, 95% CI: -0,56-1,03, p=0,56, I2=76%)67.
Два РКТ, исследовавшие высокую дозу (15 мг/сут) метилфолата (наиболее биоактивного метаболита фолиевой кислоты) в качестве вспомогательного средства для лечения БДР, обнаружили от умеренного до большого влияния на депрессивные симптомы (N=99, n=2, SMD=0,73, 95% CI: 0,28-1,19, p=0,002, I2=3%)67. Не было никаких свидетельств неблагоприятных последствий или статистической неоднородности. Однако при включении более низких доз метилфолата (7,5 мг / сут) не наблюдалось значимых эффектов на депрессию (N=249, n=3, SMD=0,34, 95% CI: -0,4– 1,08, p=0,37, I2=81%).
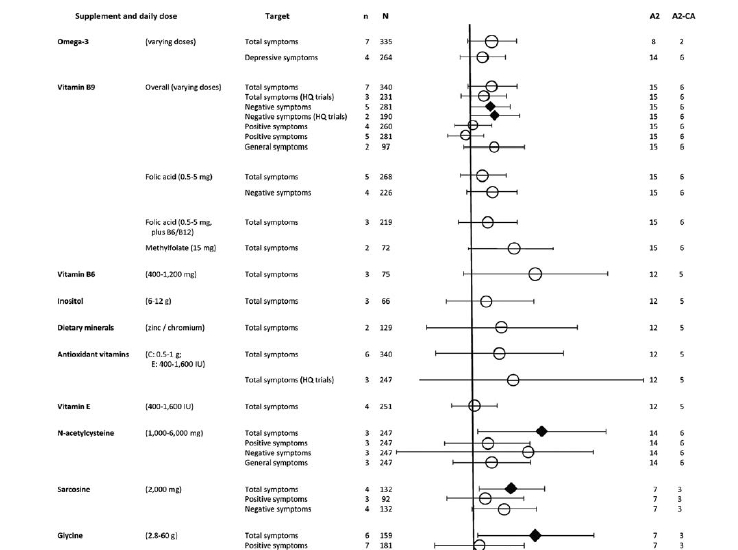
Семь РКТ (N=340) исследовали добавки на основе фолатов в качестве вспомогательного лечения шизофрении54. Витамин В9 вводили в виде метилфолата (n=2) или фолиевой кислоты (n=5), а также в комбинации с витаминами В6 и В12 (n=3). В общем анализе небольшие эффекты витамина В9 на общие симптомы не были статистически значимыми (SMD=0,20, 95% CI: -0,02-0,41, p=0,08, I2=0), а анализ подгрупп высококачественных исследований подтвердил отсутствие общих эффектов (N=231, n=3, SMD=0,15, 95% CI: -0,11-0,42, p=0,26, I2=0%). Добавки на основе фолиевой кислоты были неэффективны по суммарной оценке симптомов при введении в виде фолиевой кислоты (N=268, n=5, SMD=0,13, 95% CI: -0,12- 0,37, p=0,32, I2=0%), даже в сочетании с другими гомоцистеин-редуцирующими витаминами группы В (т.е. В6 и В12) (N=219, n=3, SMD=0,18, 95% CI: -0,13- 0,5, p=0,24, I2=16%). Однако влияние на суммарную оценку симптомов в двух исследованиях высоких доз метилфолата (15 мг/сут) приближалось к статистической значимости (N=72, n=2, SMD=0,45, 95% CI: 0,02-0,92, p=0,06, I2=0%).
Добавки на основе фолатов не оказывали существенного влияния на позитивные симптомы, общую психопатологию или депрессивные симптомы у пациентов с шизофренией54. Однако они уменьшали негативные симптомы в большей степени, чем плацебо (N=281, n=5, SMD=0,25, 95% CI: 0,01-0,49, p=0,04, I2=0). Эффект сохранялся в высококачественных РКТ (N=190, n=2, SMD=0,30, 95% CI: 0,00-0,60, p=0,05, I2=0), но стал несущественным при исключении РКТ с использованием 15 мг/сут метилфолата (N=226, n=4, SMD=0,23, 95% CI: -0,04-0,50, p=0,10, I2=0%)54.
Достоверно выявлена более низкая частота серьезных нежелательных явлений по сравнению с плацебо в течение использования фолатов у больных шизофренией (N=241, n=4, RR=0,32, 95% CI: 0,12-0,82, p=0,02, I2=0%)54.
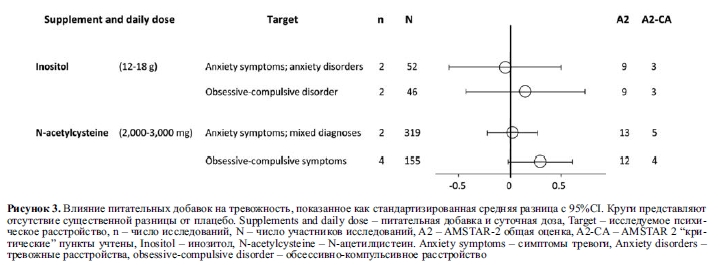
При шизофрении прием инозитола (6-12 г/сут) не превосходил плацебо по суммарной оценке симптомов (N=66, n=3, SMD=0,155, 95% CI: -0,35– 0,58, p=0,63, I2=87,2%)53. Среди лиц с биполярным аффективным расстройством инозитол (5,7-19 г/сут) не оказывал влияния на депрессивные симптомы (N=42, n=2, SMD=-0,11, 95% CI: -0,75– 0,52, p=0,72, I2=0%) или уровень ответа на лечение (RR=0,63, 95% CI: 0,35-1,12, p=0,12, I2=22%)68. При тревожных расстройствах инозитол (12-18 г/сут) не оказывал влияния на оценки шкалы тревоги Гамильтона (N=52, n=2, SMD=0,04, 95% CI: -0,58 – 0,51, p=0,89) и оценки симптомов в группах пациентов с ОКР (N=46, n=2, SMD=0,15, 95% CI:– 0,43-0,73, p=0,60)68.
Прекращение приема не приводило к различиям в группах пациентов с приемом инозитола и плацебо68. Однако прием инозитола был связан с тенденцией к более высокой частоте желудочно-кишечных расстройств, в сравнении с плацебо (N=183, n=6, SMD=3,26, 95% CI: 0,94-11,34, p=0,06, I2=0%).
Одиннадцать РКТ исследовали эффективность минеральных добавок для лечения депрессии, используя либо цинк, либо магний. Цинк вводился в дозе 25 мг/сут в качестве дополнительного лечения БДР и оказывал умеренное значимое влияние на депрессивные симптомы (N=104, n=4, SMD=0,66, 95% CI: 0,26-1,06, p<0,01)65. Хотя не было никаких доказательств гетерогенности (I2=0%), все включенные РКТ были идентифицированы как имеющие высокий риск отсева из-за отсутствия анализа намерения лечения у пациентов. У лиц с депрессией, выявленной с помощью самоотчетных измерений, добавление магния в дозе 225-4000 мг/сут не имело эффектов, выходящих за рамки плацебо (N=538, n=8, SMD=0,22, 95% CI: -0,17– 0,48, I2=30,9%)70. Нет доступных данных о магнии в качестве вспомогательного лечения при диагностированном БДР.
При объединенном анализе антиоксидантных витаминов (Витамин С и витамин Е: N=340, n=6, SMD=0,296, 95% CI: -0,39– 0,98, p=0,40, I2=40,6%); минеральных добавок (цинк и хром: N=129, n=2, SMD=0,324, 95% CI: -0,48– 1,13, p=0,43, I2=0%); или витамина В6 (N=75, n=3, SMD=0,682, 95% CI: -0,09– 1,45, Р=0,08, I2=58,4%) значительных терапевтических эффектов не выявлено53.
Как терапевтический вариант для управления побочными эффектами антипсихотиков, витамин Е не показал никаких отличий от плацебо по уровням улучшения при тардивной дискинезии52. Тем не менее, он достоверно снижал риск “обострения” тардивной дискинезии в течение 1 года (N=85, n=5, RR=0,23, 95% CI: 0,07-0,76), хотя этот результат был основан на низкокачественных исследованиях52.
Все витаминные и минеральные добавки, по-видимому, имеют хорошие профили безопасности при шизофрении, причем ни одна из них не вызывает большего числа побочных явлений чем плацебо52,53.
Полиненасыщенные жирные кислоты являются наиболее широко оцениваемой пищевой добавкой при различных психиатрических состояниях, вводимой в виде омега-3 жирных кислот, включая эйкозапентаеновую кислоту (ЭПК) и докозагексаеновую кислоту (ДГК), и омега-6 жирных кислот, таких как линолевая кислота (ЛК).
В 13 независимых РКТ c 1233 людьми с БДР, добавки с омега-3 (средняя дозировка: 1422 мг/сутки ЭПК) уменьшили депрессивные симптомы (SMD=0,398, 95% CI: 0,114-0,682, р=0,006, I2 неизвестен), без доказательств о систематической ошибке64. При использовании в дополнении к антидепрессантам при БДР, омега-3 жирные кислоты (930-4400 мг/сутки ЭПК) также произвели среднее влияние на депрессивные симптомы (N=448, n=11, SMD=0.608, 95% CI: 0.154-1.062, p=0.009, I2=82%), хотя была некоторая индикация систематической ошибки75 в публикации. Последующий анализ омега-3 в качестве вспомогательного средства к антидепрессантам при БДР дал аналогичные результаты (N=402, n=10, SMD=0.48, 95% CI: 0.11-0.84, p=0.01, I2=64%), хотя и вновь продемонстрировал доказательства значительной системной ошибки в публикации65. Поправка на системную ошибку в публикации позволила получить меньшие (но все же значимые) оценки эффектов омега-3 в качестве вспомогательного лечения БДР (SMD=0,19, 95% CI: 0,00-0,38, p=0,049).
Анализы подгрупп показали, что добавки омега-3 были эффективны только в качестве вспомогательного лечения БДР в когортах без сопутствующих заболеваний (N=201, n=6, SMD=0,74, 95% CI: 0,34-1,13, p<0,01, I2=42%), тогда как не было никаких признаков эффективности в группах, где БДР встречалось в сочетании с кардиометаболическими или неврологическими заболеваниями (N=201, n=4, SMD=0,05, 95% CI: -0,4-0,5, p=0,82, I2=45%)65. Кроме того, омега-3 были неэффективны для лечения БДР у беременных (N=121, n=3, SMD=0,24, 95% CI: -0,73– 1,21, p=0,63, I2=85%)59. Дальнейший анализ подгрупп лиц с депрессией (но без диагноза БДР) выявил небольшие положительные эффекты омега-3 при депрессивных симптомах (N=759, n=12, SMD=0,22, 95% CI: 0,01-0,43, p<0,05, I2=46%).
В исследованиях рассматривавших различные омега-3 кислоты для лиц с любой клинической депрессией, дополнения препаратов, содержащих ≥50% докозагексаеновой кислоты не имели никаких преимуществ перед плацебо (N=469, n=6, SMD=-0.028, 95% CI: -0.21-0.16, p>0.1)51. Однако добавки омега-3, содержащие >50% ЭПК, оказывали умеренно выраженное положительное влияние на депрессивные симптомы (N=969, n=23, SMD=0,61, 95% CI: 0,38-0,85, p<0,001). Снова, системная ошибка публикации была очевидна, и оцененные положительные влияния омега-3 препарата с высоким содержанием ЭПК были уменьшены, но все еще оказывались значительными даже после корректировки (SMD=0,42, 95% CI: 0.18-0.65, Р<0.001).
Дальнейший анализ различных форм ЭПК указал на несколько большее влияние на депрессивные симптомы в исследованиях с использованием препарата более 12-ти недель (N=274, n=4, SMD=1,07, р<0,01), по сравнению с периодом менее 12-недель (N=695, n=19, SMD=0,55, р<0,001), и с теми, кто использует омега-3 в качестве дополнительной терапии (N=535, n=15, SMD=0,72, р<0,001), а не в качестве монотерапии при депрессии (N=434, n=8, SMD=0,44, р=0,017)51.
Исследование у пациентов возрастом ≥65 лет с клинической депрессией (или с пограничными значениями на основании методов самооценки), показало, что омега-3 (средняя дозировка 1,3 г/сутки ЭПК/ДГК) имел значительно большее влияние на депрессивные симптомы в сравнении с плацебо (SMD=0,94, 95% CI: 0,5-1,37, p<0,001, I2=32,7%), хотя только в ограниченном количестве исследований с небольшим числом участников (N=187, n=4).
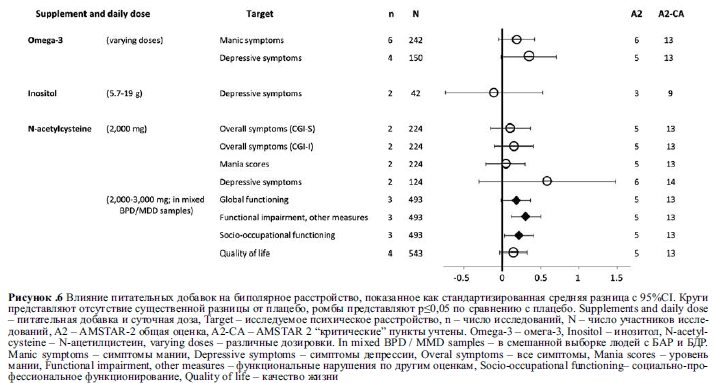
Во всех плацебо-контролируемых исследованиях омега-3 ПНЖК у людей с биполярным аффективным расстройством, эффекты на манию не были значимыми (N=242, n=6, SMD=0,198, 95% CI: -0,037– 0,433, p=0,10, I2=0%), хотя были небольшие положительные эффекты на депрессию (N=305, n=6, SMD=0,338, 95% CI: 0,035-0,641, p=0,029, I2=30%)75. Анализ, включающий только двойные слепые исследования, обнаружил аналогичные положительные эффекты для биполярной депрессии, хотя и не достигшие статистической значимости (N=150, n=4, SMD=0.36, 95% CI: -0.01– 0.73, p=0.051, I2=8%)76. Большинство исследований были определены как имеющие низкий риск системной ошибки, и не показали никаких признаков того, что омега-3 увеличил частоту нежелательных явлений или мании/гипомании при биполярном аффективном расстройстве.
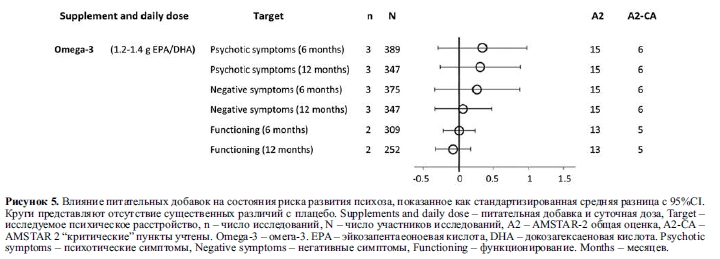
Три исследования (N=512), изучавшие влияние омега-3 (1200-1400 мг/сут) в качестве монотерапии для предотвращения развития психоза у молодых людей, отвечающих критериям “риска”, не показали никаких признаков положительного влияния (все р>0,1) по сравнению с плацебо в течение 26 недель (OR=0,64, 95% CI: 0,15-2,68) или 52 недель (OR=0,64, 95% CI: 0,18-2,26)60.
У молодых людей в группе риска психоза, добавки ПНЖК также были неэффективны в течение 52 недель для уменьшения ослабленных психотических симптомов (N=347, n=3, SMD=0,31, 95% CI: -0,26– 0,88, I2=80%)61, негативных симптомов (N=347, n=3, SMD=0,06, 95% CI: -0,35– 0,46, I2=63%)62 и функциональных нарушений (N=252, n=2, SMD=-0,08, 95% CI: -0,33– 0,17)63. Аналогичные нулевые эффекты также наблюдались в более коротких (т.е. 12 и 26 недель) временных интервалах61-63.
Изучение профилей безопасности показало, что ЭПК хорошо переносится при психотических расстройствах и не вызывает побочных эффектов, кроме легкого расстройства желудочно-кишечного тракта55. В группах риска, пробное снижение применяемых препаратов омега-3 не отличалось от плацебо60
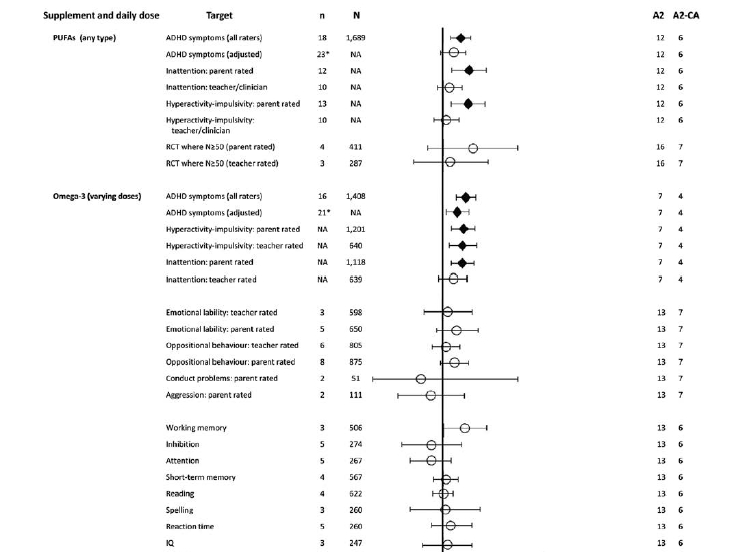
В 16 РКТ, сообщающих о доменах симптомов СДВГ, наблюдались значительные преимущества как для гиперактивности/импульсивности (SMD=0,209, 95% CI: 0,059-0,358, p=0,006), так и для дефицита внимания (SMD=0,162, 95% CI: 0,047-0,276, p=0,006)77. Анализ подгрупп показал, что значительные преимущества от ПНЖК наблюдались только на оцененных родителями показателях, без влияния на оценки общей симптоматики, гиперактивности/импульсивности или невнимательности от учителей/клиницистов77. Последующий анализ с использованием более строгих критериев учета РКТ (и исключая данные из исследований с менее чем 50 участниками), не выявил преимуществ добавления ПНЖК на оцененные учителями симптомы СДВГ (N=287, n=3, SMD=0,08, 95% CI: -0,32-0,47, p=0,56, I2=0%), а положительный эффект на родительскую оценку также не достиг статистической значимости (N=411, n=4, SMD=0,32, 95% CI: -0,15– 0,8, p=0,098, I2=52,4%).
Омега-3 добавки (120-2513 мг/сут; в среднем: 616 мг/сут) снижали общую оценку симптомов СДВГ значительно больше, чем плацебо (N=1,408, n=16, SMD=0,26, 95% CI: 0,15-0,37, p<0,001, I2=25%)79. Несмотря на статистически значимый характер, величина пользы была незначительной при применении анализа триммирования и заполнения для корректировки на погрешность публикации (SMD=0,16, 95% CI: 0,03-0,28). Аналогичные малые эффекты наблюдались для обеих областей симптомов гиперактивности-импульсивности (SMD=0,26, 95% CI: 0,13-0,39, p<0,001) и дефицита внимания (SMD=0,22, 95% CI: 0,1-0,34, p<0,001). Последующие анализы (хотя и включающие меньшее количество испытаний) повторили эти выводы о небольших, но значительных эффектах добавок омега-3 на суммарные баллы, гиперактивность-импульсивность и симптомы нарушений внимания80.
Что касается поведенческих сопутствующих заболеваний, то не было никаких признаков влияния омега-3 на эмоциональную лабильность, проблемы с поведением или агрессию у молодых людей с СДВГ. Только влияние на оппозиционное поведение по оценке родителей достигло значимости в первичном анализе (SMD=0,2, 95% CI: 0,03-0,38, p=0,02, I2=0,2%). Тенденция к положительному влиянию на оппозиционное поведение по оценке родителей наблюдалась также при применении строгих критериев учета (SMD=0,15, 95% CI: -0,006-0,31, p=0,06, I2=8%), а также при рассмотрении только высококачественных исследований (SMD=0,2, 95% CI: 0,03-0,38, p=0,02, I2=0,2%).
Что касается когнитивной дисфункции, то единственные положительные эффекты омега-3 у молодых людей с СДВГ наблюдались в индивидуальных оценках заданий по количеству пропусков (N=214, n=3, SMD=1,09, 95% CI: 0,43-1,75, p=0,001, I2=75%) и ошибкам в поручениях (N=85, n=2, SMD=2,14, 95% CI: 1,24-3,03, p<0,001, I2=63%)81. Положительная динамика была выявлена для суммарных баллов рабочей памяти (N=506, n=3, SMD=0,23, 95% CI: -0,001-0,46, p=0,05, I2=33,9%)82 и индивидуальных баллов заданий отсроченного воспроизведения (N=224, n=2, SMD=0,37, 95% CI: от -0,05 до 0,79, p=0,08, I2=55%).
Омега-3 не давал никаких преимуществ в задачах на оперативную память (N=224, n=2, SMD=0,06, 95% CI: -0.21– 0.34, p=0,66, I2=0%) и обработку информации (N=309, n=4, SMD=0,46, 95% CI: -0,29 – 1,21, p=0.23, I2=89%)81, и не приводил к каким-либо улучшениям в суммарных когнитивных оценках для общего IQ (N=247, n=3, SMD=0,05, 95% CI: -0,21 – 0,32, р=0,71, I2=0%), ингибировании (n=274, N=5, SMD=-0,12, 95% CI: -0,44– 0,2, р=0,47, i2=42,8%), внимании (N=267, n=5, SMD=-0,12, 95% CI: -0,33– 0,1, p=0,28, I2=0%), кратковременной памяти (N=567, n=4, SMD=0,03, 95% CI: -0,10– 0,16, p=0,64, I2=0%), чтении (N=622, n=4, SMD=0,01, 95% CI: -0,09– 0,12, p=0,79, I2=0%), правописании (N=260, N=3, SMD=0,03, 95% CI: -0,34– 0,40, p=0,89, I2=48,9%), или времени реакции (N=260, N=5, SMD=0,09, 95% CI: -0,13– 0,3, P=0,44, I2=0%)82.
N-ацетилцистеин является нутрицевтической формой аминокислоты цистеина, которая в изобилии содержится в высокобелковых продуктах, и действует как предшественник глутатиона, который обладает антиоксидантной активностью во всем организме.
Это была наиболее часто оцениваемая аминокислотная добавка при психических расстройствах. В смешанной выборке из 574 человек с высоким уровнем депрессии (коморбидной или первичной) адъювантное лечение N-ацетилцистеином (2-3 г/сут) достоверно снижало депрессивные симптомы (n=5, SMD=0,37, 95% CI: 0,19-0,55, p=0,001, I2=92,64%), но не оказывало влияния на воспринимаемое качество жизни (N=543, n=4, SMD=0,14, 95% CI: -0,04-0,32, p=0,14, I2=68%)72. Между исследованиями наблюдалась высокая неоднородность, но не было никаких доказательств системной ошибки публикаций.
У людей с расстройствами настроения (включая биполярное расстройство и БДР; N=493, n=3) N-ацетилцистеин в дозе 2-3 г/сут оказывал небольшое, но значительное влияние по сравнению с плацебо на общее функционирование (SMD=0,19, 95% CI: 0,01-0,39, p=0,04, I2=64%) и социальное функционирование (SMD=0,22, 95% CI: 0,03-0,41, p=0,02, I2=67%). Он также значительно улучшил другие показатели функциональных нарушений (SMD=0,31, 95% CI: 0,12-0,50, p=0,002, I2=86%)72.
В трех РКТ у людей с шизофренией (N=247) дополнительное лечение N-ацетилцистеином значительно снижало общую оценку симптомов (Р=0,74, 95% CI: 0,06-1,43, р=0,03). Хотя включенные исследования были оценены как высококачественные, общая сила доказательств была слабой из-за высокого риска системной ошибки публикации и значительной неоднородности существующих данных (I2=84%)56. В отношении подгрупп симптомов отмечалась незначительная тенденция к благоприятному влиянию на негативные симптомы (SMD=0,59, 95% CI: -0,10-2,00, p=0,08, I2=93%), но не было эффектов, выходящих за рамки плацебо для позитивных симптомов (SMD=0,16, 95% CI: -0,29-0,62, p=0,48, I2=66%) или общей симптоматики (SMD=0,2, 95% CI: -0,21-0,62, p=0,34, I2=59%) 56.
В качестве адъювантного лечения для лиц с биполярным аффективным расстройством (N=224, n=2), 2 г/сут N-ацетилцистеин не отличался от плацебо в его влиянии на общую тяжесть заболевания (Clinical Global Impression– Severity, CGI-S: SMD=0,11, 95% CI: -0,15– 0,37, p=0,42, I2=90%, и Clinical Global Impression– Improvement, CGI-I: SMD=0,16, 95% CI: -0,09 до 0,42, p=0,22, I2=0%) или оценки мании (N=224, N=2, SMD=0,05, 95% CI: -0,2– 0,31, р=0,68, I2=0,01%)72. N-ацетилцистеин также оказался неэффективным при депрессивных симптомах у людей с биполярным расстройством (N=124, n=2, SMD=0,59, 95% CI: -0,3-1,48, p=0,19, I2=83%)56.
У 155 лиц с обсессивно-компульсивным расстройством, принимающих препараты (в основном СИОЗС), при добавлении к терапии 2-3 г/сутки N-ацетилцистеина выявлена тенденция в сторону уменьшения обсессивно-компульсивных симптомов (N=4, SMD=0,295, 95% CI: -0,018–0,608, р=0,064, I2=65%)74. N-ацетилцистеин (2-2,4 г/сут) также не оказывал существенного влияния на симптомы тревоги в объединенной смешанной выборке людей с психическими расстройствами (N=319, n=2, SMD=0,03, 95% CI: -0,21– 0,28, p=0,80, I2=0%) 72.
Во всех вышеперечисленных расстройствах частота возникновения и усугубления нежелательных эффектов от приема N-ацетилцистеина существенно не отличалась от плацебо56,72,74. Не было выявлено достоверной разницы в частоте легких нежелательных эффектов (особенно в отношении желудочно-кишечных симптомов) у людей с шизофренией (N=186, n=2, OR=1,56, 95% CI: 0,87-2,80, p=0,14, I2=0)56, но добавление N-ацетилцистеина ассоциировалось с более высокими показателями легких нежелательных явлений при расстройствах настроения (N=574, n=5, OR=1,61, 95% CI: 1,01-2,59, p=0,049) 72.
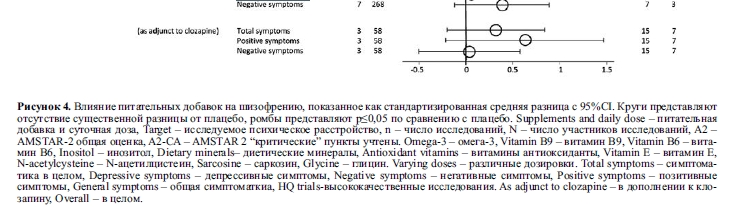
Влияние на негативные симптомы не достигало статистически значимого уровня (саркозин: N=132, n=4, SMD=0,32, 95% CI: -0,03-0,66, p=0,07; глицин: N=268, n=7, SMD=0,39, 95% CI: -0,11-0,9, p=0,13)57. Однако значительные преимущества для негативных симптомов наблюдались у лиц, получавших отличные от клозапина антипсихотики (саркозин: N=112, n=3, SMD=0,39, p=0,04; глицин: N=219, n=5, SMD=0,60, p=0,05; CI и I2 не представлены)57.
Как дополнение к лечению клозапином (N=58, n=3)58, глицин был неэффективен для позитивных (SMD=0,63, 95% CI: -0,21-1,48, I2 не сообщается), негативных (SMD=0,03, 95% CI: -0,51– 0,57, I2 не сообщается) и общих симптомов (SMD=0,32, 95% CI: -0,2– 0,84, I2 не сообщается). Не было получено достоверных данных о действии саркозина в качестве вспомогательного средства с клозапином.
Пребиотики и пробиотики
В нашем исследовании не было выявлено мета-анализов эффектов пребиотиков или пробиотиков на психические расстройства. Однако в группах лиц с легкой и умеренной депрессией (как определено по пороговым значениям на клинически валидированных шкалах), пробиотические препараты различных штаммов и доз снижали депрессивные симптомы значительно больше, чем плацебо (N=163, n=3, SMD=0,684, 95% CI: 0,0712-1,296, p=0,029)71.
Самой большой доказательной силой обладает питательная добавка с омега-3, в частности ЭПК. Многочисленные мета-анализы показали, что она оказывает значительное влияние на людей с депрессией, в том числе высококачественные мета-анализы с хорошей уверенностью в результатах, определенных AMSTAR-264. Данные мета-анализов показали, что омега-3 эффективен при назначении в дополнение к антидепрессантам51,64. Как монотерапия, данные менее убедительны для омега-3, пока препараты, содержащие ДГК не приносят очевидной пользы при БДР51,64.
Омега-3 добавки, по-видимому, имеют наибольшую пользу при введении в виде формул с высоким содержанием ЭПК, поскольку значительные взаимосвязи между дозировкой ЭПК и размерами эффекта также наблюдаются в высококачественных мета-анализах РКТ59,64. Новые данные РКТ также указывают на то, что омега-3 может быть наиболее полезным для пациентов, имеющих повышенные маркеры воспаления. Имеющиеся мета-анализы показывают, что прием омега-3 не эффективен у пациентов с депрессией как сопутствующей патологией хронических физических состояний65, в том числе кардиометаболических заболеваний, что было воспроизведено в последующих исследованиях84. В свете нынешних данных, омега-3, кажется, представляют собой безопасный адъювантный метод лечения.
Необходимы дополнительные исследования, касающиеся эффективности омега-3 добавок при других состояниях психического здоровья. Например, омега-3 был показан как потенциально полезный для детей с СДВГ, опять же с высокими дозировками ЭПК, дающими наибольшие эффекты79. Однако незначительные размеры эффекта после коррекции по систематической ошибке публикации, наряду с низким качеством обзора, выявленным AMSTAR-2, снижают уверенность в выводах. Кроме того, в то время как существующие данные мета-анализов обнаружили отсутствие значительных преимуществ у людей с шизофренией55,59, последующие испытания у молодых людей с первым психотическим эпизодом сообщили о более положительных, хотя и смешанных результатах85,86, предположительно приписываемых нейропротекторным эффектам87,88.
Было обнаружено, что дополнительное лечение добавками на основе фолатов значительно уменьшает симптомы БДР и негативные симптомы при шизофрении54,67. Однако в обоих случаях рейтинги AMSTAR-2 указывали на низкую уверенность в результатах обзора, а положительные общие эффекты в этих мета-анализах были обусловлены в основном РКТ высокой дозы (15 мг/сут) метилфолата. Метилфолат легко всасывается, преодолевая любые генетические предрасположенности к мальабсорбции фолиевой кислоты и успешно преодолевая гематоэнцефалический барьер. Действительно, плацебо-контролируемое исследование метилфолата при шизофрении сообщило о значительном увеличении количества белого вещества в течение всего 12 недель, что сопровождалось уменьшением негативных симптомов.
РКТ, не охваченные в нашем мета-обзоре92 и ретроспективном анализе диаграмм93, показали преимущества добавления метилфолата при других психических расстройствах. Учитывая это, наряду с отсутствием побочных эффектов (на самом деле, значительно меньше побочных явлений в выборках, получающих лечение по сравнению с плацебо), необходимы дальнейшие исследования метилфолата в качестве вспомогательного лечения психических расстройств.
Что касается других витаминов (таких как витамины Е, С или D), минералов (цинк и магний) или инозитола, то в настоящее время нет убедительных доказательств, подтверждающих их эффективность при любом психическом расстройстве, хотя следует упомянуть о новых доказательствах, касающихся положительного воздействия добавок витамина D при тяжелой депрессии.
Помимо витаминов, минералов и омега-3 жирных кислот, некоторые аминокислоты в настоящее время появляются в качестве перспективных вспомогательных средств лечения психических расстройств. Хотя доказательства все еще находятся в стадии становления, N-ацетилцистеин в частности (в дозах 2000 мг/сут или выше) был показан как потенциально эффективный для уменьшения депрессивных симптомов и улучшения функционального восстановления в смешанных психиатрических выборках72. Кроме того, значительное снижение общих симптомов шизофрении наблюдалось при использовании N-ацетилцистеина в качестве вспомогательного лечения, хотя и с существенной гетерогенностью между исследованиями, особенно по продолжительности исследования (на самом деле, N-ацетилцистеин имеет очень замедленное начало действия около 6 месяцев56,94).
N-ацетилцистеин действует как предшественник глутатиона, основного эндогенного антиоксиданта, нейтрализующего клеточный реактивный кислород и азот95. Производство глутатиона в астроцитах ограничено цистеином. Пероральный глутатион и L-цистеин расщепляются метаболизмом первого прохода и не увеличивают уровни глутатиона мозга, в отличие от перорального N-ацетилцистеина, который легче усваивается и, как было показано, увеличивает глутатион мозга в животных моделях96. Кроме того, было показано, что N-ацетилцистеин увеличивает высвобождение дофамина у животных моделей96.
N-ацетилцистеин может помочь в лечении шизофрении, биполярного аффективного расстройства и депрессии за счет снижения окислительного стресса и уменьшения глутаматергической дисфункции96, но имеет более широкие доклинические эффекты на митохондрии, апоптоз, нейрогенез и удлинение теломер неопределенного клинического значения.
NMDA-рецепторы активируются путем связывания с D-серином или глицином97. Саркозин является естественным ингибитором транспорта глицина и может выступать в качестве ко-агониста NMDA98. Как таковые, D-cерин, глицин и саркозин могут улучшить психотические симптомы через модуляцию NMDA99. Мы обнаружили снижение общих психотических симптомов, но не негативных симптомов, при применении глицина и саркозина. Кроме того, мы обнаружили, что глицин не был эффективен в комбинации с клозапином. Это может быть связано с тем, что клозапин уже действует как агонист участка глицина NMDA-рецептора97.
Роль микробиома кишечника в психическом здоровье также является быстро развивающейся областью исследований. Микробиота кишечника значительно отличается между людьми с психическими расстройствами и здоровым контролем, и недавние исследования фекальной трансплантации с использованием мышей без микробов показывают, что эти различия могут играть причинную роль в симптомах психического расстройства41,100,101.
В настоящее время начинают появляться интервенционные исследования, направленные на изучение влияния пробиотических препаратов на клинические исходы при психических расстройствах71. Мы включили один недавний мета-анализ, который оценивал объединенное влияние пробиотических вмешательств на депрессивные симптомы: в то время как первичный анализ не сообщил о значительном эффекте, умеренно большой эффект в трех включенных исследованиях предполагает, что пробиотики могут быть полезны для тех, у кого есть клинический диагноз депрессии, а не субклинические симптомы71. Однако необходимы дополнительные исследования, чтобы воспроизвести эти результаты, оценить долгосрочную безопасность пробиотических вмешательств и выяснить оптимальный режим дозирования и наиболее эффективные пребиотические и пробиотические штаммы102.
В то время как этот мета-обзор выделил потенциальные роли для использования питательных добавок, это не должно быть предназначено для замены улучшения рациона питания. Плохое физическое здоровье людей с психическими заболеваниями хорошо документировано103, и чрезмерное и нездоровое потребление пищи, по-видимому, является ключевым фактором этого4,5. Улучшение качества питания связано с уменьшением смертности от всех причин104, в то время как мультивитаминные и мультиминеральные добавки не могут улучшить продолжительность жизни18-20.
Мета-анализ диетических вмешательств у людей с тяжелыми психическими заболеваниями выявил преимущества по ряду аспектов физического здоровья105. Маловероятно, что стандартная добавка питательных веществ сможет охватить все полезные аспекты улучшенного питания. Кроме того, цельные продукты могут содержать витамины и минералы в различных формах, в то время как питательные добавки могут обеспечивать только одну форму. Например, витамин Е встречается естественным образом в восьми формах, но питательные добавки могут обеспечить только одну форму. Диетические вмешательства также уменьшают избыток пищевых элементов, таких как соль, которая является ключевым фактором преждевременной смертности13.
В то время как улучшение рациона питания, по-видимому, играет четкую роль в увеличении продолжительности жизни и предотвращении хронических заболеваний, в настоящее время нет исследований, оценивающих это у людей с психическими расстройствами. Кроме того, хотя недавние мета-анализы РКТ показали, что улучшение питания уменьшает симптомы депрессии в общей популяции106, необходимы более тщательно разработанные исследования для подтверждения преимуществ диетических вмешательств для людей с диагностированными психическими состояниями25.
Наши данные следует рассматривать в свете некоторых ограничений. Во-первых, хотя мета-анализы РКТ, как правило, представляют собой верхний уровень доказательств, важно признать, что многие из результатов, включенных в этот мета-обзор, имели значительную степень неоднородности между включенными исследованиями или были основаны на небольшом числе исследований. Следующим шагом в этой области исследований является переход от мета-анализа на уровне исследования к мета-анализу на уровне пациента, поскольку это позволит получить более персонализированную картину эффектов пищевых добавок, полученных в результате адекватного анализа модераторов, медиаторов и подгрупп. Кроме того, было бы желательно сравнить питательные добавки в одном и том же исследовании.
Признано, что люди с психическими расстройствами обычно принимают пищевые добавки в комбинации.
некоторых случаях, исследование поддерживало этот подход, наиболее обыкновенно в форме мультивитаминного/ минерального комплексов107. Однако недавние исследования в области депрессии показали, что ”больше не обязательно лучше», когда дело доходит до сложных формул108. Следует отметить, что недавние крупные клинические исследования пациентов с расстройствами настроения показали, что комбинации питательных веществ могут не иметь более мощный эффект, и в некоторых случаях плацебо было более эффективным47,108,109.
В заключении, в настоящее время существует огромное количество исследований, изучающих эффективность пищевых добавок у людей с психическими расстройствами, причем некоторые питательные вещества в настоящее время продемонстрировали эффективность в конкретных условиях, а другие – все более выраженный потенциал. Существует большая потребность в определении задействованных механизмов наряду с изучением последствий в конкретных группах населения, таких как молодежь и лица, находящиеся на ранних стадиях заболевания. Четко обоснован целевой подход, который может проявляться как направленное на биомаркеры лечение, основанное на ключевых уровнях питательных веществ, маркерах воспаления и фармакогеномике83,91,110.
Благодарности
J. Firth получает поддержку от Blackmores Institute Fellowship; J. Sarris от National Health and Medical Research Council (NHMRC) Clinical Research Fellowship (APP1125000); M. Berk от NHMRC Senior Principal Research Fellowship (APP1059660 and APP1156072). B. Stubbs читает клинические лекции при поддержке Health Education England and the National Institute for Health Research (NIHR) Integrated Clinical Academy Programme (ICA-CL-2017-03-001); K. Allott получает поддержку от Career Development Fellowship from the NHMRC (APP1141207); D. Siskind частично поддерживается Early Career Fellowship from the NHMRC (APP1111136); W. Marx поддерживается Deakin University postdoctoral fellowship. Мнения, выраженные в настоящем документе, принадлежат авторам, и могут не совпадать с мнением вышеупомянутых организаций.
DOI:10.1002/wps.20672
Редактура: к.м.н. Чумаков Е.М. (Санкт-Петербург)
Firth J, Teasdale SB, Allott K. The efficacy and safety of nutrient supplements in the treatment of mental disorders: a meta-review of meta-analyses of randomized controlled trials. World Psychiatry. 2019;18(3):308–24.
Роль питания в психическом здоровье становится все более признанной. Наряду с обычным приемом пищи, рацион питания также может включать «пищевые добавки», среди которых полиненасыщенные жирные кислоты (ПНЖК), витамины, минералы, антиоксиданты, аминокислоты и пре/пробиотики. В последнее время появилось большое количество мета-анализов изучения пищевых добавок при лечении психических расстройств. Чтобы подготовить мета-обзор этих важнейших данных, мы собрали и оценили все мета-анализы рандомизированных контролируемых исследований (РКТ), в которых сообщается об эффективности и безопасности пищевых добавок при частых и тяжелых психических расстройствах. Наш системный поиск выявил 33 мета-анализа плацебо-контролируемых РКТ с первичным анализом, включающих данные о результатах о 10951 человек. Наиболее убедительные доказательства были найдены в отношении ПНЖК (особенно эйкозапентаеновой кислоты) при использовании в качестве дополнительного средства в лечении депрессии. Более новые данные свидетельствуют о том, что ПНЖК также могут быть полезны при синдроме дефицита внимания/гиперактивности, в то время как доказательств эффективности при лечении шизофрении не получено. Добавки на основе фолата широко исследовались как адъювантная терапия при лечении депрессии и шизофрении, с положительным эффектом при высоких дозах метилфолата в РКТ при лечении большого депрессивного расстройства. Появились новые данные в пользу того, что N-ацетилцистеин является полезным вспомогательным средством при расстройствах настроения и шизофрении. Все пищевые добавки имели хорошие профили безопасности, без признаков серьезных побочных эффектов или противопоказаний к применению вместе с психиатрическими препаратами. В заключении, врачи должны быть проинформированы о пищевых добавках с установленной эффективностью для лечения определенных состояний (таких как эйкозапентаеновая кислота при депрессии), но также должны быть осведомлены о тех пищевых добавках, которые пока не имеют должной доказательной базы. Будущие исследования должны быть направлены на изучение основных механизмов действия, а также на то, какие лица могут извлечь наибольшую пользу из этих пищевых добавок.
Ключевые слова: пищевые добавки, полиненасыщенные жирные кислоты, омега-3, эйкозапентаеновая кислота, метилфолат, витамин D, N-ацетилцистеин, депрессия, шизофрения, синдром дефицита внимания/гиперактивности, адъювантное лечение.
В настоящее время имеются многочисленные данные, свидетельствующие о том, что люди с психическими расстройствами обычно потребляют избыточное количество продуктов с высоким содержанием жира и сахара, при недостаточном потреблении продуктов с высоким содержанием питательных веществ по сравнению с населением в целом1-5. Связь между неправильным питанием и психическими заболеваниями, по-видимому, сохраняется даже при учете других факторов, которые могли бы объяснить эту связь, таких как социальная депривация или ожирение, и не объясняется обратной причинно-следственной связью1,6.
Кроме того, хотя метаболические и гормональные побочные эффекты психотропных препаратов могут влиять на прием пищи7,8, неправильное питание, по-видимому, присутствует даже до постановки психиатрических диагнозов. Например, при депрессии, плохое питание предшествует и действует как фактор риска для развития расстройства6,9,10. Аналогично при психотических расстройствах, различные дефициты питания проявляются еще до начала антипсихотического лечения11.
В настоящее время ясна роль диеты для поддержания физического здоровья, так как изучено влияние питания на развитие кардиометаболических заболеваний, рака и преждевременной смертности12,13. Параллельно все больше признается потенциальное влияние диеты на психические расстройства14,15. Однако, питательные вещества могут потребляться в пищу не только при обычных приемах пищи, но и в виде пищевых добавок16. Добавки, как правило, используют для: а) коррекции недостаточного питания (или при низком уровне питательных веществ в плазме); б) приема специфических питательных веществ в больших чем обычно дозах, для достижения определенных физиологических целей; в) обеспечения питательных веществ в более биодосутпной форме, что важно для людей с генетическими особенностями или при проблемах со здоровьем, при которых усвоение питательных веществ может быть нарушено. Эти добавки могут быть получены как синтетическим путем, так и естественным, непосредственно из пищи. Как правило, речь идет о витаминах (например, фолиевая кислота, витамин D), минералах (например, цинк, магний), пре- и пробиотиках (из конкретных штаммов кишечных бактерий), полиненасыщенных жирных кислотах (ПНЖК) (обычно омега-3 рыбные масла) или аминокислотах (например, N-ацетилцистеин, глицин).
Питательные добавки широко используются в популяции. Например, в США более половины взрослого населения принимают те или иные пищевые добавки17. Но доказательств того, что такое широкое применение снижает заболеваемость или преждевременную смертность, нет (даже наиболее качественные исследования, например витамина D18 и E19,20, были отрицательными). Тем не менее, некоторые конкретные питательные добавки связаны с пользой для здоровья у конкретных групп населения или клинических состояний (например беременным женщинам рекомендуется добавить в рацион фолиевую кислоту, для снижения риска развития дефицита нервной трубки у плода21; при тяжелой анемии рекомендуется назначается витамин B1222; пероральный прием препаратов цинка – терапия первой линии при болезни Вильсона23; и национальная медицинская ассоциация рекомендует омега-3 жирные кислоты пациентам с перенесенным инфарктом миокарда24).
В настоящее время наблюдается повышенный академический и клинический интерес к роли питательных добавок для лечения различных психических расстройств14-16. Этот рост исследований частично объясняется нашим развивающимся пониманием нейробиологических основ психических заболеваний, которые подразумевают использование определенных питательных веществ в качестве вспомогательного лечения по целому ряду причин25.
Во-первых, недавние клинические исследования показали, что многие психические расстройства сопряжены с повышением уровня маркеров окислительного стресса и воспаления26-29, а также была отмечена связь между эффективностью фармакологических препаратов и коррекцией образа жизни при психических расстройствах с изменением этих биомаркеров30,31. Таким образом, антиоксидантные и противовоспалительные свойства некоторых пищевых добавок (таких как N-ацетилцистеин32 и омега-3 жирные кислоты33) указывают на то, что они могут быть полезны при лечении психических расстройств, вызванных воспалением и окислительным стрессом.
Во-вторых, в настоящее время имеются данные крупных исследований, показывающие, что психотические расстройства и расстройства настроения связаны со снижением сывороточного уровня основных питательных веществ, таких как цинк34,35, фолат36,37 и витамин D38,39. Поскольку эти дефициты, вероятно, связаны со степенью ответа на лечение и клиническим исходом в этих популяциях11,34,40, существует возможность того, что добавление питательных веществ может улучшить результаты лечения.
В-третьих, появляются некоторые данные о том, что психические расстройства могут быть связаны с дисфункцией кишечного микробиома41,42. Поскольку кишечные бактерии могут быть модифицированы с помощью микронутриентов и пре/пробиотиков43,44, это позволяет предположить, что некоторые пре/пробиотические добавки могут быть потенциально полезными новыми терапевтическими вариантами, заслуживающими дальнейшего исследования45,46.
Наряду с теоретическим потенциалом пищевых добавок, нацеленных на определенные аспекты психических расстройств, существует также огромное количество клинических испытаний и мета-анализов, изучающих их использование в психиатрическом лечении в качестве профилактики47,48. Тем не менее, их роль все еще остается неясной. Это, вероятно, связано с отсутствием четкого и современного руководства для врачей и исследователей в отношении их: а) относительной эффективности для улучшения клинических исходов у людей с психическими заболеваниями; и б) безопасности для использования, особенно в сочетании с препаратами психиатрического профиля.
Цель настоящего мета-обзора состоит в том, чтобы обобщить и оценить данные высшего уровня об эффективности и безопасности пищевых добавок при лечении психических расстройств, а также изучить условия, при которых они могут быть эффективными. Для этого мы идентифицировали, синтезировали и оценили все доступные данные из мета-анализов рандомизированных контролируемых исследований (РКТ), изучающих качество доказательств для всех пищевых добавок при различных психических расстройствах. Наряду с предоставлением четкого обзора эффективности конкретных питательных добавок при различных расстройствах, мы также стремились изучить, какие дозы и симптоматические цели являются наиболее подходящими, в то же время дополнительно сообщая о безопасности и переносимости.
МЕТОДЫ
Стратегия поиска и синтез данных были проведены в соответствии с заявлением PRISMA49 и следовали предварительно зарегистрированному протоколу (PROSPERO: CRD42018105880).Систематический поиск
Алгоритм поиска заголовков и ключевых слов представлен в Таблице 1. Систематический поиск проводился с использованием Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, Health Technology Assessment Database, Allied и Complementary Medicine (AMED), PsycINFO и Ovid MEDLINE(R) по состоянию на 1 февраля 2019 года.
Поиск Google Scholar был проведен с использованием тех же ключевых слов, чтобы выявить любые дополнительные соответствующие статьи. Также был проведен поиск по спискам литературы включенных в обзор статей.

Критерии отбора
Критерии отбора были организованы в соответствии со структурой отчетности PICO (Участники (Participants), Вмешательства (Interventions), Сравнения (Comparisons), Результаты (Outcomes)), как описано ниже.
Участники
Мы включили исследования лиц с часто встречающимися и тяжелыми психическими расстройствами, т.е. депрессивными расстройствами, биполярным аффективным расстройством (тип I и II), шизофренией и другими психотическими расстройствами, тревожными и связанными со стрессом расстройствами, диссоциативными расстройствами, расстройствами личности и синдромом дефицита внимания/гиперактивности (СДВГ). Были также включены исследования лиц, отвечающих критериям “сверхвысокого риска” или “клинического высокого риска” развития психотического расстройства.Все исследования вышеуказанных состояний были отобраны при условии, что по меньшей мере 75% выборки имели подтвержденное психическое заболевание или состояние риска, подтвержденное либо клиническим анамнезом, либо достижением установленных пороговых значений при достоверных скрининговых исследованиях. Исследования, изучающие влияние пищевых добавок на психическое здоровье в общей популяции, включались только в том случае, если имелись данные из подгруппы людей с психическими заболеваниями (при этом 75% выборки соответствовали вышеуказанным критериям). Исследования, изучающие пищевые добавки только для улучшения дефицита питания, связанного с расстройствами пищевого поведения или злоупотребления психоактивными веществами, были исключены. Исследования, изучающие нарушения развития центральной нервной системы (например, аутизм, умственная отсталость) или нейродегенеративные расстройства (например, деменция), также не включались.
Вмешательства
Все питательные добавки, рассмотренные для этого мета-обзора, использовались или как дополнительная терапия, или в качестве монотерапии. Питательные добавки были определены как витамины, минералы, макроэлементы, жирные кислоты или аминокислоты (включая пероральные формы), обычно встречающиеся в рационе человека. Метаанализ модификации диеты и травяных добавок включен не был.
Сравнения
Поскольку это исследование было направлено на предоставление доказательств высшего уровня, были включены только мета-анализы РКТ.
Результаты
Все данные о изменениях физического и/или психического здоровья (включая изменения в клинических показателях, частоте ответов и побочных эффектах) из мета-анализов РКТ, изучавших пищевые добавки для любого расстройства, соответствующего критериям включения, были включены в этот мета-обзор. Мета-анализ классифицировался как приемлемый, если: а) он четко указывал критерии отбора, исследования и сравнения, согласованные с критериями участника, исследования и сравнения, перечисленными выше; б) он сообщал о систематическом поиске с процедурой скрининга; в) он использовал систематическое извлечение данных и сообщал объединенные непрерывные или категориальные данные о результатах более чем одного исследования.Там, где перекрещивались данные о пищевой добавке для конкретного результата/расстройства, использовался самый последний обновленный мета-анализ, если он охватывал более 75% испытаний в более ранней версии. В тех случаях, когда более ранние мета-анализы представляли уникальные результаты, путем включения большего числа исследований или использования отдельных анализов подгрупп, эти данные использовались в качестве дополнительных анализов для нашего мета-обзора.
Оценка качества включенных мета-анализов
Качество соответствующих критериям включения мета-анализов оценивалось с использованием 2 версии «Инструмента для проведения оценки систематических обзоров» (“A Measurement Tool to Assess Systematic Reviews” Version 2 (AMSTAR-2))50, обновленной версии оригинального AMSTAR, предназначенной для лучшей оценки качества обзора и уверенности в результатах.AMSTAR-2 оценивает 16 пунктов, которые отражают качество систематического обзора/мета-анализа. Семь из них были определены как “критические», которые использовались для определения общей уверенности в результатах обзора50. Для целей нашего мета-обзора включенные мета-анализы были оценены по всем 16 пунктам AMSTAR-2, и также получили отдельную оценку за количество “критических” пунктов.
Извлечение и анализ данных
Первичный анализ был сфокусирован на влиянии питательных веществ на показатели физического или психического здоровья, полученные в результате соответствующих мета-анализов. Для каждой пищевой добавки, при каждом расстройстве, мы вручную извлекли данные о степени эффекта в виде стандартизированных средних различий (SMD) с 95% доверительными интервалами (CI) по сравнению с плацебо, а также сообщили о вероятности случайности при сравнении (значение p). Данные были первоначально извлечены пятью авторами (KA, ST, WM, MS, DS), а затем перепроверены на качество с дублированием извлечения данных четырьмя независимыми авторами (JF, BS, JC, FS).В соответствии с общепринятыми трактовками, SMD были классифицированы как незначительные (<0,2), малые (0,2-0,4), умеренные (0,4-0,8) или большие (>0,8). В тех случаях, когда мета-анализы давали размеры эффекта, скорректированные на системную ошибку, это сообщались вместе с основными наблюдаемыми эффектами и интерпретировались как первичные результаты анализа. В тех случаях, когда непрерывные результаты были представлены в виде взвешенных средних различий или необработанных средних различий, они были пересчитаны в SMD (Hedges’ g) с использованием комплексного мета-анализа 3.0. В тех случаях, когда оригинальные мета-анализы сообщали о положительном влиянии питательных веществ в виде отрицательных величин эффекта (чтобы представить уменьшение симптомов), они были перекодированы в положительные, так что все представленные здесь величины эффекта являются положительными значениями, которые непосредственно указывают на пользу от использования питательных веществ по сравнению с плацебо, или отрицательными значениями, когда плацебо было связано с лучшими результатами, чем влияние питательных веществ. В тех случаях, когда мета-анализ применял модели фиксированных эффектов для расчета размеров эффекта пищевых добавок по сравнению с плацебо, они также пересчитывались с использованием модели случайных эффектов, так что SMD между добавками/расстройствами подлежали сравнению.
Результаты вторичных анализов, фокусирующихся на безопасности и переносимости, как правило, сообщались как категориальные исходы (относительные частоты нежелательных эффектов или прекращения лечения в сравнениях применения препаратов с плацебо). Они были извлечены в виде коэффициентов шансов (OR) или коэффициентов риска (RR) в соответствии с первоначальными результатами.
Как для первичного, так и для вторичного анализа мы также извлекли число участников (N), а также количество исследований/сравнений (n), из которых был получен размер объединенного эффекта. Кроме того, гетерогенность была количественно определена с использованием статистики I2 и классифицирована как низкая (I2<25%), умеренная (I2=25-50%) или высокая (I2>50%).
Там, где сообщалось, были также извлечены все дополнительные характеристики исследования, особенно в отношении используемой пищевой добавки (включая тип, дозу и остальные факторы), образец и диагностические детали, а также любые соответствующие выполненные анализы подгрупп (например, разделение испытаний высокого/низкого качества, конкретных подвыборок пациентов или уровней дозировки).
Потенциальное влияние системной ошибки публикации оценивалось везде, где имелись достаточные данные для соответствующего анализа, и скорректированные размеры эффекта (при контроле за небольшим системной ошибкой исследования) представлены вместе с основными выводами.
РЕЗУЛЬТАТЫ
 Результаты систематического поиска
Результаты систематического поискаПоиск обнаружил 1194 результатов, которые были уменьшены до 737 после удаления дубликатов. Еще одна потенциально приемлемая статья была получена из дополнительного поиска Google Scholar. Оценка заголовков и абстрактов отсеяла еще 597 статей, в то время как 141 статья была извлечена и рассмотрена в полном объеме. Из них 108 не подходили для участия. Таким образом, в общей сложности для этого мета-обзора были включены приемлемые данные из 33 независимых мета-анализов РКТ пищевых добавок при психических расстройствах (см. Рисунок 1).
Мета-анализы изучали РКТ полиненасыщенных жирных кислот, витаминов, минералов, аминокислотных добавок и пре/пробиотиков, с первичным анализом, включавшим результаты в общей сложности от 10951 человека. Все мета-анализы основывались на питательных добавках, вводимых в сочетании с “обычным лечением” (без указания схем лечения) или в качестве дополнительного лечения к определенному классу психотропных препаратов (например, селективные ингибиторы обратного захвата серотонина (СИОЗС) при депрессии или антипсихотики при шизофрении). Только один из мета-анализов сообщил о питательной добавке в качестве монотерапии для психического расстройства (т.е. омега-3 жирные кислоты для депрессии), в то время как другие специально не исключали пациентов, принимающих лекарства. Никакие мета-анализы напрямую не сравнивали пищевые добавки с психотропными препаратами. Все исследования51-82 были плацебо-контролируемыми.
Конкретные психические состояния (и отмеченные результаты лечения), рассматриваемые в этом мета-обзоре, включают: шизофрению (изучение общих симптомов наряду с позитивными, негативными, общими и депрессивными симптомами и позднюю дискинезию)52-59; состояния риска развития психоза (изучение ослабленных симптомов психоза, негативных симптомов, перехода к психозу и функционирования)60-63; депрессивные расстройства (включая любую клиническую депрессию, диагностированное большое депрессивное расстройство (БДР), депрессию во время беременности, в пожилом возрасте или как сопутствующую патологию к хроническим состояниям здоровья)51,59,64-73; состояния, связанные с тревогой и стрессом (включая генерализованное тревожное расстройство, обсессивно-компульсивное расстройство (ОКР) и трихотилломанию)68,72,74; биполярное аффективное расстройство I и II типов (изучение общих симптомов, биполярной мании, биполярной депрессии, функциональных нарушений и качества жизни)56,68,72,75,76; и СДВГ (включая сложные симптомы, гиперактивность-импульсивность, невнимательность, поведенческие сопутствующие нарушения, такие как агрессия, и когнитивное функционирование)77-82.
Оценка качества включенных метаанализов
Оценка качества мета-анализов приводится вместе с соответствующими результатами на рисунках 2-7. Мета-анализы были оценены между 4 и 16 пунктами AMSTAR-2 (медиана: 12, среднее значение: 12). Большинство мета-анализов (25 из 33) придерживались пяти или более из семи “критических” пунктов, но только пять из них придерживались всех пунктов52,58,64,78,80. Двадцать шесть из тридцати трех включенных метаанализов были опубликованы в 2016-2019 годах.Эффективность и безопасность пищевых добавок при психических расстройствах
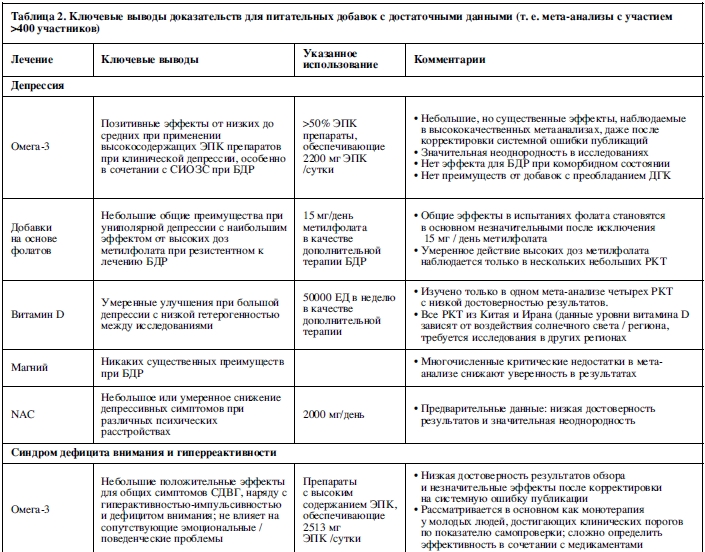
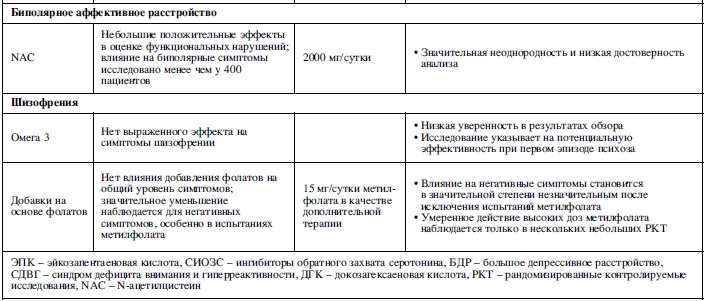
На рисунках 2-7 показана эффективность добавок питательных веществ (как определено мета-анализами) для всех клинических исходов, зарегистрированных в различных психических состояниях, включая депрессивные расстройства (Рисунок 2), тревожные расстройства (Рисунок 3), шизофрению (Рисунок 4), состояния риска развития психоза (Рисунок 5), биполярное аффективное расстройство (Рисунок 6) и СДВГ (Рисунок 7). На этих рисунках также показано общее качество мета-анализа. Питательные добавки с достаточным количеством данных (т.е. из мета-анализа с участием >400 участников) выделены в таблице 2. Для всех оцениваемых питательных веществ особенности этих результатов, наряду с данными о безопасности и переносимости, подробно описаны ниже.










Витамины и минералы
Добавки на основе фолатовНаиболее широко оцененной витаминной добавкой для лечения психических расстройств был витамин В9, который также называют “фолат». Его можно вводить как добавку в виде фолиевой кислоты, фолиниевой кислоты или метилфолата (который также известен как l-метилфолат, левомефоловая кислота или 5-метилтетрагидрофолат).
В качестве дополнения к СИОЗС у 904 лиц с униполярной депрессией (в основном БДР), добавки на основе фолатов (включая фолиевую кислоту и метилфолат, вводимые в различных дозах) были связаны со значительным снижением депрессивных симптомов по сравнению с плацебо, хотя между исследованиями была большая гетерогенность (n=7, SMD=0,37, 95% CI: 0,01-0,72, p=0,04, I2=79%)67.
При введении витамина В9 в виде фолиевой кислоты (0,5-10 мг/сут) достоверного влияния на депрессивные симптомы не наблюдалось (N=657, n=4, SMD=0,4, 95% CI: -0,08– 0,88, p=0,1, I2=83%). Значительные эффекты наблюдались в двух испытаниях с использованием низкой дозы (<5 мг/сут) фолиевой кислоты (N=190, SMD=0,57, 95% CI: 0,23-0,91, p<0,001, I2=25%), в то время как не наблюдалось существенных преимуществ от доз ≥5 мг/сут (N=467, n=2, SMD=0,24, 95% CI: -0,56-1,03, p=0,56, I2=76%)67.
Два РКТ, исследовавшие высокую дозу (15 мг/сут) метилфолата (наиболее биоактивного метаболита фолиевой кислоты) в качестве вспомогательного средства для лечения БДР, обнаружили от умеренного до большого влияния на депрессивные симптомы (N=99, n=2, SMD=0,73, 95% CI: 0,28-1,19, p=0,002, I2=3%)67. Не было никаких свидетельств неблагоприятных последствий или статистической неоднородности. Однако при включении более низких доз метилфолата (7,5 мг / сут) не наблюдалось значимых эффектов на депрессию (N=249, n=3, SMD=0,34, 95% CI: -0,4– 1,08, p=0,37, I2=81%).
Семь РКТ (N=340) исследовали добавки на основе фолатов в качестве вспомогательного лечения шизофрении54. Витамин В9 вводили в виде метилфолата (n=2) или фолиевой кислоты (n=5), а также в комбинации с витаминами В6 и В12 (n=3). В общем анализе небольшие эффекты витамина В9 на общие симптомы не были статистически значимыми (SMD=0,20, 95% CI: -0,02-0,41, p=0,08, I2=0), а анализ подгрупп высококачественных исследований подтвердил отсутствие общих эффектов (N=231, n=3, SMD=0,15, 95% CI: -0,11-0,42, p=0,26, I2=0%). Добавки на основе фолиевой кислоты были неэффективны по суммарной оценке симптомов при введении в виде фолиевой кислоты (N=268, n=5, SMD=0,13, 95% CI: -0,12- 0,37, p=0,32, I2=0%), даже в сочетании с другими гомоцистеин-редуцирующими витаминами группы В (т.е. В6 и В12) (N=219, n=3, SMD=0,18, 95% CI: -0,13- 0,5, p=0,24, I2=16%). Однако влияние на суммарную оценку симптомов в двух исследованиях высоких доз метилфолата (15 мг/сут) приближалось к статистической значимости (N=72, n=2, SMD=0,45, 95% CI: 0,02-0,92, p=0,06, I2=0%).
Добавки на основе фолатов не оказывали существенного влияния на позитивные симптомы, общую психопатологию или депрессивные симптомы у пациентов с шизофренией54. Однако они уменьшали негативные симптомы в большей степени, чем плацебо (N=281, n=5, SMD=0,25, 95% CI: 0,01-0,49, p=0,04, I2=0). Эффект сохранялся в высококачественных РКТ (N=190, n=2, SMD=0,30, 95% CI: 0,00-0,60, p=0,05, I2=0), но стал несущественным при исключении РКТ с использованием 15 мг/сут метилфолата (N=226, n=4, SMD=0,23, 95% CI: -0,04-0,50, p=0,10, I2=0%)54.
Достоверно выявлена более низкая частота серьезных нежелательных явлений по сравнению с плацебо в течение использования фолатов у больных шизофренией (N=241, n=4, RR=0,32, 95% CI: 0,12-0,82, p=0,02, I2=0%)54.
Инозитол
При общем анализе влияния инозитола (3,6-19 г/сут, медиана 12 г/сут) на депрессивные симптомы при биполярном аффективном расстройстве, униполярной депрессии и предменструальном дисфорическом расстройстве достоверных отличий от плацебо обнаружено не было (N=188, n=7, SMD=0,35, 95% CI: -0,2– 0,89, p=0,22, I2=70%)68. Инозитол также был неэффективен при исследовании в качестве дополнения к СИОЗС при БДР (N=78, n=2, SMD=-0,17, 95% CI: -0,66– 0,33, p=0,50, I2=0%) и для депрессивных симптомов при предменструальном дисфорическом расстройстве (N=58, n=2, SMD=1,15, 95% CI: -0,08– 2,39, p=0,07, I2=78%)68.При шизофрении прием инозитола (6-12 г/сут) не превосходил плацебо по суммарной оценке симптомов (N=66, n=3, SMD=0,155, 95% CI: -0,35– 0,58, p=0,63, I2=87,2%)53. Среди лиц с биполярным аффективным расстройством инозитол (5,7-19 г/сут) не оказывал влияния на депрессивные симптомы (N=42, n=2, SMD=-0,11, 95% CI: -0,75– 0,52, p=0,72, I2=0%) или уровень ответа на лечение (RR=0,63, 95% CI: 0,35-1,12, p=0,12, I2=22%)68. При тревожных расстройствах инозитол (12-18 г/сут) не оказывал влияния на оценки шкалы тревоги Гамильтона (N=52, n=2, SMD=0,04, 95% CI: -0,58 – 0,51, p=0,89) и оценки симптомов в группах пациентов с ОКР (N=46, n=2, SMD=0,15, 95% CI:– 0,43-0,73, p=0,60)68.
Прекращение приема не приводило к различиям в группах пациентов с приемом инозитола и плацебо68. Однако прием инозитола был связан с тенденцией к более высокой частоте желудочно-кишечных расстройств, в сравнении с плацебо (N=183, n=6, SMD=3,26, 95% CI: 0,94-11,34, p=0,06, I2=0%).
Другие витамины и минералы
Установлено, что витамин D достоверно снижает депрессивные симптомы у пациентов с клинической депрессией (N=948, n=4, SMD=0,58, 95% CI: 0,45-0,72, p<0,01, I2=0%). Эта оценка включала данные не слепых исследований с использованием внутримышечных инъекций69. Тем не менее, при повторном анализе данных с использованием только двойных слепых РКТ пероральных добавок аналогичные положительные эффекты наблюдались при дозах 1,500-7,143 МЕ/сут (N=828, n=3, SMD=0,57, 95% CI: 0,43-0,71, p<0,001, I2=0%).Одиннадцать РКТ исследовали эффективность минеральных добавок для лечения депрессии, используя либо цинк, либо магний. Цинк вводился в дозе 25 мг/сут в качестве дополнительного лечения БДР и оказывал умеренное значимое влияние на депрессивные симптомы (N=104, n=4, SMD=0,66, 95% CI: 0,26-1,06, p<0,01)65. Хотя не было никаких доказательств гетерогенности (I2=0%), все включенные РКТ были идентифицированы как имеющие высокий риск отсева из-за отсутствия анализа намерения лечения у пациентов. У лиц с депрессией, выявленной с помощью самоотчетных измерений, добавление магния в дозе 225-4000 мг/сут не имело эффектов, выходящих за рамки плацебо (N=538, n=8, SMD=0,22, 95% CI: -0,17– 0,48, I2=30,9%)70. Нет доступных данных о магнии в качестве вспомогательного лечения при диагностированном БДР.
При объединенном анализе антиоксидантных витаминов (Витамин С и витамин Е: N=340, n=6, SMD=0,296, 95% CI: -0,39– 0,98, p=0,40, I2=40,6%); минеральных добавок (цинк и хром: N=129, n=2, SMD=0,324, 95% CI: -0,48– 1,13, p=0,43, I2=0%); или витамина В6 (N=75, n=3, SMD=0,682, 95% CI: -0,09– 1,45, Р=0,08, I2=58,4%) значительных терапевтических эффектов не выявлено53.
Как терапевтический вариант для управления побочными эффектами антипсихотиков, витамин Е не показал никаких отличий от плацебо по уровням улучшения при тардивной дискинезии52. Тем не менее, он достоверно снижал риск “обострения” тардивной дискинезии в течение 1 года (N=85, n=5, RR=0,23, 95% CI: 0,07-0,76), хотя этот результат был основан на низкокачественных исследованиях52.
Все витаминные и минеральные добавки, по-видимому, имеют хорошие профили безопасности при шизофрении, причем ни одна из них не вызывает большего числа побочных явлений чем плацебо52,53.
Полиненасыщенные жирные кислоты
Депрессия и биполярное аффективное расстройствоПолиненасыщенные жирные кислоты являются наиболее широко оцениваемой пищевой добавкой при различных психиатрических состояниях, вводимой в виде омега-3 жирных кислот, включая эйкозапентаеновую кислоту (ЭПК) и докозагексаеновую кислоту (ДГК), и омега-6 жирных кислот, таких как линолевая кислота (ЛК).
В 13 независимых РКТ c 1233 людьми с БДР, добавки с омега-3 (средняя дозировка: 1422 мг/сутки ЭПК) уменьшили депрессивные симптомы (SMD=0,398, 95% CI: 0,114-0,682, р=0,006, I2 неизвестен), без доказательств о систематической ошибке64. При использовании в дополнении к антидепрессантам при БДР, омега-3 жирные кислоты (930-4400 мг/сутки ЭПК) также произвели среднее влияние на депрессивные симптомы (N=448, n=11, SMD=0.608, 95% CI: 0.154-1.062, p=0.009, I2=82%), хотя была некоторая индикация систематической ошибки75 в публикации. Последующий анализ омега-3 в качестве вспомогательного средства к антидепрессантам при БДР дал аналогичные результаты (N=402, n=10, SMD=0.48, 95% CI: 0.11-0.84, p=0.01, I2=64%), хотя и вновь продемонстрировал доказательства значительной системной ошибки в публикации65. Поправка на системную ошибку в публикации позволила получить меньшие (но все же значимые) оценки эффектов омега-3 в качестве вспомогательного лечения БДР (SMD=0,19, 95% CI: 0,00-0,38, p=0,049).
Анализы подгрупп показали, что добавки омега-3 были эффективны только в качестве вспомогательного лечения БДР в когортах без сопутствующих заболеваний (N=201, n=6, SMD=0,74, 95% CI: 0,34-1,13, p<0,01, I2=42%), тогда как не было никаких признаков эффективности в группах, где БДР встречалось в сочетании с кардиометаболическими или неврологическими заболеваниями (N=201, n=4, SMD=0,05, 95% CI: -0,4-0,5, p=0,82, I2=45%)65. Кроме того, омега-3 были неэффективны для лечения БДР у беременных (N=121, n=3, SMD=0,24, 95% CI: -0,73– 1,21, p=0,63, I2=85%)59. Дальнейший анализ подгрупп лиц с депрессией (но без диагноза БДР) выявил небольшие положительные эффекты омега-3 при депрессивных симптомах (N=759, n=12, SMD=0,22, 95% CI: 0,01-0,43, p<0,05, I2=46%).
В исследованиях рассматривавших различные омега-3 кислоты для лиц с любой клинической депрессией, дополнения препаратов, содержащих ≥50% докозагексаеновой кислоты не имели никаких преимуществ перед плацебо (N=469, n=6, SMD=-0.028, 95% CI: -0.21-0.16, p>0.1)51. Однако добавки омега-3, содержащие >50% ЭПК, оказывали умеренно выраженное положительное влияние на депрессивные симптомы (N=969, n=23, SMD=0,61, 95% CI: 0,38-0,85, p<0,001). Снова, системная ошибка публикации была очевидна, и оцененные положительные влияния омега-3 препарата с высоким содержанием ЭПК были уменьшены, но все еще оказывались значительными даже после корректировки (SMD=0,42, 95% CI: 0.18-0.65, Р<0.001).
Дальнейший анализ различных форм ЭПК указал на несколько большее влияние на депрессивные симптомы в исследованиях с использованием препарата более 12-ти недель (N=274, n=4, SMD=1,07, р<0,01), по сравнению с периодом менее 12-недель (N=695, n=19, SMD=0,55, р<0,001), и с теми, кто использует омега-3 в качестве дополнительной терапии (N=535, n=15, SMD=0,72, р<0,001), а не в качестве монотерапии при депрессии (N=434, n=8, SMD=0,44, р=0,017)51.
Исследование у пациентов возрастом ≥65 лет с клинической депрессией (или с пограничными значениями на основании методов самооценки), показало, что омега-3 (средняя дозировка 1,3 г/сутки ЭПК/ДГК) имел значительно большее влияние на депрессивные симптомы в сравнении с плацебо (SMD=0,94, 95% CI: 0,5-1,37, p<0,001, I2=32,7%), хотя только в ограниченном количестве исследований с небольшим числом участников (N=187, n=4).
Во всех плацебо-контролируемых исследованиях омега-3 ПНЖК у людей с биполярным аффективным расстройством, эффекты на манию не были значимыми (N=242, n=6, SMD=0,198, 95% CI: -0,037– 0,433, p=0,10, I2=0%), хотя были небольшие положительные эффекты на депрессию (N=305, n=6, SMD=0,338, 95% CI: 0,035-0,641, p=0,029, I2=30%)75. Анализ, включающий только двойные слепые исследования, обнаружил аналогичные положительные эффекты для биполярной депрессии, хотя и не достигшие статистической значимости (N=150, n=4, SMD=0.36, 95% CI: -0.01– 0.73, p=0.051, I2=8%)76. Большинство исследований были определены как имеющие низкий риск системной ошибки, и не показали никаких признаков того, что омега-3 увеличил частоту нежелательных явлений или мании/гипомании при биполярном аффективном расстройстве.
Шизофрения и состояния, подверженные риску психоза
В качестве адъювантного лечения для людей с шизофренией эффект омега-3 (2-3 г/сут ЭПК) не достигал статистической значимости на общую оценку симптомов (N=335, n=7, SMD=0,242, 95% CI: -0,028– 0,512, p=0,08, I2=33,8%)55. Добавки омега-3 не выявили значимого влияния на депрессивные симптомы у людей с шизофренией (N=264, n=4, SMD=0,14, 95% CI: -0,11– 0,39, p=0,28, I2=8%) 59.Три исследования (N=512), изучавшие влияние омега-3 (1200-1400 мг/сут) в качестве монотерапии для предотвращения развития психоза у молодых людей, отвечающих критериям “риска”, не показали никаких признаков положительного влияния (все р>0,1) по сравнению с плацебо в течение 26 недель (OR=0,64, 95% CI: 0,15-2,68) или 52 недель (OR=0,64, 95% CI: 0,18-2,26)60.
У молодых людей в группе риска психоза, добавки ПНЖК также были неэффективны в течение 52 недель для уменьшения ослабленных психотических симптомов (N=347, n=3, SMD=0,31, 95% CI: -0,26– 0,88, I2=80%)61, негативных симптомов (N=347, n=3, SMD=0,06, 95% CI: -0,35– 0,46, I2=63%)62 и функциональных нарушений (N=252, n=2, SMD=-0,08, 95% CI: -0,33– 0,17)63. Аналогичные нулевые эффекты также наблюдались в более коротких (т.е. 12 и 26 недель) временных интервалах61-63.
Изучение профилей безопасности показало, что ЭПК хорошо переносится при психотических расстройствах и не вызывает побочных эффектов, кроме легкого расстройства желудочно-кишечного тракта55. В группах риска, пробное снижение применяемых препаратов омега-3 не отличалось от плацебо60
Синдром дефицита внимания и гиперреактивности
У молодых людей и детей с СДВГ общий анализ любых добавок ПНЖК (включая любые добавки омега-3 и омега-6 в различных дозах), показал значительные эффекты, выходящие за рамки плацебо для оценки симптомов СДВГ (N=1689, n=18, SMD=0,192, 95% CI: 0,086-0,297, p<0,001, I2=19,3%)77. Тем не менее, после корректировки на системную ошибку публикации, влияние ПНЖК на оценку симптомов не достигло значимых величин (SMD=0,118, 95% CI: -0,014– 0,250, p=0,08).В 16 РКТ, сообщающих о доменах симптомов СДВГ, наблюдались значительные преимущества как для гиперактивности/импульсивности (SMD=0,209, 95% CI: 0,059-0,358, p=0,006), так и для дефицита внимания (SMD=0,162, 95% CI: 0,047-0,276, p=0,006)77. Анализ подгрупп показал, что значительные преимущества от ПНЖК наблюдались только на оцененных родителями показателях, без влияния на оценки общей симптоматики, гиперактивности/импульсивности или невнимательности от учителей/клиницистов77. Последующий анализ с использованием более строгих критериев учета РКТ (и исключая данные из исследований с менее чем 50 участниками), не выявил преимуществ добавления ПНЖК на оцененные учителями симптомы СДВГ (N=287, n=3, SMD=0,08, 95% CI: -0,32-0,47, p=0,56, I2=0%), а положительный эффект на родительскую оценку также не достиг статистической значимости (N=411, n=4, SMD=0,32, 95% CI: -0,15– 0,8, p=0,098, I2=52,4%).
Омега-3 добавки (120-2513 мг/сут; в среднем: 616 мг/сут) снижали общую оценку симптомов СДВГ значительно больше, чем плацебо (N=1,408, n=16, SMD=0,26, 95% CI: 0,15-0,37, p<0,001, I2=25%)79. Несмотря на статистически значимый характер, величина пользы была незначительной при применении анализа триммирования и заполнения для корректировки на погрешность публикации (SMD=0,16, 95% CI: 0,03-0,28). Аналогичные малые эффекты наблюдались для обеих областей симптомов гиперактивности-импульсивности (SMD=0,26, 95% CI: 0,13-0,39, p<0,001) и дефицита внимания (SMD=0,22, 95% CI: 0,1-0,34, p<0,001). Последующие анализы (хотя и включающие меньшее количество испытаний) повторили эти выводы о небольших, но значительных эффектах добавок омега-3 на суммарные баллы, гиперактивность-импульсивность и симптомы нарушений внимания80.
Что касается поведенческих сопутствующих заболеваний, то не было никаких признаков влияния омега-3 на эмоциональную лабильность, проблемы с поведением или агрессию у молодых людей с СДВГ. Только влияние на оппозиционное поведение по оценке родителей достигло значимости в первичном анализе (SMD=0,2, 95% CI: 0,03-0,38, p=0,02, I2=0,2%). Тенденция к положительному влиянию на оппозиционное поведение по оценке родителей наблюдалась также при применении строгих критериев учета (SMD=0,15, 95% CI: -0,006-0,31, p=0,06, I2=8%), а также при рассмотрении только высококачественных исследований (SMD=0,2, 95% CI: 0,03-0,38, p=0,02, I2=0,2%).
Что касается когнитивной дисфункции, то единственные положительные эффекты омега-3 у молодых людей с СДВГ наблюдались в индивидуальных оценках заданий по количеству пропусков (N=214, n=3, SMD=1,09, 95% CI: 0,43-1,75, p=0,001, I2=75%) и ошибкам в поручениях (N=85, n=2, SMD=2,14, 95% CI: 1,24-3,03, p<0,001, I2=63%)81. Положительная динамика была выявлена для суммарных баллов рабочей памяти (N=506, n=3, SMD=0,23, 95% CI: -0,001-0,46, p=0,05, I2=33,9%)82 и индивидуальных баллов заданий отсроченного воспроизведения (N=224, n=2, SMD=0,37, 95% CI: от -0,05 до 0,79, p=0,08, I2=55%).
Омега-3 не давал никаких преимуществ в задачах на оперативную память (N=224, n=2, SMD=0,06, 95% CI: -0.21– 0.34, p=0,66, I2=0%) и обработку информации (N=309, n=4, SMD=0,46, 95% CI: -0,29 – 1,21, p=0.23, I2=89%)81, и не приводил к каким-либо улучшениям в суммарных когнитивных оценках для общего IQ (N=247, n=3, SMD=0,05, 95% CI: -0,21 – 0,32, р=0,71, I2=0%), ингибировании (n=274, N=5, SMD=-0,12, 95% CI: -0,44– 0,2, р=0,47, i2=42,8%), внимании (N=267, n=5, SMD=-0,12, 95% CI: -0,33– 0,1, p=0,28, I2=0%), кратковременной памяти (N=567, n=4, SMD=0,03, 95% CI: -0,10– 0,16, p=0,64, I2=0%), чтении (N=622, n=4, SMD=0,01, 95% CI: -0,09– 0,12, p=0,79, I2=0%), правописании (N=260, N=3, SMD=0,03, 95% CI: -0,34– 0,40, p=0,89, I2=48,9%), или времени реакции (N=260, N=5, SMD=0,09, 95% CI: -0,13– 0,3, P=0,44, I2=0%)82.
Аминокислоты
N-ацетилцистеинN-ацетилцистеин является нутрицевтической формой аминокислоты цистеина, которая в изобилии содержится в высокобелковых продуктах, и действует как предшественник глутатиона, который обладает антиоксидантной активностью во всем организме.
Это была наиболее часто оцениваемая аминокислотная добавка при психических расстройствах. В смешанной выборке из 574 человек с высоким уровнем депрессии (коморбидной или первичной) адъювантное лечение N-ацетилцистеином (2-3 г/сут) достоверно снижало депрессивные симптомы (n=5, SMD=0,37, 95% CI: 0,19-0,55, p=0,001, I2=92,64%), но не оказывало влияния на воспринимаемое качество жизни (N=543, n=4, SMD=0,14, 95% CI: -0,04-0,32, p=0,14, I2=68%)72. Между исследованиями наблюдалась высокая неоднородность, но не было никаких доказательств системной ошибки публикаций.
У людей с расстройствами настроения (включая биполярное расстройство и БДР; N=493, n=3) N-ацетилцистеин в дозе 2-3 г/сут оказывал небольшое, но значительное влияние по сравнению с плацебо на общее функционирование (SMD=0,19, 95% CI: 0,01-0,39, p=0,04, I2=64%) и социальное функционирование (SMD=0,22, 95% CI: 0,03-0,41, p=0,02, I2=67%). Он также значительно улучшил другие показатели функциональных нарушений (SMD=0,31, 95% CI: 0,12-0,50, p=0,002, I2=86%)72.
В трех РКТ у людей с шизофренией (N=247) дополнительное лечение N-ацетилцистеином значительно снижало общую оценку симптомов (Р=0,74, 95% CI: 0,06-1,43, р=0,03). Хотя включенные исследования были оценены как высококачественные, общая сила доказательств была слабой из-за высокого риска системной ошибки публикации и значительной неоднородности существующих данных (I2=84%)56. В отношении подгрупп симптомов отмечалась незначительная тенденция к благоприятному влиянию на негативные симптомы (SMD=0,59, 95% CI: -0,10-2,00, p=0,08, I2=93%), но не было эффектов, выходящих за рамки плацебо для позитивных симптомов (SMD=0,16, 95% CI: -0,29-0,62, p=0,48, I2=66%) или общей симптоматики (SMD=0,2, 95% CI: -0,21-0,62, p=0,34, I2=59%) 56.
В качестве адъювантного лечения для лиц с биполярным аффективным расстройством (N=224, n=2), 2 г/сут N-ацетилцистеин не отличался от плацебо в его влиянии на общую тяжесть заболевания (Clinical Global Impression– Severity, CGI-S: SMD=0,11, 95% CI: -0,15– 0,37, p=0,42, I2=90%, и Clinical Global Impression– Improvement, CGI-I: SMD=0,16, 95% CI: -0,09 до 0,42, p=0,22, I2=0%) или оценки мании (N=224, N=2, SMD=0,05, 95% CI: -0,2– 0,31, р=0,68, I2=0,01%)72. N-ацетилцистеин также оказался неэффективным при депрессивных симптомах у людей с биполярным расстройством (N=124, n=2, SMD=0,59, 95% CI: -0,3-1,48, p=0,19, I2=83%)56.
У 155 лиц с обсессивно-компульсивным расстройством, принимающих препараты (в основном СИОЗС), при добавлении к терапии 2-3 г/сутки N-ацетилцистеина выявлена тенденция в сторону уменьшения обсессивно-компульсивных симптомов (N=4, SMD=0,295, 95% CI: -0,018–0,608, р=0,064, I2=65%)74. N-ацетилцистеин (2-2,4 г/сут) также не оказывал существенного влияния на симптомы тревоги в объединенной смешанной выборке людей с психическими расстройствами (N=319, n=2, SMD=0,03, 95% CI: -0,21– 0,28, p=0,80, I2=0%) 72.
Во всех вышеперечисленных расстройствах частота возникновения и усугубления нежелательных эффектов от приема N-ацетилцистеина существенно не отличалась от плацебо56,72,74. Не было выявлено достоверной разницы в частоте легких нежелательных эффектов (особенно в отношении желудочно-кишечных симптомов) у людей с шизофренией (N=186, n=2, OR=1,56, 95% CI: 0,87-2,80, p=0,14, I2=0)56, но добавление N-ацетилцистеина ассоциировалось с более высокими показателями легких нежелательных явлений при расстройствах настроения (N=574, n=5, OR=1,61, 95% CI: 1,01-2,59, p=0,049) 72.
Модуляторы рецепторов N-метил-D-аспартата
Аминокислоты саркозин и глицин (которые встречаются в природе в мясе, молочных продуктах и бобовых) также были оценены как вспомогательные средства лечения шизофрении, благодаря их потенциальному действию в качестве модуляторов рецепторов N-метил-D-аспартата (NMDA)57. Ни саркозин (в дозе 2 г/сут), ни глицин (в дозе 2,8-60 г/сут) не оказывали никакого влияния на позитивные симптомы, хотя оба они значительно снижали общую психопатологию в качестве дополнения к антипсихотической терапии (саркозин: N=132, n=4, SMD=0,41, 95% CI: 0,06-0,76, p=0,02, I2 не сообщалось; глицин: N=159, n=6, SMD=0,66, 95% CI: 0,04-1,28, p=0,04, I2 не сообщалось)57.Влияние на негативные симптомы не достигало статистически значимого уровня (саркозин: N=132, n=4, SMD=0,32, 95% CI: -0,03-0,66, p=0,07; глицин: N=268, n=7, SMD=0,39, 95% CI: -0,11-0,9, p=0,13)57. Однако значительные преимущества для негативных симптомов наблюдались у лиц, получавших отличные от клозапина антипсихотики (саркозин: N=112, n=3, SMD=0,39, p=0,04; глицин: N=219, n=5, SMD=0,60, p=0,05; CI и I2 не представлены)57.
Как дополнение к лечению клозапином (N=58, n=3)58, глицин был неэффективен для позитивных (SMD=0,63, 95% CI: -0,21-1,48, I2 не сообщается), негативных (SMD=0,03, 95% CI: -0,51– 0,57, I2 не сообщается) и общих симптомов (SMD=0,32, 95% CI: -0,2– 0,84, I2 не сообщается). Не было получено достоверных данных о действии саркозина в качестве вспомогательного средства с клозапином.
Пребиотики и пробиотики
В нашем исследовании не было выявлено мета-анализов эффектов пребиотиков или пробиотиков на психические расстройства. Однако в группах лиц с легкой и умеренной депрессией (как определено по пороговым значениям на клинически валидированных шкалах), пробиотические препараты различных штаммов и доз снижали депрессивные симптомы значительно больше, чем плацебо (N=163, n=3, SMD=0,684, 95% CI: 0,0712-1,296, p=0,029)71.
ОБСУЖДЕНИЕ
Этот мета-обзор объединил и оценил все последние данные высшего уровня из мета-анализов РКТ, изучающих эффективность и безопасность пищевых добавок при психических расстройствах. Мы определили 33 подходящих мета-анализа, опубликованных с 2012 года (26 с 2016 года), с первичными анализами, включающими 10951 человека с психиатрическими состояниями (в частности, депрессивными расстройствами, тревожными и связанными со стрессом расстройствами, шизофренией, состояниями риска психоза, биполярным аффективным расстройством и СДВГ), рандомизированными либо к пищевым добавкам (включая омега-3 жирные кислоты, витамины, минералы, N-ацетилцистеин и другие аминокислоты), либо к группе плацебо-контроля. Хотя большинство оцененных пищевых добавок не значительно улучшили результаты психического здоровья вне условий контроля (см. диаграммы 2-7), некоторые из них действительно обеспечивали эффективное адъювантное лечение конкретных психических расстройств при определенных условиях.Самой большой доказательной силой обладает питательная добавка с омега-3, в частности ЭПК. Многочисленные мета-анализы показали, что она оказывает значительное влияние на людей с депрессией, в том числе высококачественные мета-анализы с хорошей уверенностью в результатах, определенных AMSTAR-264. Данные мета-анализов показали, что омега-3 эффективен при назначении в дополнение к антидепрессантам51,64. Как монотерапия, данные менее убедительны для омега-3, пока препараты, содержащие ДГК не приносят очевидной пользы при БДР51,64.
Омега-3 добавки, по-видимому, имеют наибольшую пользу при введении в виде формул с высоким содержанием ЭПК, поскольку значительные взаимосвязи между дозировкой ЭПК и размерами эффекта также наблюдаются в высококачественных мета-анализах РКТ59,64. Новые данные РКТ также указывают на то, что омега-3 может быть наиболее полезным для пациентов, имеющих повышенные маркеры воспаления. Имеющиеся мета-анализы показывают, что прием омега-3 не эффективен у пациентов с депрессией как сопутствующей патологией хронических физических состояний65, в том числе кардиометаболических заболеваний, что было воспроизведено в последующих исследованиях84. В свете нынешних данных, омега-3, кажется, представляют собой безопасный адъювантный метод лечения.
Необходимы дополнительные исследования, касающиеся эффективности омега-3 добавок при других состояниях психического здоровья. Например, омега-3 был показан как потенциально полезный для детей с СДВГ, опять же с высокими дозировками ЭПК, дающими наибольшие эффекты79. Однако незначительные размеры эффекта после коррекции по систематической ошибке публикации, наряду с низким качеством обзора, выявленным AMSTAR-2, снижают уверенность в выводах. Кроме того, в то время как существующие данные мета-анализов обнаружили отсутствие значительных преимуществ у людей с шизофренией55,59, последующие испытания у молодых людей с первым психотическим эпизодом сообщили о более положительных, хотя и смешанных результатах85,86, предположительно приписываемых нейропротекторным эффектам87,88.
Было обнаружено, что дополнительное лечение добавками на основе фолатов значительно уменьшает симптомы БДР и негативные симптомы при шизофрении54,67. Однако в обоих случаях рейтинги AMSTAR-2 указывали на низкую уверенность в результатах обзора, а положительные общие эффекты в этих мета-анализах были обусловлены в основном РКТ высокой дозы (15 мг/сут) метилфолата. Метилфолат легко всасывается, преодолевая любые генетические предрасположенности к мальабсорбции фолиевой кислоты и успешно преодолевая гематоэнцефалический барьер. Действительно, плацебо-контролируемое исследование метилфолата при шизофрении сообщило о значительном увеличении количества белого вещества в течение всего 12 недель, что сопровождалось уменьшением негативных симптомов.
РКТ, не охваченные в нашем мета-обзоре92 и ретроспективном анализе диаграмм93, показали преимущества добавления метилфолата при других психических расстройствах. Учитывая это, наряду с отсутствием побочных эффектов (на самом деле, значительно меньше побочных явлений в выборках, получающих лечение по сравнению с плацебо), необходимы дальнейшие исследования метилфолата в качестве вспомогательного лечения психических расстройств.
Что касается других витаминов (таких как витамины Е, С или D), минералов (цинк и магний) или инозитола, то в настоящее время нет убедительных доказательств, подтверждающих их эффективность при любом психическом расстройстве, хотя следует упомянуть о новых доказательствах, касающихся положительного воздействия добавок витамина D при тяжелой депрессии.
Помимо витаминов, минералов и омега-3 жирных кислот, некоторые аминокислоты в настоящее время появляются в качестве перспективных вспомогательных средств лечения психических расстройств. Хотя доказательства все еще находятся в стадии становления, N-ацетилцистеин в частности (в дозах 2000 мг/сут или выше) был показан как потенциально эффективный для уменьшения депрессивных симптомов и улучшения функционального восстановления в смешанных психиатрических выборках72. Кроме того, значительное снижение общих симптомов шизофрении наблюдалось при использовании N-ацетилцистеина в качестве вспомогательного лечения, хотя и с существенной гетерогенностью между исследованиями, особенно по продолжительности исследования (на самом деле, N-ацетилцистеин имеет очень замедленное начало действия около 6 месяцев56,94).
N-ацетилцистеин действует как предшественник глутатиона, основного эндогенного антиоксиданта, нейтрализующего клеточный реактивный кислород и азот95. Производство глутатиона в астроцитах ограничено цистеином. Пероральный глутатион и L-цистеин расщепляются метаболизмом первого прохода и не увеличивают уровни глутатиона мозга, в отличие от перорального N-ацетилцистеина, который легче усваивается и, как было показано, увеличивает глутатион мозга в животных моделях96. Кроме того, было показано, что N-ацетилцистеин увеличивает высвобождение дофамина у животных моделей96.
N-ацетилцистеин может помочь в лечении шизофрении, биполярного аффективного расстройства и депрессии за счет снижения окислительного стресса и уменьшения глутаматергической дисфункции96, но имеет более широкие доклинические эффекты на митохондрии, апоптоз, нейрогенез и удлинение теломер неопределенного клинического значения.
NMDA-рецепторы активируются путем связывания с D-серином или глицином97. Саркозин является естественным ингибитором транспорта глицина и может выступать в качестве ко-агониста NMDA98. Как таковые, D-cерин, глицин и саркозин могут улучшить психотические симптомы через модуляцию NMDA99. Мы обнаружили снижение общих психотических симптомов, но не негативных симптомов, при применении глицина и саркозина. Кроме того, мы обнаружили, что глицин не был эффективен в комбинации с клозапином. Это может быть связано с тем, что клозапин уже действует как агонист участка глицина NMDA-рецептора97.
Роль микробиома кишечника в психическом здоровье также является быстро развивающейся областью исследований. Микробиота кишечника значительно отличается между людьми с психическими расстройствами и здоровым контролем, и недавние исследования фекальной трансплантации с использованием мышей без микробов показывают, что эти различия могут играть причинную роль в симптомах психического расстройства41,100,101.
В настоящее время начинают появляться интервенционные исследования, направленные на изучение влияния пробиотических препаратов на клинические исходы при психических расстройствах71. Мы включили один недавний мета-анализ, который оценивал объединенное влияние пробиотических вмешательств на депрессивные симптомы: в то время как первичный анализ не сообщил о значительном эффекте, умеренно большой эффект в трех включенных исследованиях предполагает, что пробиотики могут быть полезны для тех, у кого есть клинический диагноз депрессии, а не субклинические симптомы71. Однако необходимы дополнительные исследования, чтобы воспроизвести эти результаты, оценить долгосрочную безопасность пробиотических вмешательств и выяснить оптимальный режим дозирования и наиболее эффективные пребиотические и пробиотические штаммы102.
В то время как этот мета-обзор выделил потенциальные роли для использования питательных добавок, это не должно быть предназначено для замены улучшения рациона питания. Плохое физическое здоровье людей с психическими заболеваниями хорошо документировано103, и чрезмерное и нездоровое потребление пищи, по-видимому, является ключевым фактором этого4,5. Улучшение качества питания связано с уменьшением смертности от всех причин104, в то время как мультивитаминные и мультиминеральные добавки не могут улучшить продолжительность жизни18-20.
Мета-анализ диетических вмешательств у людей с тяжелыми психическими заболеваниями выявил преимущества по ряду аспектов физического здоровья105. Маловероятно, что стандартная добавка питательных веществ сможет охватить все полезные аспекты улучшенного питания. Кроме того, цельные продукты могут содержать витамины и минералы в различных формах, в то время как питательные добавки могут обеспечивать только одну форму. Например, витамин Е встречается естественным образом в восьми формах, но питательные добавки могут обеспечить только одну форму. Диетические вмешательства также уменьшают избыток пищевых элементов, таких как соль, которая является ключевым фактором преждевременной смертности13.
В то время как улучшение рациона питания, по-видимому, играет четкую роль в увеличении продолжительности жизни и предотвращении хронических заболеваний, в настоящее время нет исследований, оценивающих это у людей с психическими расстройствами. Кроме того, хотя недавние мета-анализы РКТ показали, что улучшение питания уменьшает симптомы депрессии в общей популяции106, необходимы более тщательно разработанные исследования для подтверждения преимуществ диетических вмешательств для людей с диагностированными психическими состояниями25.
Наши данные следует рассматривать в свете некоторых ограничений. Во-первых, хотя мета-анализы РКТ, как правило, представляют собой верхний уровень доказательств, важно признать, что многие из результатов, включенных в этот мета-обзор, имели значительную степень неоднородности между включенными исследованиями или были основаны на небольшом числе исследований. Следующим шагом в этой области исследований является переход от мета-анализа на уровне исследования к мета-анализу на уровне пациента, поскольку это позволит получить более персонализированную картину эффектов пищевых добавок, полученных в результате адекватного анализа модераторов, медиаторов и подгрупп. Кроме того, было бы желательно сравнить питательные добавки в одном и том же исследовании.
Признано, что люди с психическими расстройствами обычно принимают пищевые добавки в комбинации.
некоторых случаях, исследование поддерживало этот подход, наиболее обыкновенно в форме мультивитаминного/ минерального комплексов107. Однако недавние исследования в области депрессии показали, что ”больше не обязательно лучше», когда дело доходит до сложных формул108. Следует отметить, что недавние крупные клинические исследования пациентов с расстройствами настроения показали, что комбинации питательных веществ могут не иметь более мощный эффект, и в некоторых случаях плацебо было более эффективным47,108,109.
В заключении, в настоящее время существует огромное количество исследований, изучающих эффективность пищевых добавок у людей с психическими расстройствами, причем некоторые питательные вещества в настоящее время продемонстрировали эффективность в конкретных условиях, а другие – все более выраженный потенциал. Существует большая потребность в определении задействованных механизмов наряду с изучением последствий в конкретных группах населения, таких как молодежь и лица, находящиеся на ранних стадиях заболевания. Четко обоснован целевой подход, который может проявляться как направленное на биомаркеры лечение, основанное на ключевых уровнях питательных веществ, маркерах воспаления и фармакогеномике83,91,110.
Благодарности
J. Firth получает поддержку от Blackmores Institute Fellowship; J. Sarris от National Health and Medical Research Council (NHMRC) Clinical Research Fellowship (APP1125000); M. Berk от NHMRC Senior Principal Research Fellowship (APP1059660 and APP1156072). B. Stubbs читает клинические лекции при поддержке Health Education England and the National Institute for Health Research (NIHR) Integrated Clinical Academy Programme (ICA-CL-2017-03-001); K. Allott получает поддержку от Career Development Fellowship from the NHMRC (APP1141207); D. Siskind частично поддерживается Early Career Fellowship from the NHMRC (APP1111136); W. Marx поддерживается Deakin University postdoctoral fellowship. Мнения, выраженные в настоящем документе, принадлежат авторам, и могут не совпадать с мнением вышеупомянутых организаций.
DOI:10.1002/wps.20672
Список исп. литературыСкрыть список1. Firth J, Stubbs B, Teasdale SB et al. Diet as a hot topic in psychiatry: a population-scale study of nutritional intake and inflammatory potential in severe mental illness. World Psychiatry 2018;17:365-7.
2. Teasdale SB, Ward PB, Samaras K et al. Dietary intake of people with severe mental illness: systematic review and meta-analysis. Br J Psychiatry 2019; 214:251-9.
3. van den Berk-Clark C, Secrest S, Walls J et al. Association between posttraumatic stress disorder and lack of exercise, poor diet, obesity, and co-occuring smoking: a systematic review and meta-analysis. Health Psychol 2018;37:407-16.
4. Woo H, Kim D, Hong Y-S et al. Dietary patterns in children with attention deficit/hyperactivity disorder (ADHD). Nutrients 2014;6:1539-53.
5. Howard AL, Robinson M, Smith GJ et al. ADHD is associated with a “Western” dietary pattern in adolescents. J Atten Disord 2011;15:
403-11.
6. Jacka FN, Cherbuin N, Anstey KJ et al. Does reverse causality explain the relationship between diet and depression? J Affect Disord 2015;175:248-50.
7. Salvi V, Mencacci C, Barone-Adesi F. H1-histamine receptor affinity predicts weight gain with antidepressants. Eur Neuropsychopharmacol 2016; 26:1673-7.
8. Firth J, Teasdale SB, Jackson SE et al. Do reductions in ghrelin contribute towards antipsychotic-induced weight gain? Schizophr Res (in press).
9. Tolkien K, Bradburn S, Murgatroyd C. An anti-inflammatory diet as a potential intervention for depressive disorders: a systematic review and meta-analysis. Clin Nutr (in press).
10. Lassale C, Batty GD, Baghdadli A et al. Healthy dietary indices and risk of depressive outcomes: a systematic review and meta-analysis of observational studies. Mol Psychiatry 2019;24:965-86.
11. Firth J, Carney R, Stubbs B et al. Nutritional deficiencies and clinical correlates in first-episode psychosis: a systematic review and meta-analysis. Schizophr Bull 2018;44:1275-92.
12. Swinburn BA, Kraak VI, Allender S et al. The global syndemic of obesity, undernutrition, and climate change: the Lancet Commission report. Lancet 2019;393:791-846.
13. GBD 2017 Diet Collaborators. Health effects of dietary risks in 195 countries, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019;393:1958-72.
14. Sarris J, Logan AC, Akbaraly TN et al. Nutritional medicine as mainstream in psychiatry. Lancet Psychiatry 2015;2:271-4.World Psychiatry 18:3– October 2019 323
15. Sarris J, Logan AC, Akbaraly TN et al. International Society for Nutritional Psychiatry Research consensus position statement: nutritional medicine in modern psychiatry. World Psychiatry 2015;14:370-1.
16. Fernstrom JD. Can nutrient supplements modify brain function? Am J Clin Nutr 2000;71:1669S-73S.
17. Kantor ED, Rehm CD, Du M et al. Trends in dietary supplement use among US adults from 1999-2012. JAMA 2016;316:1464-74.
18. Wactawski-Wende J, Kotchen JM, Anderson GL et al. Calcium plus vitamin D supplementation and the risk of colorectal cancer. N Engl J Med 2006; 354:684-96.
19. Jenkins DJ, Spence JD, Giovannucci EL et al. Supplemental vitamins and minerals for CVD prevention and treatment. J Am Coll Cardiol 2018;71: 2570-84.
20. Lonn E, Bosch J, Yusuf S et al. Effects of long-term vitamin E supplementation on cardiovascular events and cancer: a randomized controlled trial. JAMA 2005;293:1338-47.
21. Pitkin RM. Folate and neural tube defects. Am J Clin Nutr 2007;85:285S-8S.
22. Lederle FA. Oral cobalamin for pernicious anemia: medicine’s best kept secret? JAMA 1991;265: 94-5.
23. Ala A, Walker AP, Ashkan K et al. Wilson’s disease. Lancet 2007;369:397- 408.
24. Siscovick DS, Barringer TA, Fretts AM et al. Omega-3 polyunsaturated fatty acid (fish oil) supplementation and the prevention of clinical cardiovascular disease: a science advisory from the American Heart Association. Circulation 2017;135:e867-84.
25. Berk M, Jacka FN. Diet and depression – from confirmation to implementation. JAMA 2019;321:842-3.
26. Berk M, Williams LJ, Jacka FN et al. So depression is an inflammatory disease, but where does the inflammation come from? BMC Med 2013;11:200.
27. Miller BJ, Buckley P, Seabolt W et al. Meta-analysis of cytokine alterations in schizophrenia: clinical status and antipsychotic effects. Biol Psychiatry 2011;70:663-71.
28. Berk M, Kapczinski F, Andreazza A et al. Pathways underlying neuroprogression in bipolar disorder: focus on inflammation, oxidative stress and neurotrophic factors. Neurosci Biobehav Rev 2011;35:
804-17.
29. Irwin MR, Piber D. Insomnia and inflammation: a two hit model of depression risk and prevention. World Psychiatry 2018;17:359-61.
30. Köhler CA, Freitas TH, Stubbs B et al. Peripheral alterations in cytokine and chemokine levels after antidepressant drug treatment for major depressive disorder: systematic review and meta-analysis. Mol Neurobiol 2018;55:4195-4206.
31. Schuch FB, Deslandes AC, Stubbs B et al. Neurobiological effects of exercise on major depressive disorder: a systematic review. Neurosci Biobehav Rev 2016;61:1-11.
32. Dodd S, Dean O, Copolov DL et al. N-acetylcysteine for antioxidant therapy: pharmacology and clinical utility. Expert Opin Biol Ther 2008;8:1955-62.
33. Simopoulos AP. Omega-3 fatty acids in inflammation and autoimmune diseases. J Am Coll Nutr 2002;21:495-505.
34. Swardfager W, Herrmann N, Mazereeuw G et al. Zinc in depression: a meta-analysis. Biol Psychiatry 2013;74:872-8.
35. Joe P, Petrilli M, Malaspina D et al. Zinc in schizophrenia: a meta-analysis. Gen Hosp Psychiatry 2018;53:19-24.
36. Gilbody S, Lightfoot T, Sheldon T. Is low folate a risk factor for depression? A meta-analysis and exploration of heterogeneity. J Epidemiol Commun Health 2007;61:631-7.
37. Belbasis L, Kohler CA, Stefanis N et al. Risk factors and peripheral biomarkers for schizophrenia spectrum disorders: an umbrella review of meta-analyses. Acta Psychiatr Scand 2018;137:88-97.
38. Anglin RES, Samaan Z, Walter SD et al. Vitamin D deficiency and depression in adults: systematic review and meta-analysis. Br J Psychiatry 2013;202:100-7.
39. Murri MB, Respino M, Masotti M et al. Vitamin D and psychosis: mini meta-analysis. Schizophr Res 2013;150:235-9.
40. Lally J, Ajnakina O, Singh N et al. Vitamin D and clinical symptoms in first episode psychosis (FEP): a prospective cohort study. Schizophr Res 2019;204:381-8.
41. Zheng P, Zeng B, Liu M et al. The gut microbiome from patients with schizophrenia modulates the glutamate-glutamine-GABA cycle and schizophrenia-relevant behaviors in mice. Sci Adv 2019;5:eaau8317.
42. Valles-Colomer M, Falony G, Darzi Y et al. The neuroactive potential of the human gut microbiota in quality of life and depression. Nat Microbiol 2019;4:623-32.
43. Biesalski HK. Nutrition meets the microbiome: micronutrients and the microbiota. Ann NY Acad Sci 2016;1372:53-64.
44. Delzenne NM, Neyrinck AM, Bäckhed F et al. Targeting gut microbiota in obesity: effects of prebiotics and probiotics. Nat Rev Endocrinol 2011;7:639.
45. Dash S, Clarke G, Berk M et al. The gut microbiome and diet in psychiatry: focus on depression. Curr Opin Psychiatry 2015;28:1-6.
46. Kaplan BJ, Rucklidge JJ, Romijn A et al. The emerging field of nutritional mental health: inflammation, the microbiome, oxidative stress, and mitochondrial function. Clin Psychol Sci 2015;3:964-80.
47. Bot M, Brouwer IA, Roca M et al. Effect of multinutrient supplementation and food-related behavioral activation therapy on prevention of major depressive disorder among overweight or obese adults with subsyndromal depressive symptoms: the MooDFOOD randomized clinical trial. JAMA 2019;321:858-68.
48. Freedman R, Hunter SK, Hoffman MC. Prenatal primary prevention of mental illness by micronutrient supplements in pregnancy. Am J Psychiatry 2018;175:607-19.
49. Moher D, Liberati A, Tetzlaff J et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 2009; 6:e1000097.
50. Shea BJ, Reeves BC, Wells G et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ 2017;358:j4008.
51. Hallahan B, Ryan T, Hibbeln JR et al. Efficacy of omega-3 highly unsaturated fatty acids in the treatment of depression. Br J Psychiatry 2016;209:192- 201.
52. Bergman H, Walker DM, Nikolakopoulou A et al. Systematic review of interventions for treating or preventing antipsychotic-induced tardive dyskinesia. Health Technol Assess 2017;21:1-218.
53. Firth J, Stubbs B, Sarris J et al. The effects of vitamin and mineral supplementation on symptoms of schizophrenia: a systematic review and meta-analysis. Psychol Med 2017;47:1515-27.
54. Sakuma K, Matsunaga S, Nomura I et al. Folic acid/methylfolate for the treatment of psychopathology in schizophrenia: a systematic review and meta-analysis. Psychopharmacology 2018:235:2303-14.
55. Fusar-Poli P, Berger G. Eicosapentaenoic acid interventions in schizophrenia: meta-analysis of randomized, placebo-controlled studies. J Clin Psychopharmacol 2012;32:179-85.
56. Zheng W, Zhang QE, Cai DB et al. N-acetylcysteine for major mental disorders: a systematic review and meta-analysis of randomized controlled trials. Acta Psychiatr Scand 2018;137:391-400.
57. Singh SP, Singh V. Meta-analysis of the efficacy of adjunctive NMDA receptor modulators in chronic schizophrenia. CNS Drugs 2011;25:859- 85.
58. Siskind DJ, Lee M, Ravindran A et al. Augmentation strategies for clozapine refractory schizophrenia: a systematic review and meta-analysis. Aust N Z J Psychiatry 2018;52:751-67.
59. Grosso G, Pajak A, Marventano S et al. Role of omega-3 fatty acids in the treatment of depressive disorders: a comprehensive meta-analysis of randomized clinical trials. PLoS One 2014;9:e96905.
60. Davies C, Cipriani A, Ioannidis JPA et al. Lack of evidence to favor specific preventive interventions in psychosis: a network meta-analysis. World Psychiatry 2018;17:196-209.
61. Devoe DJ, Farris MS, Townes P et al. Attenuated psychotic symptom interventions in youth at risk of psychosis: a systematic review and meta-analysis. Early Interv Psychiatry 2019;13:3-17.
62. Devoe DJ, Peterson A, Addington J. Negative symptom interventions in youth at risk of psychosis: a systematic review and network meta-analysis. Schizophr Bull 2018;44:807-23.
63. Devoe DJ, Farris MS, Townes P et al. Interventions and social functioning in youth at risk of psychosis: a systematic review and meta-analysis. Early Interv Psychiatry 2019;13:169-80.
64. Mocking RJ, Harmsen I, Assies J et al. Meta-analysis and meta-regression of omega-3 polyunsaturated fatty acid supplementation for major depressive disorder. Transl Psychiatry 2016;6:e756.
65. Schefft C, Kilarski LL, Bschor T et al. Efficacy of adding nutritional supplements in unipolar depression: a systematic review and meta-analysis. Eur Neuropsychopharmacol 2017;27:1090-109.
66. Bae JH, Kim G. Systematic review and meta-analysis of omega-3-fatty acids in elderly patients with depression. Nutr Res 2018;50:1-9.
67. Roberts E, Carter B, Young AH. Caveat emptor: folate in unipolar depressive illness, a systematic review and meta-analysis. J Psychopharmacol 2018;32:377-84.
68. Mukai T, Kishi T, Matsuda Y et al. A meta-analysis of inositol for depressionand anxiety disorders. Hum Psychopharmacol 2014;29:55-63
69. Vellekkatt F, Menon V. Efficacy of vitamin D supplementation in major depression: a meta-analysis of randomized controlled trials. J Postgrad Med 2019;65:74-80.
70. Phelan D, Molero P, Martinez-Gonzalez MA et al. Magnesium and mood disorders: systematic review and meta-analysis. BJPsych Open 2018;4:167- 79.
71. Ng QX, Peters C, Ho CYX et al. A meta-analysis of the use of probiotics to alleviate depressive symptoms. J Affect Disord 2018;228:13-9.
72. Fernandes BS, Dean OM, Dodd S et al. N-acetylcysteine in depressive symptoms and functionality: a systematic review and meta-analysis. J Clin Psychiatry 2016;77:e457-e66.
73. Sarris J, Murphy J, Mischoulon D et al. Adjunctive nutraceuticals for depression: a systematic review and meta-analyses. Am J Psychiatry 2016;173:575- 87.
74. Couto JP, Moreira R. Oral N-acetylcysteine in the treatment of obsessive-compulsive disorder: a systematic review of the clinical evidence. Prog Neuropsychopharmacol Biol Psychiatry 2018;86:245-54.
75. Sarris J, Mischoulon D, Schweitzer I. Omega-3 for bipolar disorder: meta-analyses of use in mania and bipolar depression. J Clin Psychiatry 2012; 73:81-6.
76. Rosenblat JD, Kakar R, Berk M et al. Anti-inflammatory agents in the treatment of bipolar depression: a systematic review and meta-analysis. Bipolar Disord 2016;18:89-101.
77. Puri BK, Martins JG. Which polyunsaturated fatty acids are active in children with attention-deficit hyperactivity disorder receiving PUFA supplementation? A fatty acid validated meta-regression analysis of randomized controlled trials. Prostaglandins Leukot Essent Fatty Acids 2014;90:179-89.
78. Goode AP, Coeytaux RR, Maslow GR et al. Nonpharmacologic treatments for attention-deficit/hyperactivity disorder: a systematic review. Pediatrics 2018;141:e20180094.
79. Hawkey E, Nigg JT. Omega-3 fatty acid and ADHD: blood level analysis and meta-analytic extension of supplementation trials. Clin Psychol Rev 2014;34:496-505.
80. Cooper RE, Tye C, Kuntsi J et al. The effect of omega-3 polyunsaturated fatty acid supplementation on emotional dysregulation, oppositional behaviour and conduct problems in ADHD: a systematic review and meta-analysis. J Affect Disord 2016;190:474-82.
81. Chang JPC, Su KP, Mondelli V et al. Omega-3 polyunsaturated fatty acids in youths with attention deficit hyperactivity disorder: a systematic review and meta-analysis of clinical trials and biological studies. Neuropsychopharmacology 2018;43:534-45.
82. Cooper RE, Tye C, Kuntsi J et al. Omega-3 polyunsaturated fatty acid supplementation and cognition: a systematic review and meta-analysis. J Psychopharmacol 2015;29:753-63.
83. Rapaport MH, Nierenberg AA, Schettler PJ et al. Inflammation as a predictive biomarker for response to omega-3 fatty acids in major depressive disorder: a proof-of-concept study. Mol Psychiatry 2016;21:71-9.
84. Jiang W, Whellan DJ, Adams KF et al. Long-chain omega-3 fatty acid supplements in depressed heart failure patients: results of the OCEAN trial. JACC Heart Fail 2018;6:833-43.
85. Pawełczyk T, Grancow-Grabka M, Kotlicka-Antczak M et al. A randomized controlled study of the efficacy of six-month supplementation with concentrated fish oil rich in omega-3 polyunsaturated fatty acids in first episode schizophrenia. J Psychiatr Res 2016;73:34-44.
86. Robinson DG, Gallego JA, John M et al. A potential role for adjunctive omega-3 polyunsaturated fatty acids for depression and anxiety symptoms in recent onset psychosis: results from a 16 week randomized placebo-controlled trial for participants concurrently treated with risperidone. Schizophr Res 2019;204:295-303.
87. Pawełczyk T, Piatkowska-Janko E, Bogorodzki P et al. Omega-3 fatty acid supplementation may prevent loss of gray matter thickness in the left parieto-occipital cortex in first episode schizophrenia: a secondary outcome analysis of the OFFER randomized controlled study. Schizophr Res 2018;195:168-75.
88. Firth J, Rosenbaum S, Ward PB et al. Adjunctive nutrients in first-episode psychosis: a systematic review of efficacy, tolerability and neurobiological mechanisms. Early Interv Psychiatry 2018;12:774-83.
89. Farah A. The role of L-methylfolate in depressive disorders. CNS Spectr 2009;14:2-7.
90. Fava M, Mischoulon D. Folate in depression: efficacy, safety, differences in formulations, and clinical issues. J Clin Psychiatry 2009;70:12-7.
91. Roffman JL, Petruzzi LJ, Tanner AS et al. Biochemical, physiological and clinical effects of l-methylfolate in schizophrenia: a randomized controlled trial. Mol Psychiatry 2018;23:316-22.
92. Kakar MS, Jehangir S, Mustafa M et al. Therapeutic efficacy of combination therapy of l-methylfolate and escitalopram in depression. Pak Armed Forces Med J 2017;67:976-81.
93. Rainka M, Aladeen T, Westphal E et al. L-methylfolate calcium in adolescents and children: a retrospective analysis. Presented at the Annual Meeting of the American Academy of Neurology, Los Angeles, April 2018.
94. Breier A, Liffick E, Hummer TA et al. Effects of 12-month, double-blind N-acetyl cysteine on symptoms, cognition and brain morphology in early phase schizophrenia spectrum disorders. Schizophr Res 2018;199:395- 402.
95. Yolland CO, Phillipou A, Castle DJ et al. Improvement of cognitive function in schizophrenia with N-acetylcysteine: a theoretical review. Nutr Neurosci (in press).
96. Dean O, Giorlando F, Berk M. N-acetylcysteine in psychiatry: current therapeutic evidence and potential mechanisms of action. J Psychiatry Neurosci 2011;36:78-86.
97. Moghaddam B, Javitt DJN. From revolution to evolution: the glutamate hypothesis of schizophrenia and its implication for treatment. Neuropsychopharmacology 2012;37:4-15.
98. Zhang HX, Hyrc K, Thio LL. The glycine transport inhibitor sarcosine is an NMDA receptor co-agonist that differs from glycine. J Physiol 2009;587: 3207-20.
99. Slyepchenko A, Maes M, Jacka FN et al. Gut microbiota, bacterial translocation, and interactions with diet: pathophysiological links between major depressive disorder and non-communicable medical comorbidities. Psychother Psychosom 2017;86:31-46.
100. Zheng P, Zeng B, Zhou C et al. Gut microbiome remodeling induces depressive-like behaviors through a pathway mediated by the host’s metabolism. Mol Psychiatry 2016;21:786-96.
101. Cheung SG, Goldenthal AR, Uhlemann A-C et al. Systematic review of gut microbiota and major depression. Front Psychiatry 2019;10:34.
102. Kao A, Safarikova J, Marquardt T et al. Pro-cognitive effect of a prebiotic in psychosis: a double blind placebo controlled cross-over study. Schizophr Res 2019;208:460-1.
103. Liu NH, Daumit GL, Dua T et al. Excess of mortality in person with severe mental disorders: a multilevel intervention framework and priorities for clinical practice, policy and research agendas. World Psychiatry 2017;16:30-40.
104. Reedy J, Krebs-Smith SM, Miller PE et al. Higher diet quality is associated with decreased risk of all-cause, cardiovascular disease, and cancer mortality among older adults. J Nutr 2014;144:881-9.
105. Teasdale SB, Ward PB, Rosenbaum S et al. Solving a weighty problem: systematic review and meta-analysis of nutrition interventions in severe mental illness. Br J Psychiatry 2017;210:110-8.
106. Firth J, Marx W, Dash S et al. The effects of dietary improvement on symptoms of depression and anxiety: a meta-analysis of randomized controlled trials. Psychosom Med 2019;8:265-80.
107. Rucklidge JJ, Kaplan BJ. Broad-spectrum micronutrient treatment for attention-deficit/hyperactivity disorder: rationale and evidence to date. CNS Drugs 2014;28:775-85.
108. Sarris J, Byrne GJ, Stough C et al. Nutraceuticals for major depressive disorder – more is not merrier: an 8-week double-blind, randomised, controlled trial. J Affect Disord 2019;245:1007-15.
109. Berk M, Turner A, Malhi GS et al. A randomised controlled trial of a mitochondrial therapeutic target for bipolar depression: mitochondrial agents, N-acetylcysteine, and placebo. BMC Med 2019;17:18.
110. Shelton RC, Pencina MJ, Barrentine LW et al. Association of obesity and inflammatory marker levels on treatment outcome: results from a double-blind, randomized study of adjunctive L-methylfolate calcium in patients with MDD who are inadequate responders to SSRIs. J Clin Psychiatry 2015;76:1635-41.
