Психиатрия Всемирная психиатрия
Психиатрия Всемирная психиатрия
№01 2018
Измерение и улучшение качества оказания помощи в области психического здоровья: глобальная перспектива №01 2018
Номера страниц в выпуске:30-38
Перевод: Мурашко А.А. (Москва), Шишкина О.А. (Москва)
Редактура: к.м.н. Федотов И.А. (Рязань)
Психические расстройства по всему миру схожи, однако качество медицинской помощи в области этих расстройств не улучшается, так же как не улучшается и качество оказания медицинской помощи при соматических заболеваниях. В данном исследовании мы показали условия продвижения количественных измерений как инструмента улучшения качества помощи в области психических расстройств. Мы выделили ключевые барьеры, включая недостаток стандартизированной информации по данным ресурсам, основанным на информационных технологиях, ограниченность научной доказательности для измерения качества оказания психиатрической помощи, недостаток доступности образования и поддержки, а также культуральные барьеры при интеграции психиатрической помощи в общемедицинскую сеть. Мы описываем несколько инноваций, которые внедряются по всему миру и могут уменьшить эти барьеры. Основываясь на этом опыте, мы предлагаем несколько рекомендаций для улучшения качества психиатрической помощи. Для получателей и организаторов в области психического здоровья важно иметь портфолио, включающее валидизированные методы измерения исходов в пределах спектров различных состояний. Необходимо внедрить в существующую электронную базу элементы общих данных. Исходы психических расстройств требуют регулярной оценки, и именно помощь, основанная на измерении, должна стать частью всей культуры и системы оказания медицинской помощи. Система оказания медицинской помощи требует валидизированного способа качественных измерений для выявления наиболее уязвимых групп населения, требующих медицинской помощи и анализа недочетов. Еще больше внимания должно быть уделено обучению сотрудников в направлении увеличения объема и качества медицинской помощи. Область улучшения качества психиатрической помощи является командным делом, требующим координации между различными сферами, включающими защиту прав пациентов, а также увеличение ресурсов и оплаты от получателя помощи и системы здравоохранения.
Ключевые слова: психические расстройства, качество помощи, измерения качества, информированность о здоровье, электронные записи о здоровье, пациент-ориентированные исходы, системы оказания медицинской помощи, стратегия здоровья.
Редактура: к.м.н. Федотов И.А. (Рязань)
Психические расстройства по всему миру схожи, однако качество медицинской помощи в области этих расстройств не улучшается, так же как не улучшается и качество оказания медицинской помощи при соматических заболеваниях. В данном исследовании мы показали условия продвижения количественных измерений как инструмента улучшения качества помощи в области психических расстройств. Мы выделили ключевые барьеры, включая недостаток стандартизированной информации по данным ресурсам, основанным на информационных технологиях, ограниченность научной доказательности для измерения качества оказания психиатрической помощи, недостаток доступности образования и поддержки, а также культуральные барьеры при интеграции психиатрической помощи в общемедицинскую сеть. Мы описываем несколько инноваций, которые внедряются по всему миру и могут уменьшить эти барьеры. Основываясь на этом опыте, мы предлагаем несколько рекомендаций для улучшения качества психиатрической помощи. Для получателей и организаторов в области психического здоровья важно иметь портфолио, включающее валидизированные методы измерения исходов в пределах спектров различных состояний. Необходимо внедрить в существующую электронную базу элементы общих данных. Исходы психических расстройств требуют регулярной оценки, и именно помощь, основанная на измерении, должна стать частью всей культуры и системы оказания медицинской помощи. Система оказания медицинской помощи требует валидизированного способа качественных измерений для выявления наиболее уязвимых групп населения, требующих медицинской помощи и анализа недочетов. Еще больше внимания должно быть уделено обучению сотрудников в направлении увеличения объема и качества медицинской помощи. Область улучшения качества психиатрической помощи является командным делом, требующим координации между различными сферами, включающими защиту прав пациентов, а также увеличение ресурсов и оплаты от получателя помощи и системы здравоохранения.
Ключевые слова: психические расстройства, качество помощи, измерения качества, информированность о здоровье, электронные записи о здоровье, пациент-ориентированные исходы, системы оказания медицинской помощи, стратегия здоровья.
Перевод: Мурашко А.А. (Москва), Шишкина О.А. (Москва)
Редактура: к.м.н. Федотов И.А. (Рязань)
Психические расстройства по всему миру схожи, однако качество медицинской помощи в области этих расстройств не улучшается, так же как не улучшается и качество оказания медицинской помощи при соматических заболеваниях. В данном исследовании мы показали условия продвижения количественных измерений как инструмента улучшения качества помощи в области психических расстройств. Мы выделили ключевые барьеры, включая недостаток стандартизированной информации по данным ресурсам, основанным на информационных технологиях, ограниченность научной доказательности для измерения качества оказания психиатрической помощи, недостаток доступности образования и поддержки, а также культуральные барьеры при интеграции психиатрической помощи в общемедицинскую сеть. Мы описываем несколько инноваций, которые внедряются по всему миру и могут уменьшить эти барьеры. Основываясь на этом опыте, мы предлагаем несколько рекомендаций для улучшения качества психиатрической помощи. Для получателей и организаторов в области психического здоровья важно иметь портфолио, включающее валидизированные методы измерения исходов в пределах спектров различных состояний. Необходимо внедрить в существующую электронную базу элементы общих данных. Исходы психических расстройств требуют регулярной оценки, и именно помощь, основанная на измерении, должна стать частью всей культуры и системы оказания медицинской помощи. Система оказания медицинской помощи требует валидизированного способа качественных измерений для выявления наиболее уязвимых групп населения, требующих медицинской помощи и анализа недочетов. Еще больше внимания должно быть уделено обучению сотрудников в направлении увеличения объема и качества медицинской помощи. Область улучшения качества психиатрической помощи является командным делом, требующим координации между различными сферами, включающими защиту прав пациентов, а также увеличение ресурсов и оплаты от получателя помощи и системы здравоохранения.
Ключевые слова: психические расстройства, качество помощи, измерения качества, информированность о здоровье, электронные записи о здоровье, пациент-ориентированные исходы, системы оказания медицинской помощи, стратегия здоровья.
(World Psychiatry 2018;17:30–38)
Психические расстройства во всем мире являются причиной 32% лет нетрудоспособности и 13% лет адаптации к нетрудоспособности в скорректированном сроке жизни1. Более того, лица с этими расстройствами выявляют повышенные уровни смертности от распространенных медицинских состояний2-4. Среди лиц с психическими расстройствами различия в качестве и исходах оказания медицинской помощи более явно выражены для расовых/этнических меньшинств6-8 и у представителей групп низкого социально-экономического статуса9. Тяжелые психические расстройства (например, шизофрения и биполярное расстройство) становятся выделяющейся категорией в общей статистике. По данным исследований, представители этой группы умирают на 8–25 лет раньше, чем в общей популяции10,11. Несмотря на вклад психических расстройств в общее бремя болезней, качество помощи при этих расстройствах остается субоптимальным и существуют недочеты в оценке и оказании психиатрической помощи во всем мире12-18.
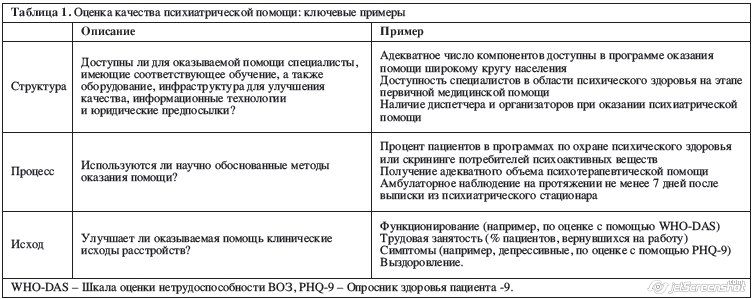
Качество помощи, как описано в Donabedian framework, включает структуру или организацию помощи, влияние структуры на клинический процесс помощи в оказанном объеме и, в конечном счете, исходы оказания медицинской помощи на уровне пациента19-21 (табл. 1). Эта системно-уровневая перспектива оценки качества оказания медицинской помощи стала основой для двух медицинских докладов институтов США: Crossing the Quality Chasm22 в 2001 году и Improving the Quality of Health Care for Mental and Substance-Use Conditions23 в 2006 году.
Сообщение Crossing the Quality Chasm подчеркнуло шесть целей на пути к улучшению качества: безопасность, эффективность, пациент-ориентированность, своевременность, рациональность и беспристрастность помощи, – которые все вместе можно оформить в постулат «Качественные проблемы происходят обычно не из-за нехватки финансирования, знаний, старания или ресурсов, потраченных на медицинскую помощь, а из-за фундаментальных недостатков организации этой помощи»22. В докладе 2006 года в дальнейшем также отмечено существование недостатков в качестве оказания психиатрической помощи и прозвучал призыв к системным попыткам улучшения качества в этой области23.
Тем не менее общее качество психиатрической помощи едва ли было улучшено со времени этих публикаций, а в некоторых случаях – со временем и ухудшилось24. В США только треть нуждающихся получают адекватную медицинскую психиатрическую помощь25. Уровень качества психиатрической помощи низок, и улучшения мало сравнимы с улучшениями, происходящими в системе общей медицинской помощи26. Например, недавние результаты показали, что менее чем половина пациентов с бюджетной страховкой получают адекватное амбулаторное наблюдение после госпитализации в психиатрический стационар27. Это постоянное упущение в качестве медицинской помощи образовалось из-за недостатков систематических методов оценки качества. Мы не можем улучшить то, что не измеряется.
Так как стоимость медицинского обслуживания растет и психические расстройства становятся все более распространенными по всему миру, руководители психиатрических служб будут нуждаться в обоснованной информации о качестве помощи, для того чтобы определить нужды населения и принять решение, как улучшить оказание помощи, а также применить эффективные стратегии для улучшения качества и уменьшения недостатков. В данной статье описывается текущее состояние оценки качества психиатрической помощи, проблемы изложены в международном контексте и предполагают следующий шаг для системы психиатрической помощи по всему миру для лучшего применения оценки качества и, в конечном счете, улучшения качества психиатрической помощи.
Структурные компоненты оказания медицинской помощи, такие как ресурсы (специалисты, обучение, оборудование) и стратегии, поддерживающие помощь, основанную на доказанных данных, являются фундаментальными в достижении высокого качества помощи. Однако пока не будут выбраны надлежащие способы измерения для документирования процессов и результатов, а также проведения мероприятий по улучшению помощи, не будет достигнуто необходимых желаемых результатов.
В идеальном случае измерение процесса может заполнить эти пробелы и дать оценку – рекомендована ли эта практика, основанная на доказательствах. Эти измерения обычно включают операциональные клинические руководства в специфически определенных наименованиях и нумерациях, используя данные, которые могут быть надежно получены из возможно оцененных источников данных. Однако многие широко используемые методы измерения процессов в области психического здоровья мало доказательны для использования в оценке качества психической помощи и улучшения исходов. Лишь несколько исследований касались качества оценки процесса оказания помощи для улучшения функционирования пациентов и клинических исходов в ракурсе ответа на вопрос о клинической валидности этих измерений. Недавно были отмечены некоторые значительные исключения, показавшие, что измерения для улучшения процесса оказания помощи (например, подходящая фармакотерапия, продолжительность лечения и использование психотерапии) связаны с уменьшением смертности28-31 и тяжести расстройства32. До сих пор среди существующих методов измерения процесса в области психического здоровья, которые могут быть упомянуты, не все были подтверждены подобным образом25,26,33-39.
Оценка методов измерения исходов исследует, действительно ли получаемая пациентом помощь улучшает его/ее симптомы – например, улучшение или ремиссия по шкале Опросника здоровья пациента-9 (PHQ-9) или функционирование. Эти измерения также могут использоваться при планировании, мониторинге и изменениях параметров помощи (например, изменение в лечении, мультикомпонентность, сотрудничество с другими специалистами). Однако для рассмотрения сложности психических расстройств оценка исхода психического расстройства должна фокусироваться не только на симптомах и функционировании, но и на таких параметрах, как качество жизни, выздоровление и пребывание в социуме.
Более того, использование измерений исходов с целью оценки качества психиатрической помощи предполагает сложные подходы фиксации для контроля, учитывающие факторы риска со стороны пациента, такие как тяжесть расстройства, история расстройства/статус здоровья, социально-демографические факторы для минимизации ложного эффекта «пожинания плодов» с наиболее здоровых пациентов. Таким образом, это может стать проблемой, как правило, из-за ограниченной доступности сведений о психиатрических симптомах, социальном контексте и других характеристиках пациентов. В большей степени есть необходимость для сбалансированности портфолио измерений добавить данные об опыте пациентов, чтобы иметь представление о структуре системы помощи, которую они получали, а также самоотчетов по исходам.
Кроме того, недостатки методов и инструментов измерений исходов в сфере оказания психиатрической помощи включены в текущие информационные системы и другие быстро меняющиеся технологии. Недостатки обычного общесистемного сбора в пределах существующей электронной системы медицинской помощи могут в конечном счете препятствовать длительным улучшениям качества. Для смягчения данных проблем эксперты системы психического здоровья включают помощь, основанную на измерениях, для продвижения использования измерений исходов в повседневности.
Помощь, основанная на измерениях, является центральным компонентом модели лечения хронических заболеваний40-42 и использует сбор данных для реализации пациент-ориентированных планов лечения. Это достигается специальным диспетчером медицинской помощи, который также координирует лечение между различными специалистами, в соответствии с текущим состоянием пациента и его предпочтениями. Модель лечения хронических заболеваний была показана в нескольких рандомизированных исследованиях для улучшения исходов физического и психического здоровья при различных психических расстройствах с небольшими дополнительными затратами или без таковых42. Медицинская помощь, основанная на измерении, полагается на клинические измерения (например, PHQ-9, mental health vital signs), а также систематическую, лонгитудную и ориентированную на действие помощь для записи и оценки ответа на изменения в индивидуальных исходах, таких как тяжесть симптомов и достижение целей.
Ключевыми межнациональными примерами помощи, основанной на измерении, являются Improving Access to Psy-chological Therapies (IAPT) – программа в National Health Service Великобритании43,44, голландская модель комплексного лечения в первичной психиатрической помощи – Depression Initiative45 и австралийская модель True-Blue46. Примечательно, что после пилотного тестирования и успешной оценки IAPT была распространена в Великобритании для по меньшей мере 1,5 млн взрослых для оценки медицинской помощи ежегодно до 2020/21 года47, а модель комплексного лечения первичной психиатрической помощи была включена в Нидерландах в список национально необходимых пособий как часть медицинской страховки45. Однако эти программы не коснулись всех пациентов с психическими расстройствами, и большинство специалистов, оказывающих медицинскую помощь, не применяют основанное на измерениях лечение в повседневной практике48,49.
В США есть более наглядные примеры общественных и частных программ лечения, основанных на измерениях, и первичной и специализированной психиатрической помощи, утвержденные как клинические инструменты, но не используемые широко для оценки качества. Примерами внедренных в США в отдельные группы пациентов методов измерений являются Sequenced Treatment Alternatives to Relieve Depression (STAR*D)50, Department of Veterans Affairs Behavioral Health Laboratory model51,52 и Department of Defense Behavioral Health Data Portal53. В штате Миннесота инициатива The Depression Improvement Across Minnesota, Offering a New Direction (DIA-MOND) осуществляет основанную на измерениях помощь для поддержки стандартных улучшений качества как часть финансовой системы для организации лечения депрессии54.
Развитие и применение измерений качества психиатрической помощи отстает в сравнении с другими областями медицины. Например, в США измерение качества используется при хронических расстройствах для оценки компенсации через Medicare, правительственную программу страховки для пожилых лиц (например, Value-Based Purchasing Modifier55), Medicaid56, State Medicaid Reporting Programs57 и стандартные методы оценки качества лечения в частном секторе (например, PhysicianCompare.Gov58, Hospital-Compare.Gov59). Тем не менее, несмотря на паритетные законы в области психического здоровья, принятые десять лет назад, которые устанавливают равнозначное покрытие для психических расстройств и доступность свыше 500 методов измерений для мониторинга качества психиатрической помощи, только 5% этих измерений в действительности используются в вышеупомянутых программах оценки качества, и только 10% этих измерений утверждены Американским национальным форумом качества60 (например, Value Based Inpatient Psychiatry Quality Reporting Program61). Большинство из этих доступных методов измерений (72%) фокусируются на процессах довольно отдаленных от исходов (например, скрининг/оценка)60 вместо измерений процесса, выражающих адекватность или интенсивность психиатрического лечения.
С другой стороны, существует много недостатков в доказательности для поддержания измерения качества психиатрической помощи, особенно для исходов, наиболее значимых для пациентов, так же как и специфической популяции, например для детей. Эти измерения имеют недостаток в оценке специфичных для популяции состояний, например таких, как тревожные расстройства, и в оценке глубины основанных на доказательстве методов лечения, например психотерапии. В то время как имеется устоявшаяся доказанность методов лечения, таких как психофармакотерапия, психотерапия со специальным руководством (например, когнитивно-бихевиоральная психотерапия), и групповые интервенции (ассертивно-поведенческая терапия), доказательность многих других психосоциальных интервенций нуждается в дальнейшем развитии62. Для психотерапии, основанной на доказательствах, качество измерений не может полностью зафиксировать адекватность оказания помощи. Более того, многие поставщики медицинских услуг могут систематизировать психосоциальные интервенции в данные руководства, но не в качестве подтверждения, что помощь была точно соответствующей23,63.
Также отмечается недостаточное внимание к развитию и внедрению измерений производительности, отражающих мнение пациентов и выбор лечения. Как результат, лишь несколько методов измерений используются при оценке качества психиатрической помощи, в особенности уровня выздоровления. US Substance Abuse and Mental Health Services Administration определяет выздоровление после психического расстройства как «процесс изменения, через который индивидуум улучшает его здоровье и самочувствие, жизнь и саморегуляцию и старается достигнуть своего наивысшего потенциала»64. Все же определение допустимых методов измерения выздоровления было затруднено из-за недостатка понимания функционального определения выздоровления, которое можно измерить для поставщиков медицинских услуг, в научном сообществе, и, что наиболее важно, для получающих психиатрическую помощь. В то время как это частично не связано с субъективными процессами выздоровления, это привело к большой вариабельности в надежности и валидности методов и инструментов измерения выздоровления. Помимо нужд для дальнейшей доказательности, в поддержание развития клинического направления и широкого спектра обоснованных и полезных исходов, сообщаемых пациентом, в развитие и тестирование качества психиатрической помощи и измерения выздоровления был сделан небольшой вклад для оценки их обоснованности, применимости и всесторонности.
Более того, область психического здоровья находится далеко позади других сфер медицины из-за внедрения технологий, особенно технологии информирования о здоровье для овладения релевантной информацией о нем, которая может поддержать отчетность по качеству психиатрической помощи. Несмотря на систему поощрений для внедрения электронной фиксации данных о здоровье (например, HITECH акт в США), нет специфических требований по всему миру для строгого включения данных, касающихся психического здоровья, в электронные записи. В настоящее время многие методы измерения психиатрической помощи не связаны с существующими источниками данных, которые в большинстве случаев опираются на данные жалоб вместо сопоставления со сведениями, полученными из электронных записей о здоровье или по электронным записям пациентов26,65. В результате эти измерения не могут автоматически формировать значимые данные60, которые, в свою очередь, могли бы поддержать измерение качества и дать необходимую информацию для повседневной практики. Кроме того, лица, оказывающие психиатрическую помощь, часто используют иные электронные медицинские системы записей, в отличие от коллег из общей медицины, или не имеют доступа к этим системам вовсе, что создает большие проблемы для включения области психического здоровья в измерение качества и улучшения помощи для пациентов, которым часто необходим координированный сервис для сравнения между различными секторами.
В некоторых странах, в которых существуют базы данных о претензиях или базы электронных медицинских записей, автоматизированное измерение психиатрической помощи было адаптировано в том или ином виде66,67. Например, Национальная служба здоровья Великобритании (UK National Health Service) имеет долгую традицию использования электронных медицинских данных в звене первичной помощи для общего измерения качества, что наиболее заметно в Системе качества исходов (Quality Outcomes Framework) – это самая большая программа в мире, основанная на оплате по результату. На протяжении последних 10 лет Национальная служба здоровья (National Health Service) пыталась включить аналогичную программу по системе возмещения, основанную на исходе, в сферу психиатрической помощи68.
В этой системе координат обычные измерения являются обязательными для оценки финансирования. Однако проблемы администрирования повлекли за собой и риск «игры» (например, ошибочные отчеты для повышения производительности), что привело к сопротивлению со стороны профессионалов68,69. Сейчас программа была отложена на неопределенный срок в пользу более мелких областей работы70. Одной из этих областей является ранее упомянутая IAPT инициатива, внедрившая обычное измерение исходов с помощью валидизированных инструментов, таких как PHQ-9 и Шкалы клинических исходов в повседневном измерении (CORE), – и может показать хорошие исходы, что приведет к дальнейшему субсидированию и законодательной помощи71. В Канаде было внедрено измерение качества психиатрической помощи в электронных медицинских записях67. Тем не менее, из-за давней стигматизации и функциональных проблем, лица, получающие психиатрическую помощь, могут чувствовать себя уязвленными сбором такой информации. В целом, интеграция информационных технологий о здоровье в повседневную практику оказания психиатрической помощи является первостепенной для поддержания помощи, основанной на измерении, для психического здоровья72,73.
Кроме того, неоднородность образования лиц, оказывающих помощь, и требований сертификации в сфере психиатрической помощи также может препятствовать внедрению измерений качества психиатрической помощи. Например, несмотря на их выраженное вовлечение в психиатрическую помощь, только менее чем треть социальных работников США получают образование по измерению качества и эффективности клинической практики74. Более того, многие проблемы, которые лица, оказывающие помощь, адресуют своим пациентам, включают потребности за пределами системы оказания помощи (трудоустройство, жилищные условия, образование, уголовное правосудие и социальное обеспечение), и качество помощи этих сервисов редко измеряется для обеспечения улучшения исходов психического здоровья и выздоровления. Эти сервисы часто требуют координации между различными сферами, условиями, организациями и даже секторами, но появляется мало стимулов к улучшению качества, когда отсутствуют методы измерения для оценки соответствия для этих сервисов. Заметное исключение этого было первоочередной целью Американского проекта межорганизационного прекращения бездомности ветеранов, где Американский департамент по делам ветеранов начал работу с другими федеральными, региональными и местными организациями для обеспечения бездомных ветеранов ваучерами на жилье и отслеживания результатов в последующем75.
Наконец, культурные и административные различия между лицами, оказывающими помощь в сфере физического и психического здоровья, препятствуют измерению качества. Сервисы «Физического» и «Психического здоровья» во многих странах, если не в большинстве, часто отделены на клиническом, организационном, политическом и финансовом уровнях. Психиатрическая помощь также требует больше командных усилий между психиатрами, социальными работниками, психологами и руководителями.
Международные инновации в оценке качества включают в себя Assessment Instrument for Mental Health Systems Всемирной организации здравоохранения (ВОЗ)76 и International Initiative for Mental Health Leadership77, которая предоставляет данные об отчетности, возможности сообщать и устанавливать данные по странам.
В Голландии регулярный контроль за результатами был включен в механизмы возмещения расходов на медицинское страхование. Таким образом оцениваются три аспекта качества: эффективность лечения, безопасность и удовлетворенность клиента – посредством 10 показателей, которые оцениваются в начале и в конце лечения78. Инициатива предусматривает, что показатели собираются централизованно и публикуются прозрачно с целью стимулировать постоянное повышение качества.
В Австралии в 2000 году было принято решение об использовании стандартизированных показателей результативности для всех, кто получал помощь в области психического здоровья, и все австралийские штаты подписали соглашения о представлении регулярно собираемых данных по результатам и совокупности случаев. Основными показателями результатов являются шкала оценки здоровья нации (HoNOS) и инструмент оценки качества жизни. Для того чтобы реализовать эту инициативу в таких больших масштабах, требуются значительные инвестиции в организации, предоставляющие услуги в области психического здоровья, постоянное обучение и программа развития взаимодействия79.
В Новой Зеландии поставщики психиатрических услуг ориентированы на ключевые показатели, такие как уменьшение замкнутости и изоляции, снижение уровня самоубийств80. В Великобритании National Health Service Benchmarking Network81 – это сотрудничество между всеми организациями, оказывающими услуги в области психического здоровья, которые предоставляют данные для сравнения своих собственных показателей деятельности с другими. Сеть бенчмаркинга была разработана из-за предполагаемой неадекватности национальной системы сбора данных и отсутствия обратной связи по большому объему собранных данных. Как инициатива «на местах», сеть бенчмаркинга требует активного участия и динамичного руководства.
В США предпринимаются национальные усилия по определению междисциплинарных показателей оценки качества психиатрической помощи и определению, кто ответственен за повышение качества. В департаменте по делам ветеранов центральным руководством установлены меры по повышению качества для реализации в более чем 160 медицинских центрах. В то время как качество психиатрической помощи в департаменте задокументировано, распространены региональные различия в процессе и результатах лечения82-86. Таким образом, с учетом того, что региональные руководители психиатрической службы ответственны за повышение качества, департамент запустил национальные инициативы по повышению качества помощи и уменьшению различий в оказании психиатрической помощи, во многом посредством разработки Единого руководства по оказанию психиатрической помощи (Uniform Mental Health Services Handbook)87 и внедрения специалистов в области психического здоровья в первичную медицинскую помощь для обеспечения интегрированной помощи. Департамент также спонсировал национальное внедрение научно обоснованной психотерапии посттравматического стрессового расстройства88.
Модели оплаты по результатам работы, также называемые «оплатой на основе воспринимаемой ценности» (это подход, при котором цена формируется на основе ценности для потребителя. – Прим. пер.)89, не менее часто пропагандируются в США и по всему миру. Такие инициативы вознаграждают организации за улучшение результатов и начинают использоваться в области психического здоровья90,91. Другие инновации включают помощь вне стен клиник, в частности оценку реабилитационных служб92 и развитие мобильного здравоохранения для сбора данных о результатах65,93. Центры услуг по программам Medicare и Medicaid в США также разворачивают инициативы, посредством которых стремятся повысить заинтересованность специалистов в применении доказательных методов и организаций, оказывающих медицинские услуги, в их поддержке. Основной целью было включение психиатрической помощи в первичное звено медицинской помощи, куда обращаются большинство пациентов с симптомами психических расстройств в начальной стадии. Согласно Breakthrough Series Института по развитию здравоохранения были применены бизнес-практики для внедрения длительного лечения депрессии в первичное звено медицинской помощи94. Кроме того, существуют и другие инновации в области интеграции психического здоровья в первичную помощь (например, исследовательская сеть системы здравоохранения, местные центры психического здоровья – система здравоохранения Чероки95), однако существует мало механизмов для расширения их масштабов и дальнейшего распространения.
В Великобритании комитет по качеству и инновациям внедряет систему оплаты за работу в области психического здоровья, в рамках которой выплаты основаны на достижении национальных целевых показателей повышения качества96. Целевые показатели устанавливаются на локальном уровне, но в соответствии с центрально установленными задачами. Тем не менее неизбежные различия в оказании медицинской помощи затрудняют разработку показателей качества в области психического здоровья.
Наконец, в настоящее время предпринимаются усилия по привлечению групп с участием многих заинтересованных сторон к обеспечению обратной связи на протяжении всего процесса разработки и внедрения оценки качества. В то время как врачи-клиницисты часто в состоянии обеспечить исходные данные для разработки способов оценки качества, получение обратной связи от потребителей и их опекунов также считается важным97. Byron и соавт.98 описывают процесс вовлечения заинтересованных сторон на всех уровнях разработки оценки качества и реализации в законе об улучшении финансирования программы медицинского страхования детей (Children’s Health Insurance Program Reauthorization Act – CHIPRA). План разработки оценки качества описывает запланированный процесс, включая привлечение заинтересованных сторон99. Национальный форум по качеству использует метод консенсуса для рассмотрения и одобрения показателей, включая время на общественное обсуждение100. Кроме того, центры услуг по программам Medicare и Medicaid недавно созвали группы экспертов, в которые включены клиницисты, статисты, эксперты по повышению качества и методисты, для разработки, отбора и утверждения показателей101.

Во-вторых, должны быть разработаны и внедрены общие критерии для диагнозов, клинической оценки и «витальных» признаков психического здоровья, которые также следует интегрировать с существующей электронной медицинской документацией и другими инструментами информационных технологий, такими как смартфоны. Другие компоненты, которые необходимо стандартизировать, включают кодирование в электронной учетной документации и административных базах данных медицинских вмешательств, таких данных, как медикаментозная терапия, психотерапия (включая мероприятия по оценке сообразности и применения по назначению) и другие виды терапии или ухода. Такие инновации, как обработка естественного языка или автоматизированный сбор данных из электронной медицинской документации, уже применяются для облегчения сбора данных с целью получения информации (например, данные о бездомности или суицидальном риске), которая не является очевидной.
В-третьих, результаты лечения в области психического здоровья должны оцениваться на регулярной основе, и помощь, основанная на оценке, должна быть не только внедрена в имеющиеся технологии, но и стать частью культуры лечения и здравоохранения. Было показано, что регулярная оценка результатов связана с улучшениями в оказании услуг и более низким уровнем повторных госпитализаций103, в то время как нерегулярная оценка результатов незначительно влияет на повышение качества104. Более того, регулярная оценка результатов, о которой оповещали клинициста и которая была использована для совместного с пациентом принятия решений по лечению, вела к улучшению качества жизни105. Показатели оценки качества, посредством которых можно вести мониторинг данных о качестве в режиме реального времени, необходимо применять в системах здравоохранения, чтобы содействовать повышению качества, и необходимо отслеживать непреднамеренные, неучтенные последствия.
В-четвертых, системы здравоохранения должны обеспечивать инвестиции, руководство и координацию в целях совершенствования и обеспечения связи источников данных для оценки качества в различных условиях. Здравоохранение должно будет вовлекать поставщиков и потребителей в процесс утверждения показателей качества и разработки мер, отвечающих потребностям поставщиков и потребителей, а не администрации. Слишком часто систематическая оценка качества результатов обусловлена желанием сообщить данные политикам или сократить расходы, а не стремлением улучшить качество оказываемой помощи отдельным лицам, что может иметь неблагоприятные последствия, если сотрудники (которые должны предоставлять данные) воспринимают это как отвлекающий фактор, не имеющий большого значения. Такие меры, как сеть бенчмаркинга Великобритании, являются хорошим способом внедрения этих перспектив106.
Наконец, системы здравоохранения нуждаются в действенном способе стратификации показателей качества, с тем чтобы устранить потенциальные пробелы среди субпопуляций и выявить группы, в которых наиболее необходимо повышение качества. Большое значение имеет более длительное обучение персонала и повышение его эффективности. Стратегии повышения качества и подотчетности необходимо адаптировать, разрабатывать и регулярно применять в психиатрических учреждениях.
В табл. 2 мы предлагаем масштабный многоуровневый процесс, который очерчивает препятствия оценки качества и потенциальные средства, ведущие к повышению качества107. Этот процесс, основанный на Обучающей модели организации здравоохранения Национальной академии медицины США (US National Academy of Medicine Learning Health Care System), был доработан, чтобы включить в него «рычаги», направленные на организационные барьеры в психиатрическом здравоохранении108. Обучающая модель организации здравоохранения предполагает использование существующих данных (например, электронные медицинские записи) для внедрения и оценки инноваций и новых методов среди различных организаций с целью улучшения здоровья населения.

Рекомендации по повышению качества психиатрической помощи, представленные здесь, можно применять в здравоохранении в целом. В действительности, область психического здоровья стала первопроходцем во множестве других инноваций в здравоохранении, таких как вовлечение общества в оказание помощи, применение инновационных моделей интегрированной помощи, равно как и пациент-ориентированных мер по реабилитации. Кроме того, на примере психиатрической помощи были изучены ошибки, которые должны быть учтены при развитии обучающей модели организации здравоохранения в других отраслях здравоохранения. Долгие годы пациенты и члены их семей боролись за пациент-ориентированную помощь и больший акцент на личные цели пациента, помимо получения медицинских услуг.
Разнородные источники оказания психиатрической помощи также усложняют здравоохранению задачу учитывать мнение и взгляды персонала, включая медсестер, социальных работников, и увеличивающееся количество аналогичных специалистов, в повышении качества. Неудивительно, что многие методы по повышению качества, использованные в психиатрической области здравоохранения, повлияли на развивающуюся область имплементационной науки (implementation science)109, которая заключается в изучении поведенческих изменений у поставщиков в контексте организационных ограничений. Наконец, развитие моделей оплаты на основе «воспринимаемой ценности», которая вознаграждает организации по оказанию медицинской помощи и поставщиков на основе достижения результатов, а не увеличения объема, является многообещающим методом повышения качества психиатрической помощи.
БЛАГОДАРНОСТИ
Данная работа выполнена при поддержке Department of Veterans Affairs, Veterans Health Administration, the Irving Institute, и National Institutes of Health (R01 MH 099898). Дополнительная поддержка была оказана Commonwealth Fund (грант № 20141104) и National Center for Advancing Translational Sciences, National Institutes of Health (грант № UL1 TR000040). В работе представлены взгляды авторов, которые не обязательно отражают позицию Department of Veterans Affairs, the National Institutes of Health или других организаций.
DOI: 10.1002/wps.20482
Редактура: к.м.н. Федотов И.А. (Рязань)
Психические расстройства по всему миру схожи, однако качество медицинской помощи в области этих расстройств не улучшается, так же как не улучшается и качество оказания медицинской помощи при соматических заболеваниях. В данном исследовании мы показали условия продвижения количественных измерений как инструмента улучшения качества помощи в области психических расстройств. Мы выделили ключевые барьеры, включая недостаток стандартизированной информации по данным ресурсам, основанным на информационных технологиях, ограниченность научной доказательности для измерения качества оказания психиатрической помощи, недостаток доступности образования и поддержки, а также культуральные барьеры при интеграции психиатрической помощи в общемедицинскую сеть. Мы описываем несколько инноваций, которые внедряются по всему миру и могут уменьшить эти барьеры. Основываясь на этом опыте, мы предлагаем несколько рекомендаций для улучшения качества психиатрической помощи. Для получателей и организаторов в области психического здоровья важно иметь портфолио, включающее валидизированные методы измерения исходов в пределах спектров различных состояний. Необходимо внедрить в существующую электронную базу элементы общих данных. Исходы психических расстройств требуют регулярной оценки, и именно помощь, основанная на измерении, должна стать частью всей культуры и системы оказания медицинской помощи. Система оказания медицинской помощи требует валидизированного способа качественных измерений для выявления наиболее уязвимых групп населения, требующих медицинской помощи и анализа недочетов. Еще больше внимания должно быть уделено обучению сотрудников в направлении увеличения объема и качества медицинской помощи. Область улучшения качества психиатрической помощи является командным делом, требующим координации между различными сферами, включающими защиту прав пациентов, а также увеличение ресурсов и оплаты от получателя помощи и системы здравоохранения.
Ключевые слова: психические расстройства, качество помощи, измерения качества, информированность о здоровье, электронные записи о здоровье, пациент-ориентированные исходы, системы оказания медицинской помощи, стратегия здоровья.
(World Psychiatry 2018;17:30–38)
Психические расстройства во всем мире являются причиной 32% лет нетрудоспособности и 13% лет адаптации к нетрудоспособности в скорректированном сроке жизни1. Более того, лица с этими расстройствами выявляют повышенные уровни смертности от распространенных медицинских состояний2-4. Среди лиц с психическими расстройствами различия в качестве и исходах оказания медицинской помощи более явно выражены для расовых/этнических меньшинств6-8 и у представителей групп низкого социально-экономического статуса9. Тяжелые психические расстройства (например, шизофрения и биполярное расстройство) становятся выделяющейся категорией в общей статистике. По данным исследований, представители этой группы умирают на 8–25 лет раньше, чем в общей популяции10,11. Несмотря на вклад психических расстройств в общее бремя болезней, качество помощи при этих расстройствах остается субоптимальным и существуют недочеты в оценке и оказании психиатрической помощи во всем мире12-18.
Качество помощи, как описано в Donabedian framework, включает структуру или организацию помощи, влияние структуры на клинический процесс помощи в оказанном объеме и, в конечном счете, исходы оказания медицинской помощи на уровне пациента19-21 (табл. 1). Эта системно-уровневая перспектива оценки качества оказания медицинской помощи стала основой для двух медицинских докладов институтов США: Crossing the Quality Chasm22 в 2001 году и Improving the Quality of Health Care for Mental and Substance-Use Conditions23 в 2006 году.

Сообщение Crossing the Quality Chasm подчеркнуло шесть целей на пути к улучшению качества: безопасность, эффективность, пациент-ориентированность, своевременность, рациональность и беспристрастность помощи, – которые все вместе можно оформить в постулат «Качественные проблемы происходят обычно не из-за нехватки финансирования, знаний, старания или ресурсов, потраченных на медицинскую помощь, а из-за фундаментальных недостатков организации этой помощи»22. В докладе 2006 года в дальнейшем также отмечено существование недостатков в качестве оказания психиатрической помощи и прозвучал призыв к системным попыткам улучшения качества в этой области23.
Тем не менее общее качество психиатрической помощи едва ли было улучшено со времени этих публикаций, а в некоторых случаях – со временем и ухудшилось24. В США только треть нуждающихся получают адекватную медицинскую психиатрическую помощь25. Уровень качества психиатрической помощи низок, и улучшения мало сравнимы с улучшениями, происходящими в системе общей медицинской помощи26. Например, недавние результаты показали, что менее чем половина пациентов с бюджетной страховкой получают адекватное амбулаторное наблюдение после госпитализации в психиатрический стационар27. Это постоянное упущение в качестве медицинской помощи образовалось из-за недостатков систематических методов оценки качества. Мы не можем улучшить то, что не измеряется.
Так как стоимость медицинского обслуживания растет и психические расстройства становятся все более распространенными по всему миру, руководители психиатрических служб будут нуждаться в обоснованной информации о качестве помощи, для того чтобы определить нужды населения и принять решение, как улучшить оказание помощи, а также применить эффективные стратегии для улучшения качества и уменьшения недостатков. В данной статье описывается текущее состояние оценки качества психиатрической помощи, проблемы изложены в международном контексте и предполагают следующий шаг для системы психиатрической помощи по всему миру для лучшего применения оценки качества и, в конечном счете, улучшения качества психиатрической помощи.
ТЕКУЩЕЕ СОСТОЯНИЕ ОЦЕНКИ КАЧЕСТВА ПСИХИАТРИЧЕСКОЙ ПОМОЩИ
Во всем мире попытки стандартизации оценки оказания психиатрической помощи развиваются очень медленно. Изменение и описание качества помощи в обычном контексте не дает предпосылок для улучшения качества помощи на уровне врачей, равно как и подконтрольность механизмов, включая публичные обсуждения, а также финансовые взыскания и поощрения. Однако измерение качества психиатрической помощи является важной проблемой по всему миру, так как она может быть разной в зависимости от особенностей организационной структуры в каждой конкретной стране. В целом, измерение структуры, процесса и исхода лечения включено в аттестацию, стандартизацию, измерение качества и рутинную отчетность психиатрической службы. Каждые из этих пунктов имеет сильные и слабые стороны, и неизбежно необходим баланс между этими категориями медицинской помощи.Структурные компоненты оказания медицинской помощи, такие как ресурсы (специалисты, обучение, оборудование) и стратегии, поддерживающие помощь, основанную на доказанных данных, являются фундаментальными в достижении высокого качества помощи. Однако пока не будут выбраны надлежащие способы измерения для документирования процессов и результатов, а также проведения мероприятий по улучшению помощи, не будет достигнуто необходимых желаемых результатов.
В идеальном случае измерение процесса может заполнить эти пробелы и дать оценку – рекомендована ли эта практика, основанная на доказательствах. Эти измерения обычно включают операциональные клинические руководства в специфически определенных наименованиях и нумерациях, используя данные, которые могут быть надежно получены из возможно оцененных источников данных. Однако многие широко используемые методы измерения процессов в области психического здоровья мало доказательны для использования в оценке качества психической помощи и улучшения исходов. Лишь несколько исследований касались качества оценки процесса оказания помощи для улучшения функционирования пациентов и клинических исходов в ракурсе ответа на вопрос о клинической валидности этих измерений. Недавно были отмечены некоторые значительные исключения, показавшие, что измерения для улучшения процесса оказания помощи (например, подходящая фармакотерапия, продолжительность лечения и использование психотерапии) связаны с уменьшением смертности28-31 и тяжести расстройства32. До сих пор среди существующих методов измерения процесса в области психического здоровья, которые могут быть упомянуты, не все были подтверждены подобным образом25,26,33-39.
Оценка методов измерения исходов исследует, действительно ли получаемая пациентом помощь улучшает его/ее симптомы – например, улучшение или ремиссия по шкале Опросника здоровья пациента-9 (PHQ-9) или функционирование. Эти измерения также могут использоваться при планировании, мониторинге и изменениях параметров помощи (например, изменение в лечении, мультикомпонентность, сотрудничество с другими специалистами). Однако для рассмотрения сложности психических расстройств оценка исхода психического расстройства должна фокусироваться не только на симптомах и функционировании, но и на таких параметрах, как качество жизни, выздоровление и пребывание в социуме.
Более того, использование измерений исходов с целью оценки качества психиатрической помощи предполагает сложные подходы фиксации для контроля, учитывающие факторы риска со стороны пациента, такие как тяжесть расстройства, история расстройства/статус здоровья, социально-демографические факторы для минимизации ложного эффекта «пожинания плодов» с наиболее здоровых пациентов. Таким образом, это может стать проблемой, как правило, из-за ограниченной доступности сведений о психиатрических симптомах, социальном контексте и других характеристиках пациентов. В большей степени есть необходимость для сбалансированности портфолио измерений добавить данные об опыте пациентов, чтобы иметь представление о структуре системы помощи, которую они получали, а также самоотчетов по исходам.
Кроме того, недостатки методов и инструментов измерений исходов в сфере оказания психиатрической помощи включены в текущие информационные системы и другие быстро меняющиеся технологии. Недостатки обычного общесистемного сбора в пределах существующей электронной системы медицинской помощи могут в конечном счете препятствовать длительным улучшениям качества. Для смягчения данных проблем эксперты системы психического здоровья включают помощь, основанную на измерениях, для продвижения использования измерений исходов в повседневности.
Помощь, основанная на измерениях, является центральным компонентом модели лечения хронических заболеваний40-42 и использует сбор данных для реализации пациент-ориентированных планов лечения. Это достигается специальным диспетчером медицинской помощи, который также координирует лечение между различными специалистами, в соответствии с текущим состоянием пациента и его предпочтениями. Модель лечения хронических заболеваний была показана в нескольких рандомизированных исследованиях для улучшения исходов физического и психического здоровья при различных психических расстройствах с небольшими дополнительными затратами или без таковых42. Медицинская помощь, основанная на измерении, полагается на клинические измерения (например, PHQ-9, mental health vital signs), а также систематическую, лонгитудную и ориентированную на действие помощь для записи и оценки ответа на изменения в индивидуальных исходах, таких как тяжесть симптомов и достижение целей.
Ключевыми межнациональными примерами помощи, основанной на измерении, являются Improving Access to Psy-chological Therapies (IAPT) – программа в National Health Service Великобритании43,44, голландская модель комплексного лечения в первичной психиатрической помощи – Depression Initiative45 и австралийская модель True-Blue46. Примечательно, что после пилотного тестирования и успешной оценки IAPT была распространена в Великобритании для по меньшей мере 1,5 млн взрослых для оценки медицинской помощи ежегодно до 2020/21 года47, а модель комплексного лечения первичной психиатрической помощи была включена в Нидерландах в список национально необходимых пособий как часть медицинской страховки45. Однако эти программы не коснулись всех пациентов с психическими расстройствами, и большинство специалистов, оказывающих медицинскую помощь, не применяют основанное на измерениях лечение в повседневной практике48,49.
В США есть более наглядные примеры общественных и частных программ лечения, основанных на измерениях, и первичной и специализированной психиатрической помощи, утвержденные как клинические инструменты, но не используемые широко для оценки качества. Примерами внедренных в США в отдельные группы пациентов методов измерений являются Sequenced Treatment Alternatives to Relieve Depression (STAR*D)50, Department of Veterans Affairs Behavioral Health Laboratory model51,52 и Department of Defense Behavioral Health Data Portal53. В штате Миннесота инициатива The Depression Improvement Across Minnesota, Offering a New Direction (DIA-MOND) осуществляет основанную на измерениях помощь для поддержки стандартных улучшений качества как часть финансовой системы для организации лечения депрессии54.
ОСОБЫЕ ПРОБЛЕМЫ В ИЗМЕРЕНИИ КАЧЕСТВА ПСИХИАТРИЧЕСКОЙ ПОМОЩИ
В США и по всему миру измерение качества психиатрической помощи и лечение, основанное на измерении, имеют слабую инфраструктуру на фоне общей системы оказания медицинской помощи. Это происходит из-за многочисленных барьеров, специфически связанных с психическим здоровьем, которые включают ограничения в стратегиях и технологии, ограничения научной доказательности в измерении качества психического здоровья, из-за недостатка знаний и поддержки у специалистов, а также культуральных барьеров для интеграции служб психического здоровья в общемедицинскую сеть.Развитие и применение измерений качества психиатрической помощи отстает в сравнении с другими областями медицины. Например, в США измерение качества используется при хронических расстройствах для оценки компенсации через Medicare, правительственную программу страховки для пожилых лиц (например, Value-Based Purchasing Modifier55), Medicaid56, State Medicaid Reporting Programs57 и стандартные методы оценки качества лечения в частном секторе (например, PhysicianCompare.Gov58, Hospital-Compare.Gov59). Тем не менее, несмотря на паритетные законы в области психического здоровья, принятые десять лет назад, которые устанавливают равнозначное покрытие для психических расстройств и доступность свыше 500 методов измерений для мониторинга качества психиатрической помощи, только 5% этих измерений в действительности используются в вышеупомянутых программах оценки качества, и только 10% этих измерений утверждены Американским национальным форумом качества60 (например, Value Based Inpatient Psychiatry Quality Reporting Program61). Большинство из этих доступных методов измерений (72%) фокусируются на процессах довольно отдаленных от исходов (например, скрининг/оценка)60 вместо измерений процесса, выражающих адекватность или интенсивность психиатрического лечения.
С другой стороны, существует много недостатков в доказательности для поддержания измерения качества психиатрической помощи, особенно для исходов, наиболее значимых для пациентов, так же как и специфической популяции, например для детей. Эти измерения имеют недостаток в оценке специфичных для популяции состояний, например таких, как тревожные расстройства, и в оценке глубины основанных на доказательстве методов лечения, например психотерапии. В то время как имеется устоявшаяся доказанность методов лечения, таких как психофармакотерапия, психотерапия со специальным руководством (например, когнитивно-бихевиоральная психотерапия), и групповые интервенции (ассертивно-поведенческая терапия), доказательность многих других психосоциальных интервенций нуждается в дальнейшем развитии62. Для психотерапии, основанной на доказательствах, качество измерений не может полностью зафиксировать адекватность оказания помощи. Более того, многие поставщики медицинских услуг могут систематизировать психосоциальные интервенции в данные руководства, но не в качестве подтверждения, что помощь была точно соответствующей23,63.
Также отмечается недостаточное внимание к развитию и внедрению измерений производительности, отражающих мнение пациентов и выбор лечения. Как результат, лишь несколько методов измерений используются при оценке качества психиатрической помощи, в особенности уровня выздоровления. US Substance Abuse and Mental Health Services Administration определяет выздоровление после психического расстройства как «процесс изменения, через который индивидуум улучшает его здоровье и самочувствие, жизнь и саморегуляцию и старается достигнуть своего наивысшего потенциала»64. Все же определение допустимых методов измерения выздоровления было затруднено из-за недостатка понимания функционального определения выздоровления, которое можно измерить для поставщиков медицинских услуг, в научном сообществе, и, что наиболее важно, для получающих психиатрическую помощь. В то время как это частично не связано с субъективными процессами выздоровления, это привело к большой вариабельности в надежности и валидности методов и инструментов измерения выздоровления. Помимо нужд для дальнейшей доказательности, в поддержание развития клинического направления и широкого спектра обоснованных и полезных исходов, сообщаемых пациентом, в развитие и тестирование качества психиатрической помощи и измерения выздоровления был сделан небольшой вклад для оценки их обоснованности, применимости и всесторонности.
Более того, область психического здоровья находится далеко позади других сфер медицины из-за внедрения технологий, особенно технологии информирования о здоровье для овладения релевантной информацией о нем, которая может поддержать отчетность по качеству психиатрической помощи. Несмотря на систему поощрений для внедрения электронной фиксации данных о здоровье (например, HITECH акт в США), нет специфических требований по всему миру для строгого включения данных, касающихся психического здоровья, в электронные записи. В настоящее время многие методы измерения психиатрической помощи не связаны с существующими источниками данных, которые в большинстве случаев опираются на данные жалоб вместо сопоставления со сведениями, полученными из электронных записей о здоровье или по электронным записям пациентов26,65. В результате эти измерения не могут автоматически формировать значимые данные60, которые, в свою очередь, могли бы поддержать измерение качества и дать необходимую информацию для повседневной практики. Кроме того, лица, оказывающие психиатрическую помощь, часто используют иные электронные медицинские системы записей, в отличие от коллег из общей медицины, или не имеют доступа к этим системам вовсе, что создает большие проблемы для включения области психического здоровья в измерение качества и улучшения помощи для пациентов, которым часто необходим координированный сервис для сравнения между различными секторами.
В некоторых странах, в которых существуют базы данных о претензиях или базы электронных медицинских записей, автоматизированное измерение психиатрической помощи было адаптировано в том или ином виде66,67. Например, Национальная служба здоровья Великобритании (UK National Health Service) имеет долгую традицию использования электронных медицинских данных в звене первичной помощи для общего измерения качества, что наиболее заметно в Системе качества исходов (Quality Outcomes Framework) – это самая большая программа в мире, основанная на оплате по результату. На протяжении последних 10 лет Национальная служба здоровья (National Health Service) пыталась включить аналогичную программу по системе возмещения, основанную на исходе, в сферу психиатрической помощи68.
В этой системе координат обычные измерения являются обязательными для оценки финансирования. Однако проблемы администрирования повлекли за собой и риск «игры» (например, ошибочные отчеты для повышения производительности), что привело к сопротивлению со стороны профессионалов68,69. Сейчас программа была отложена на неопределенный срок в пользу более мелких областей работы70. Одной из этих областей является ранее упомянутая IAPT инициатива, внедрившая обычное измерение исходов с помощью валидизированных инструментов, таких как PHQ-9 и Шкалы клинических исходов в повседневном измерении (CORE), – и может показать хорошие исходы, что приведет к дальнейшему субсидированию и законодательной помощи71. В Канаде было внедрено измерение качества психиатрической помощи в электронных медицинских записях67. Тем не менее, из-за давней стигматизации и функциональных проблем, лица, получающие психиатрическую помощь, могут чувствовать себя уязвленными сбором такой информации. В целом, интеграция информационных технологий о здоровье в повседневную практику оказания психиатрической помощи является первостепенной для поддержания помощи, основанной на измерении, для психического здоровья72,73.
Кроме того, неоднородность образования лиц, оказывающих помощь, и требований сертификации в сфере психиатрической помощи также может препятствовать внедрению измерений качества психиатрической помощи. Например, несмотря на их выраженное вовлечение в психиатрическую помощь, только менее чем треть социальных работников США получают образование по измерению качества и эффективности клинической практики74. Более того, многие проблемы, которые лица, оказывающие помощь, адресуют своим пациентам, включают потребности за пределами системы оказания помощи (трудоустройство, жилищные условия, образование, уголовное правосудие и социальное обеспечение), и качество помощи этих сервисов редко измеряется для обеспечения улучшения исходов психического здоровья и выздоровления. Эти сервисы часто требуют координации между различными сферами, условиями, организациями и даже секторами, но появляется мало стимулов к улучшению качества, когда отсутствуют методы измерения для оценки соответствия для этих сервисов. Заметное исключение этого было первоочередной целью Американского проекта межорганизационного прекращения бездомности ветеранов, где Американский департамент по делам ветеранов начал работу с другими федеральными, региональными и местными организациями для обеспечения бездомных ветеранов ваучерами на жилье и отслеживания результатов в последующем75.
Наконец, культурные и административные различия между лицами, оказывающими помощь в сфере физического и психического здоровья, препятствуют измерению качества. Сервисы «Физического» и «Психического здоровья» во многих странах, если не в большинстве, часто отделены на клиническом, организационном, политическом и финансовом уровнях. Психиатрическая помощь также требует больше командных усилий между психиатрами, социальными работниками, психологами и руководителями.
ИННОВАЦИИ В СФЕРЕ ОЦЕНКИ И СОВЕРШЕНСТВОВАНИЯ КАЧЕСТВА ОКАЗАНИЯ ПСИХИАТРИЧЕСКОЙ ПОМОЩИ
Во всем мире внедряется ряд инноваций для оценки и повышения качества психиатрической помощи. Эти инициативы сочетают в себе достижения в технологичной или основанной на оценке помощи с совместными усилиями по привлечению пациентов и поставщиков медицинских услуг к непрерывной оценке и повышению качества.Международные инновации в оценке качества включают в себя Assessment Instrument for Mental Health Systems Всемирной организации здравоохранения (ВОЗ)76 и International Initiative for Mental Health Leadership77, которая предоставляет данные об отчетности, возможности сообщать и устанавливать данные по странам.
В Голландии регулярный контроль за результатами был включен в механизмы возмещения расходов на медицинское страхование. Таким образом оцениваются три аспекта качества: эффективность лечения, безопасность и удовлетворенность клиента – посредством 10 показателей, которые оцениваются в начале и в конце лечения78. Инициатива предусматривает, что показатели собираются централизованно и публикуются прозрачно с целью стимулировать постоянное повышение качества.
В Австралии в 2000 году было принято решение об использовании стандартизированных показателей результативности для всех, кто получал помощь в области психического здоровья, и все австралийские штаты подписали соглашения о представлении регулярно собираемых данных по результатам и совокупности случаев. Основными показателями результатов являются шкала оценки здоровья нации (HoNOS) и инструмент оценки качества жизни. Для того чтобы реализовать эту инициативу в таких больших масштабах, требуются значительные инвестиции в организации, предоставляющие услуги в области психического здоровья, постоянное обучение и программа развития взаимодействия79.
В Новой Зеландии поставщики психиатрических услуг ориентированы на ключевые показатели, такие как уменьшение замкнутости и изоляции, снижение уровня самоубийств80. В Великобритании National Health Service Benchmarking Network81 – это сотрудничество между всеми организациями, оказывающими услуги в области психического здоровья, которые предоставляют данные для сравнения своих собственных показателей деятельности с другими. Сеть бенчмаркинга была разработана из-за предполагаемой неадекватности национальной системы сбора данных и отсутствия обратной связи по большому объему собранных данных. Как инициатива «на местах», сеть бенчмаркинга требует активного участия и динамичного руководства.
В США предпринимаются национальные усилия по определению междисциплинарных показателей оценки качества психиатрической помощи и определению, кто ответственен за повышение качества. В департаменте по делам ветеранов центральным руководством установлены меры по повышению качества для реализации в более чем 160 медицинских центрах. В то время как качество психиатрической помощи в департаменте задокументировано, распространены региональные различия в процессе и результатах лечения82-86. Таким образом, с учетом того, что региональные руководители психиатрической службы ответственны за повышение качества, департамент запустил национальные инициативы по повышению качества помощи и уменьшению различий в оказании психиатрической помощи, во многом посредством разработки Единого руководства по оказанию психиатрической помощи (Uniform Mental Health Services Handbook)87 и внедрения специалистов в области психического здоровья в первичную медицинскую помощь для обеспечения интегрированной помощи. Департамент также спонсировал национальное внедрение научно обоснованной психотерапии посттравматического стрессового расстройства88.
Модели оплаты по результатам работы, также называемые «оплатой на основе воспринимаемой ценности» (это подход, при котором цена формируется на основе ценности для потребителя. – Прим. пер.)89, не менее часто пропагандируются в США и по всему миру. Такие инициативы вознаграждают организации за улучшение результатов и начинают использоваться в области психического здоровья90,91. Другие инновации включают помощь вне стен клиник, в частности оценку реабилитационных служб92 и развитие мобильного здравоохранения для сбора данных о результатах65,93. Центры услуг по программам Medicare и Medicaid в США также разворачивают инициативы, посредством которых стремятся повысить заинтересованность специалистов в применении доказательных методов и организаций, оказывающих медицинские услуги, в их поддержке. Основной целью было включение психиатрической помощи в первичное звено медицинской помощи, куда обращаются большинство пациентов с симптомами психических расстройств в начальной стадии. Согласно Breakthrough Series Института по развитию здравоохранения были применены бизнес-практики для внедрения длительного лечения депрессии в первичное звено медицинской помощи94. Кроме того, существуют и другие инновации в области интеграции психического здоровья в первичную помощь (например, исследовательская сеть системы здравоохранения, местные центры психического здоровья – система здравоохранения Чероки95), однако существует мало механизмов для расширения их масштабов и дальнейшего распространения.
В Великобритании комитет по качеству и инновациям внедряет систему оплаты за работу в области психического здоровья, в рамках которой выплаты основаны на достижении национальных целевых показателей повышения качества96. Целевые показатели устанавливаются на локальном уровне, но в соответствии с центрально установленными задачами. Тем не менее неизбежные различия в оказании медицинской помощи затрудняют разработку показателей качества в области психического здоровья.
Наконец, в настоящее время предпринимаются усилия по привлечению групп с участием многих заинтересованных сторон к обеспечению обратной связи на протяжении всего процесса разработки и внедрения оценки качества. В то время как врачи-клиницисты часто в состоянии обеспечить исходные данные для разработки способов оценки качества, получение обратной связи от потребителей и их опекунов также считается важным97. Byron и соавт.98 описывают процесс вовлечения заинтересованных сторон на всех уровнях разработки оценки качества и реализации в законе об улучшении финансирования программы медицинского страхования детей (Children’s Health Insurance Program Reauthorization Act – CHIPRA). План разработки оценки качества описывает запланированный процесс, включая привлечение заинтересованных сторон99. Национальный форум по качеству использует метод консенсуса для рассмотрения и одобрения показателей, включая время на общественное обсуждение100. Кроме того, центры услуг по программам Medicare и Medicaid недавно созвали группы экспертов, в которые включены клиницисты, статисты, эксперты по повышению качества и методисты, для разработки, отбора и утверждения показателей101.

РЕКОМЕНДАЦИИ
Мы предлагаем ряд рекомендаций по реализации оценки качества как универсальное средство для повышения качества психиатрической помощи. Во-первых, тем, кто получает, и тем, кто оказывает психиатрические услуги, потребуются утвержденные показатели оценки результатов лечения пациента по всему спектру возможных состояний, а также для особых групп населения, включая детей/подростков102. Более того, необходимы обоснованные показатели оценки доступности психиатрической помощи, чтобы оценить качество помощи вне клиники. Показатели должны быть валидны по всей триаде Донабедиана (ресурсы, процесс, результаты).Во-вторых, должны быть разработаны и внедрены общие критерии для диагнозов, клинической оценки и «витальных» признаков психического здоровья, которые также следует интегрировать с существующей электронной медицинской документацией и другими инструментами информационных технологий, такими как смартфоны. Другие компоненты, которые необходимо стандартизировать, включают кодирование в электронной учетной документации и административных базах данных медицинских вмешательств, таких данных, как медикаментозная терапия, психотерапия (включая мероприятия по оценке сообразности и применения по назначению) и другие виды терапии или ухода. Такие инновации, как обработка естественного языка или автоматизированный сбор данных из электронной медицинской документации, уже применяются для облегчения сбора данных с целью получения информации (например, данные о бездомности или суицидальном риске), которая не является очевидной.
В-третьих, результаты лечения в области психического здоровья должны оцениваться на регулярной основе, и помощь, основанная на оценке, должна быть не только внедрена в имеющиеся технологии, но и стать частью культуры лечения и здравоохранения. Было показано, что регулярная оценка результатов связана с улучшениями в оказании услуг и более низким уровнем повторных госпитализаций103, в то время как нерегулярная оценка результатов незначительно влияет на повышение качества104. Более того, регулярная оценка результатов, о которой оповещали клинициста и которая была использована для совместного с пациентом принятия решений по лечению, вела к улучшению качества жизни105. Показатели оценки качества, посредством которых можно вести мониторинг данных о качестве в режиме реального времени, необходимо применять в системах здравоохранения, чтобы содействовать повышению качества, и необходимо отслеживать непреднамеренные, неучтенные последствия.
В-четвертых, системы здравоохранения должны обеспечивать инвестиции, руководство и координацию в целях совершенствования и обеспечения связи источников данных для оценки качества в различных условиях. Здравоохранение должно будет вовлекать поставщиков и потребителей в процесс утверждения показателей качества и разработки мер, отвечающих потребностям поставщиков и потребителей, а не администрации. Слишком часто систематическая оценка качества результатов обусловлена желанием сообщить данные политикам или сократить расходы, а не стремлением улучшить качество оказываемой помощи отдельным лицам, что может иметь неблагоприятные последствия, если сотрудники (которые должны предоставлять данные) воспринимают это как отвлекающий фактор, не имеющий большого значения. Такие меры, как сеть бенчмаркинга Великобритании, являются хорошим способом внедрения этих перспектив106.
Наконец, системы здравоохранения нуждаются в действенном способе стратификации показателей качества, с тем чтобы устранить потенциальные пробелы среди субпопуляций и выявить группы, в которых наиболее необходимо повышение качества. Большое значение имеет более длительное обучение персонала и повышение его эффективности. Стратегии повышения качества и подотчетности необходимо адаптировать, разрабатывать и регулярно применять в психиатрических учреждениях.
В табл. 2 мы предлагаем масштабный многоуровневый процесс, который очерчивает препятствия оценки качества и потенциальные средства, ведущие к повышению качества107. Этот процесс, основанный на Обучающей модели организации здравоохранения Национальной академии медицины США (US National Academy of Medicine Learning Health Care System), был доработан, чтобы включить в него «рычаги», направленные на организационные барьеры в психиатрическом здравоохранении108. Обучающая модель организации здравоохранения предполагает использование существующих данных (например, электронные медицинские записи) для внедрения и оценки инноваций и новых методов среди различных организаций с целью улучшения здоровья населения.

ЗАКЛЮЧЕНИЕ
Улучшение качества психиатрической помощи – это «командный спорт», требующий координации с множеством поставщиков услуг, привлечение адвокатов по правам потребителей, привлечение ресурсов и мотивация тех, кто оплачивает медицинскую помощь и здравоохранения в целом. На рисунке представлена дорожная карта по оценке и повышению качества психиатрической помощи. Во-первых, пациенты, организации и системы здравоохранения должны вносить свой вклад в выбор показателей оценки и их внедрение. Необходимые для этого шаги включают утверждение доказательной базы для показателей оценки качества посредством клинических рекомендаций, оформление рекомендаций таким образом, чтобы показатели качества имели числитель и знаменатель, основанные на данных, которые легко получить в условиях медицинских учреждений, тестирование показателей качества на их надежность и валидность (удостоверяясь в том, что они не ведут к манипулированию), доработка показателей, одобренных пациентами, организациями и представителями здравоохранения, равно как и профессиональными организациями, адаптация показателей для применения в повседневной практике, соотношение показателей в различных условиях (например, первичная помощь, социальные услуги) и, наконец, обозначение ответственных за оценку – осуществление перманентного контроля и разработку стратегий по повышению качества в случае необходимости.Рекомендации по повышению качества психиатрической помощи, представленные здесь, можно применять в здравоохранении в целом. В действительности, область психического здоровья стала первопроходцем во множестве других инноваций в здравоохранении, таких как вовлечение общества в оказание помощи, применение инновационных моделей интегрированной помощи, равно как и пациент-ориентированных мер по реабилитации. Кроме того, на примере психиатрической помощи были изучены ошибки, которые должны быть учтены при развитии обучающей модели организации здравоохранения в других отраслях здравоохранения. Долгие годы пациенты и члены их семей боролись за пациент-ориентированную помощь и больший акцент на личные цели пациента, помимо получения медицинских услуг.
Разнородные источники оказания психиатрической помощи также усложняют здравоохранению задачу учитывать мнение и взгляды персонала, включая медсестер, социальных работников, и увеличивающееся количество аналогичных специалистов, в повышении качества. Неудивительно, что многие методы по повышению качества, использованные в психиатрической области здравоохранения, повлияли на развивающуюся область имплементационной науки (implementation science)109, которая заключается в изучении поведенческих изменений у поставщиков в контексте организационных ограничений. Наконец, развитие моделей оплаты на основе «воспринимаемой ценности», которая вознаграждает организации по оказанию медицинской помощи и поставщиков на основе достижения результатов, а не увеличения объема, является многообещающим методом повышения качества психиатрической помощи.
БЛАГОДАРНОСТИ
Данная работа выполнена при поддержке Department of Veterans Affairs, Veterans Health Administration, the Irving Institute, и National Institutes of Health (R01 MH 099898). Дополнительная поддержка была оказана Commonwealth Fund (грант № 20141104) и National Center for Advancing Translational Sciences, National Institutes of Health (грант № UL1 TR000040). В работе представлены взгляды авторов, которые не обязательно отражают позицию Department of Veterans Affairs, the National Institutes of Health или других организаций.
DOI: 10.1002/wps.20482
Список исп. литературыСкрыть список1. Vigo D, Thornicroft G, Atun R. Estimating the true global burden of mental illness. Lancet Psychiatry 2016;3:171-8.
2. De Hert M, Correll CU, Bobes J et al. Physical illness in patients with severe mental disorders. I. Prevalence, impact of medications and disparities in health care. World Psychiatry 2011;10:52-77.
3. Goldberg D. The detection and treatment of depression in the physically ill. World Psychiatry 2010;9:16-20.
4. Lin EH, Rutter CM, Katon W et al. Depression and advanced complications of diabetes: a prospective cohort study. Diabetes Care 2010; 33:264-9.
5. Walker ER, McGee RE, Druss BG. Mortality in mental disorders and global disease burden implications: a systematic review and metaanalysis. JAMA Psychiatry 2015;72:334-41.
6. Carson N, Vesper A, Chen C et al. Quality of follow-up after hospitalization for mental illness among patients fr om racial-ethnic minority groups. Psychiatr Serv 2014;65:888-6.
7. Cook BL, Zuvekas SH, Carson N et al. Assessing racial/ethnic disparities in treatment across episodes of mental health care. Health Serv Res 2014;49:206-29.
8. Coleman KJ, Stewart C, Waitzfelder BE et al. Racial-ethnic differences in psychiatric diagnoses and treatment across 11 health care systems in the Mental Health Research Network. Psychiatr Serv 2016;67:749-57.
9. Case A, Deaton A. Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century. Proc Natl Acad Sci USA 2015;112:15078-83.
10. Parks J, Svendsen D, Singer P et al. Morbidity and mortality in people with serious mental illness. Alexandria: National Association of State Mental Health Program Directors, 2006.
11. Liu NH, Daumit GL, Dua Tet al. Excess mortality in persons with severe mental disorders: a multilevel intervention framework and priorities for clinical practice, policy and research agendas.World Psychiatry 2017;16:30-40.
12. Demyttenaere K, Bruffaerts R, Posada-Villa J et al. Prevalence, severity, and unmet need for treatment of mental disorders in the World Health Organization World Mental Health Surveys. JAMA 2004;291:2581-90.
13. Esposito E, Wang JL, Adair CE et al. Frequency and adequacy of depression treatment in a Canadian population sample. Can J Psychiatry 2007;52:780-9.
14. Harris MG, Hobbs MJ, Burgess PM et al. Frequency and quality of mental health treatment for affective and anxiety disorders among Australian adults. Med J Aust 2015;202:185-9.
15. Lopes CS, Hellwig N, de Azevedo e Silva G et al. Inequities in access to depression treatment: results of the Brazilian National Health Survey – PNS. Int J Equity Health 2016;15:154.
16. Lu CY, Roughead E. New users of antidepressant medications: first episode duration and predictors of discontinuation. Eur J Clin Pharmacol 2012;68:65-71.
17. Wang PS, Aguilar-Gaxiola S, Alonso J et al. Use of mental health services for anxiety, mood, and substance disorders in 17 countries in the WHO World Mental Health Surveys. Lancet 2007;370:841-50.
18. Whiteford HA, Degenhardt L, Rehm J et al. Global burden of disease attributable to mental and substance use disorders: findings fr om
the Global Burden of Disease Study 2010. Lancet 2013;382:1575-
86.
19. Donabedian A. Evaluating the quality of medical care. Milbank Q 2005;83:691-729.
20. Donabedian A. The quality of care: how can it be assessed? JAMA 1988;260:1743-8.
21. Kilbourne AM, Fullerton C, Dausey D et al. A framework for measuring quality and promoting accountability across silos: the case of mental disorders and co-occurring conditions. Qual Saf Health Care 2010;19:113-6.
22. US Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Washington: National Academies Press, 2001.
23. US Institute of Medicine. Improving the quality of health care for mental and substanceuse conditions. Washington: National Academies Press, 2006.
24. Hayes JF, Marston L, Walters K et al. Mortality gap for people with bipolar disorder and schizophrenia: UK-based cohort study 2000–2014. Br J Psychiatry 2017;211:175-81.
25. Wang PS, Demler O, Kessler RC. Adequacy of treatment for serious mental illness in the United States. Am J Publ Health 2002;92:92-8.
26. Pincus HA, Scholle SH, Spaeth-Rublee B et al. Quality measures for mental health and substance use: gaps, opportunities, and challenges. Health Aff 2016;35:1000-8.
27. US National Committee for Quality Assurance. The state of health care quality, 2016. Washington: National Committee for Quality Assurance, 2016.
28. Harris AHS, Gupta S, Bowe T et al. Predictive validity of two process-of-care quality measures for residential substance use disorder treatment. Addict Sci Clin Pract 2015;10:22.
29. Schmidt EM, Gupta S, Bowe T et al. Predictive validity of outpatient follow-up after detoxification as a quality measure. J Addict Med 2017;11:205-10.
30. Watkins KE, Paddock SM, Hudson TJ et al. Association between process measures and mortality in individuals with opioid use disorders. Drug Alcohol Depend 2017;177:307-14.
31. Watkins KE, Paddock SM, Hudson TJ et al. Association between quality measures and mortality in individuals with co-occurring mental health and substance use disorders. J Subst Abuse Treat 2016;69:1-8.
32. Schmidt EM, Gupta S, Bowe T et al. Predictive validity of a quality measure for intensive substance use disorder treatment. Subst Abus 2017;38:317-23.
33. Bremer RW, Scholle SH, Keyser D et al. Pay for performance in behavioral health. Psychiatr Serv 2008;59:1419-29.
34. Dausey DJ, Pincus HA, Herrell JM. Performance measurement for co-occurring mental health and substance use disorders. Subst Abuse Treat Prev Policy 2009;4:18.
35. Hepner KA, Watkins KE, Farmer CM et al. Quality of care measures for the management of unhealthy alcohol use. J Subst Abuse Treat 2017;76:11-7.
36. Kilbourne AM, Keyser D, Pincus HA. Challenges and opportunities in measuring the quality of mental health care. Can J Psychiatry 2010;55:549-57.
37. Martsolf GR, Osilla KC, Mandel D et al. Assessing the quality and value of psychological health care in civilian health plans: lessons and implications for the Military Health System. Rand Health Q 2016;5:16.
38. Watkins K, Horvitz-Lennon M, Caldarone LB, et al. Developing medical record-based performance indicators to measure the quality of mental healthcare. J Health Qual 2011;33:49-66.
39. Watkins KE, Keyser DJ, Smith B et al. Transforming mental healthcare in the Veterans Health Administration: a model for measuring performance to improve access, quality, and outcomes. J Health Qual 2010;32:33-42.
40. Wagner EH, Austin BT, Von Korff M. Organizing care for patients with chronic illness. Milbank Q 1996;74:511-44.
41. Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. JAMA 2002;288:1775-9.
42. Woltmann E, Grogan-Kaylor A, Perron B et al. Comparative effectiveness of collaborative chronic care models for mental health conditions across primary, specialty, and behavioral health care settings: systematic review and meta-analysis. Am J Psychiatry 2012;169:790-804.
43. Pincus HA, Jun M, Franx G et al. How can we link general medical and behavioral health care? International models for practice and policy. Psychiatr Serv 2015;66:775-7.
44. Richards DA, Bower P, Pagel C et al. Delivering stepped care: an analysis of implementation in routine practice. Implement Sci 2012;7:3.
45. Goorden M, Huijbregts KML, van Marwijk HWJ et al. Cost-utility of collaborative care for major depressive disorder in primary care in the Netherlands. J Psychosom Res 2015;79:316-23.
46. Morgan MAJ, Coates MJ, Dunbar JA et al. The TrueBlue model of collaborative care using practice nurses as case managers for depression alongside diabetes or heart disease: a randomised trial. BMJ Open 2013;3:e002171.
47. NHS England. Adult mental health: common mental health problems. Implementing the five year forward view for mental health. London: NHS England, 2016.
48. Hatfield D, McCullough L, Frantz SH et al. Do we know when our clients get worse? An investigation of therapists’ ability to detect negative client change. Clin Psychol Psychother 2010;17:25-32.
49. Zimmerman M, McGlinchey JB. Why don’t psychiatrists use scales to measure outcome when treating depressed patients? J Clin Psychiatry 2008;69:1916-9.
50. Trivedi MH, Rush AJ, Wisniewski SR et al. Evaluation of outcomes with citalopram for depression using measurement-based care in STAR*D: implications for clinical practice. Am J Psychiatry 2006;163:28-40.
51. Oslin DW, Ross J, Sayers S et al. Screening, assessment, and management of depression in VA primary care clinics: the Behavioral Health Laboratory. J Gen Intern Med 2006;21:46-50.
52. Tew J, Klaus J, Oslin DW. The Behavioral Health Laboratory: building a stronger foundation for the patient-centered medical home. Fam Syst Health 2010;28:130-45.
53. US Department of Defense. Plan for development of procedure to measure data on mental health care provided by the Department of Defense. Washington: US Department of Defense, 2016.
54. US Institute for Clinical Systems Improvement. The DIAMOND program: treatment for patients with depression in primary care. Bloomington: US Institute for Clinical Systems Improvement, 2016.
55. US Centers for Medicare & Medicaid Services. Value-based payment modifier. Baltimore: US Centers forMedicare & Medicaid Services, 2017.
56. Zivin K, O’Malley A, Bigby J et al. Behavioral health integration in primary care: a review and implications for payment reform. Mathematica Policy Research, 2016.
57. Seibert J, Fields S, Fullerton CA et al. Use of quality measures for Medicaid behavioral health services by state agencies: implications for health care reform. Psychiatr Serv 2015;66:585-91.
58. US Centers for Medicare & Medicaid Services. Physician compare. Baltimore: US Centers for Medicare & Medicaid Services, 2017.
59. US Centers for Medicare & Medicaid Services. Hospital compare. Baltimore: US Centers for Medicare & Medicaid Services, 2017.
60. Patel MM, Brown JD, Croake S, et al. The current state of behavioral health quality measures: wh ere are the gaps? Psychiatr Serv 2015; 66:865-71.
61. US Centers for Medicare & Medicaid Services. Inpatient Psychiatric Facilities Quality Reporting (IPFQR) Program. Baltimore: US Centers for Medicare & Medicaid Services, 2017.
62. US Institute of Medicine. Psychosocial interventions for mental and substance use disorders: a framework for establishing evidence based standards. Washington: National Academies Press, 2015.
63. Gaynes B, Brown C, Lux LJ et al. Relationship between use of quality measures and improved outcomes in serious mental illness. Rockville: US Agency for Healthcare Research and Quality, 2015.
64. US Substance Abuse and Mental Health Services Administration. Recovery and recovery support. Rockville: US Substance Abuse and Mental Health Services Administration, 2015.
65. Ranallo PA, Kilbourne AM, Whatley AS et al. Behavioral health information technology: from chaos to clarity. Health Aff 2016;35:1106-13.
66. Druss BG, Dimitropoulos L. Advancing the adoption, integration and testing of technological advancements within existing care systems. Gen Hosp Psychiatry 2013;35:345-8.
67. Riahi S, Fischler I, Stuckey MI et al. The value of electronic medical record implementation in mental health care: a case study. JMIR Med Inform 2017;5:e1.
68. Yeomans D. Clustering in mental health payment by results: a critical summary for the clinician. Adv Psychiatr Treat 2014;20:227-34.
69. UK Royal College of Psychiatrists. Royal College of Psychiatrists’ statement on mental health Payment Systems (formerly Payment by Results). London: UK Royal College of Psychiatrists, 2014.
70. Wang R, Shaw I, Middleton H. Delaying the implementation of Payment by Results in mental health: the application of standardisation. Ment Health Rev 2015;20:156-65.
71. McShane M, Mitchell E. Person centred coordinated care: wh ere does the QOF point us? BMJ 2015;350:h2540.
72. Harding KJ, Rush AJ, Arbuckle M et al. Measurement-based care in psychiatric practice: a policy framework for implementation. J Clin Psychiatry 2011;72:1136-43.
73. Fortney JC, Unützer J, Wrenn G et al. A tipping point for measurement-based care. Psychiatr Serv 2017;68:179-88.
74. Insel TR. Translating scientific opportunity into public health impact: a strategic plan for research on mental illness. Arch Gen Psychiatry 2009;66:128-33.
75. US Department of Veterans Affairs. VA is working to end homelessness among veterans. Washington: US Department of Veterans Affairs, 2017.
76. World Health Organization. WHO-AIMS mental health systems in selected low-income and middle-income countries: a WHO-AIMS cross-national analysis. Geneva: World Health Organization, 2009.
77. International Initiative for Mental Health Leadership. IIMHL and IIDL Annual report. Lambton Quay: International Initiative for Mental Health Leadership, 2016.
78. Dutch Association of Mental Health and Addiction Care. Performance indicators mental health care in the Netherlands. www. ggznederland.nl
79. Burgess P, Coombs T, Clarke A et al. Achievements inmental health outcome measurement in Australia: reflections on progress made by the Australian Mental Health Outcomes and Classification Network (AMHOCN). Int J Ment Health Syst 2012;6:4.
80. New Zealand Mental Health and Addictions KPI Programme. KPI Dashboard for financial years 2013/14 to 2016/17 YTD (Jul-Dec). www.mhakpi.health.nz
81. UK National Health Service Benchmarking Network. Work programme report 2016/17. Manchester: UK National Health Service, 2017.
82. Hussey PS, Ringel JS, Ahluwalia S, et al. Resources and capabilities of the Department of Veterans Affairs to provide timely and accessible care to veterans. Rand Health Q 2016;5:14.
83. Shields M, Rosenthal M. Quality of inpatient psychiatric care at VA, other government, nonprofit, and for-profit hospitals: a comparison. Psychiatr Serv 2017;68:225-30.
84. O’Hanlon C, Huang C, Sloss E et al. Comparing VA and non-VA quality of care: a systematic review. J Gen Intern Med 2017;32:105-21.
85. Watkins KE, Smith B, Akincigil A et al. The quality of medication treatment for mental disorders in the Department of Veterans Affairs and in private-sector plans. Psychiatr Serv 2016;67:391-6.
86. Hepner KA, Paddock SM, Watkins KE et al. Veterans’ perceptions of behavioral health care in the Veterans Health Administration: a national survey. Psychiatr Serv 2014;65:988-96.
87. US Department of Veterans Affairs. Uniform Mental Health Services in VA Medical Centers and Clinics. Washington: US Department of Veterans Affairs, 2008.
88. Sayer NA, Rosen CS, Bernardy NC et al. Context matters: team and organizational factors associated with reach of evidence-based psychotherapies for PTSD in the Veterans Health Administration. Adm Policy Ment Health 2017; 44:904-18.
89. Roland M, Guthrie B. Quality and outcomes framework: what have we learnt? BMJ 2016; 354:i4060.
90. Bao Y, McGuire TG, Chan YF et al. Value-based payment in implementing evidence-based care: the Mental Health Integration Program in Washington state. Am J Manag Care 2017;23:48-53.
91. Unützer J, Chan Y-F, Hafer E et al. Quality improvement with pay-for-performance incentives in integrated behavioral health care. Am J Publ Health 2012;102:e41-5.
92. Pincus HA, Spaeth-Rublee B, Sara G et al. A review of mental health recovery programs in selected industrialized countries. Int J Ment Health Syst 2016;10:73.
93. Price M, Yuen EK, Goetter EM et al. mHealth: a mechanism to deliver more accessible, more effective mental health care. Clin Psychol Psychother 2014;21:427-36.
94. US Institute for Health Care Improvement. The Breakthrough Series: IHI’s collaborative model for achieving breakthrough improvement. Cambridge: US Institute for Healthcare Improvement, 2003.
95. Agency for Healthcare Research and Quality. Cherokee health systems. www.integrationacademy. ahrq.gov
96. Ramanuj PP, Breslau J, Strathdee G et al. Carrots and sticks on opposite sides of the Atlantic: integration incentives for people with serious mental illness in England. Psychiatr Serv 2016;68:430-2.
97. US Institute of Medicine. Quality measurement. Psychosocial interventions for mental and substance use disorders: a framework for establishing evidence-based standards.Washington: National Academies Press, 2015.
98. Byron SC, Gardner W, Kleinman LC et al. Developing measures for pediatric quality: methods and experiences of the CHIPRA Pediatric Quality Measures Program grantees. Acad Pediatr 2014;14(Suppl. 5):S27-32.
99. US Centers for Medicare & Medicaid Services. CMS quality measure development plan: supporting the transition to theMerit-based Incentive Payment System (MIPS) and Alternative Payment Models (APMs). Baltimore: Centers for Medicare & Medicaid Services, 2016.
100. US National Quality Forum. Consensus development process. www.qualityforum.org
101. US Centers for Medicare & Medicaid Services. Technical expert panels. Baltimore: US Centers for Medicare & Medicaid Services, 2017.
102. Hall CL, Moldavsky M, Taylor J et al. Implementation of routine outcome measurement in child and adolescent mental health services in the United Kingdom: a critical perspective. Eur Child Adolesc Psychiatry 2014;23:239-42.
103. Slade M, McCrone P, Kuipers E et al. Use of standardised outcome measures in adult mental health services: randomised controlled trial. Br J Psychiatry 2006;189:330-6.
104. Ashaye OA, Livingston G, Orrell MW. Does standardized needs assessment improve the outcome of psychiatric day hospital care for older people? A randomized controlled trial. Aging Ment Health 2003;7:195-9.
105. Priebe S, McCabe R, Bullenkamp J et al. The impact of routine outcome measurement on treatment processes in community mental health care: approach and methods of the MECCA study. Epidemiol Psychiatr Soc 2002; 11:198-205.
106. NHS Scotland. Mental health project final report. Edinburgh: Scottish Government, 2008.
107. Pincus HA, Hough L, Houtsinger JK et al. Emerging models of depression care: multilevel (‘6 P’) strategies. Int J Methods Psychiatr Res 2003;12:54-63.
108. US Institute of Medicine. Best care at lower cost: the path to continuously learning health care in America. Washington: National Academies Press, 2013.
109. Chambers DA, Feero WG, Khoury MJ. Convergence of implementation science, precision medicine, and the learning health care system: a new model for biomedical research. JAMA 2016;315:1941-2.


