Психиатрия Всемирная психиатрия
Психиатрия Всемирная психиатрия
№02 2016
Сахарный диабет при шизофрении, биполярном расстройстве, большом депрессивном расстройстве: систематический обзор и крупномасштабный мета-анализ №02 2016
Номера страниц в выпуске:166-174
Сахарный диабет II типа (СД2Т) значительно повышает риск развития сердечно-сосудистых заболеваний и может пагубно влиять на здоровье людей с тяжелыми психическими расстройствами (ТПР), т. е. шизофренией, биполярным расстройством или большим депрессивным расстройством. Целями данного мета-анализа стали: а) описание частотности СД2Т у людей с ТПР б) анализ влияния демографических факторов, особенностей болезни и лечения, а также методов оценки риска СД2Т в) описание уровня заболеваемости СД2Т на основании исследований, сравнивающих людей с определенными ТПР и популяцию в целом. Распространенность СД2Т, скорректированная методом обрезки и заполнения (trim and fill), на выборке из 438245 человек с ТПР составила 11,3% (95% CI: 10.0%-12.6%). У не принимавших антипсихотики пациентов распространенность СД2Т составила 2.9% (95% CI: 1.7%-4.8%). Значительной разницы в диагностических подгруппах выявлено не было. Сравнительный мета-анализ установил, что у людей с множественными эпизодами ТПР (N=133,470) вероятность СД2Т значительно выше, чем у соответствующей контрольной группы (N=5,622,664): относительный риск, RR=1.85, 95% CI: 1.45-2.37, p<0.001. Распространенность СД2Т достоверно выше в каждой из трех главных диагностических подгрупп в сравнении с соответствующей контрольной группой. СД2Т у женщин с ТПР встречается чаще, чем у мужчин (RR=1.43, 95% CI: 1.20-1.69, p<0.001). Мультивариантный мета-регрессионный анализ показал, что единственным значительным фактором повышения риска СД2Т являются множественные эпизоды ТПР в сравнении с первым эпизодом заболевания (r2=0.52, p<0.001). Распространенность СД2Т выше среди пациентов, принимающих антипсихотики, за исключением арипипразола и амисульприда. Для лечения и диагностики СД2Т необходимы регулярный скрининг и мультидисциплинарный подход. При выборе терапевтической стратегии следует принимать во внимание риск возникновения СД2Т при лечении определенными антипсихотиками.
Ключевые слова: Сахарный диабет, тяжелое психическое расстройство, шизофрения, биполярное расстройство, большое депрессивное расстройство, антипсихотики
(World Psychiatry 2016; 15: 166–174)
Ключевые слова: Сахарный диабет, тяжелое психическое расстройство, шизофрения, биполярное расстройство, большое депрессивное расстройство, антипсихотики
(World Psychiatry 2016; 15: 166–174)
Сахарный диабет II типа (СД2Т) значительно повышает риск развития сердечно-сосудистых заболеваний и может пагубно влиять на здоровье людей с тяжелыми психическими расстройствами (ТПР), т. е. шизофренией, биполярным расстройством или большим депрессивным расстройством. Целями данного мета-анализа стали: а) описание частотности СД2Т у людей с ТПР б) анализ влияния демографических факторов, особенностей болезни и лечения, а также методов оценки риска СД2Т в) описание уровня заболеваемости СД2Т на основании исследований, сравнивающих людей с определенными ТПР и популяцию в целом. Распространенность СД2Т, скорректированная методом обрезки и заполнения (trim and fill), на выборке из 438245 человек с ТПР составила 11,3% (95% CI: 10.0%-12.6%). У не принимавших антипсихотики пациентов распространенность СД2Т составила 2.9% (95% CI: 1.7%-4.8%). Значительной разницы в диагностических подгруппах выявлено не было. Сравнительный мета-анализ установил, что у людей с множественными эпизодами ТПР (N=133,470) вероятность СД2Т значительно выше, чем у соответствующей контрольной группы (N=5,622,664): относительный риск, RR=1.85, 95% CI: 1.45-2.37, p<0.001. Распространенность СД2Т достоверно выше в каждой из трех главных диагностических подгрупп в сравнении с соответствующей контрольной группой. СД2Т у женщин с ТПР встречается чаще, чем у мужчин (RR=1.43, 95% CI: 1.20-1.69, p<0.001). Мультивариантный мета-регрессионный анализ показал, что единственным значительным фактором повышения риска СД2Т являются множественные эпизоды ТПР в сравнении с первым эпизодом заболевания (r2=0.52, p<0.001). Распространенность СД2Т выше среди пациентов, принимающих антипсихотики, за исключением арипипразола и амисульприда. Для лечения и диагностики СД2Т необходимы регулярный скрининг и мультидисциплинарный подход. При выборе терапевтической стратегии следует принимать во внимание риск возникновения СД2Т при лечении определенными антипсихотиками.
Ключевые слова: Сахарный диабет, тяжелое психическое расстройство, шизофрения, биполярное расстройство, большое депрессивное расстройство, антипсихотики
(World Psychiatry 2016; 15: 166–174)
У людей с тяжелыми психическими расстройствами (ТПР) – шизофренией, биполярным расстройством или большим депрессивным расстройством (БДР) – риск преждевременной смерти в 2-3 раза выше, чем в целом в популяции1,2. Разрыв в смертности означает, что ожидаемая продолжительность жизни сокращается на 10-20 лет3,4, и этот разрыв продолжает расширяться5. Наиболее важной причиной сокращения ожидаемой продолжительности жизни являются сердечно-сосудистые заболевания (ССЗ)6. К основным факторам риска относится прием антипсихотических препаратов и нездоровый образ жизни7, и эти риски возрастают из-за затруднений в доступе к медицинской помощи8-12.
СД2Т – серьезный фактор риска ССЗ. Он приводит к двукратному повышению риска возникновения ишемической болезни сердца, различных видов инсультов и смерти, связанной с другими заболеваниями кровеносных сосудов13,14. Предупреждение и лечение СД2Т требуют особого внимания в клинической практике, в особенности в популяции с повышенным риском ССЗ и преждевременной смерти15,16.
Недавно вышедшие мета-анализы17-20 показали, что во всех диагностических подгруппах ТПР риск СД2Т выше, чем в целом в популяции. Однако, на данный момент недостаточно данных о мета-аналитическом сравнении рисков возникновения СД2Т у пациентов с различными психиатрическими диагнозами. Кроме того, нет мета-аналитических данных, в которых объединены все основные диагностические подгруппы ТПР, а информации о заболеваемости СД2Т среди людей с ТПР, принимающих различные антипсихотические препараты, недостаточно.
Масштабные исследования групп с ТПР могут считаться достоверными, если факторы риска изучаются на материале большого количества исследований и участников, с разделением факторов риска СД2Т, как связанных с ТПР, так и независящих от этих заболеваний. Объединение данных по основным диагностическим категориям позволяет изучить эффект демографических переменных (пол, возраст, продолжительность болезни, условия проведения исследования, географическое расположение) и лекарств (в особенности нормотимиков и антипсихотиков, назначенных при психотических и непсихотических состояниях). Если в результате проведенной работы будет выявлено различие в рисках, эта информация может быть использована врачами при планировании диагностики и лечения.
Учитывая вышеупомянутые пробелы в литературных данных, мы предприняли попытку составить крупномасштабный обзор и мета-анализ распространенности СД2Т у людей с шизофренией и подобными психотическими расстройствами, биполярным расстройством или БДР. В наши цели входило: а) определить частотность СД2Т у людей с ТПР б) проанализировать влияние демографии, характера болезни и лечения, а также методов оценки СД2Т в) определить распространенность СД2Т на основании результатов исследований, в которых напрямую сравниваются люди с ТПР и популяция в целом.
Критерии включения и исключения
Данный систематический обзор был проведен в соответствии с руководствами “Мета-анализ обсервационных исследований в эпидемиологии” (MOOSE)21 и стандартом “Предпочтительные параметры отчетности для систематических обзоров и мета-анализа” (PRISMA)22.
В обзор были включены наблюдательные (поперечные, ретроспективные и проспективные) и рандомизированные контролируемые исследования взрослых с шизофренией или подобными психотическими расстройствами, биполярным расстройством или БДР в соответствии с DSM-IV-TR или МКБ-10, вне зависимости от обстоятельств лечения (стационар, амбулатория, смешанный тип), содержащие данные о распространенности СД2Т.
Нами были исключены исследования, содержащие критерии включения/исключения, касающиеся наличия или отсутствия ССЗ. При необходимости мы связывались с авторами, чтобы подтвердить релевантность исследований и получить данные, которые были нужны для нашего анализа, но не были приведены в тексте публикации.
Критерии поиска, отбора и оценки исследований
Два ревьюера (DV, BS) независимо друг от друга проводили поиск в базах данных Medline, Psyc-ARTICLES, Embase и CINAHL за период до 1 августа 2015 г., без ограничений по языку. Для поиска были использованы следующие ключевые слова: “диабет” ИЛИ “глюкоза” И “тяжелое психическое расстройство” ИЛИ “острое психическое расстройство” ИЛИ “шизофрения” ИЛИ “психоз” ИЛИ “биполярное расстройство” ИЛИ “депрессия” ИЛИ “депрессивное расстройство” в названии статьи, аннотации или терминах для индексации (ключевых словах). Использовался также ручной поиск по спискам ссылок из обозреваемых работ и недавних систематических обзоров.
После исключения повторяющихся статей авторы обзора просмотрели названия и аннотации всех потенциально подходящих статей. В соответствии с критериями отбора, на основании консенсуса был составлен список статей. Затем оба автора обзора, рассмотрев полное содержание статей, на основании консенсуса составили окончательный список. К процессу в качестве посредника привлекался третий автор (СС). Методологическая экспертиза включала в себя оценку систематических ошибок (искажение результатов, дублирование данных, предпочтительная публикация положительных результатов).
Статистический анализ
Из-за предполагаемой гетерогенности, был проведен мета-анализ случайных эффектов. Гетерогенность была измерена с помощью Q-статистики (которая всегда приводится в конце описания результатов как второе или финальное значение p).
Мы рассчитали относительный риск (RR) для оценки распространенности СД2Т в подгруппах ТПР и сравнения на основании тех исследований, в которых это сравнение проводилось. Кроме того, мы сравнили распространенность СД2Т у людей с шизофренией, биполярным расстройством и БДР с контрольной группой, подходящей по возрасту и полу, также с использованием результатов исследований, в которых это сравнение проводилось. При проведении обоих анализов использовались только те сравнения групп ТПР или сравнения группы ТПР с популяцией в целом, которые проводились в рамках одного и того же исследования, чтобы свести к минимуму вариативность показателей распространенности СД2Т, возникающую из-за разницы в выборках и методиках проведения исследований.
Затем мы применили ко всему набору данных анализ по подгруппам, чтобы выявить разницу между тремя главными диагностическими подгруппами, между пациентами с множественными эпизодами и пациентами с первым эпизодом, мужчинами и женщинами, популяционными (population-based) и непопуляционными (non-population based) исследованиями, между классами препаратов (антипсихотики, антидепрессанты, нормотимики), географическими регионами. Чтобы снизить гетерогенность, мы не проводили расчет диагностических и половых различий в исследованиях, а выбрали данные из исследований, в которых проводилось сравнение пациентов по этим параметрам. Затем мы провели мета-регрессионный анализ, чтобы выявить потенциальные факторы риска (возраст, процент мужчин, продолжительность болезни, распространенность курения. методы оценки СД2Т) с помощью программы Comprehensive Meta Analysis (версия 3).
Проверка на систематические публикационные ошибки (publication bias) была проведена с помощью регрессии Эггера23 и теста Бэгг-Мазумдар24, при значении p меньше 0,5 предполагалось наличие ошибки. Встречаясь с систематической публикационной ошибкой, мы применяли метод согласования и заполнения(trim and fill)25, чтобы убрать исследования с наименьшим количеством участников с позитивной стороны воронкообразного графика и повторно пересчитать величину эффекта, пока график не станет симметричным относительно (нового) размера эффекта.
Результаты поиска и участники
После исключения дубликатов и нерелевантных статей мы отобрали 323 публикации, из которых 118 (включающих 135 источников о распространенности СД2Т) соответствовали установленным критериям (Рисунок 1). По запросу автор может предоставить перечень включенных и исключенных исследований (с объяснением причин включения или исключения).
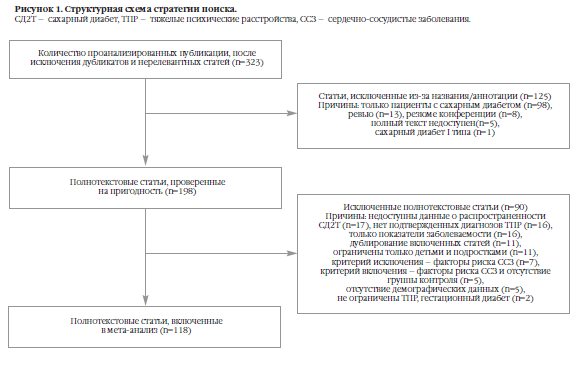
Окончательная выборка составила 438245 человек с ТПР и 5622664 человек в группе контроля. Размер выборок варьировался от 12 до 143943 участников, с медианным размером 270 человек. Средний возраст участников с ТПР – 44,3 года (от 23,1 до 77,6 лет); 56.8% – мужчины (разброс 0-100); 69% – белой расы (разброс 0-100; 37 исследований). Средняя продолжительность болезни – 16,1 лет (от 0 до 35 лет; 29 исследований). В 31 исследовании (N=77,028) сообщалось о распространенности курения, 44.5% (95% CI: 29.2%-60.4%) участников курили.
Заболеваемость СД2Т
Средняя взвешенная распространенность СД2Т среди 438245 человек с ТПР – 10.2% (95% CI: 9.1%-11.4%; Q=14228.7, p<0.001). Тест Бэгг-Мазумдара (Kendall’s tau=0.15, p=0.009) и тест Эггера (bias= -5.39, 95% CI: -7.33 to -3.45, p<0.001) показали наличие публикационной ошибки. После применения метода согласования и заполнения для коррекции 13 исследований, распространенность СД2Т составила 11.3% (95% CI: 10.0%-12.6
Анализ подгрупп и предикторов развития СД2Т
Параметры и тип исследования
Суммарная распространенность при различных режимах лечения (стационар, амбулатория, внебольничные пациенты, смешанные условия), типах исследования (поперечные, ретроспективные и проспективные исследования, популяционные и непопуляционные), медианном годе сбора данных (до или после 2000 г.), методах выявления СД2Т (анализ крови, сообщение пациента, медкарта) приведена в Таблице 1. Раздельные мета-регрессии приведены в Таблице 2.
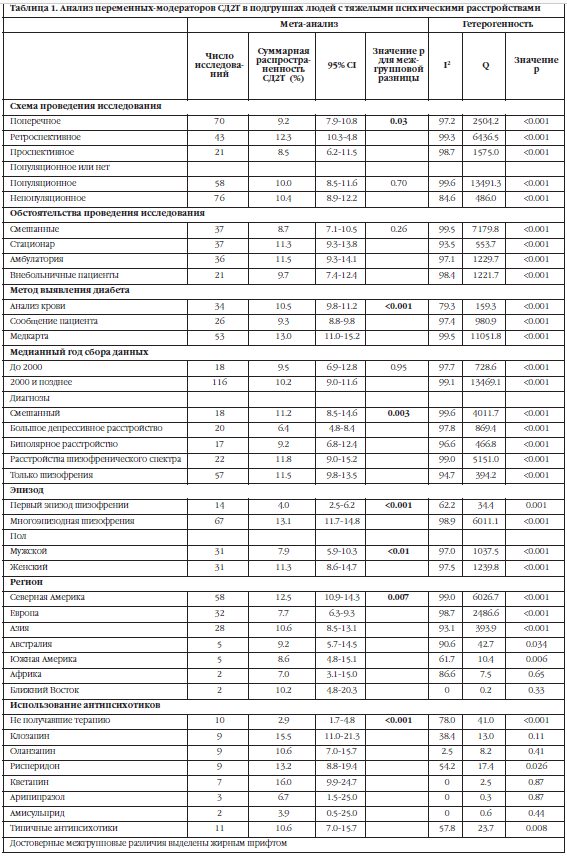
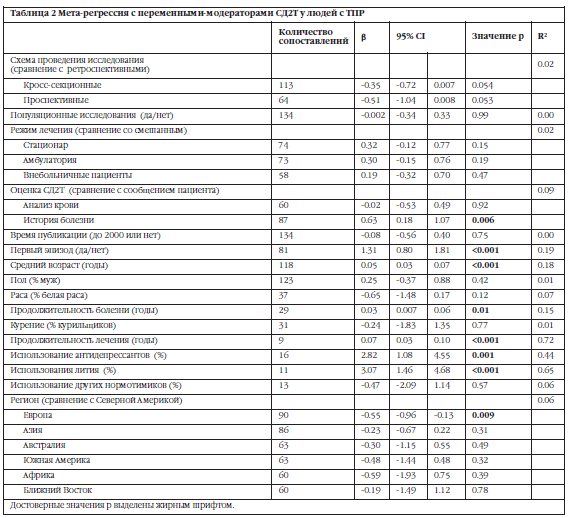
Различия в режимах лечения и времени сбора данных не отразились на результатах. Также распространенность СД2Т не зависит от того является исследование популяционным или нет. С другой стороны, в исследованиях, основанных на данных из медкарт, распространенность СД2Т выше, чем в исследованиях, основанных на сообщениях пациента. Тенденция к увеличению распространенности СД2Т была найдена в ретроспективных исследованиях в сравнении с поперечными (p=0.054) и проспективными (p=0.053) исследованиями.
Диагностические подгруппы
Суммарная распространенность СД2Т в различных диагностических подгруппах представлена в Таблице 1. Мета-анализы относительного риска выявили отсутствие значительной разницы по СД2Т в исследованиях, непосредственно сравнивающих только шизофрению (14.1%, 95% CI:9.8%-20.2%; Q=5, p=0.51; N=4,963) с расстройствами шизофренического спектра (включая шизоаффективное расстройство, шизофреноформное расстройство и связанные психозы) (18.3%, 95% CI:14.9%-22.2%; Q=2.1, p=0.34; N=694) (три исследования; отношение шансов, OR=0.80; 95% CI: 0.52-1.25, z= -0.97, p=0.33; Q=2.66, p=0.26, I2=24.9).
То же самое верно для сравнения шизофрении (13.7%, 95% CI: 8.2%-22.1%; Q=131, p<0.01; N=6,005) с биполярным расстройством (13.7%, 95% CI: 9.2%-20.0%; Q=46, p<0.01; N=3,138) (шесть исследований; OR=1.22, 95% CI: 0.84-1.77, z=1.08, p=0.28; Q=17.1, p=0.004, I2=70.8); и шизофрении (13.7%, 95% CI: 11.6%-16.1%; Q=0.3, p=0.58; N=893) с БДР (11.1%, 95% CI: 9.2%-13.3%; N=911) (два исследования; OR=1.27, 95% CI: 0.96-1.68, z=1.66, p=0.10; Q=6.0, p=0.80, I2=0). Исследований, непосредственно сравнивающих распространенность СД2Т у пациентов с биполярным расстройством и БДР, было недостаточно для анализа .
Сравнение показателей СД2Т у пациентов с множественными эпизодами и у пациентов с первым эпизодом внутри разных диагностических подгрупп (см Табл. 1) показало, что среди пациентов с первым эпизодом шизофрении (4.0%, 95%CI: 2.5%-6.2%) распространенность СД2Т значительно ниже, чем у пациентов с множественными эпизодами (13.1%, 95% CI:11.7%-14.8%, z523.89, p<0.001). Отсутствие данных о пациентах с первым эпизодом биполярного расстройства или БДР помешало провести подобное сравнение в этих диагностических подгруппах.
Демографические переменные
Мета-анализ относительного риска в 29 исследованиях, непосредственно сравнивающих частотность СД2Т у мужчин (N=35,400) и женщин (N=33,283) с ТПР показал более высокую распространенность СД2Т у женщин (RR=1.43; 95% CI: 1.20-1.69, p<0.001).
Суммарная распространенность СД2Т по географическим регионам представлена в Таблице 1. Распространенность СД2Т значительно выше в Северной Америке (12.5%, 95% CI: 10.9%-14.3%; 58 исследований), чем в Европе (7.7%, 95% CI: 6.3%-9.3%; 32 исследования) (p<0.001). Других существенных географических различий не выявлено.
Раздельный мета-регрессионный анализ (см Табл. 2) показал, что более высокая частотность СД2Т обусловлена старшим возрастом, большей длительностью болезни, первым эпизодом (а не множественными эпизодами), но не полом, расой и статусом в отношении курения.
Когда все значительные демографические предикторы были введены в многовариантную мета-регрессионную модель, множественные эпизоды в сравнении с первым эпизодом (β=1.889, 95% CI: 0.1445-3.6335, z=2.12, p=0.03) остались единственной значительной переменной-модератором вариативности СД2Т.
Окончательная многовариантная модель дает объяснение для более чем половины случаев гетерогенности в исследованиях о частотности СД2Т (r2=0.52, p<0.001)
Применение лекарств
Раздельный регрессионный мета-анализ (табл. 2) показал, что на распространенность СД2Т значительно влияет продолжительность лечения, частота назначения антидепрессантов и препаратов лития, но не других нормотимиков.
В двадцати статьях, включая 64 анализа, сообщается о монотерапии антипсихотиками и частотности СД2Т. Наименьшая распространенность СД2Т была выявлена у участников, не получавших лечение антипсихотиками (2.9%, 95% CI: 1.7%-4.8%). За исключением арипипразола и амисульприда, все антипсихотики значительно (p<0.05) повышали риск СД2Т, по сравнению с участниками, не проходившими лечение антипсихотиками (Табл. 1). За исключением повышения риска при приеме кветиапина относительно оланзапина (p=0.04), мы не обнаружили различий в уровне риска у отдельных препаратов. Риск возникновения СД2Т у пациентов, принимавших клозапин, на уровне тенденции (p=0.05) был выше в сравнении с пациентами, принимавшими оланзапин.
Относительное увеличение частоты СД2Т (RR) в диагностических подгруппах в сравнении с остальным населением
34 исследования содержат данные о распространенности СД2Т у пациентов с множественными эпизодами шизофрении в сравнении со здоровыми людьми, три исследования сравнивают пациентов с первым эпизодом шизофрении и контрольную группу. В суммарном мета-анализе относительного роста риска пациенты с множественными эпизодами ТПР (N=133,470; 12.2%, 95% CI: 9.7-15.2%; Q=6166, p<0.01) имели значительно более высокий риск СД2Т (RR=1.85, 95% CI: 1.45-2.37, p<0.001; Q=1302.0, p<0.001; 38 исследований), чем остальное население (N=5,622,664; 6.2%, 95% CI: 4.8%-8.0%; Q=18,592, p<0.01). У пациентов с первым эпизодом (4.4%, 95% CI: 2.5%-7.6%; Q=2, p=0.4) не было значительных различий в распространенности СД2Т по сравнению с контрольной группой (0.9%, 95% CI: 0.03%-2.4%; Q=3, p=0.3) (RR=4.64, 95% CI: 0.73-29.3, p=0.10; Q=1302.0, p=0.23; три исследования).
По сравнению со здоровыми людьми в контрольной группе относительное увеличение частоты СД2Т у пациентов с шизофренией или связанными психотическими расстройствами равнялось 2,04 (N=115,538; 95% CI: 1.69-2.49, p<0.001; Q=1302.0, p<0.001, I²=97.8; 29 исследований); у пациентов с биполярным расстройством – 1,89 (N=4,688; 95% CI: 1.29-2.77, p<0.001; Q=2.2, p=0.34, I²=7.3; шесть исследований), у пациентов с большим депрессивным расстройством – 1,43 (N=10,895; 95% CI: 0.88-2.25, p=0.029; Q=2.15, p=0.34; три исследования).
Распространенность СД2Т в каждой из трех диагностических подгрупп повышалась по сравнению с остальным населением одинаково, сравнительный мета-анализ не выявил значительной разницы между подгруппами с шизофренией, расстройствами шизофренического спектра, биполярным расстройством и большим депрессивным расстройством. Таким образом, на частотность СД2Т, скорее всего, влияют факторы, не связанные с диагнозом, такие как гипергликемия после приема психотропных препаратов26, нездоровый образ жизни на протяжении длительного времени27,28, а также вероятные генетические факторы, связанные как с психиатрическими, так и с общемедицинскими рисками29.
Впервые в рамках большого мета-анализа нами было показано, что риск СД2Т действительно возрастает по мере увеличения длительности лечения, подтверждение чему было также дано в мультивариантной мета-регрессионной модели, в которой уникальным значимым предиктором, объяснявшим половину дисперсии, являлись множественные эпизоды заболевания. Также мы обнаружили значительное повышение распространенности СД2Т в Северной Америке по сравнению с Европой, соответствующее уровню распространенности в общей популяции30, что предполагает комбинированное влияние генетических факторов, образа жизни и/или факторов окружающей среды.
Знание о факторах, повышающих риск СД2Т, поможет выявить тех, кто нуждается в особенно интенсивном наблюдении и лечебно-диагностических интервенциях. В отличие от остального населения, у женщин с ТПР, как мы выяснили, риск развития СД2Т выше, чем у мужчин. Это наблюдение требует дальнейших исследований, но, может быть, это связано с тем, что женщины с ТПР более склонны к общему и центральному ожирению, чем мужчины32, а центральное ожирение является важным фактором риска гипергликемии.
С другой стороны, только малая часть проанализированных исследований содержит информацию о среднем возрасте женщин и мужчин, и есть вероятность, что женщины с шизофрений были старше, что могло отразиться на результатах.
Результаты нашего исследования также показывают, что у людей с множественными эпизодами шизофрении распространенность СД2Т была выше, чем у людей с первым эпизодом. Данный мета-анализ подтверждает то, что диагноз первого эпизода является уникальным предиктором меньшей распространенности СД2Т вне зависимости от возраста, что также было выявлено в недавнем анализе распространенности метаболического синдрома у пациентов с теми же тремя основными ТПР33. Полученные результаты указывают на необходимость раннего предупреждающего вмешательства с целью уменьшить кардиометаболический риск у людей с ТПР. Потребуются дальнейшие исследования для изучения механизмов, лежащих в основе повышения риска СД2Т при переходе заболевания от начального эпизода к множественным эпизодам заболевания.
Наши данные подтверждают полученные ранее доказательства того, что прием психотропных препаратов, включая антидепрессанты, препараты лития и антипсихотики26, повышает распространенность СД2Т.
За исключением арипипразола и амисульприда, все антипсихотики связаны со значительным повышением риска СД2Т в сравнении с пациентами, не принимавшими антипсихотики. Различия в рисках возникновения отклонений уровня глюкозы описаны в литературе, при этом наивысший риск наблюдается при терапии клозапином, оланзапином и кветапином25,34,35.
В данном мета-анализе терапия кветапином (и клозапином на уровне тенденции) приводила даже к более высоким рискам возникновения СД2Т, чем терапия оланзапином. Однако, из-за того, что нельзя исключить эффекта искажения данных тогда, когда пациенты с риском СД2Т или даже с СД2Т, появившемся на фоне приема таких повышающих риск лекарств, как оланзапин, могли быть переведены на другой антипсихотик, в том числе кветапин, это наблюдение, во избежание ошибочной атрибуции, следует интерпретировать с осторожностью.
Наконец, как и ожидалось, самый низкий показатель распространенности СД2Т наблюдался в тех исследованиях где информация о диагнозе основывалась на сообщениях самих пациентов: в этих случаях распространенность СД2Т оказывалась значительно ниже по сравнению с данными из амбулаторных карт. Скорее всего, это объясняется тем, что исследования на основе амбулаторных карт отслеживают состояние пациента в длительном периоде наблюдения, превышая продолжительность времени, в котором болезнь могла проявиться. В соответствии с этой интерпретацией в ретроспективных исследованиях распространенность СД2Т была выше, чем в проспективных.
Клинические аспекты
В нашем мета-анализе были подчеркнуты географические различия, отражающие разный уровень распространенности СД2Т в целом, и указывающие на возможное влияние образа жизни и других факторов окружающей среды в совокупности или отдельно от генетически заданного риска. Таким образом, принимая во внимание наблюдаемое повышение риска СД2Т, приоритетной задачей в комплексном лечении людей с ТПР36-39 должен стать скрининг и минимизация факторов риска (включая неблагоприятные факторы, связанные с образом жизни и подбор определенных антипсихотических препаратов).
Наши данные четко демонстрируют, что людей с ТПР следует рассматривать как «гомогенную группу высокого риска», нуждающуюся в упреждающем скрининге СД2Т. Особенно важно с самого начала установить исходный уровень риска СД2Т для того, чтобы следить за последующими изменениями в ходе лечения. Сбор анамнеза и обследование должны включать в себя как минимум: а) историю сердечно-сосудистых заболеваний, СД2Т или других связанных болезней; б) семейный анамнез преждевременного развития сердечно-сосудистых заболеваний, СД2Т или других связанных заболеваний; в) курение, характер питания и уровень физической активности; г) вес, рост и объем талии; д) уровень сахара натощак и/или анализ на гликированный гемоглобин; е) артериальное давление (средний показатель двух измерений); и ж) история приема лекарств39.
В связи с тем, что метод диагностики СД2Т значительно повлиял на результаты оценки распространенности данного заболевания, рекомендуется проверить уровень глюкозы в плазме крови натощак (при наличии возможности провести глюкозотолерантный тест в качестве золотого стандарта диагностики), прежде чем назначать какие-либо антипсихотические препараты. Частота проведения оценки обмена глюкозы зависит от медицинской истории пациента и наличия факторов риска. Для пациентов, принимающих антипсихотические препараты с нормальным уровнем глюкозы в начале лечения, рекомендуется повторить анализы через 12 недель, а в дальнейшем повторять как минимум каждый год или чаще, если пациент относится к группе высокого риска, т. е. при значительном наборе веса, гестационном диабете в послеродовом периоде, диабете у родственников первой линии40. У пациентов с СД2Т (или с преддиабетом) анализы на сахар в крови и гликированный гемоглобин должны выполняться чаще (примерно каждые 3-6 месяцев). Ежегодное обследование должно включать в себя оценку факторов риска сердечно-сосудистых заболеваний, уровня клубочковой фильтрации, альбумин-креатининового соотношения, осмотр глаз (желательно с фотографированием глазного дна), осмотр стоп для выявления ранних признаков осложнений41.
Несмотря на рекомендации, скрининг СД2Т и скрининг факторов риска сердечно-сосудистых заболеваний по-прежнему проводят реже, чем следует, с небольшим улучшением ситуации в последнее десятилетие12. Низкая частота выполнения анализа на сахар (44.3%; 95% CI: 36.3%-52.4%)12 может отражать наличие препятствий как со стороны пациентов, так и со стороны врачей. Отношение врачей к скринингу в рамках лечения психических заболеваний в свою очередь отражает недостаток понимания того, кто ответственен за этот скрининг, что и когда нужно измерять, как интерпретировать результаты, а также отсутствие доступа к необходимому оборудованию41 и плохо налаженное взаимодействие между теми, кто оказывает первичную и специализированную медицинскую помощь. Без систематического скрининга, приводящегося в соответствии с подробными рекомендациями и с использованием доступных и точных диагностических тестов, истинная распространенность СД2Т у пациентов с ТПР останется неизвестной и недооцененной.
Даже после того, как поставлен диагноз СД2Т, многим психически больным не предлагают своевременное лечение42. В связи с этим следует уточнить, что стандартный скрининг – только первый шаг. Психиатрические центры должны согласовывать действия с диабетическими центрами для того, чтобы определить общую методику ухода за больными и обеспечить комплексный подход к людям, страдающим психическими болезнями и СД2Т. Такой подход соответствовал бы современной потребности в отказе от изолированного подхода к физическому и психическому здоровью, которая получила международную поддержку в декларации «Здоровая активная жизнь» (www.iphys.org.au).
Пациентов с диагнозом СД2Т должна регулярно осматривать многопрофильная группа специалистов, включающая врачей, медсестер, работающих с диабетиками, физиотерапевтов или спортивных врачей и диетологов, которые проявят снимание не только к диабету, но к вопросам, связанным с другими факторами риска и сопутствующими патологиями.
После выявления СД2Т людям с ТПР, скорее всего, понадобится дополнительная фармакологическая поддержка, но вряд ли она значительно отличается от той, которую получают пациенты из общей популяции. Тем не менее, врачам нужно иметь в виду то, что ухудшение психического здоровья может привести к ухудшению контроля над СД2Т, а комплексное лечение может потребовать коррекции плана терапии диабета.
Ограничения
Хотя это самый полный и подробный мета-анализ по проблеме СД2Т у людей с ТПР на сегодняшний день, мы признаем существование некоторых ограничений, вытекающих из проблем, связанных с исходными данными.
Во-первых, лишь в нескольких исследованиях СД2Т диагностировался с помощью глюкозотолерантного теста, являющегося золотым стандартом диагностики. Исследованиям, основанным на амбулаторных картах, свойственны проблемы с предвзятостью в отборе данных и недостаточной надежностью диагноза СД2Т. Во-вторых, поскольку наши исследования в основном основаны на поперечных, а не на продольных срезах, направленность связи между приемом лекарств и риском СД2Т не может быть точно определена; так что, возможно, люди с наследственной предрасположенностью к нарушению обмена веществ с большей вероятностью будут получать антипсихотики. Также, из-за того что во многих исследованиях приводятся поперечные срезы, возможно, что людям с ТПР, у которых предполагался риск развития нарушения обмена глюкозы, назначали антипсихотики со сниженным риском, такие как арипипразол и амисульприд.
В-третьих, не были указаны и проконтролированы такие параметры, как клинические подтипы большого депрессивного расстройства и биполярного расстройства. В четвертых, достоверности любого мета-анализа угрожают свойственные всем анализам различия между исследованиями и системные публикационные ошибки. Тем не менее, мы скорректировали системные публикационные ошибки методом согласования и заполнения, и смогли объяснить больше половины различий между исследованиями в нашем многомерном метарегрессионном анализе. В-пятых, низкое качество данных о факторах образа жизни препятствовала мета-аналитической оценке этих факторов в качестве переменных-модераторов и переменных-медиаторов.
Направление дальнейших исследований
В связи с тем, что при лечении биполярного расстройства43 и БДР44 все чаще в качестве препаратов первой линии используются антипсихотики, необходимы дополнительные исследования механизмов возникновения гипергликемии после начала терапии. Кроме того, следует выяснить, насколько значительно влияют на риск СД2Т определенные клинические подтипы депрессии (меланхолическая, психотическая, атипичная или недифференцированная), типы биполярного расстройства (тип 1 или 2), аффективный статус (маниакальный, депрессивный, смешанный или эутимический), различные антидепрессанты и нормотимики. Например, ранее в исследованиях45 было обнаружено, что некоторые антидепрессанты в определенных обстоятельствах уменьшают гипергликемию, нормализуют уровень сахара, а также увеличивают чувствительность к инсулину, в то время как другие, включая трициклические антидепрессанты, могут обострять гликемическую дисфункцию или оказывать незначительное влияние на уровень сахара46,47.
Кроме того, требует дальнейшего изучения сложная и недостаточно проясненная патофизиология связи ТПР и СД2Т. Появляются доказательства48 того, что у ТПР и СД2Т есть общие патофизиологические черты, включая гипоталамо-гипофизарно-надпочечниковую и митохондриальную дисфункцию. нейровоспаление, генетические связи и эпигенетические взаимодействия.
Также следует всесторонне оценить факторы риска СД2Т и определить оптимальный режим мониторинга и необходимых мероприятий. В заключение следует отметить, что требуется долгосрочное наблюдение для точной оценки более отдаленных последствий, таких как ишемическая болезнь, затраты на лечение и преждевременная смертность49.
Ключевые слова: Сахарный диабет, тяжелое психическое расстройство, шизофрения, биполярное расстройство, большое депрессивное расстройство, антипсихотики
(World Psychiatry 2016; 15: 166–174)
У людей с тяжелыми психическими расстройствами (ТПР) – шизофренией, биполярным расстройством или большим депрессивным расстройством (БДР) – риск преждевременной смерти в 2-3 раза выше, чем в целом в популяции1,2. Разрыв в смертности означает, что ожидаемая продолжительность жизни сокращается на 10-20 лет3,4, и этот разрыв продолжает расширяться5. Наиболее важной причиной сокращения ожидаемой продолжительности жизни являются сердечно-сосудистые заболевания (ССЗ)6. К основным факторам риска относится прием антипсихотических препаратов и нездоровый образ жизни7, и эти риски возрастают из-за затруднений в доступе к медицинской помощи8-12.
СД2Т – серьезный фактор риска ССЗ. Он приводит к двукратному повышению риска возникновения ишемической болезни сердца, различных видов инсультов и смерти, связанной с другими заболеваниями кровеносных сосудов13,14. Предупреждение и лечение СД2Т требуют особого внимания в клинической практике, в особенности в популяции с повышенным риском ССЗ и преждевременной смерти15,16.
Недавно вышедшие мета-анализы17-20 показали, что во всех диагностических подгруппах ТПР риск СД2Т выше, чем в целом в популяции. Однако, на данный момент недостаточно данных о мета-аналитическом сравнении рисков возникновения СД2Т у пациентов с различными психиатрическими диагнозами. Кроме того, нет мета-аналитических данных, в которых объединены все основные диагностические подгруппы ТПР, а информации о заболеваемости СД2Т среди людей с ТПР, принимающих различные антипсихотические препараты, недостаточно.
Масштабные исследования групп с ТПР могут считаться достоверными, если факторы риска изучаются на материале большого количества исследований и участников, с разделением факторов риска СД2Т, как связанных с ТПР, так и независящих от этих заболеваний. Объединение данных по основным диагностическим категориям позволяет изучить эффект демографических переменных (пол, возраст, продолжительность болезни, условия проведения исследования, географическое расположение) и лекарств (в особенности нормотимиков и антипсихотиков, назначенных при психотических и непсихотических состояниях). Если в результате проведенной работы будет выявлено различие в рисках, эта информация может быть использована врачами при планировании диагностики и лечения.
Учитывая вышеупомянутые пробелы в литературных данных, мы предприняли попытку составить крупномасштабный обзор и мета-анализ распространенности СД2Т у людей с шизофренией и подобными психотическими расстройствами, биполярным расстройством или БДР. В наши цели входило: а) определить частотность СД2Т у людей с ТПР б) проанализировать влияние демографии, характера болезни и лечения, а также методов оценки СД2Т в) определить распространенность СД2Т на основании результатов исследований, в которых напрямую сравниваются люди с ТПР и популяция в целом.
МЕТОДЫ
Критерии включения и исключения
Данный систематический обзор был проведен в соответствии с руководствами “Мета-анализ обсервационных исследований в эпидемиологии” (MOOSE)21 и стандартом “Предпочтительные параметры отчетности для систематических обзоров и мета-анализа” (PRISMA)22.
В обзор были включены наблюдательные (поперечные, ретроспективные и проспективные) и рандомизированные контролируемые исследования взрослых с шизофренией или подобными психотическими расстройствами, биполярным расстройством или БДР в соответствии с DSM-IV-TR или МКБ-10, вне зависимости от обстоятельств лечения (стационар, амбулатория, смешанный тип), содержащие данные о распространенности СД2Т.
Нами были исключены исследования, содержащие критерии включения/исключения, касающиеся наличия или отсутствия ССЗ. При необходимости мы связывались с авторами, чтобы подтвердить релевантность исследований и получить данные, которые были нужны для нашего анализа, но не были приведены в тексте публикации.
Критерии поиска, отбора и оценки исследований
Два ревьюера (DV, BS) независимо друг от друга проводили поиск в базах данных Medline, Psyc-ARTICLES, Embase и CINAHL за период до 1 августа 2015 г., без ограничений по языку. Для поиска были использованы следующие ключевые слова: “диабет” ИЛИ “глюкоза” И “тяжелое психическое расстройство” ИЛИ “острое психическое расстройство” ИЛИ “шизофрения” ИЛИ “психоз” ИЛИ “биполярное расстройство” ИЛИ “депрессия” ИЛИ “депрессивное расстройство” в названии статьи, аннотации или терминах для индексации (ключевых словах). Использовался также ручной поиск по спискам ссылок из обозреваемых работ и недавних систематических обзоров.
После исключения повторяющихся статей авторы обзора просмотрели названия и аннотации всех потенциально подходящих статей. В соответствии с критериями отбора, на основании консенсуса был составлен список статей. Затем оба автора обзора, рассмотрев полное содержание статей, на основании консенсуса составили окончательный список. К процессу в качестве посредника привлекался третий автор (СС). Методологическая экспертиза включала в себя оценку систематических ошибок (искажение результатов, дублирование данных, предпочтительная публикация положительных результатов).
Статистический анализ
Из-за предполагаемой гетерогенности, был проведен мета-анализ случайных эффектов. Гетерогенность была измерена с помощью Q-статистики (которая всегда приводится в конце описания результатов как второе или финальное значение p).
Мы рассчитали относительный риск (RR) для оценки распространенности СД2Т в подгруппах ТПР и сравнения на основании тех исследований, в которых это сравнение проводилось. Кроме того, мы сравнили распространенность СД2Т у людей с шизофренией, биполярным расстройством и БДР с контрольной группой, подходящей по возрасту и полу, также с использованием результатов исследований, в которых это сравнение проводилось. При проведении обоих анализов использовались только те сравнения групп ТПР или сравнения группы ТПР с популяцией в целом, которые проводились в рамках одного и того же исследования, чтобы свести к минимуму вариативность показателей распространенности СД2Т, возникающую из-за разницы в выборках и методиках проведения исследований.
Затем мы применили ко всему набору данных анализ по подгруппам, чтобы выявить разницу между тремя главными диагностическими подгруппами, между пациентами с множественными эпизодами и пациентами с первым эпизодом, мужчинами и женщинами, популяционными (population-based) и непопуляционными (non-population based) исследованиями, между классами препаратов (антипсихотики, антидепрессанты, нормотимики), географическими регионами. Чтобы снизить гетерогенность, мы не проводили расчет диагностических и половых различий в исследованиях, а выбрали данные из исследований, в которых проводилось сравнение пациентов по этим параметрам. Затем мы провели мета-регрессионный анализ, чтобы выявить потенциальные факторы риска (возраст, процент мужчин, продолжительность болезни, распространенность курения. методы оценки СД2Т) с помощью программы Comprehensive Meta Analysis (версия 3).
Проверка на систематические публикационные ошибки (publication bias) была проведена с помощью регрессии Эггера23 и теста Бэгг-Мазумдар24, при значении p меньше 0,5 предполагалось наличие ошибки. Встречаясь с систематической публикационной ошибкой, мы применяли метод согласования и заполнения(trim and fill)25, чтобы убрать исследования с наименьшим количеством участников с позитивной стороны воронкообразного графика и повторно пересчитать величину эффекта, пока график не станет симметричным относительно (нового) размера эффекта.
РЕЗУЛЬТАТЫ
Результаты поиска и участники
После исключения дубликатов и нерелевантных статей мы отобрали 323 публикации, из которых 118 (включающих 135 источников о распространенности СД2Т) соответствовали установленным критериям (Рисунок 1). По запросу автор может предоставить перечень включенных и исключенных исследований (с объяснением причин включения или исключения).

Окончательная выборка составила 438245 человек с ТПР и 5622664 человек в группе контроля. Размер выборок варьировался от 12 до 143943 участников, с медианным размером 270 человек. Средний возраст участников с ТПР – 44,3 года (от 23,1 до 77,6 лет); 56.8% – мужчины (разброс 0-100); 69% – белой расы (разброс 0-100; 37 исследований). Средняя продолжительность болезни – 16,1 лет (от 0 до 35 лет; 29 исследований). В 31 исследовании (N=77,028) сообщалось о распространенности курения, 44.5% (95% CI: 29.2%-60.4%) участников курили.
Заболеваемость СД2Т
Средняя взвешенная распространенность СД2Т среди 438245 человек с ТПР – 10.2% (95% CI: 9.1%-11.4%; Q=14228.7, p<0.001). Тест Бэгг-Мазумдара (Kendall’s tau=0.15, p=0.009) и тест Эггера (bias= -5.39, 95% CI: -7.33 to -3.45, p<0.001) показали наличие публикационной ошибки. После применения метода согласования и заполнения для коррекции 13 исследований, распространенность СД2Т составила 11.3% (95% CI: 10.0%-12.6
Анализ подгрупп и предикторов развития СД2Т
Параметры и тип исследования
Суммарная распространенность при различных режимах лечения (стационар, амбулатория, внебольничные пациенты, смешанные условия), типах исследования (поперечные, ретроспективные и проспективные исследования, популяционные и непопуляционные), медианном годе сбора данных (до или после 2000 г.), методах выявления СД2Т (анализ крови, сообщение пациента, медкарта) приведена в Таблице 1. Раздельные мета-регрессии приведены в Таблице 2.


Различия в режимах лечения и времени сбора данных не отразились на результатах. Также распространенность СД2Т не зависит от того является исследование популяционным или нет. С другой стороны, в исследованиях, основанных на данных из медкарт, распространенность СД2Т выше, чем в исследованиях, основанных на сообщениях пациента. Тенденция к увеличению распространенности СД2Т была найдена в ретроспективных исследованиях в сравнении с поперечными (p=0.054) и проспективными (p=0.053) исследованиями.
Диагностические подгруппы
Суммарная распространенность СД2Т в различных диагностических подгруппах представлена в Таблице 1. Мета-анализы относительного риска выявили отсутствие значительной разницы по СД2Т в исследованиях, непосредственно сравнивающих только шизофрению (14.1%, 95% CI:9.8%-20.2%; Q=5, p=0.51; N=4,963) с расстройствами шизофренического спектра (включая шизоаффективное расстройство, шизофреноформное расстройство и связанные психозы) (18.3%, 95% CI:14.9%-22.2%; Q=2.1, p=0.34; N=694) (три исследования; отношение шансов, OR=0.80; 95% CI: 0.52-1.25, z= -0.97, p=0.33; Q=2.66, p=0.26, I2=24.9).
То же самое верно для сравнения шизофрении (13.7%, 95% CI: 8.2%-22.1%; Q=131, p<0.01; N=6,005) с биполярным расстройством (13.7%, 95% CI: 9.2%-20.0%; Q=46, p<0.01; N=3,138) (шесть исследований; OR=1.22, 95% CI: 0.84-1.77, z=1.08, p=0.28; Q=17.1, p=0.004, I2=70.8); и шизофрении (13.7%, 95% CI: 11.6%-16.1%; Q=0.3, p=0.58; N=893) с БДР (11.1%, 95% CI: 9.2%-13.3%; N=911) (два исследования; OR=1.27, 95% CI: 0.96-1.68, z=1.66, p=0.10; Q=6.0, p=0.80, I2=0). Исследований, непосредственно сравнивающих распространенность СД2Т у пациентов с биполярным расстройством и БДР, было недостаточно для анализа .
Сравнение показателей СД2Т у пациентов с множественными эпизодами и у пациентов с первым эпизодом внутри разных диагностических подгрупп (см Табл. 1) показало, что среди пациентов с первым эпизодом шизофрении (4.0%, 95%CI: 2.5%-6.2%) распространенность СД2Т значительно ниже, чем у пациентов с множественными эпизодами (13.1%, 95% CI:11.7%-14.8%, z523.89, p<0.001). Отсутствие данных о пациентах с первым эпизодом биполярного расстройства или БДР помешало провести подобное сравнение в этих диагностических подгруппах.
Демографические переменные
Мета-анализ относительного риска в 29 исследованиях, непосредственно сравнивающих частотность СД2Т у мужчин (N=35,400) и женщин (N=33,283) с ТПР показал более высокую распространенность СД2Т у женщин (RR=1.43; 95% CI: 1.20-1.69, p<0.001).
Суммарная распространенность СД2Т по географическим регионам представлена в Таблице 1. Распространенность СД2Т значительно выше в Северной Америке (12.5%, 95% CI: 10.9%-14.3%; 58 исследований), чем в Европе (7.7%, 95% CI: 6.3%-9.3%; 32 исследования) (p<0.001). Других существенных географических различий не выявлено.
Раздельный мета-регрессионный анализ (см Табл. 2) показал, что более высокая частотность СД2Т обусловлена старшим возрастом, большей длительностью болезни, первым эпизодом (а не множественными эпизодами), но не полом, расой и статусом в отношении курения.
Когда все значительные демографические предикторы были введены в многовариантную мета-регрессионную модель, множественные эпизоды в сравнении с первым эпизодом (β=1.889, 95% CI: 0.1445-3.6335, z=2.12, p=0.03) остались единственной значительной переменной-модератором вариативности СД2Т.
Окончательная многовариантная модель дает объяснение для более чем половины случаев гетерогенности в исследованиях о частотности СД2Т (r2=0.52, p<0.001)
Применение лекарств
Раздельный регрессионный мета-анализ (табл. 2) показал, что на распространенность СД2Т значительно влияет продолжительность лечения, частота назначения антидепрессантов и препаратов лития, но не других нормотимиков.
В двадцати статьях, включая 64 анализа, сообщается о монотерапии антипсихотиками и частотности СД2Т. Наименьшая распространенность СД2Т была выявлена у участников, не получавших лечение антипсихотиками (2.9%, 95% CI: 1.7%-4.8%). За исключением арипипразола и амисульприда, все антипсихотики значительно (p<0.05) повышали риск СД2Т, по сравнению с участниками, не проходившими лечение антипсихотиками (Табл. 1). За исключением повышения риска при приеме кветиапина относительно оланзапина (p=0.04), мы не обнаружили различий в уровне риска у отдельных препаратов. Риск возникновения СД2Т у пациентов, принимавших клозапин, на уровне тенденции (p=0.05) был выше в сравнении с пациентами, принимавшими оланзапин.
Относительное увеличение частоты СД2Т (RR) в диагностических подгруппах в сравнении с остальным населением
34 исследования содержат данные о распространенности СД2Т у пациентов с множественными эпизодами шизофрении в сравнении со здоровыми людьми, три исследования сравнивают пациентов с первым эпизодом шизофрении и контрольную группу. В суммарном мета-анализе относительного роста риска пациенты с множественными эпизодами ТПР (N=133,470; 12.2%, 95% CI: 9.7-15.2%; Q=6166, p<0.01) имели значительно более высокий риск СД2Т (RR=1.85, 95% CI: 1.45-2.37, p<0.001; Q=1302.0, p<0.001; 38 исследований), чем остальное население (N=5,622,664; 6.2%, 95% CI: 4.8%-8.0%; Q=18,592, p<0.01). У пациентов с первым эпизодом (4.4%, 95% CI: 2.5%-7.6%; Q=2, p=0.4) не было значительных различий в распространенности СД2Т по сравнению с контрольной группой (0.9%, 95% CI: 0.03%-2.4%; Q=3, p=0.3) (RR=4.64, 95% CI: 0.73-29.3, p=0.10; Q=1302.0, p=0.23; три исследования).
По сравнению со здоровыми людьми в контрольной группе относительное увеличение частоты СД2Т у пациентов с шизофренией или связанными психотическими расстройствами равнялось 2,04 (N=115,538; 95% CI: 1.69-2.49, p<0.001; Q=1302.0, p<0.001, I²=97.8; 29 исследований); у пациентов с биполярным расстройством – 1,89 (N=4,688; 95% CI: 1.29-2.77, p<0.001; Q=2.2, p=0.34, I²=7.3; шесть исследований), у пациентов с большим депрессивным расстройством – 1,43 (N=10,895; 95% CI: 0.88-2.25, p=0.029; Q=2.15, p=0.34; три исследования).
ОБСУЖДЕНИЕ
Насколько нам известно, это первый мета-анализ СД2Т, включающий и сравнивающий данные о трех основных ТПР, а именно о шизофрении вместе с расстройствами шизофренического спектра, биполярном расстройстве и большом депрессивном расстройстве. Приблизительно у каждого десятого человека с ТПР (11.3%; 95% CI: 10.0%-12.6%) наблюдался СД2Т, при этом почти в два раза, по сравнению с остальным населением, увеличивалась частота СД2Т у людей с многоэпизодными ТПР (RR=1.85, 95% CI: 1.45-2.37).Распространенность СД2Т в каждой из трех диагностических подгрупп повышалась по сравнению с остальным населением одинаково, сравнительный мета-анализ не выявил значительной разницы между подгруппами с шизофренией, расстройствами шизофренического спектра, биполярным расстройством и большим депрессивным расстройством. Таким образом, на частотность СД2Т, скорее всего, влияют факторы, не связанные с диагнозом, такие как гипергликемия после приема психотропных препаратов26, нездоровый образ жизни на протяжении длительного времени27,28, а также вероятные генетические факторы, связанные как с психиатрическими, так и с общемедицинскими рисками29.
Впервые в рамках большого мета-анализа нами было показано, что риск СД2Т действительно возрастает по мере увеличения длительности лечения, подтверждение чему было также дано в мультивариантной мета-регрессионной модели, в которой уникальным значимым предиктором, объяснявшим половину дисперсии, являлись множественные эпизоды заболевания. Также мы обнаружили значительное повышение распространенности СД2Т в Северной Америке по сравнению с Европой, соответствующее уровню распространенности в общей популяции30, что предполагает комбинированное влияние генетических факторов, образа жизни и/или факторов окружающей среды.
Знание о факторах, повышающих риск СД2Т, поможет выявить тех, кто нуждается в особенно интенсивном наблюдении и лечебно-диагностических интервенциях. В отличие от остального населения, у женщин с ТПР, как мы выяснили, риск развития СД2Т выше, чем у мужчин. Это наблюдение требует дальнейших исследований, но, может быть, это связано с тем, что женщины с ТПР более склонны к общему и центральному ожирению, чем мужчины32, а центральное ожирение является важным фактором риска гипергликемии.
С другой стороны, только малая часть проанализированных исследований содержит информацию о среднем возрасте женщин и мужчин, и есть вероятность, что женщины с шизофрений были старше, что могло отразиться на результатах.
Результаты нашего исследования также показывают, что у людей с множественными эпизодами шизофрении распространенность СД2Т была выше, чем у людей с первым эпизодом. Данный мета-анализ подтверждает то, что диагноз первого эпизода является уникальным предиктором меньшей распространенности СД2Т вне зависимости от возраста, что также было выявлено в недавнем анализе распространенности метаболического синдрома у пациентов с теми же тремя основными ТПР33. Полученные результаты указывают на необходимость раннего предупреждающего вмешательства с целью уменьшить кардиометаболический риск у людей с ТПР. Потребуются дальнейшие исследования для изучения механизмов, лежащих в основе повышения риска СД2Т при переходе заболевания от начального эпизода к множественным эпизодам заболевания.
Наши данные подтверждают полученные ранее доказательства того, что прием психотропных препаратов, включая антидепрессанты, препараты лития и антипсихотики26, повышает распространенность СД2Т.
За исключением арипипразола и амисульприда, все антипсихотики связаны со значительным повышением риска СД2Т в сравнении с пациентами, не принимавшими антипсихотики. Различия в рисках возникновения отклонений уровня глюкозы описаны в литературе, при этом наивысший риск наблюдается при терапии клозапином, оланзапином и кветапином25,34,35.
В данном мета-анализе терапия кветапином (и клозапином на уровне тенденции) приводила даже к более высоким рискам возникновения СД2Т, чем терапия оланзапином. Однако, из-за того, что нельзя исключить эффекта искажения данных тогда, когда пациенты с риском СД2Т или даже с СД2Т, появившемся на фоне приема таких повышающих риск лекарств, как оланзапин, могли быть переведены на другой антипсихотик, в том числе кветапин, это наблюдение, во избежание ошибочной атрибуции, следует интерпретировать с осторожностью.
Наконец, как и ожидалось, самый низкий показатель распространенности СД2Т наблюдался в тех исследованиях где информация о диагнозе основывалась на сообщениях самих пациентов: в этих случаях распространенность СД2Т оказывалась значительно ниже по сравнению с данными из амбулаторных карт. Скорее всего, это объясняется тем, что исследования на основе амбулаторных карт отслеживают состояние пациента в длительном периоде наблюдения, превышая продолжительность времени, в котором болезнь могла проявиться. В соответствии с этой интерпретацией в ретроспективных исследованиях распространенность СД2Т была выше, чем в проспективных.
Клинические аспекты
В нашем мета-анализе были подчеркнуты географические различия, отражающие разный уровень распространенности СД2Т в целом, и указывающие на возможное влияние образа жизни и других факторов окружающей среды в совокупности или отдельно от генетически заданного риска. Таким образом, принимая во внимание наблюдаемое повышение риска СД2Т, приоритетной задачей в комплексном лечении людей с ТПР36-39 должен стать скрининг и минимизация факторов риска (включая неблагоприятные факторы, связанные с образом жизни и подбор определенных антипсихотических препаратов).
Наши данные четко демонстрируют, что людей с ТПР следует рассматривать как «гомогенную группу высокого риска», нуждающуюся в упреждающем скрининге СД2Т. Особенно важно с самого начала установить исходный уровень риска СД2Т для того, чтобы следить за последующими изменениями в ходе лечения. Сбор анамнеза и обследование должны включать в себя как минимум: а) историю сердечно-сосудистых заболеваний, СД2Т или других связанных болезней; б) семейный анамнез преждевременного развития сердечно-сосудистых заболеваний, СД2Т или других связанных заболеваний; в) курение, характер питания и уровень физической активности; г) вес, рост и объем талии; д) уровень сахара натощак и/или анализ на гликированный гемоглобин; е) артериальное давление (средний показатель двух измерений); и ж) история приема лекарств39.
В связи с тем, что метод диагностики СД2Т значительно повлиял на результаты оценки распространенности данного заболевания, рекомендуется проверить уровень глюкозы в плазме крови натощак (при наличии возможности провести глюкозотолерантный тест в качестве золотого стандарта диагностики), прежде чем назначать какие-либо антипсихотические препараты. Частота проведения оценки обмена глюкозы зависит от медицинской истории пациента и наличия факторов риска. Для пациентов, принимающих антипсихотические препараты с нормальным уровнем глюкозы в начале лечения, рекомендуется повторить анализы через 12 недель, а в дальнейшем повторять как минимум каждый год или чаще, если пациент относится к группе высокого риска, т. е. при значительном наборе веса, гестационном диабете в послеродовом периоде, диабете у родственников первой линии40. У пациентов с СД2Т (или с преддиабетом) анализы на сахар в крови и гликированный гемоглобин должны выполняться чаще (примерно каждые 3-6 месяцев). Ежегодное обследование должно включать в себя оценку факторов риска сердечно-сосудистых заболеваний, уровня клубочковой фильтрации, альбумин-креатининового соотношения, осмотр глаз (желательно с фотографированием глазного дна), осмотр стоп для выявления ранних признаков осложнений41.
Несмотря на рекомендации, скрининг СД2Т и скрининг факторов риска сердечно-сосудистых заболеваний по-прежнему проводят реже, чем следует, с небольшим улучшением ситуации в последнее десятилетие12. Низкая частота выполнения анализа на сахар (44.3%; 95% CI: 36.3%-52.4%)12 может отражать наличие препятствий как со стороны пациентов, так и со стороны врачей. Отношение врачей к скринингу в рамках лечения психических заболеваний в свою очередь отражает недостаток понимания того, кто ответственен за этот скрининг, что и когда нужно измерять, как интерпретировать результаты, а также отсутствие доступа к необходимому оборудованию41 и плохо налаженное взаимодействие между теми, кто оказывает первичную и специализированную медицинскую помощь. Без систематического скрининга, приводящегося в соответствии с подробными рекомендациями и с использованием доступных и точных диагностических тестов, истинная распространенность СД2Т у пациентов с ТПР останется неизвестной и недооцененной.
Даже после того, как поставлен диагноз СД2Т, многим психически больным не предлагают своевременное лечение42. В связи с этим следует уточнить, что стандартный скрининг – только первый шаг. Психиатрические центры должны согласовывать действия с диабетическими центрами для того, чтобы определить общую методику ухода за больными и обеспечить комплексный подход к людям, страдающим психическими болезнями и СД2Т. Такой подход соответствовал бы современной потребности в отказе от изолированного подхода к физическому и психическому здоровью, которая получила международную поддержку в декларации «Здоровая активная жизнь» (www.iphys.org.au).
Пациентов с диагнозом СД2Т должна регулярно осматривать многопрофильная группа специалистов, включающая врачей, медсестер, работающих с диабетиками, физиотерапевтов или спортивных врачей и диетологов, которые проявят снимание не только к диабету, но к вопросам, связанным с другими факторами риска и сопутствующими патологиями.
После выявления СД2Т людям с ТПР, скорее всего, понадобится дополнительная фармакологическая поддержка, но вряд ли она значительно отличается от той, которую получают пациенты из общей популяции. Тем не менее, врачам нужно иметь в виду то, что ухудшение психического здоровья может привести к ухудшению контроля над СД2Т, а комплексное лечение может потребовать коррекции плана терапии диабета.
Ограничения
Хотя это самый полный и подробный мета-анализ по проблеме СД2Т у людей с ТПР на сегодняшний день, мы признаем существование некоторых ограничений, вытекающих из проблем, связанных с исходными данными.
Во-первых, лишь в нескольких исследованиях СД2Т диагностировался с помощью глюкозотолерантного теста, являющегося золотым стандартом диагностики. Исследованиям, основанным на амбулаторных картах, свойственны проблемы с предвзятостью в отборе данных и недостаточной надежностью диагноза СД2Т. Во-вторых, поскольку наши исследования в основном основаны на поперечных, а не на продольных срезах, направленность связи между приемом лекарств и риском СД2Т не может быть точно определена; так что, возможно, люди с наследственной предрасположенностью к нарушению обмена веществ с большей вероятностью будут получать антипсихотики. Также, из-за того что во многих исследованиях приводятся поперечные срезы, возможно, что людям с ТПР, у которых предполагался риск развития нарушения обмена глюкозы, назначали антипсихотики со сниженным риском, такие как арипипразол и амисульприд.
В-третьих, не были указаны и проконтролированы такие параметры, как клинические подтипы большого депрессивного расстройства и биполярного расстройства. В четвертых, достоверности любого мета-анализа угрожают свойственные всем анализам различия между исследованиями и системные публикационные ошибки. Тем не менее, мы скорректировали системные публикационные ошибки методом согласования и заполнения, и смогли объяснить больше половины различий между исследованиями в нашем многомерном метарегрессионном анализе. В-пятых, низкое качество данных о факторах образа жизни препятствовала мета-аналитической оценке этих факторов в качестве переменных-модераторов и переменных-медиаторов.
Направление дальнейших исследований
В связи с тем, что при лечении биполярного расстройства43 и БДР44 все чаще в качестве препаратов первой линии используются антипсихотики, необходимы дополнительные исследования механизмов возникновения гипергликемии после начала терапии. Кроме того, следует выяснить, насколько значительно влияют на риск СД2Т определенные клинические подтипы депрессии (меланхолическая, психотическая, атипичная или недифференцированная), типы биполярного расстройства (тип 1 или 2), аффективный статус (маниакальный, депрессивный, смешанный или эутимический), различные антидепрессанты и нормотимики. Например, ранее в исследованиях45 было обнаружено, что некоторые антидепрессанты в определенных обстоятельствах уменьшают гипергликемию, нормализуют уровень сахара, а также увеличивают чувствительность к инсулину, в то время как другие, включая трициклические антидепрессанты, могут обострять гликемическую дисфункцию или оказывать незначительное влияние на уровень сахара46,47.
Кроме того, требует дальнейшего изучения сложная и недостаточно проясненная патофизиология связи ТПР и СД2Т. Появляются доказательства48 того, что у ТПР и СД2Т есть общие патофизиологические черты, включая гипоталамо-гипофизарно-надпочечниковую и митохондриальную дисфункцию. нейровоспаление, генетические связи и эпигенетические взаимодействия.
Также следует всесторонне оценить факторы риска СД2Т и определить оптимальный режим мониторинга и необходимых мероприятий. В заключение следует отметить, что требуется долгосрочное наблюдение для точной оценки более отдаленных последствий, таких как ишемическая болезнь, затраты на лечение и преждевременная смертность49.
Список исп. литературыСкрыть список1. Chesney E, Goodwin GM, Fazel S. Risks of all-cause and suicide mortality in mental disorders: a meta-review. World Psychiatry 2014;13:153-60.
2. Reininghaus U, Dutta R, Dazzan P et al. Mortality in schizophrenia and other psychoses: a 10-year follow-up of the AESOP first-episode cohort. Schizophr Bull 2015;41:664-73.
3. Chang CK, Hayes RD, Perera G et al. Life expectancy at birth for people with serious mental illness from a secondary mental health care case register in London, UK. PLoS One 2011;6:e19590.
4. Lawrence D, Hancock KJ, Kisely S. The gap in life expectancy from preventable physical illness in psychiatric patients in Western Australia: retrospective analysis of population based registers. BMJ 2013;346:f2539.
5. Saha S, Chant D, McGrath J. A systematic review of mortality in schizophrenia. Arch Gen Psychiatry 2007;64:1123-31.
6. Hoang U, Goldacre MJ, Stewart R. Avoidable mortality in people with schizophrenia or bipolar disorder in England. Acta Psychiatr Scand 2013;127:195-201.
7. De Hert M, Correll CU, Bobes J et al. Physical illness in patients with severe mental disorders. I. Prevalence, impact of medications and disparities in health care. World Psychiatry 2011; 10:52-77.
8. Mitchell AJ, Lord O. Do deficits in cardiac care influence high mortality rates in schizophrenia? A systematic review and pooled analysis. J Psychopharmacol 2010;24(Suppl. 4):69-80.
9. Mitchell AJ, Lord O, Malone D. Differences in the prescribing of medication for physical disorders in individuals with v. without mental illness: meta-analysis. Br J Psychiatry 2012;201:435-43.
10. Mitchell AJ, Malone D, Doebbeling CC. Quality of medical care for people with and without comorbid mental illness and substance misuse: systematic review of comparative studies. Br J Psychiatry 2009;194:491-9.
11. De Hert M, Vancampfort D, Correll CU et al. Guidelines for screening and monitoring of cardiometabolic risk in schizophrenia: systematic evaluation. Br J Psychiatry 2011;199:99-105.
12. Mitchell AJ, Delaffon V, Vancampfort D et al. Guideline concordant monitoring of metabolic risk in people treated with antipsychotic medication: systematic review and meta-analysis of screening practices. Psychol Med 2012;42:125-47.
13. Sarwar N, Gao P, Seshasai SR et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet 2010; 375: 2215-22.
14. Murray CJ, Vos T, Lozano R et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012;380:2197-223.
15. Grundy SM, Benjamin IJ, Burke GL et al. Diabetes and cardiovascular disease: statement for health professionals from the American Heart Association. Circulation 1999;100:1134-46.
16. World Health Organization. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus. Geneva: World Health Organization, 1999.
17. Vancampfort D, Wampers M, Mitchell AJ et al. A meta-analysis of cardiometabolic abnormalities in drug naıve, first-episode and multi-episode patients with schizophrenia versus general population controls. World Psychiatry 2013;12:240-50.
18. Stubbs B, Vancampfort D, De Hert M et al. The prevalence and predictors of type 2 diabetes in people with schizophrenia: a systematic review and comparative meta-analysis. Acta Psychiatr Scand 2015;132:144-57.
19. Vancampfort D, Mitchell AJ, De Hert M et al. Prevalence and predictors of type 2 diabetes in people with bipolar disorder: a systematic review and meta-analysis. J Clin Psychiatry 2015;76:1490-9.
20. Vancampfort D, Mitchell AJ, De Hert M et al. Type 2 diabetes in patients with major depressive disorder: a meta-analysis of prevalence estimates and predictors. Depress Anxiety 2015;32:763-73.
21. Stroup DF, Berlin JA, Morton SC et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000;283: 2008-12.
22. Moher D, Liberati A, Tetzlaff J et al. The PRISMA Group. Preferred reporting items for systematic reviews and meta-Analyses: the PRISMA Statement. PLoS Med 2009;6:e1000097.
23. Egger M, Davey SG, Schneider M et al. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997;315:629-34.
24. Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994;50:1088-101.
25. Duval S, Tweedie R. A non-parametric ‘trim and fill’ method for assessing publication bias in meta-analysis. J Am Stat Assoc 2000;95:89-98.
26. Correll CU, Detraux J, De Lepeleire J et al. Effects of antipsychotics, anti depressants and mood stabilizers on risk for physical diseases in people with schizophrenia, depression and bipolar disorder. World Psychiatry 2015;14:119-36.
27. Vancampfort D, Probst M, Knapen J et al. Associations between sedentary behaviour and metabolic parameters in patients with schizophrenia. Psychiatry Res 2012;200:73-8.
28. Vancampfort D, De Hert M, Sweers K et al. Diabetes, physical activity participation and exercise capacity in patients with schizophrenia. Psychiatry Clin Neurosci 2013;67:451-6.
29. Ellingrod VL, Taylor SF, Dalack G et al. Risk factors associated with metabolic syndrome in bipolar and schizophrenia subjects treated with anti psychotics: the role of folate pharmacogenetics. J Clin Psychopharmacol 2012;32:261-5.
30. International Diabetes Federation. IDF diabetes atlas. Sixth edition update. Brussels: International Diabetes Federation, 2014.
31. Hammerman A, Dreiher J, Klang SH et al. Antipsychotics and diabetes: an age-related association. Ann Pharmacother 2008;42:1316-22.
32. Gardner-Sood P, Lally J, Smith S et al. Cardiovascular risk factors and metabolic syndrome in people with established psychotic illnesses: baseline data from the IMPaCT randomized controlled trial. Psychol Med 2015;45: 2619-29.
33. Vancampfort D, Stubbs B, Mitchell AJ et al. Risk of metabolic syndrome and its components in people with schizophrenia, bipolar and major depressive disorders: a large scale meta-analysis of 198 studies. World Psychiatry 2015;14:339-47.
34. Nielsen J, Skadhede S, Correll CU. Antipsychotics associated with the development of type 2 diabetes in antipsychotic-naıve schizophrenia patients. Neuropsychopharmacology 2010;35:1997-2004.
35. Kessing LV, Thomsen AF, Mogensen UB et al. Treatment with antipsychotics and the risk of diabetes in clinical practice. Br J Psychiatry 2010; 197:266-71.
36. De Hert M, Dekker JM, Wood D et al. Cardiovascular disease and diabetes in people with severe mental illness position statement from the European Psychiatric Association (EPA), supported by the European Association for the Study of Diabetes (EASD) and the European Society of Cardiology (ESC). Eur Psychiatry 2009;24:412-24.
37. McIntyre RS, Alsuwaidan M, Goldstein BI et al. The Canadian Network for Mood and Anxiety Treatments (CANMAT) task force recommendations for the management of patients with mood disorders and comorbid metabolic disorders. Ann Clin Psychiatry 2012;24:69-81.
38. Vancampfort D, De Hert M, Skjerven LH et al. International Organization of Physical Therapy in Mental Health consensus on physical activity within multidisciplinary rehabilitation programmes for minimising cardio-metabolic risk in patients with schizophrenia. Disabil Rehabil 2012;34:1-12.
39. Gierisch JM, Nieuwsma JA, Bradford DW et al. Pharmacologic and behavioral interventions to improve cardiovascular risk factors in adults with serious mental illness: a systematic review and meta-analysis. J Clin Psychiatry 2014;75:424-40.
40. De Hert M, Detraux J, van Winkel R et al. Metabolic and cardiovascular adverse effects associated with antipsychotic drugs. Nat Rev Endocrinol 2011;8:114-26.
41. De Hert M, Cohen D, Bobes J et al. Physical illness in patients with severe mental disorders. II. Barriers to care, monitoring and treatment guidelines, and recommendations at the system and individual levels. World Psychiatry 2011;10:138-51.
42. Holt RI. The prevention of diabetes and cardiovascular disease in people with schizophrenia. Acta Psychiatr Scand 2015;132:86-96.
43. Pillarella J, Higashi A, Alexander GC et al. Trends in use of secondgeneration antipsychotics for treatment of bipolar disorder in the United States, 1998-2009. Psychiatr Serv 2012;63:83-6.
44. Davidson JR. Major depressive disorder treatment guidelines in America and Europe. J Clin Psychiatry 2010;71(Suppl. 1):e04.
45. Hennings JM, Schaaf L, Fulda S. Glucose metabolism and antidepressant medication. Curr Pharm Des 2012;18:5900-19.
46. Mojtabai R. Antidepressant use and glycemic control. Psychopharmacologia 2013;227:467-77.
47. Lamers F, Vogelzangs N, Merikangas KR et al. Evidence for a differential role of HPA-axis function, inflammation and metabolic syndrome in melancholic versus atypical depression. Mol Psychiatry 2013;18:692-9.
48. Manu P, Correll CU, Wampers M et al. Markers of inflammation in schizophrenia: association vs. causation. World Psychiatry 2014;13:189-92.
49. Correll CU, Joffe BI, Rosen LM et al. Cardiovascular and cerebrovascular risk factors and events associated with second-generation antipsychotic compared to antidepressant use in a non-elderly adult sample: results from a claims-based inception cohort study. World Psychiatry 2015;14:55-62.
1 июня 2016
Количество просмотров: 1927
