Клинический разбор в общей медицине №5 2022
Clinical manifestations of post-COVID-19 syndrome in men and women
Victoriya A. Sergeeva, Tatiana E. Lipatova
Abstract
Background. Approximately every third patient who passed new coronavirus infection doesn’t feel absolutely healthy even few months ago after disease. Most constantly have noted fatigue (asthenia), sleep disorders, cognitive dysfunction and cardiovascular symptoms. In spite of coexistence different terms which describe persistent post-COVID-19 clinical manifestations, all of them serve the only goal – to demonstrate that the patients need in continuing medical care and rehabilitation after acute period of disease.
Aim. Assessment of clinical manifestations of bridge syndrome in men and women.
Materials and methods. Clinical manifestations of post-COVID-19 syndrome were assessed in 80 patients (49 women and 31 men) using a clinical interview and voluntary anonymous questionnaire. The mMRC (Modified Medical Research Council) scale was used to assess the severity of dyspnea, the McNair and Kahn questionnaire – for cognitive dysfunction, the FSS (Fatigue Severity Scale) – for the severity of fatigue (asthenia), and the visual analogue scale (VAS) was used for subjective assessment of fatigue. Statistical data processing was performed using the StatPlus 2009 Professional program.
Results. Among the most frequently reported complaints of patients in the post-COVID period were fatigue, sleep disturbances, cardiovascular symptoms, pain in muscles and joints. Among women in the post-COVID syndrome, headache was more often recorded, among men – fatigue. The severity of fatigue (asthenia) was also most pronounced among men. A variety of sleep disorders were identified in the vast majority of patients. Daytime sleepiness was recorded more often in men (almost every third man); for women, a characteristic sleep disorder was nightmares, which were not observed in men. Approximately with the same frequency among both sexes, problems with falling asleep and nocturnal awakenings were revealed. Cognitive impairment was observed in approximately one in four patients who had COVID-19, regardless of gender. Statistical relationships between asthenia and cognitive dysfunction were revealed, which are more significant among men.
Conclusion. The multiplicity of post-COVID clinical manifestations among men and women raises questions about the heterogeneity and potential summation of the pathogenic mechanisms underlying each symptom. Differences in the clinical symptoms of the post-COVID-19 period among men and women may can be explained by gender-specific immune response and require further study.
Key words: post-COVID-19 syndrome, COVID-19, fatigue, sleep disorders, cognitive dysfunction.
For citation: Sergeeva V.A., Lipatova T.E. Clinical manifestations of post-COVID-19 syndrome in men and women. Clinical analysis in general medicine. 2022; 5: 16–22. DOI: 10.47407/kr2022.3.5.00158
Введение
По мере накопления клинических данных при наблюдении за перенесшими новую коронавирусную инфекцию пациентами в связи с сохранением большого количества симптомов, несмотря на окончание острого периода заболевания, возникла необходимость внедрения новой терминологии. В связи с этим в различных научных источниках стали появляться определения: long COVID-19, long-haul COVID-19, post-acute COVID-19, chronic COVID-19 и другие, отличающиеся сроками манифестации и продолжительностью клинических проявлений после перенесения инфекции, вызванной вирусом SARS-CoV-2.
Впервые на сохраняющиеся симптомы после острой фазы заболевания новой коронавирусной инфекцией обратили внимание члены исследовательской группы пациентов-ученых (The Patient-Led Research Collaborative) в апреле 2020 г. [1]. Следующим значимым этапом было внедрение в 2021 г. Всемирной организацией здравоохранения общего понятия «постковидное состояние», которое принято определять как сочетание симптомов, которые развиваются в течение 12 нед после выздоровления от COVID-19, длятся не менее
2 мес и не объясняются наличием альтернативных заболеваний. Симптомы могут возникать впервые после выздоровления от острого эпизода COVID-19 или сохраняться после первоначального заболевания. Симптомы также могут изменяться или рецидивировать с течением времени [2]. В настоящее время все большее распространение в отечественной и зарубежной литературе приобретает термин «постковидный синдром» – ПКС (post-COVID-19 syndrome), в целом соответствующий определению постковидного состояния. По мнению разных авторов, частота ПКС варьирует от 10–35% у получавших амбулаторное лечение до 85% среди пациентов, проходивших стационарное лечение по поводу новой коронавирусной инфекции, что обусловливает актуальность его дальнейшего изучения [3].
По крайней мере несколько ведущих патогенетических механизмов обсуждается в качестве основных в развитии ПКС. Во-первых, вирусоспецифические патофизиологические изменения, обусловленные механизмом проникновения вируса в клетки хозяина; во-вторых, иммунологические отклонения и воспалительные повреждения в ответ на острую инфекцию; в-третьих, ожидаемые последствия постреанимационного синдрома среди пациентов, находившихся на лечении в отделении неотложной и интенсивной терапии [4]. Предполагается, что наряду с прямым повреждающим воздействием вируса длительное системное воспаление может играть ключевую роль в происхождении различных неврологических симптомов у пациентов, перенесших COVID-19: слабость (астения), нарушения сна, когнитивная дисфункция (КД) [5, 6]. Эти же механизмы могут быть ответственны за миокардиальное повреждение и развитие различных сердечно-сосудистых симптомов в постковидный период [7]. Отмечены случаи и так называемого мультисистемного воспалительного синдрома, ассоциированного с COVID-19, первоначально описанного среди детей [8]. В отсутствие позитивного теста полимеразной цепной реакции на коронавирус у таких пациентов наблюдаются высокие титры провоспалительных цитокинов (С-реактивный белок, фибриноген, интерлейкин – ИЛ-6 и др.) и широкий спектр полиорганных клинических проявлений (сердечно-сосудистых, гастроэнтерологических, дерматологических, неврологических) [8]. В настоящее время неизвестен временной интервал манифеста мультисистемного воспалительного синдрома от начала заболевания у пациентов с новой коронавирусной инфекцией, поэтому трудно судить о том, следует ли его рассматривать в клинической картине острого периода COVID-19 или относить уже к ПКС. Среди других значимых патофизиологических механизмов ПКС весомая роль принадлежит микрососудистому повреждению, ишемии, тромбоэмболизму, оксидативному стрессу [4]. Многие клинические симптомы в постковидном периоде связывают с длительным малоподвижным состоянием и так называемым постреанимационным синдромом, которые напрямую связаны с тяжестью перенесенной новой коронавирусной инфекции [4]. Однако далеко не всегда тяжесть заболевания и длительность COVID-19 определяют течение ПКС. Многие пациенты, перенесшие инфекцию в легкой форме, без поражения легких, спустя несколько месяцев после выздоровления продолжают испытывать различные симптомы [3]. Среди наиболее часто регистрирующихся клинических проявлений отмечены слабость или астения (слабость, утомляемость), КД, нарушения сна, одышка, нарушения сердечного ритма.
Многообразие постковидных симптомов, снижение трудоспособности и в целом качества жизни значительного числа людей, в том числе молодого возраста, диктуют необходимость дальнейшего изучения проблемы с целью разработки возможных подходов реабилитации и скорейшего восстановления их здоровья.
Цель исследования – изучение и сравнительная оценка наиболее распространенных постковидных клинических проявлений среди пациентов обоих полов.
Материалы и методы
Проведено клиническое интервью и анонимное прямое анкетирование 80 пациентов (31 мужчины и 49 женщин), перенесших новую коронавирусную инфекцию не менее 12 нед назад (согласно критериям ПКС), у которых отмечались различные клинические проявления на момент проведения исследования. Все пациенты дали добровольное согласие на участие в исследовании, которое проводилось с соблюдением этических норм Хельсинкской декларации. Изучена исходная полиморбидность пациентов, принявших участие в исследовании. Критериями исключения стали наличие старческого возраста, выраженных интеллектуально-мнестических расстройств, обострение хронических заболеваний, ревматическая патология, острый коронарный синдром, онкопатология и получение химиотерапии. Для оценки ряда симптомов использовались валидизированные в Российской Федерации шкалы. Одышка оценивалась по шкале mMRC (Modified Medical Research Council). Для оценки когнитивных нарушений использовался опросник МакНера и Кана. При наборе респондентом 42 баллов и более констатировалась КД. В дополнение подробно изучены проявления астенического синдрома с использованием шкалы степени тяжести астении FSS (Fatigue Severity Scale) и визуальной аналоговой шкалы собственной оценки респондентами проявлений утомляемости, при которой респонденты могли сами оценить тяжесть своей астении по 10-балльной шкале, где 1 – минимальный уровень, 10 – максимальный. При интерпретации результатов шкалы FSS пороговым значением было 36 баллов, при наборе
36 баллов и более констатировалась клинически значимая слабость (астения).
Статистическая обработка данных производилась с помощью программы StatPlus 2009 Professional. При оценке характера распределения количественных признаков использовали критерии Колмогорова–Смирнова и Шапиро–Уилка. Все количественные показатели в работе имеют ненормальное распределение и представлены в виде медианы (Ме) и интерквартильного размаха – значения 25 и 75-го процентилей [Ме (25р; 75р)]. При сравнении независимых выборок использовали тест Манна–Уитни и тест Колмогорова–Смирнова в зависимости от величины сравниваемых групп. Для выявления и оценки тесноты связи между двумя рядами сопоставляемых количественных показателей использовался коэффициент ранговой корреляции Спирмена. При сравнении относительных показателей между группами использовался t-критерий Стьюдента. Статистически значимым было принято p-значение <0,05.
Результаты
Обследованы 80 пациентов (49 женщин и 31 мужчина), у которых более 12 нед после перенесения новой коронавирусной инфекции сохранялись различные симптомы. Группы пациентов были сопоставимы по возрасту, тяжести перенесенной инфекции COVID-19, наличию сопутствующих заболеваний. Полная характеристика сравниваемых групп отражена в таблице. Как видно из представленных данных, большая часть обследованных пациентов перенесли новую коронавирусную инфекцию в легкой и среднетяжелой форме. При этом отмечается длительное сохранение постковидных симптомов, вплоть до 6 мес и более. Проведена сравнительная оценка наиболее часто встречающихся симптомов у мужчин и женщин в
постковидный период. Результаты представлены на рис. 1. Как видно исходя из полученных результатов, доминирующими симптомами в обеих группах оказались нарушения сна и слабость. В группе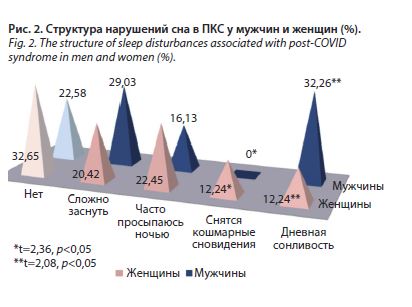
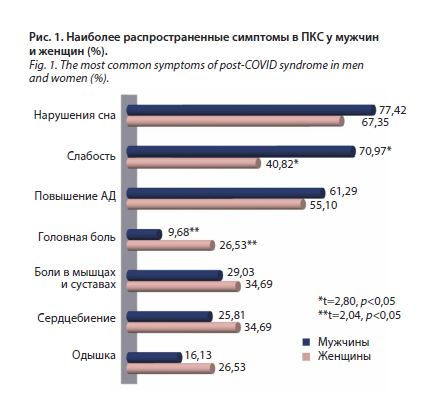 мужчин слабость со статистической значимостью встречалась чаще (70,97%), чем у женщин (40,82%); t=2,80, p<0,05. Боли в мышцах и суставах, сердцебиение, одышка встречались практически у каждой третьей женщины, частота этих симптомов среди мужчин была незначительно ниже, без статистической значимости (p>0,05). Головная боль в ПКС отмечалась, напротив, чаще у женщин (26,53%), чем у мужчин (9,68%); p<0,05. Повышение артериального давления было отмечено у 55,10% женщин в исследуемой группе и у 61,29% мужчин (p>0,05). Стоит обратить внимание, что до инфекции COVID-19 артериальная гипертензия (АГ) имелась у 32,65% женщин и 51,61% мужчин (p>0,05). В связи с этим проведено уточнение о числе новых случаев АГ в каждой группе после перенесения новой коронавирусной инфекции. Так, среди женщин 22,45% стали отмечать подъемы артериального давления de novo, среди мужчин – только 9,68% (p>0,05).
мужчин слабость со статистической значимостью встречалась чаще (70,97%), чем у женщин (40,82%); t=2,80, p<0,05. Боли в мышцах и суставах, сердцебиение, одышка встречались практически у каждой третьей женщины, частота этих симптомов среди мужчин была незначительно ниже, без статистической значимости (p>0,05). Головная боль в ПКС отмечалась, напротив, чаще у женщин (26,53%), чем у мужчин (9,68%); p<0,05. Повышение артериального давления было отмечено у 55,10% женщин в исследуемой группе и у 61,29% мужчин (p>0,05). Стоит обратить внимание, что до инфекции COVID-19 артериальная гипертензия (АГ) имелась у 32,65% женщин и 51,61% мужчин (p>0,05). В связи с этим проведено уточнение о числе новых случаев АГ в каждой группе после перенесения новой коронавирусной инфекции. Так, среди женщин 22,45% стали отмечать подъемы артериального давления de novo, среди мужчин – только 9,68% (p>0,05).
Структура нарушений сна в исследуемых группах подробно представлена на рис. 2. Как видно из диаграммы, сложности с засыпанием отмечены практически в равных долях среди мужчин (29,03%) и женщин (20,42%); p>0,05. Просыпаются часто среди ночи и отмечают недосыпание 16,13% мужчин и 22,45% женщин без статистически значимых различий (p>0,05). Кошмарные сновидения, напротив, отмечены среди жалоб только у женщин (12,24%), у мужчин данные расстройства сна не выявлены (0%); p<0,05. Возможно, это обстоятельство является следствием большей эмоциональности женщин и часто сопутствующей ей тревожности, связанной с тяжелым заболеванием, в данном случае COVID-19. Дневная сонливость была, напротив, присуща в большей степени мужчинам (32,26%) по сравнению с женщинами (12,24%); p<0,05. Такие данные представляют интерес, так как не могут быть объяснены наличием сопутствующей патологии, влияющей на этот симптом. В исследуемой группе мужчин было только 2 пациента с хронической обструктивной болезнью легких (ХОБЛ), которая при тяжелом течении либо обострении может быть причиной тяжелой гипоксемии и приводить в том числе к дневной сонливости. Кроме этого, в группе мужчин было сопоставимое с группой женщин число лиц с ожирением, для него характерен синдром альвеолярной гиповентиляции, при котором дневная сонливость является наиболее характерным симптомом [9].
Как один из ведущих симптомов в ПКС – слабость (астения) была проанализирована в каждой группе более подробно. С помощью шкалы-опросника FSS при наборе 36 баллов и более астения трактуется как клинически значимая и, чем больше баллов набирает пациент, тем тяжелее его астеническое состояние. В группе женщин Me баллов составила 28 (9; 53), у мужчин – 39 (31,75; 54); тест Колмогорова–Смирнова: p=0,0315; тест Манна–Уитни: U=943, Z=1,812, p=0,07. Таким образом, установлено, что среди мужчин отмечается не только бóльшая распространенность этого симптома в ПКС, но и бóльшая его выраженность. По визуальной аналоговой шкале среди женщин с клинически значимой астенией Ме баллов составила 5 (3; 7), среди мужчин – 5 (4; 7); статистически значимых различий между группами не получено: тест Манна–Уитни – U=863,5, Z=1,027, p=0,30. На максимальное число баллов (от 8 до 10) свою астению оценили 18,37% женщин и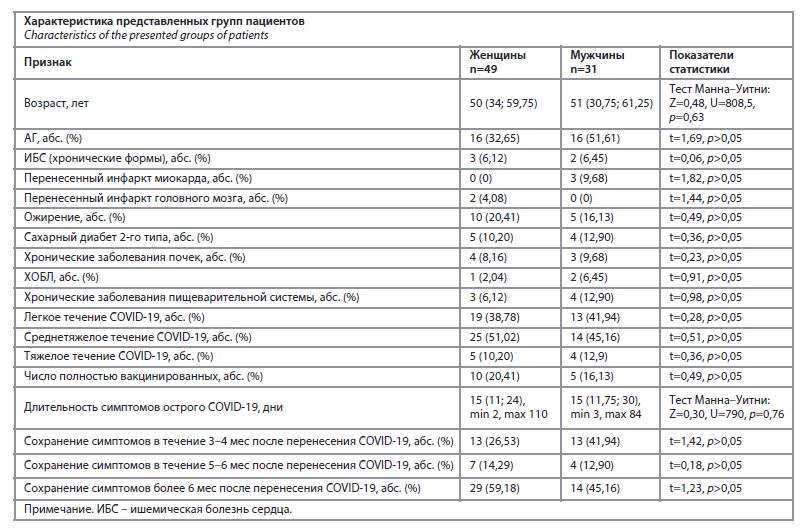 16,13% мужчин (p>0,05). Таким образом, несмотря на бóльшую выраженность клинически значимой астении, мужчины неохотно признаются в этом.
16,13% мужчин (p>0,05). Таким образом, несмотря на бóльшую выраженность клинически значимой астении, мужчины неохотно признаются в этом.
Среди пациентов с астенией (слабостью) обоих полов (n=42) наиболее частой сопутствующей жалобой в ПКС были боли в мышцах и суставах [n=16 (38,10%)], что, очевидно, дополнительно способствует снижению работоспособности и подвижности. Нарушения сна отмечены у подавляющего большинства (78,57%) респондентов этой группы, что также сказывается на бодрствовании и состоянии активности пациентов. Интересно и наблюдение изменения динамики массы тела пациентов с астенией: отмечено снижение массы тела у 24 (57,14%) из 42 пациентов с астенией. При этом статистически значимых различий по данным признакам при сравнении с группой пациентов без клинически значимой астении не получено (p>0,05).
Когнитивные расстройства остаются часто без внимания клиницистов в ПКС, так как не входят в число активных жалоб пациентов. Тем не менее, по данным многочисленных научных публикаций, составляют серьезную проблему для здравоохранения и повседневной активности лиц, перенесших новую коронавирусную инфекцию. Часто в зарубежной литературе для описания этого состояния встречается термин «brain fog» [10]. Весомое значение КД приобретает у молодых взрослых людей, составляющих основную массу трудоспособного населения. Проанализировав многочисленные опросники на выявление когнитивных нарушений, была выбрана шкала МакНера и Кана как наиболее краткая и простая для самостоятельного заполнения пациентами. По результатам суммы 42 балла и более за ответы пациентов констатируется КД, и, чем большее количество баллов пациент набирает, тем более выраженным считается нарушение. В целом КД отмечена практически с одинаковой частотой среди пациентов обоих полов: у 26,53% женщин и 25,81% мужчин (p>0,05). Не получено и статистически значимых различий в тяжести КД между группами пациентов-мужчин [30 (19,25; 43,5)] и женщин [27 (12; 44,5)]; тест Колмогорова–Смирнова: p=0,59, тест Манна–Уитни: U=836,5, Z=0,760, p=0,45). Однако отмечена интересная закономерность: в группе мужчин с астенией (n=22) КД была выявлена у 36,36% лиц, а среди мужчин без астении (n=9) когнитивных нарушений по шкале МакНера и Кана не было выявлено ни у одного пациента (0%); t=3,46, p<0,05. Статистически значимое различие получено и по количеству набранных баллов между группами мужчин с астенией [30,5 (24; 48,5)] и без нее [16 (11,75; 37)]; тест Манна–Уитни: U=45,
Z=2,35, p=0,019. Похожая ситуация наблюдалась и в группе женщин. При сравнении относительных показателей частоты встречаемости КД среди женщин с астенией [n=20 (40%)] и без нее [n=29 (17,24%)] статистические различия получены не были (t=1,71, p>0,05), однако при оценке результатов набранных баллов по шкале МакНера и Кана эти различия установлены. Так, в подгруппе пациенток с клинически значимой астенией Me баллов составила 32 (21; 62), в ее отсутствие – 21 (10,5; 38,75) балл (тест Манна–Уитни: U=394, Z=2,12, p=0,034). При оценке корреляционных взаимосвязей между астенией и КД в группе мужчин получены наиболее статистически значимые результаты (R=0,47, p=0,0081) по сравнению с группой женщин (R=0,24, p=0,092).
Обсуждение
Среди лиц обоих полов отмечаются большое разнообразие клинических симптомов в постковидный период и длительное их сохранение в независимости от тяжести перенесенной новой коронавирусной инфекции.
С наибольшей частотой регистрируются слабость (астения) и нарушения сна. Практически у каждого третьего пациента отмечаются целый ряд сердечно-сосудистых симптомов, а также боли в мышцах и суставах. Повышение АД отмечено более чем в 1/2 случаев у мужчин и женщин, при этом почти у каждой четвертой женщины подъемы АД стали регистрироваться впервые после перенесенного COVID-19. Головные боли в ПКС чаще беспокоят женщин. Данное наблюдение, безусловно, представляет интерес и соответствует результатам, полученным в исследовании испанских коллег, которые проводили отдельное наблюдение за пациентами с головной болью в постковидный период [11]. Следует признать, что в нашей работе в отличие от упоминаемой не учитывалось число лиц, отмечающих данный клинический симптом исходно, до присоединения новой коронавирусной инфекции. Кроме этого, среди женщин частота встречаемости мигрени обычно выше, чем у мужчин, в 2–3 раза.
Слабость (астения) как симптом среди мужчин встречалась в нашем исследовании чаще, чем у женщин, и была наибольшей выраженности. Данный результат также заслуживает внимания и имеет логическое объяснение. Последние годы достаточно подробно изучены и представлены гендерные различия врожденного и приобретенного иммунного ответа [12]. Известно, что женщины в наибольшей степени подвержены аутоиммунным заболеваниям в отличие от мужчин, последние в свою очередь более восприимчивы к инфекциям. Защитную роль в формировании более мощного иммунного ответа у женщин играют эстрогены и Х-хромосома [12]. Эстроген подавляет лимфопоэз Т- и В-клеток, активирует функцию В-клеток и влияет на развитие Т-клеток, а также регулирует ряд цитокинов (таких как ИЛ-1, ИЛ-10 и интерферон γ), которые модулируют иммунные реакции. В том числе и при COVID-19 продемонстрированы преимущества противовирусного и гуморального ответа у женщин по сравнению с мужчинами [12]. Андрогены снижают выраженность иммунного ответа у мужчин, что было отмечено как при изучении новой коронавирусной инфекции, так и на примере гендерных различий в эффективности вакцинации [13, 14]. Астению в ПКС чаще всего связывают с активностью системного воспаления в острый период COVID-19, так как у мужчин в связи с различиями в иммунной системе его выраженность превалирует, это потенциально сказывается на распространенности и выраженности данного симптома именно среди лиц мужского пола.
Частое наблюдение сочетания симптомов астении, болей в мышцах и суставах, потери массы тела помимо роли системного воспаления как ведущего патофизиологического механизма можно рассмотреть с позиции постковидной саркопении. Состояние саркопении характеризуется снижением мышечной силы на фоне потери мышечной массы. В случае первичного процесса это происходит на фоне старения, вторичная саркопения может быть связана с целым рядом патологических процессов, заболеваний, в том числе быть индуцированной COVID-19 [15]. Благодаря наличию рецептора ангиотензинпревращающего фермента 2 на поверхности миоцитов описано прямое повреждающее воздействие SARS-CoV-2 на мышечную ткань, также отмечено и опосредованное воздействие через выработку целого ряда провоспалительных цитокинов (С-реактивный белок, фактор некроза опухоли α, ИЛ-1, ИЛ-6) [15]. Дополнительными факторами повреждения мышечной ткани при новой коронавирусной инфекции могут быть гипоксемия, связанная с первичным поражением легочной ткани, анорексия, часто связанная с нарушением функционирования вкусовых и обонятельных рецепторов, гиподинамия, обусловленная плохим самочувствием и госпитализацией. В настоящее время вопросы постковидной саркопении активно обсуждаются в литературе.
Нарушения сна и КД, выявленные в ПКС, составляют серьезную проблему для пациентов, перенесших новую коронавирусную инфекцию. Полученные в нашей работе результаты согласуются с недавно проведенным исследованием египетских авторов, в котором до 77% пациентов в постковидном периоде могут иметь нарушения сна [16]. Патогенетические механизмы когнитивных нарушений и расстройств сна в ПКС продолжают обсуждаться. Наиболее часто они рассматриваются в плоскости взаимодействия мультисистемного воспалительного повреждения нервной системы при COVID-19 и ряда предрасполагающих факторов, обусловленных клинической картиной инфекции, вызванной SARS-CoV-2 (гипоксемией, сопутствующими психологическими расстройствами, возникновением и сохранением симптомов, нарушающих сон, – кашель, одышка, сердцебиение и др.) [4, 5]. Показано, что пациенты с наиболее тяжелым течением новой коронавирусной инфекции и с большей длительностью госпитализации отмечают более серьезные нарушения когнитивной функции и сна [10].
Заключение
В настоящее время при значительном снижении смертности и изменении клинической картины новой коронавирусной инфекции практикующим врачам приходится все чаще сталкиваться с ее последствиями в виде ПКС. При ведении пациентов с ПКС необходимо помнить о возможных различиях среди мужчин и женщин в клинических проявлениях, базирующихся на гендерных особенностях иммунологического ответа, а также учитывать наличие патологии, предшествующей инфекции COVID-19. Разнообразие симптомов со стороны различных систем и органов может удлинить время дифференциального диагноза и поиска необходимых терапевтических стратегий, поэтому накопление всесторонних сведений о течении ПКС является наиболее актуальной задачей научной медицины во всем мире.
Конфликт интересов. Авторы заявляют об отсутствии конфликта интересов.
Conflict of interests. The authors declare that there is not conflict of interests.
Источник финансирования. Авторы заявляют об отсутствии финансирования при проведении исследования.
Funding source. The authors declare that the study was not funded.
Вклад авторов. В.А. Сергеева – концепция, обработка материала, написание рукописи, редакция статьи; Т.Е. Липатова – концепция, редакция статьи, формирование выводов. Все авторы внесли значимый вклад в проведение исследования и подготовку статьи, прочли и одобрили финальную версию статьи перед публикацией, выразили согласие нести ответственность за все аспекты работы, подразумевающую надлежащее изучение и решение вопросов, связанных
с точностью или добросовестностью любой части работы.
Author contribution. V.A. Sergeeva – concept, data processing, manuscript writing, manuscript editing; T.E. Lipatova – concept, manuscript editing, drawing conclusions.
All authors made a significant contribution to the study and preparation of the article, read and approved the final version of the article before publishing, expressed their consent to be responsible for all aspects of the work involving appropriate analysis and resolution of issues related to the accuracy and integrity of all parts of the work.
Информация об авторах / Information about the authors
Сергеева Виктория Алексеевна – канд. мед. наук, доц. каф. терапии с курсами кардиологии, функциональной диагностики
и гериатрии ФГБОУ ВО «СГМУ им. В.И. Разумовского». E-mail: viktoriasergeeva@mail.ru; ORCID: 0000-0001-8737-4264;
eLibrary SPIN: 8365-0053
Victoriya A. Sergeeva – Cand. Sci. (Med.), Razumovskiy Saratov State Medical University. E-mail: viktoriasergeeva@mail.ru;
ORCID: 0000-0001-8737-4264; eLibrary SPIN: 8365-0053
Липатова Татьяна Евгеньевна – д-р мед. наук, зав. каф. терапии с курсами кардиологии, функциональной диагностики и гериатрии ФГБОУ ВО «СГМУ им. В.И. Разумовского». E-mail: lipatova.t@inbox.ru; ORCID: 0000-0002-7401-9930; eLibrary SPIN: 2483-3578
Tatiana E. Lipatova – D. Sci. (Med.), Razumovskiy Saratov State Medical University. E-mail: lipatova.t@inbox.ru; ORCID: 0000-0002-7401-9930; eLibrary SPIN: 2483-3578
Статья поступила в редакцию / The article received: 30.11.2022
Статья принята к печати / The article approved for publication: 08.12.2022
Клинический разбор в общей медицине №5 2022
Клинические проявления постковидного синдрома у мужчин и женщин
Аннотация
Обоснование. Приблизительно каждый третий пациент, перенесший новую коронавирусную инфекцию, не чувствует себя абсолютно здоровым даже спустя несколько месяцев после заболевания. Наиболее часто у пациентов отмечены слабость (астения), нарушения сна, когнитивная дисфункция и сердечно-сосудистые симптомы. Несмотря на сосуществование многочисленных терминов, описывающих персистирующие постковидные клинические проявления, все они преследуют единую цель – продемонстрировать, что пациенты нуждаются в дальнейшей медицинской помощи и реабилитации после острого периода заболевания.
Цель. Оценка клинических проявлений постковидного синдрома у мужчин и женщин.
Материалы и методы. Проведена оценка клинических проявлений постковидного синдрома у 80 пациентов (49 женщин и 31 мужчины) с помощью клинического интервью и добровольного анонимного анкетирования. Использованы шкала mMRC (Modified Medical Research Council) для оценки выраженности одышки, опросник МакНера и Кана – когнитивной дисфункции, шкалы градации степени тяжести слабости (астении) FSS (Fatigue Severity Scale) и визуальная аналоговая шкала – субъективной оценки утомляемости. Статистическая обработка данных произведена с помощью программы StatPlus 2009 Professional.
Результаты. Среди наиболее часто регистрирующихся жалоб пациентов в постковидный период отмечены астения, нарушения сна, сердечно-сосудистые симптомы, боли в мышцах и суставах. Среди женщин в постковидном синдроме чаще регистрировалась головная боль, среди мужчин – астения. Тяжесть астении также была наиболее выражена среди мужчин. Разнообразные нарушения сна были выявлены у большинства пациентов. Дневная сонливость регистрировалась чаще у мужчин (практически у каждого третьего мужчины); для женщин характерным нарушением сна были кошмарные сновидения, которые у мужчин не отмечались. Примерно с одинаковой частотой среди обоих полов выявлены проблемы с засыпанием и ночные пробуждения. Когнитивные нарушения наблюдались приблизительно у каждого четвертого пациента, перенесшего COVID-19, вне зависимости от пола. Выявлены статистические взаимосвязи астении и когнитивной дисфункции, с большей значимостью проявляющиеся среди мужчин.
Заключение. Многообразие постковидных клинических проявлений среди мужчин и женщин заставляет задуматься о неоднородности и потенциальном суммировании патогенетических механизмов, лежащих в основе каждого симптома. Различия в клинических симптомах постковидного периода среди мужчин и женщин могут быть обусловлены гендерными особенностями иммунного ответа и требуют дальнейшего изучения.
Ключевые слова: постковидный синдром, COVID-19, астения, нарушения сна, когнитивная дисфункция.
Для цитирования: Сергеева В.А., Липатова Т.Е. Клинические проявления постковидного синдрома у мужчин и женщин. Клинический разбор в общей медицине. 2022; 5: 16–22. DOI: 10.47407/kr2022.3.5.00158
Обоснование. Приблизительно каждый третий пациент, перенесший новую коронавирусную инфекцию, не чувствует себя абсолютно здоровым даже спустя несколько месяцев после заболевания. Наиболее часто у пациентов отмечены слабость (астения), нарушения сна, когнитивная дисфункция и сердечно-сосудистые симптомы. Несмотря на сосуществование многочисленных терминов, описывающих персистирующие постковидные клинические проявления, все они преследуют единую цель – продемонстрировать, что пациенты нуждаются в дальнейшей медицинской помощи и реабилитации после острого периода заболевания.
Цель. Оценка клинических проявлений постковидного синдрома у мужчин и женщин.
Материалы и методы. Проведена оценка клинических проявлений постковидного синдрома у 80 пациентов (49 женщин и 31 мужчины) с помощью клинического интервью и добровольного анонимного анкетирования. Использованы шкала mMRC (Modified Medical Research Council) для оценки выраженности одышки, опросник МакНера и Кана – когнитивной дисфункции, шкалы градации степени тяжести слабости (астении) FSS (Fatigue Severity Scale) и визуальная аналоговая шкала – субъективной оценки утомляемости. Статистическая обработка данных произведена с помощью программы StatPlus 2009 Professional.
Результаты. Среди наиболее часто регистрирующихся жалоб пациентов в постковидный период отмечены астения, нарушения сна, сердечно-сосудистые симптомы, боли в мышцах и суставах. Среди женщин в постковидном синдроме чаще регистрировалась головная боль, среди мужчин – астения. Тяжесть астении также была наиболее выражена среди мужчин. Разнообразные нарушения сна были выявлены у большинства пациентов. Дневная сонливость регистрировалась чаще у мужчин (практически у каждого третьего мужчины); для женщин характерным нарушением сна были кошмарные сновидения, которые у мужчин не отмечались. Примерно с одинаковой частотой среди обоих полов выявлены проблемы с засыпанием и ночные пробуждения. Когнитивные нарушения наблюдались приблизительно у каждого четвертого пациента, перенесшего COVID-19, вне зависимости от пола. Выявлены статистические взаимосвязи астении и когнитивной дисфункции, с большей значимостью проявляющиеся среди мужчин.
Заключение. Многообразие постковидных клинических проявлений среди мужчин и женщин заставляет задуматься о неоднородности и потенциальном суммировании патогенетических механизмов, лежащих в основе каждого симптома. Различия в клинических симптомах постковидного периода среди мужчин и женщин могут быть обусловлены гендерными особенностями иммунного ответа и требуют дальнейшего изучения.
Ключевые слова: постковидный синдром, COVID-19, астения, нарушения сна, когнитивная дисфункция.
Для цитирования: Сергеева В.А., Липатова Т.Е. Клинические проявления постковидного синдрома у мужчин и женщин. Клинический разбор в общей медицине. 2022; 5: 16–22. DOI: 10.47407/kr2022.3.5.00158
Clinical manifestations of post-COVID-19 syndrome in men and women
Victoriya A. Sergeeva, Tatiana E. Lipatova
Abstract
Background. Approximately every third patient who passed new coronavirus infection doesn’t feel absolutely healthy even few months ago after disease. Most constantly have noted fatigue (asthenia), sleep disorders, cognitive dysfunction and cardiovascular symptoms. In spite of coexistence different terms which describe persistent post-COVID-19 clinical manifestations, all of them serve the only goal – to demonstrate that the patients need in continuing medical care and rehabilitation after acute period of disease.
Aim. Assessment of clinical manifestations of bridge syndrome in men and women.
Materials and methods. Clinical manifestations of post-COVID-19 syndrome were assessed in 80 patients (49 women and 31 men) using a clinical interview and voluntary anonymous questionnaire. The mMRC (Modified Medical Research Council) scale was used to assess the severity of dyspnea, the McNair and Kahn questionnaire – for cognitive dysfunction, the FSS (Fatigue Severity Scale) – for the severity of fatigue (asthenia), and the visual analogue scale (VAS) was used for subjective assessment of fatigue. Statistical data processing was performed using the StatPlus 2009 Professional program.
Results. Among the most frequently reported complaints of patients in the post-COVID period were fatigue, sleep disturbances, cardiovascular symptoms, pain in muscles and joints. Among women in the post-COVID syndrome, headache was more often recorded, among men – fatigue. The severity of fatigue (asthenia) was also most pronounced among men. A variety of sleep disorders were identified in the vast majority of patients. Daytime sleepiness was recorded more often in men (almost every third man); for women, a characteristic sleep disorder was nightmares, which were not observed in men. Approximately with the same frequency among both sexes, problems with falling asleep and nocturnal awakenings were revealed. Cognitive impairment was observed in approximately one in four patients who had COVID-19, regardless of gender. Statistical relationships between asthenia and cognitive dysfunction were revealed, which are more significant among men.
Conclusion. The multiplicity of post-COVID clinical manifestations among men and women raises questions about the heterogeneity and potential summation of the pathogenic mechanisms underlying each symptom. Differences in the clinical symptoms of the post-COVID-19 period among men and women may can be explained by gender-specific immune response and require further study.
Key words: post-COVID-19 syndrome, COVID-19, fatigue, sleep disorders, cognitive dysfunction.
For citation: Sergeeva V.A., Lipatova T.E. Clinical manifestations of post-COVID-19 syndrome in men and women. Clinical analysis in general medicine. 2022; 5: 16–22. DOI: 10.47407/kr2022.3.5.00158
Введение
По мере накопления клинических данных при наблюдении за перенесшими новую коронавирусную инфекцию пациентами в связи с сохранением большого количества симптомов, несмотря на окончание острого периода заболевания, возникла необходимость внедрения новой терминологии. В связи с этим в различных научных источниках стали появляться определения: long COVID-19, long-haul COVID-19, post-acute COVID-19, chronic COVID-19 и другие, отличающиеся сроками манифестации и продолжительностью клинических проявлений после перенесения инфекции, вызванной вирусом SARS-CoV-2.
Впервые на сохраняющиеся симптомы после острой фазы заболевания новой коронавирусной инфекцией обратили внимание члены исследовательской группы пациентов-ученых (The Patient-Led Research Collaborative) в апреле 2020 г. [1]. Следующим значимым этапом было внедрение в 2021 г. Всемирной организацией здравоохранения общего понятия «постковидное состояние», которое принято определять как сочетание симптомов, которые развиваются в течение 12 нед после выздоровления от COVID-19, длятся не менее
2 мес и не объясняются наличием альтернативных заболеваний. Симптомы могут возникать впервые после выздоровления от острого эпизода COVID-19 или сохраняться после первоначального заболевания. Симптомы также могут изменяться или рецидивировать с течением времени [2]. В настоящее время все большее распространение в отечественной и зарубежной литературе приобретает термин «постковидный синдром» – ПКС (post-COVID-19 syndrome), в целом соответствующий определению постковидного состояния. По мнению разных авторов, частота ПКС варьирует от 10–35% у получавших амбулаторное лечение до 85% среди пациентов, проходивших стационарное лечение по поводу новой коронавирусной инфекции, что обусловливает актуальность его дальнейшего изучения [3].
По крайней мере несколько ведущих патогенетических механизмов обсуждается в качестве основных в развитии ПКС. Во-первых, вирусоспецифические патофизиологические изменения, обусловленные механизмом проникновения вируса в клетки хозяина; во-вторых, иммунологические отклонения и воспалительные повреждения в ответ на острую инфекцию; в-третьих, ожидаемые последствия постреанимационного синдрома среди пациентов, находившихся на лечении в отделении неотложной и интенсивной терапии [4]. Предполагается, что наряду с прямым повреждающим воздействием вируса длительное системное воспаление может играть ключевую роль в происхождении различных неврологических симптомов у пациентов, перенесших COVID-19: слабость (астения), нарушения сна, когнитивная дисфункция (КД) [5, 6]. Эти же механизмы могут быть ответственны за миокардиальное повреждение и развитие различных сердечно-сосудистых симптомов в постковидный период [7]. Отмечены случаи и так называемого мультисистемного воспалительного синдрома, ассоциированного с COVID-19, первоначально описанного среди детей [8]. В отсутствие позитивного теста полимеразной цепной реакции на коронавирус у таких пациентов наблюдаются высокие титры провоспалительных цитокинов (С-реактивный белок, фибриноген, интерлейкин – ИЛ-6 и др.) и широкий спектр полиорганных клинических проявлений (сердечно-сосудистых, гастроэнтерологических, дерматологических, неврологических) [8]. В настоящее время неизвестен временной интервал манифеста мультисистемного воспалительного синдрома от начала заболевания у пациентов с новой коронавирусной инфекцией, поэтому трудно судить о том, следует ли его рассматривать в клинической картине острого периода COVID-19 или относить уже к ПКС. Среди других значимых патофизиологических механизмов ПКС весомая роль принадлежит микрососудистому повреждению, ишемии, тромбоэмболизму, оксидативному стрессу [4]. Многие клинические симптомы в постковидном периоде связывают с длительным малоподвижным состоянием и так называемым постреанимационным синдромом, которые напрямую связаны с тяжестью перенесенной новой коронавирусной инфекции [4]. Однако далеко не всегда тяжесть заболевания и длительность COVID-19 определяют течение ПКС. Многие пациенты, перенесшие инфекцию в легкой форме, без поражения легких, спустя несколько месяцев после выздоровления продолжают испытывать различные симптомы [3]. Среди наиболее часто регистрирующихся клинических проявлений отмечены слабость или астения (слабость, утомляемость), КД, нарушения сна, одышка, нарушения сердечного ритма.
Многообразие постковидных симптомов, снижение трудоспособности и в целом качества жизни значительного числа людей, в том числе молодого возраста, диктуют необходимость дальнейшего изучения проблемы с целью разработки возможных подходов реабилитации и скорейшего восстановления их здоровья.
Цель исследования – изучение и сравнительная оценка наиболее распространенных постковидных клинических проявлений среди пациентов обоих полов.
Материалы и методы
Проведено клиническое интервью и анонимное прямое анкетирование 80 пациентов (31 мужчины и 49 женщин), перенесших новую коронавирусную инфекцию не менее 12 нед назад (согласно критериям ПКС), у которых отмечались различные клинические проявления на момент проведения исследования. Все пациенты дали добровольное согласие на участие в исследовании, которое проводилось с соблюдением этических норм Хельсинкской декларации. Изучена исходная полиморбидность пациентов, принявших участие в исследовании. Критериями исключения стали наличие старческого возраста, выраженных интеллектуально-мнестических расстройств, обострение хронических заболеваний, ревматическая патология, острый коронарный синдром, онкопатология и получение химиотерапии. Для оценки ряда симптомов использовались валидизированные в Российской Федерации шкалы. Одышка оценивалась по шкале mMRC (Modified Medical Research Council). Для оценки когнитивных нарушений использовался опросник МакНера и Кана. При наборе респондентом 42 баллов и более констатировалась КД. В дополнение подробно изучены проявления астенического синдрома с использованием шкалы степени тяжести астении FSS (Fatigue Severity Scale) и визуальной аналоговой шкалы собственной оценки респондентами проявлений утомляемости, при которой респонденты могли сами оценить тяжесть своей астении по 10-балльной шкале, где 1 – минимальный уровень, 10 – максимальный. При интерпретации результатов шкалы FSS пороговым значением было 36 баллов, при наборе
36 баллов и более констатировалась клинически значимая слабость (астения).
Статистическая обработка данных производилась с помощью программы StatPlus 2009 Professional. При оценке характера распределения количественных признаков использовали критерии Колмогорова–Смирнова и Шапиро–Уилка. Все количественные показатели в работе имеют ненормальное распределение и представлены в виде медианы (Ме) и интерквартильного размаха – значения 25 и 75-го процентилей [Ме (25р; 75р)]. При сравнении независимых выборок использовали тест Манна–Уитни и тест Колмогорова–Смирнова в зависимости от величины сравниваемых групп. Для выявления и оценки тесноты связи между двумя рядами сопоставляемых количественных показателей использовался коэффициент ранговой корреляции Спирмена. При сравнении относительных показателей между группами использовался t-критерий Стьюдента. Статистически значимым было принято p-значение <0,05.
Результаты
Обследованы 80 пациентов (49 женщин и 31 мужчина), у которых более 12 нед после перенесения новой коронавирусной инфекции сохранялись различные симптомы. Группы пациентов были сопоставимы по возрасту, тяжести перенесенной инфекции COVID-19, наличию сопутствующих заболеваний. Полная характеристика сравниваемых групп отражена в таблице. Как видно из представленных данных, большая часть обследованных пациентов перенесли новую коронавирусную инфекцию в легкой и среднетяжелой форме. При этом отмечается длительное сохранение постковидных симптомов, вплоть до 6 мес и более. Проведена сравнительная оценка наиболее часто встречающихся симптомов у мужчин и женщин в
постковидный период. Результаты представлены на рис. 1. Как видно исходя из полученных результатов, доминирующими симптомами в обеих группах оказались нарушения сна и слабость. В группе
Структура нарушений сна в исследуемых группах подробно представлена на рис. 2. Как видно из диаграммы, сложности с засыпанием отмечены практически в равных долях среди мужчин (29,03%) и женщин (20,42%); p>0,05. Просыпаются часто среди ночи и отмечают недосыпание 16,13% мужчин и 22,45% женщин без статистически значимых различий (p>0,05). Кошмарные сновидения, напротив, отмечены среди жалоб только у женщин (12,24%), у мужчин данные расстройства сна не выявлены (0%); p<0,05. Возможно, это обстоятельство является следствием большей эмоциональности женщин и часто сопутствующей ей тревожности, связанной с тяжелым заболеванием, в данном случае COVID-19. Дневная сонливость была, напротив, присуща в большей степени мужчинам (32,26%) по сравнению с женщинами (12,24%); p<0,05. Такие данные представляют интерес, так как не могут быть объяснены наличием сопутствующей патологии, влияющей на этот симптом. В исследуемой группе мужчин было только 2 пациента с хронической обструктивной болезнью легких (ХОБЛ), которая при тяжелом течении либо обострении может быть причиной тяжелой гипоксемии и приводить в том числе к дневной сонливости. Кроме этого, в группе мужчин было сопоставимое с группой женщин число лиц с ожирением, для него характерен синдром альвеолярной гиповентиляции, при котором дневная сонливость является наиболее характерным симптомом [9].
Как один из ведущих симптомов в ПКС – слабость (астения) была проанализирована в каждой группе более подробно. С помощью шкалы-опросника FSS при наборе 36 баллов и более астения трактуется как клинически значимая и, чем больше баллов набирает пациент, тем тяжелее его астеническое состояние. В группе женщин Me баллов составила 28 (9; 53), у мужчин – 39 (31,75; 54); тест Колмогорова–Смирнова: p=0,0315; тест Манна–Уитни: U=943, Z=1,812, p=0,07. Таким образом, установлено, что среди мужчин отмечается не только бóльшая распространенность этого симптома в ПКС, но и бóльшая его выраженность. По визуальной аналоговой шкале среди женщин с клинически значимой астенией Ме баллов составила 5 (3; 7), среди мужчин – 5 (4; 7); статистически значимых различий между группами не получено: тест Манна–Уитни – U=863,5, Z=1,027, p=0,30. На максимальное число баллов (от 8 до 10) свою астению оценили 18,37% женщин и
Среди пациентов с астенией (слабостью) обоих полов (n=42) наиболее частой сопутствующей жалобой в ПКС были боли в мышцах и суставах [n=16 (38,10%)], что, очевидно, дополнительно способствует снижению работоспособности и подвижности. Нарушения сна отмечены у подавляющего большинства (78,57%) респондентов этой группы, что также сказывается на бодрствовании и состоянии активности пациентов. Интересно и наблюдение изменения динамики массы тела пациентов с астенией: отмечено снижение массы тела у 24 (57,14%) из 42 пациентов с астенией. При этом статистически значимых различий по данным признакам при сравнении с группой пациентов без клинически значимой астении не получено (p>0,05).
Когнитивные расстройства остаются часто без внимания клиницистов в ПКС, так как не входят в число активных жалоб пациентов. Тем не менее, по данным многочисленных научных публикаций, составляют серьезную проблему для здравоохранения и повседневной активности лиц, перенесших новую коронавирусную инфекцию. Часто в зарубежной литературе для описания этого состояния встречается термин «brain fog» [10]. Весомое значение КД приобретает у молодых взрослых людей, составляющих основную массу трудоспособного населения. Проанализировав многочисленные опросники на выявление когнитивных нарушений, была выбрана шкала МакНера и Кана как наиболее краткая и простая для самостоятельного заполнения пациентами. По результатам суммы 42 балла и более за ответы пациентов констатируется КД, и, чем большее количество баллов пациент набирает, тем более выраженным считается нарушение. В целом КД отмечена практически с одинаковой частотой среди пациентов обоих полов: у 26,53% женщин и 25,81% мужчин (p>0,05). Не получено и статистически значимых различий в тяжести КД между группами пациентов-мужчин [30 (19,25; 43,5)] и женщин [27 (12; 44,5)]; тест Колмогорова–Смирнова: p=0,59, тест Манна–Уитни: U=836,5, Z=0,760, p=0,45). Однако отмечена интересная закономерность: в группе мужчин с астенией (n=22) КД была выявлена у 36,36% лиц, а среди мужчин без астении (n=9) когнитивных нарушений по шкале МакНера и Кана не было выявлено ни у одного пациента (0%); t=3,46, p<0,05. Статистически значимое различие получено и по количеству набранных баллов между группами мужчин с астенией [30,5 (24; 48,5)] и без нее [16 (11,75; 37)]; тест Манна–Уитни: U=45,
Z=2,35, p=0,019. Похожая ситуация наблюдалась и в группе женщин. При сравнении относительных показателей частоты встречаемости КД среди женщин с астенией [n=20 (40%)] и без нее [n=29 (17,24%)] статистические различия получены не были (t=1,71, p>0,05), однако при оценке результатов набранных баллов по шкале МакНера и Кана эти различия установлены. Так, в подгруппе пациенток с клинически значимой астенией Me баллов составила 32 (21; 62), в ее отсутствие – 21 (10,5; 38,75) балл (тест Манна–Уитни: U=394, Z=2,12, p=0,034). При оценке корреляционных взаимосвязей между астенией и КД в группе мужчин получены наиболее статистически значимые результаты (R=0,47, p=0,0081) по сравнению с группой женщин (R=0,24, p=0,092).
Обсуждение
Среди лиц обоих полов отмечаются большое разнообразие клинических симптомов в постковидный период и длительное их сохранение в независимости от тяжести перенесенной новой коронавирусной инфекции.
С наибольшей частотой регистрируются слабость (астения) и нарушения сна. Практически у каждого третьего пациента отмечаются целый ряд сердечно-сосудистых симптомов, а также боли в мышцах и суставах. Повышение АД отмечено более чем в 1/2 случаев у мужчин и женщин, при этом почти у каждой четвертой женщины подъемы АД стали регистрироваться впервые после перенесенного COVID-19. Головные боли в ПКС чаще беспокоят женщин. Данное наблюдение, безусловно, представляет интерес и соответствует результатам, полученным в исследовании испанских коллег, которые проводили отдельное наблюдение за пациентами с головной болью в постковидный период [11]. Следует признать, что в нашей работе в отличие от упоминаемой не учитывалось число лиц, отмечающих данный клинический симптом исходно, до присоединения новой коронавирусной инфекции. Кроме этого, среди женщин частота встречаемости мигрени обычно выше, чем у мужчин, в 2–3 раза.
Слабость (астения) как симптом среди мужчин встречалась в нашем исследовании чаще, чем у женщин, и была наибольшей выраженности. Данный результат также заслуживает внимания и имеет логическое объяснение. Последние годы достаточно подробно изучены и представлены гендерные различия врожденного и приобретенного иммунного ответа [12]. Известно, что женщины в наибольшей степени подвержены аутоиммунным заболеваниям в отличие от мужчин, последние в свою очередь более восприимчивы к инфекциям. Защитную роль в формировании более мощного иммунного ответа у женщин играют эстрогены и Х-хромосома [12]. Эстроген подавляет лимфопоэз Т- и В-клеток, активирует функцию В-клеток и влияет на развитие Т-клеток, а также регулирует ряд цитокинов (таких как ИЛ-1, ИЛ-10 и интерферон γ), которые модулируют иммунные реакции. В том числе и при COVID-19 продемонстрированы преимущества противовирусного и гуморального ответа у женщин по сравнению с мужчинами [12]. Андрогены снижают выраженность иммунного ответа у мужчин, что было отмечено как при изучении новой коронавирусной инфекции, так и на примере гендерных различий в эффективности вакцинации [13, 14]. Астению в ПКС чаще всего связывают с активностью системного воспаления в острый период COVID-19, так как у мужчин в связи с различиями в иммунной системе его выраженность превалирует, это потенциально сказывается на распространенности и выраженности данного симптома именно среди лиц мужского пола.
Частое наблюдение сочетания симптомов астении, болей в мышцах и суставах, потери массы тела помимо роли системного воспаления как ведущего патофизиологического механизма можно рассмотреть с позиции постковидной саркопении. Состояние саркопении характеризуется снижением мышечной силы на фоне потери мышечной массы. В случае первичного процесса это происходит на фоне старения, вторичная саркопения может быть связана с целым рядом патологических процессов, заболеваний, в том числе быть индуцированной COVID-19 [15]. Благодаря наличию рецептора ангиотензинпревращающего фермента 2 на поверхности миоцитов описано прямое повреждающее воздействие SARS-CoV-2 на мышечную ткань, также отмечено и опосредованное воздействие через выработку целого ряда провоспалительных цитокинов (С-реактивный белок, фактор некроза опухоли α, ИЛ-1, ИЛ-6) [15]. Дополнительными факторами повреждения мышечной ткани при новой коронавирусной инфекции могут быть гипоксемия, связанная с первичным поражением легочной ткани, анорексия, часто связанная с нарушением функционирования вкусовых и обонятельных рецепторов, гиподинамия, обусловленная плохим самочувствием и госпитализацией. В настоящее время вопросы постковидной саркопении активно обсуждаются в литературе.
Нарушения сна и КД, выявленные в ПКС, составляют серьезную проблему для пациентов, перенесших новую коронавирусную инфекцию. Полученные в нашей работе результаты согласуются с недавно проведенным исследованием египетских авторов, в котором до 77% пациентов в постковидном периоде могут иметь нарушения сна [16]. Патогенетические механизмы когнитивных нарушений и расстройств сна в ПКС продолжают обсуждаться. Наиболее часто они рассматриваются в плоскости взаимодействия мультисистемного воспалительного повреждения нервной системы при COVID-19 и ряда предрасполагающих факторов, обусловленных клинической картиной инфекции, вызванной SARS-CoV-2 (гипоксемией, сопутствующими психологическими расстройствами, возникновением и сохранением симптомов, нарушающих сон, – кашель, одышка, сердцебиение и др.) [4, 5]. Показано, что пациенты с наиболее тяжелым течением новой коронавирусной инфекции и с большей длительностью госпитализации отмечают более серьезные нарушения когнитивной функции и сна [10].
Заключение
В настоящее время при значительном снижении смертности и изменении клинической картины новой коронавирусной инфекции практикующим врачам приходится все чаще сталкиваться с ее последствиями в виде ПКС. При ведении пациентов с ПКС необходимо помнить о возможных различиях среди мужчин и женщин в клинических проявлениях, базирующихся на гендерных особенностях иммунологического ответа, а также учитывать наличие патологии, предшествующей инфекции COVID-19. Разнообразие симптомов со стороны различных систем и органов может удлинить время дифференциального диагноза и поиска необходимых терапевтических стратегий, поэтому накопление всесторонних сведений о течении ПКС является наиболее актуальной задачей научной медицины во всем мире.
Конфликт интересов. Авторы заявляют об отсутствии конфликта интересов.
Conflict of interests. The authors declare that there is not conflict of interests.
Источник финансирования. Авторы заявляют об отсутствии финансирования при проведении исследования.
Funding source. The authors declare that the study was not funded.
Вклад авторов. В.А. Сергеева – концепция, обработка материала, написание рукописи, редакция статьи; Т.Е. Липатова – концепция, редакция статьи, формирование выводов. Все авторы внесли значимый вклад в проведение исследования и подготовку статьи, прочли и одобрили финальную версию статьи перед публикацией, выразили согласие нести ответственность за все аспекты работы, подразумевающую надлежащее изучение и решение вопросов, связанных
с точностью или добросовестностью любой части работы.
Author contribution. V.A. Sergeeva – concept, data processing, manuscript writing, manuscript editing; T.E. Lipatova – concept, manuscript editing, drawing conclusions.
All authors made a significant contribution to the study and preparation of the article, read and approved the final version of the article before publishing, expressed their consent to be responsible for all aspects of the work involving appropriate analysis and resolution of issues related to the accuracy and integrity of all parts of the work.
Информация об авторах / Information about the authors
Сергеева Виктория Алексеевна – канд. мед. наук, доц. каф. терапии с курсами кардиологии, функциональной диагностики
и гериатрии ФГБОУ ВО «СГМУ им. В.И. Разумовского». E-mail: viktoriasergeeva@mail.ru; ORCID: 0000-0001-8737-4264;
eLibrary SPIN: 8365-0053
Victoriya A. Sergeeva – Cand. Sci. (Med.), Razumovskiy Saratov State Medical University. E-mail: viktoriasergeeva@mail.ru;
ORCID: 0000-0001-8737-4264; eLibrary SPIN: 8365-0053
Липатова Татьяна Евгеньевна – д-р мед. наук, зав. каф. терапии с курсами кардиологии, функциональной диагностики и гериатрии ФГБОУ ВО «СГМУ им. В.И. Разумовского». E-mail: lipatova.t@inbox.ru; ORCID: 0000-0002-7401-9930; eLibrary SPIN: 2483-3578
Tatiana E. Lipatova – D. Sci. (Med.), Razumovskiy Saratov State Medical University. E-mail: lipatova.t@inbox.ru; ORCID: 0000-0002-7401-9930; eLibrary SPIN: 2483-3578
Статья поступила в редакцию / The article received: 30.11.2022
Статья принята к печати / The article approved for publication: 08.12.2022
