Клинический разбор в общей медицине №2 2023
Abstract
The paper presents current data on the impact of endogenous and exogenous triggers on the clinical manifestations of acne. The major triggers are discussed in detail. The importance of genetic factors for the development of dermatosis is reported. The role of hormonal factor, hyperandrogenism, in the pathogenesis of the disease is displayed. The data on the adverse effects of stress on the course of acne are provided. The association of the diet with the acne exacerbation/onset is exposed. The negative role of smoking in triggering the non-inflammatory type acne is reported.
Keywords: acne, inflammation, Western diet, hyperandrogenism, polycystic ovary syndrome, stress.
For citation: Kail-Goryachkina M.V. The role of endogenous and exogenous triggers in the development of acne. Clinical review for general practice. 2023; 4 (2): 90–96. DOI: 10.47407/kr2023.4.2.00210
Акне является одним из наиболее распространенных хронических воспалительных заболеваний кожи, которое проявляется поражением сально-волосяного аппарата; дерматоз характеризуется появлением открытых и закрытых комедонов, папул, пустул и узлов. Развивающийся в результате осложнения акне – симптомокомплекс постакне представляет собой в большинстве случаев вторичную гиперпигментацию (36%), неравномерную текстуру кожи (30%), рубцы (26%), а также эритематозные пятна (6%), атеромы и милиумы (2%) [1, 2].
По данным глобального исследования бремени болезней (Global Burden of Disease Study), проведенного в 2010 г., акне страдают примерно 650 млн человек во всем мире. По показателю распространенности воспалительных заболеваний кожи дерматоз занимает
8-е место. В предпубертатном или пубертатном периоде в той или иной степени с проблемой акне сталкиваются 90% девушек и 100% юношей. У девушек угревые высыпания появляются раньше, чем у юношей, нередко незадолго до начала первой менструации. У юношей акне дебютирует позже, но носит более тяжелый и распространенный характер. В 12-летнем возрасте акне наблюдается у 37,1% девочек и 15,4% мальчиков, в 16 лет – уже у 38,8 и 53,3% соответственно, а вот для acne tarda (поздних угрей) характерно существенное преобладание женщин 82,1% против 17,9%, недаром за рубежом существует устоявшаяся аббревиатура – adult female acne, характеризующая данную группу пациентов [2–7].
Патогенез акне состоит из патологического взаимодействия между несколькими процессами, такими как воспаление, фолликулярная гиперкератинизация (приводящая к «закупорке» устья сально-волосяного фолликула), гиперпродукция секрета сальных желез, микробная колонизация Сutibacterium acnes (филотипа IA1 риботипов RT4 и RT5) с формированием биопленок, а также гормонального фактора (абсолютной или периферической гиперандрогении) [8–10].
В настоящее время доказано, что важнейшем звеном в патогенезе акне является воспаление. В 28% случаев воспаление образуется de novo, минуя стадию комедонов. Данный постулат подтверждается в работе A. Jeremy и соавт., которые продемонстрировали, что воспалительный процесс в той или иной мере наблюдался при всех проявлениях и стадиях болезни: от непораженной кожи в доклинической стадии (характеризующейся образованием микрокомедонов) до симптомокомплекса постакне. Основополагающая роль при этом отводится провоспалительному цитокину – интерлейкину (ИЛ)-1, экспрессия которого значительно увеличивается в пораженной коже независимо от наличия или отсутствия С. аcnes. Немаловажную роль в развитии воспалительного процесса играют и другие провоспалительные цитокины, такие как фактор некроза опухоли (ФНО), ИЛ-6, ИЛ-8, ИЛ-10 и ИЛ-12, а также интегрины, матриксные металлопротеиназы (matrix metalloproteinases, MMP), макрофаги, дендритные клетки и CD4+ T-клетки [11, 12].
В норме кератиноциты и себоциты постоянно экспрессируют провоспалительные цитокины, однако под действием различных триггерных факторов происходят их индукция и гиперсекреция. C. acnes является комменсальным липофильным факультативным анаэробным микроорганизмом кожи человека и служит одним из основных триггеров для развития воспалительной реакции посредством активации врожденного или приобретенного иммунного ответа [12, 13].
Необходимо также помнить, что способность C. acnes к образованию биопленок как сложных полимикробных ассоциаций способствует формированию устойчивости к защитным механизмам хозяина и лекарственным препаратам, а также может служить резервуаром для иных патогенных микроорганизмов, таких как Staphylococcus aureus, что может существенно утяжелить течение акне. Адгезионное свойство матрицы биопленки C. acnes приводит к усилению сцепления корнеоцитов в области воронки сально-волосяного фолликула за счет выделения «биологического клея», которым является гликокаликсный полимер. Данное свойство микроорганизма играет важную роль в образовании сально-роговой пробки и развитии комедоногенеза [12, 14].
Среди клинических проявлений акне чаще (в 70–80% случаев) встречается среднетяжелая – папуло-пустулезная форма. Легкая комедональная форма и самое тяжелое проявление дерматоза – конглобатные угри – отмечаются значительно реже (у 15–20% больных) [15, 16].
При обзоре различных эпидемиологических исследований за период последних 20 лет (1999–2021 гг.) выявлено, что на распространенность, риск возникновения и утяжеления течения акне оказывают влияние различные эндогенные и экзогенные триггеры. К эндогенным триггерам относят генетический фактор и гиперандрогению. К экзогенным – стресс, рацион питания и диетические предпочтения, курение, прием ряда лекарственных препаратов (анаболические стероиды, противотуберкулезные препараты, глюкокортикоиды и др.), травматизацию кожи (наиболее часто вследствие выдавливания пациентами акне-элементов), нерациональный уход за кожей, в том числе и вследствие неадекватного назначения косметологических процедур, экологический фактор (негативное воздействие внешней среды: загрязнение кожи маслами, керосином, бензином, пылью производственного происхождения, УФ-облучение) [8, 15, 17–20].
Несмотря на то что конкретные генетические маркеры акне пока не найдены, а обнаружены лишь полиморфизмы генов, регулирующих врожденную иммунную систему кожи и метаболизм стероидных гормонов, акне считается генетически обусловленным наследственным мультифакториальным заболеванием с высоким семейным накоплением. Наследственная предрасположенность выявляется примерно в 59,9–81,1% случаев. Установлено, что развитие тяжелых, длительно текущих, торпидных форм акне наиболее вероятно, если в анамнезе заболевание имеется у обоих родителей [21, 22].
В настоящие время проводятся различные генетические исследования, посвященные акне. Наиболее перспективным является поиск генов-кандидатов, т.е. генов, связанных с акне. Очевидно, что в развитии акне принимает участие множество генов. Одни из них ответственны за развитие гиперандрогении, или патологической реакции на нормальное содержание андрогенов. Получены данные, что к развитию тяжелых форм акне приводит мутация гена CYP17-34C, кодирующего цитохром P450c17a, который является одним из ключевых ферментов в биосинтезе андрогенов. Доказано, что полиморфизм гена ангиотензинпревращающего фермента – АСЕ (делеция/включение) связан с тяжелыми формами акне с отягощенным семейным анамнезом. Было обнаружено, что короткая длина повторения гена CAG и специфические галотипы андрогенного рецептора связаны с риском развития акне и, следовательно, могут рассматриваться как достоверный маркер предрасположенности к данному поражению кожи. Полиморфизм гена инсулиноподобного фактора роста –
IGF-1, состоящего из вариабельных повторов цитозина и аденозина, влияет на эксперссию IGF-1 и на тяжесть течения дерматоза у взрослых женщин, а полиморфизм гена CYT17-34T в форме гомозиготы был обнаружен у пациентов мужского пола с тяжелыми формами акне [15, 23–26].
Исследования по распределению и степени тяжести акне среди различных популяций указывают на этнические особенности заболевания. Акне наиболее подвержены европейцы (29%) и афроамериканцы (25%), дерматоз развивается реже (10%) и протекает в более легкой форме у японцев и китайцев. Интересными наблюдениями, подтверждающими важную роль внешних и внутренних факторов в возникновении, развитии и утяжелении течения акне, являются популяции, полностью свободные от этого дерматоза. К ним относятся эскимосы, жители острова Окинавы, индейцы, у которых частота встречаемости акне равна нулю. Данный феномен можно объяснить сочетанием различных внешних и внутренних факторов, таких как окружающая среда, пищевой рацион (натуральные продукты питания, полученные в результате охоты и собирательства), на который не оказала влияния западная диета, генетическая разнородность данных популяций и западного общества [15, 27, 28].
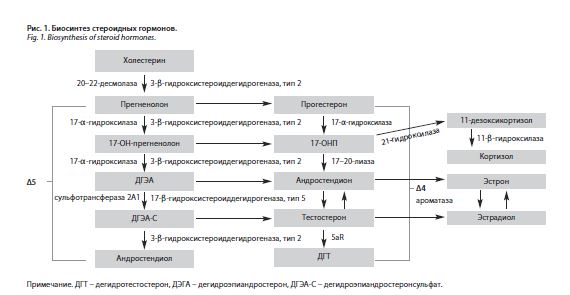 Под гиперандрогенией понимают нарушения синтеза, метаболизма и транспорта андрогенов в организме человека. Исходным соединением для биосинтеза андрогенов, как и других стероидных гормонов, является стероидный спирт холестерин, который поступает в организм человека с продуктами животного происхождения или синтезируется в печени. Синтез стероидов осуществляется по двум путям: 4-й дельта-путь происходит в яичниках (клетки внутренней теки и стромы), 5-й дельта-путь в сетчатой зоне коры надпочечников (рис. 1). Основными яичниковыми андрогенами являются тестостерон и андростендион, надпочечниковыми – дегидроэпиандростерон (ДЭГА) и дегидроэпиандростеронсульфат (ДГЭА-С). Продукцию яичниковых андрогенов стимулирует лютеинизирующий гормон, а надпочечниковых – адренокортикотропный гормон (АКТГ) [8, 29].
Под гиперандрогенией понимают нарушения синтеза, метаболизма и транспорта андрогенов в организме человека. Исходным соединением для биосинтеза андрогенов, как и других стероидных гормонов, является стероидный спирт холестерин, который поступает в организм человека с продуктами животного происхождения или синтезируется в печени. Синтез стероидов осуществляется по двум путям: 4-й дельта-путь происходит в яичниках (клетки внутренней теки и стромы), 5-й дельта-путь в сетчатой зоне коры надпочечников (рис. 1). Основными яичниковыми андрогенами являются тестостерон и андростендион, надпочечниковыми – дегидроэпиандростерон (ДЭГА) и дегидроэпиандростеронсульфат (ДГЭА-С). Продукцию яичниковых андрогенов стимулирует лютеинизирующий гормон, а надпочечниковых – адренокортикотропный гормон (АКТГ) [8, 29].
Кроме того, андрогены (около 50%) образуются за счет периферического метаболизма стероидов, в том числе и в коже, недаром немецкий ученый Шмитц назвал кожу самой большой эндокринной железой в организме. Периферическое взаимопревращение яичниковых и надпочечниковых гормонов ведет к трансформации низкоактивных андрогенов в высокоактивные. Так, андростендион превращается в тестостерон, который, в свою очередь, в коже под действием фермента 5-α-редуктазы метаболизируется в свой более сильный метаболит дегидротестостерон (ДГТ), оказывающий основное андрогенное действие в тканях-мишенях [16, 29].
Гиперандрогения служит одной из визитных карточек эндокринного неблагополучия женской репродуктивной сферы и клинически проявляется несколькими группами признаков, отражающих андрогенизацию организма: андрогензависимая дермопатия, дефеминизация, маскулинизация и вирилизация наружных половых органов [8, 16, 29].
По происхождению гиперандрогения может быть:
• истинной (абсолютной) – из овариального или надпочечникового источника, связана с повышением уровня андрогенов в крови. Истинная гиперандрогения может иметь функциональный или опухолевый генез;
• транспортной (снижение секреции половых стероидов, связывающих глобулины – ПССГ).
• периферической (рецепторной), связанной с повышенной чувствительностью андрогеновых рецепторов – АР к андрогенам при нормальном их количестве;
• метаболической, связанной с повышенной активностью фермента 5-α-редуктазы;
• ятрогенной, связанной с приемом лекарственных средств;
• гиперандрогения при системных заболеваниях и заболеваниях гипоталамо-гипофизарной системы (сахарный диабет 2-го типа и ожирение, болезнь Иценго–Кушинга, акромегалия и др.)
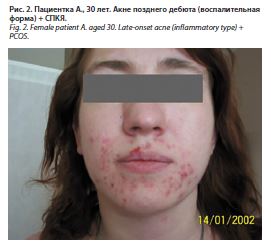 К яичниковой гиперандрогении функционального генеза относятся синдром поликистозных яичников (СПКЯ), который имеет место и в практике врача-дерматолога при междисциплинарном ведении пациенток с СПКЯ и акне (рис. 2). СПКЯ является одним из наиболее частых эндокринных расстройств у женщин репродуктивного возраста. В общей популяции женщин репродуктивного возраста распространенность синдрома составляет от 8 до 21%. Часто СПКЯ сопряжен с андрогензависмой дермопатией: акне, гирсутизмом, алопецией. Европейским обществом репродукции и эмбриологии человека (European Society of Human Reproduction and Embryology, ESHRE) и Американским обществом репродуктивной медицины (American Society for Reproductive Medicine, ASRM) [Роттердам, 2003] выделены основные критерии СПКЯ: олигоановуляция, гиперандрогения (клиническая или биохимическая), поликистозная морфология яичников по данным ультразвукового исследования. Согласно ASRM/ESHRE (2003 г.), International PCOS Network (2018 г.), наличие любых 2 из 3 основных критериев определяет наличие диагноза СПКЯ. Помимо андрогензависимой дермопатии СПКЯ часто сопряжен с ожирением, часто по мужскому типу (44%), а также ассоциирован с повышенным риском метаболических нарушений, в том числе инсулинорезистентности и сахарного диабета 2-го типа. Кроме того, существует связь между СПКЯ и риском развития карциномы эндометрия, сердечно-сосудистых и церебральных катастроф, депрессии и психосексуальных расстройств, апноэ сна [8, 30–32].
К яичниковой гиперандрогении функционального генеза относятся синдром поликистозных яичников (СПКЯ), который имеет место и в практике врача-дерматолога при междисциплинарном ведении пациенток с СПКЯ и акне (рис. 2). СПКЯ является одним из наиболее частых эндокринных расстройств у женщин репродуктивного возраста. В общей популяции женщин репродуктивного возраста распространенность синдрома составляет от 8 до 21%. Часто СПКЯ сопряжен с андрогензависмой дермопатией: акне, гирсутизмом, алопецией. Европейским обществом репродукции и эмбриологии человека (European Society of Human Reproduction and Embryology, ESHRE) и Американским обществом репродуктивной медицины (American Society for Reproductive Medicine, ASRM) [Роттердам, 2003] выделены основные критерии СПКЯ: олигоановуляция, гиперандрогения (клиническая или биохимическая), поликистозная морфология яичников по данным ультразвукового исследования. Согласно ASRM/ESHRE (2003 г.), International PCOS Network (2018 г.), наличие любых 2 из 3 основных критериев определяет наличие диагноза СПКЯ. Помимо андрогензависимой дермопатии СПКЯ часто сопряжен с ожирением, часто по мужскому типу (44%), а также ассоциирован с повышенным риском метаболических нарушений, в том числе инсулинорезистентности и сахарного диабета 2-го типа. Кроме того, существует связь между СПКЯ и риском развития карциномы эндометрия, сердечно-сосудистых и церебральных катастроф, депрессии и психосексуальных расстройств, апноэ сна [8, 30–32].
При акне велика роль психоэмоциональных нарушений, связанных с проблемой «дефекта внешности». Локализация дерматоза на открытых участках кожи (лице, верхней половине груди и спине) приносит пациентам, особенно девушкам и женщинам, глубокие психические страдания, негативно влияя на качество жизни. Установлена высокая значимость психосоциальных последствий акне, сопоставимых с таковыми при сахарном диабете, раке, эпилепсии. У больных с акне даже легкой или средней степени тяжести симптомы депрессии были более выраженными, чем у пациентов с очаговой алопецией, атопическим дерматитом и псориазом. Для пациентов с акне характерны избыточные личные реакции на стрессорный фактор: 90% больных, страдающих акне, испытывают эстетический дискомфорт; 62% – имеют трудности в общении с другими людьми, 45% – отмечают сложности на работе или учебе. Среди лиц с акне отмечается большое количество (64%)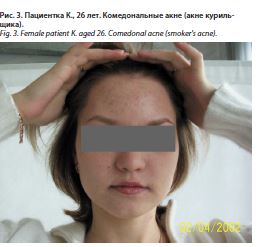 неработающих, социально нереализованных женщин с неустроенной личной жизнью. Распространенность тревоги среди больных с акне достигает 68,3%, а распространенность депрессии колеблется от 8,8 до 51,9% случаев, чаще возникая у женщин и в ряде случаев коррелируя со степенью тяжести акне. Частота суицидальных мыслей у подростков с акне наблюдается 2,6 раза чаще по сравнению с их сверстниками без патологии кожи [15, 33–36].
неработающих, социально нереализованных женщин с неустроенной личной жизнью. Распространенность тревоги среди больных с акне достигает 68,3%, а распространенность депрессии колеблется от 8,8 до 51,9% случаев, чаще возникая у женщин и в ряде случаев коррелируя со степенью тяжести акне. Частота суицидальных мыслей у подростков с акне наблюдается 2,6 раза чаще по сравнению с их сверстниками без патологии кожи [15, 33–36].
Патологический механизм стресса при акне реализуется следующими путями. При стрессе, как известно, происходит активная выработка кортикотропин-рилизинг-гормона (КРТГ) в гипоталамусе, затем КРТГ стимулирует выделение в кровь АКТГ, который, в свою очередь, передает сигнал о стрессе надпочечникам, в результате чего происходит повышенная секреция стероидных гормонов надпочечников, которые вызывают обострение акне. КРТГ может также действовать на сально-волосяной фолликул напрямую, вызывая обострение акне, так как себоциты сально-волосяного фолликула имеют рецепторы (CRHR-1, CRHR-2) к КРТГ и способны реагировать на его воздействие сразу после выделения гормона из гипоталамуса [19].
Кроме того, установлено, что в развитии стресса при акне большую роль играют нейропептиды – биологически активные вещества белковой природы, такие как субстанция Р. Было выявлено, что уровень субстанции Р в крови у пациентов с акне находится в прямой корреляции с уровнем переносимого стресса при отсутствии таковой связи у людей без данного заболевания. Субстанция Р синтезируется в центральной и периферической нервной системе, также ее выделяют моноциты, макрофаги, кератиноциты, меланоциты, фибробласты. Кожа людей со склонностью к акне характеризуется обилием нервных окончаний, увеличенным числом нервных волокон, способных секретировать субстанцию Р, а также большим числом тучных клеток. Рецепторы к субстанции Р имеются на тучных клетках, лимфоцитах, макрофагах, себоцитах, меланоцитах, клетках кровеносных сосудов и т.д. Активация рецепторов к субстанции Р, расположенных на себоцитах, вызывает повышенную пролиферацию и дифференцировку сальных желез, а также увеличивает синтез липидов в себоцитах, стимулируя продукцию кожного сала; способствует дегрануляции тучных клеток, результатом чего становится выход гистамина и других медиаторов воспаления: ИЛ-1, ИЛ-2, ФНО-α, VEGF (Vascular Endothelial Growth Factor) в межклеточное пространство, приводя к развитию воспалительной реакции, таким образом вызывая обострение или утяжеление акне [37–39].
В последние десятилетия в большом количестве зарубежных исследований подтверждена связь между развитием и/или обострением акне и так называемой западной диетой, которая отличается высоким потреблением коровьего молока и молочных продуктов, калорийной пищи с высоким гликемическим индексом, сладостей, большого количества жиров и мяса. Западная диета также характеризуется нарушением соотношения между омега-6- и омега-3-жирными кислотами в пользу омега-6-жирных кислот (в пищевом рационе их содержится в 10 раз больше).
Патологический механизм реализуется по следующим путям:
1. Молоко (молочные продукты) увеличивают уровни инсулина и инсулиноподобного фактора роста 1 (ИФР-1), в результате чего происходит активация двух киназ, вызывающих фосфорилирование FOXO1, ко-супрессора АР. FoxO1 покидает ядро андрогензависимых клеток, открывая АР. ДГТ связывается с АР. Этот процесс называется «сигнальный путь инсулина/ИФР-1» [19].
2. ИФР-1 стимулирует липогенез в сальных железах, индуцируя факторы подсемейства SREBP (sterol regulatory element-bilding protein), что приводит к увеличению выработки кожного сала и повышает содержание мононенасыщенных жирных кислот и создает благоприятные условия для колонизации С. acnes [40].
3. Активация комплекса mTORC1 – mammalian target of rapamycin (нутриент-чувствительная киназа механической мишени рапамицина), ключевого регулятора клеточного роста. mTORC1 активируется углеводами, аминокислотами. При активации mTORC1 анаболические процессы преобладают над катаболическими, в результате происходят усиление клеточной пролиферации, активация себоцитов, воспаление и обострение акне [41].
4. Продукты с высоким гликемическим индексом приводят к повышению уровня инсулина, который подавляет синтез ПССГ, соответственно, увеличивая концентрацию свободного тестостерона в сыворотке крови, что приводит к образованию акне [8, 19].
Кроме того, в молочной промышленности 75–90% сырья для производства молока берется от беременных коров, оно содержит в 3,4 раза больше андростендиона, в 1,3 раза больше тестостерона, в 1,2 раза больше ДГЭА, чем молоко небеременных коров [42].
В многоцентровых исследованиях по типу случай-контроль, проведенных как в Европе, так и в Азии на
3 тыс. пациентов мужского и женского пола с различными формами акне (предподростковые акне, аcne vulgaris, acne tarda) в возрасте от 10 до 30 лет с различной степенью тяжести заболевания (в большинстве случаев папуло-пустулезные акне средней/среднетяжелой степени тяжести), было выявлено, что употребление молока более трех раз в неделю или более двух стаканов в день увеличивает риск развития тяжелых и среднетяжелых форм дерматоза. В малазийском исследовании, опубликованном в 2012 г., были получены сходные данные. Всего исследовали 88 пациентов обоего пола (основная/контрольная группа) в возрасте от 18 до 30 лет. У 81,8% пациентов основной группы семейный анамнез по акне был отягощен. При анализе результатов обнаружено, что употребление молока и мороженого более одного раза в неделю увеличивает проявления акне в
4 раза по сравнению с теми, кто употребляет эти продукты менее одного раза в неделю [43–46].
В ряде исследований отмечено, что частое употребление шоколада связано с высоким риском появления акне и утяжеления клинической картины заболевания, а сочетанное употребление молочных продуктов и шоколада оказывает комбинированное отрицательное влияние на дерматоз и способствует ухудшению клинической картины заболевания [47, 48].
В турецком исследовании, проведенном в 2019 г. на 106 добровольцах (53 пациента с акне и 53 человека без акне), были проанализированы рацион и возможность продуктов питания провоцировать/утяжелять акне. Средний возраст испытуемых составил около 25 лет.
В отношении массы тела, роста, индекса массы тела между группами не было отмечено статистически значимой разницы. При статистическом сравнении групп оказалось, что употребление сыра было выше в группе пациентов с акне, при этом в отношении употребления молока, йогурта, мороженого, кефира такой закономерности зафиксировано не было. Также установлено, что тяжесть акне усиливается по мере увеличения потребления углеводов в группе пациентов с акне; но не увеличивается по мере увеличения потребления жиров [49].
В ряде зарубежных исследований отмечено, что высокое потребление рыбы снижает риск развития акне, однако потребление морепродуктов может быть связано с повышенным риском развития дерматоза. Употребление достаточного количества фруктов и овощей также может нивелировать проявления заболевания. Эти наблюдаемые защитные эффекты могут быть связаны с жирными кислотами омега-3, содержащимися в рыбе, и высоким содержанием клетчатки во фруктах и овощах, которые могут снижать уровень ИФР-1, тем самым уменьшая проявления акне [50, 51].
Курение вызывает особый тип акне – atypical post-adolescent acne (APAA), которое характеризуется преобладанием открытых и закрытых комедонов (невоспалительное акне) с локализацией в области лица (рис. 3). Известно, что курильщики подвержены более высокому риску невоспалительных акне по сравнению с некурящими, а количество выкуренных сигарет не влияет на тяжесть высыпаний. Никотин провоцирует продукцию кожного сала через активацию нейрональных (никотиновых) ацетилхолиновых рецепторов, что приводит к усилению кератинизации в фолликулярном инфундибулуме, снижает концентрацию витамина Е – природного антиоксиданта, транспортируемого себумом на поверхность кожи, который способен нивелировать негативное воздействие никотина. Это и является причиной усугубления течения угревой сыпи и развития ретенционных поражений. Кроме того, сигаретный дым содержит большое количество арахидоновой кислоты и полициклических ароматических углеводородов, которые могут стимулировать зависимый от фосфолипазы А2 путь воспаления и усугублять течение акне [52, 53].
Таким образом, несомненна роль экзогенных и эндогенных триггеров, оказывающих влияние на проявление, течение и степень тяжести акне. Потенциальными факторами, которые с наибольшей вероятностью могут повлиять на течение заболевания, являются генетический фактор, гормонально-эндокринные нарушения, стресс, а также образ жизни пациента. При курации пациентов с акне необходимо учитывать внутренние и внешние факторы, негативно воздействующие на дерматоз, и по возможности нивелировать их.
Конфликт интересов. Автор заявляет об отсутствии конфликта интересов.
Conflict of interests. The author declares that there is not conflict of interests.
Каиль-Горячкина Мария Владимировна – канд. мед. наук, врач-дерматолог Клиники кожных и венерических болезней,
ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: ultra1147@mail.ru; ORCID: 0000-0002-1023-4279
Mariya V. Kail-Goryachkina – Сand. Sci. (Med.), Sechenov First Moscow State Medical University (Sechenov University).
E-mail: ultra1147@mail.ru; ORCID: 0000-0002-1023-4279
Поступила в редакцию / Received: 20.03.2023
Поступила после рецензирования / Revised: 22.03.2023
Принята к публикации / Accepted: 23.03.2023
Клинический разбор в общей медицине №2 2023
Роль эндогенных и экзогенных триггеров в развитии акне
Аннотация
В статье представлены современные данные о влиянии эндогенных и экзогенных триггеров на клиническую картину акне. Подробно разобраны основные из них. Отмечена значимость генетического фактора в развитии дерматоза. Показана роль гормонального фактора – гиперандрогении в патогенезе заболевания. Приведены данные о негативном воздействии стресса на течение акне. Выявлена связь между пищевым рационом и обострением/появлением акне. Отмечена негативная роль курения в провоцировании невоспалительных акне.
Ключевые слова: акне, воспаление, западная диета, гиперандрогения, синдром поликистозных яичников, стресс.
Для цитирования: Каиль-Горячкина М.В. Роль эндогенных и экзогенных триггеров в развитии акне. Клинический разбор в общей медицине. 2023; 4 (2): 90–96. DOI: 10.47407/kr2023.4.2.00210
В статье представлены современные данные о влиянии эндогенных и экзогенных триггеров на клиническую картину акне. Подробно разобраны основные из них. Отмечена значимость генетического фактора в развитии дерматоза. Показана роль гормонального фактора – гиперандрогении в патогенезе заболевания. Приведены данные о негативном воздействии стресса на течение акне. Выявлена связь между пищевым рационом и обострением/появлением акне. Отмечена негативная роль курения в провоцировании невоспалительных акне.
Ключевые слова: акне, воспаление, западная диета, гиперандрогения, синдром поликистозных яичников, стресс.
Для цитирования: Каиль-Горячкина М.В. Роль эндогенных и экзогенных триггеров в развитии акне. Клинический разбор в общей медицине. 2023; 4 (2): 90–96. DOI: 10.47407/kr2023.4.2.00210
Abstract
The paper presents current data on the impact of endogenous and exogenous triggers on the clinical manifestations of acne. The major triggers are discussed in detail. The importance of genetic factors for the development of dermatosis is reported. The role of hormonal factor, hyperandrogenism, in the pathogenesis of the disease is displayed. The data on the adverse effects of stress on the course of acne are provided. The association of the diet with the acne exacerbation/onset is exposed. The negative role of smoking in triggering the non-inflammatory type acne is reported.
Keywords: acne, inflammation, Western diet, hyperandrogenism, polycystic ovary syndrome, stress.
For citation: Kail-Goryachkina M.V. The role of endogenous and exogenous triggers in the development of acne. Clinical review for general practice. 2023; 4 (2): 90–96. DOI: 10.47407/kr2023.4.2.00210
Акне является одним из наиболее распространенных хронических воспалительных заболеваний кожи, которое проявляется поражением сально-волосяного аппарата; дерматоз характеризуется появлением открытых и закрытых комедонов, папул, пустул и узлов. Развивающийся в результате осложнения акне – симптомокомплекс постакне представляет собой в большинстве случаев вторичную гиперпигментацию (36%), неравномерную текстуру кожи (30%), рубцы (26%), а также эритематозные пятна (6%), атеромы и милиумы (2%) [1, 2].
По данным глобального исследования бремени болезней (Global Burden of Disease Study), проведенного в 2010 г., акне страдают примерно 650 млн человек во всем мире. По показателю распространенности воспалительных заболеваний кожи дерматоз занимает
8-е место. В предпубертатном или пубертатном периоде в той или иной степени с проблемой акне сталкиваются 90% девушек и 100% юношей. У девушек угревые высыпания появляются раньше, чем у юношей, нередко незадолго до начала первой менструации. У юношей акне дебютирует позже, но носит более тяжелый и распространенный характер. В 12-летнем возрасте акне наблюдается у 37,1% девочек и 15,4% мальчиков, в 16 лет – уже у 38,8 и 53,3% соответственно, а вот для acne tarda (поздних угрей) характерно существенное преобладание женщин 82,1% против 17,9%, недаром за рубежом существует устоявшаяся аббревиатура – adult female acne, характеризующая данную группу пациентов [2–7].
Патогенез акне состоит из патологического взаимодействия между несколькими процессами, такими как воспаление, фолликулярная гиперкератинизация (приводящая к «закупорке» устья сально-волосяного фолликула), гиперпродукция секрета сальных желез, микробная колонизация Сutibacterium acnes (филотипа IA1 риботипов RT4 и RT5) с формированием биопленок, а также гормонального фактора (абсолютной или периферической гиперандрогении) [8–10].
В настоящее время доказано, что важнейшем звеном в патогенезе акне является воспаление. В 28% случаев воспаление образуется de novo, минуя стадию комедонов. Данный постулат подтверждается в работе A. Jeremy и соавт., которые продемонстрировали, что воспалительный процесс в той или иной мере наблюдался при всех проявлениях и стадиях болезни: от непораженной кожи в доклинической стадии (характеризующейся образованием микрокомедонов) до симптомокомплекса постакне. Основополагающая роль при этом отводится провоспалительному цитокину – интерлейкину (ИЛ)-1, экспрессия которого значительно увеличивается в пораженной коже независимо от наличия или отсутствия С. аcnes. Немаловажную роль в развитии воспалительного процесса играют и другие провоспалительные цитокины, такие как фактор некроза опухоли (ФНО), ИЛ-6, ИЛ-8, ИЛ-10 и ИЛ-12, а также интегрины, матриксные металлопротеиназы (matrix metalloproteinases, MMP), макрофаги, дендритные клетки и CD4+ T-клетки [11, 12].
В норме кератиноциты и себоциты постоянно экспрессируют провоспалительные цитокины, однако под действием различных триггерных факторов происходят их индукция и гиперсекреция. C. acnes является комменсальным липофильным факультативным анаэробным микроорганизмом кожи человека и служит одним из основных триггеров для развития воспалительной реакции посредством активации врожденного или приобретенного иммунного ответа [12, 13].
Необходимо также помнить, что способность C. acnes к образованию биопленок как сложных полимикробных ассоциаций способствует формированию устойчивости к защитным механизмам хозяина и лекарственным препаратам, а также может служить резервуаром для иных патогенных микроорганизмов, таких как Staphylococcus aureus, что может существенно утяжелить течение акне. Адгезионное свойство матрицы биопленки C. acnes приводит к усилению сцепления корнеоцитов в области воронки сально-волосяного фолликула за счет выделения «биологического клея», которым является гликокаликсный полимер. Данное свойство микроорганизма играет важную роль в образовании сально-роговой пробки и развитии комедоногенеза [12, 14].
Среди клинических проявлений акне чаще (в 70–80% случаев) встречается среднетяжелая – папуло-пустулезная форма. Легкая комедональная форма и самое тяжелое проявление дерматоза – конглобатные угри – отмечаются значительно реже (у 15–20% больных) [15, 16].
При обзоре различных эпидемиологических исследований за период последних 20 лет (1999–2021 гг.) выявлено, что на распространенность, риск возникновения и утяжеления течения акне оказывают влияние различные эндогенные и экзогенные триггеры. К эндогенным триггерам относят генетический фактор и гиперандрогению. К экзогенным – стресс, рацион питания и диетические предпочтения, курение, прием ряда лекарственных препаратов (анаболические стероиды, противотуберкулезные препараты, глюкокортикоиды и др.), травматизацию кожи (наиболее часто вследствие выдавливания пациентами акне-элементов), нерациональный уход за кожей, в том числе и вследствие неадекватного назначения косметологических процедур, экологический фактор (негативное воздействие внешней среды: загрязнение кожи маслами, керосином, бензином, пылью производственного происхождения, УФ-облучение) [8, 15, 17–20].
Несмотря на то что конкретные генетические маркеры акне пока не найдены, а обнаружены лишь полиморфизмы генов, регулирующих врожденную иммунную систему кожи и метаболизм стероидных гормонов, акне считается генетически обусловленным наследственным мультифакториальным заболеванием с высоким семейным накоплением. Наследственная предрасположенность выявляется примерно в 59,9–81,1% случаев. Установлено, что развитие тяжелых, длительно текущих, торпидных форм акне наиболее вероятно, если в анамнезе заболевание имеется у обоих родителей [21, 22].
В настоящие время проводятся различные генетические исследования, посвященные акне. Наиболее перспективным является поиск генов-кандидатов, т.е. генов, связанных с акне. Очевидно, что в развитии акне принимает участие множество генов. Одни из них ответственны за развитие гиперандрогении, или патологической реакции на нормальное содержание андрогенов. Получены данные, что к развитию тяжелых форм акне приводит мутация гена CYP17-34C, кодирующего цитохром P450c17a, который является одним из ключевых ферментов в биосинтезе андрогенов. Доказано, что полиморфизм гена ангиотензинпревращающего фермента – АСЕ (делеция/включение) связан с тяжелыми формами акне с отягощенным семейным анамнезом. Было обнаружено, что короткая длина повторения гена CAG и специфические галотипы андрогенного рецептора связаны с риском развития акне и, следовательно, могут рассматриваться как достоверный маркер предрасположенности к данному поражению кожи. Полиморфизм гена инсулиноподобного фактора роста –
IGF-1, состоящего из вариабельных повторов цитозина и аденозина, влияет на эксперссию IGF-1 и на тяжесть течения дерматоза у взрослых женщин, а полиморфизм гена CYT17-34T в форме гомозиготы был обнаружен у пациентов мужского пола с тяжелыми формами акне [15, 23–26].
Исследования по распределению и степени тяжести акне среди различных популяций указывают на этнические особенности заболевания. Акне наиболее подвержены европейцы (29%) и афроамериканцы (25%), дерматоз развивается реже (10%) и протекает в более легкой форме у японцев и китайцев. Интересными наблюдениями, подтверждающими важную роль внешних и внутренних факторов в возникновении, развитии и утяжелении течения акне, являются популяции, полностью свободные от этого дерматоза. К ним относятся эскимосы, жители острова Окинавы, индейцы, у которых частота встречаемости акне равна нулю. Данный феномен можно объяснить сочетанием различных внешних и внутренних факторов, таких как окружающая среда, пищевой рацион (натуральные продукты питания, полученные в результате охоты и собирательства), на который не оказала влияния западная диета, генетическая разнородность данных популяций и западного общества [15, 27, 28].
Кроме того, андрогены (около 50%) образуются за счет периферического метаболизма стероидов, в том числе и в коже, недаром немецкий ученый Шмитц назвал кожу самой большой эндокринной железой в организме. Периферическое взаимопревращение яичниковых и надпочечниковых гормонов ведет к трансформации низкоактивных андрогенов в высокоактивные. Так, андростендион превращается в тестостерон, который, в свою очередь, в коже под действием фермента 5-α-редуктазы метаболизируется в свой более сильный метаболит дегидротестостерон (ДГТ), оказывающий основное андрогенное действие в тканях-мишенях [16, 29].
Гиперандрогения служит одной из визитных карточек эндокринного неблагополучия женской репродуктивной сферы и клинически проявляется несколькими группами признаков, отражающих андрогенизацию организма: андрогензависимая дермопатия, дефеминизация, маскулинизация и вирилизация наружных половых органов [8, 16, 29].
По происхождению гиперандрогения может быть:
• истинной (абсолютной) – из овариального или надпочечникового источника, связана с повышением уровня андрогенов в крови. Истинная гиперандрогения может иметь функциональный или опухолевый генез;
• транспортной (снижение секреции половых стероидов, связывающих глобулины – ПССГ).
• периферической (рецепторной), связанной с повышенной чувствительностью андрогеновых рецепторов – АР к андрогенам при нормальном их количестве;
• метаболической, связанной с повышенной активностью фермента 5-α-редуктазы;
• ятрогенной, связанной с приемом лекарственных средств;
• гиперандрогения при системных заболеваниях и заболеваниях гипоталамо-гипофизарной системы (сахарный диабет 2-го типа и ожирение, болезнь Иценго–Кушинга, акромегалия и др.)
При акне велика роль психоэмоциональных нарушений, связанных с проблемой «дефекта внешности». Локализация дерматоза на открытых участках кожи (лице, верхней половине груди и спине) приносит пациентам, особенно девушкам и женщинам, глубокие психические страдания, негативно влияя на качество жизни. Установлена высокая значимость психосоциальных последствий акне, сопоставимых с таковыми при сахарном диабете, раке, эпилепсии. У больных с акне даже легкой или средней степени тяжести симптомы депрессии были более выраженными, чем у пациентов с очаговой алопецией, атопическим дерматитом и псориазом. Для пациентов с акне характерны избыточные личные реакции на стрессорный фактор: 90% больных, страдающих акне, испытывают эстетический дискомфорт; 62% – имеют трудности в общении с другими людьми, 45% – отмечают сложности на работе или учебе. Среди лиц с акне отмечается большое количество (64%)
Патологический механизм стресса при акне реализуется следующими путями. При стрессе, как известно, происходит активная выработка кортикотропин-рилизинг-гормона (КРТГ) в гипоталамусе, затем КРТГ стимулирует выделение в кровь АКТГ, который, в свою очередь, передает сигнал о стрессе надпочечникам, в результате чего происходит повышенная секреция стероидных гормонов надпочечников, которые вызывают обострение акне. КРТГ может также действовать на сально-волосяной фолликул напрямую, вызывая обострение акне, так как себоциты сально-волосяного фолликула имеют рецепторы (CRHR-1, CRHR-2) к КРТГ и способны реагировать на его воздействие сразу после выделения гормона из гипоталамуса [19].
Кроме того, установлено, что в развитии стресса при акне большую роль играют нейропептиды – биологически активные вещества белковой природы, такие как субстанция Р. Было выявлено, что уровень субстанции Р в крови у пациентов с акне находится в прямой корреляции с уровнем переносимого стресса при отсутствии таковой связи у людей без данного заболевания. Субстанция Р синтезируется в центральной и периферической нервной системе, также ее выделяют моноциты, макрофаги, кератиноциты, меланоциты, фибробласты. Кожа людей со склонностью к акне характеризуется обилием нервных окончаний, увеличенным числом нервных волокон, способных секретировать субстанцию Р, а также большим числом тучных клеток. Рецепторы к субстанции Р имеются на тучных клетках, лимфоцитах, макрофагах, себоцитах, меланоцитах, клетках кровеносных сосудов и т.д. Активация рецепторов к субстанции Р, расположенных на себоцитах, вызывает повышенную пролиферацию и дифференцировку сальных желез, а также увеличивает синтез липидов в себоцитах, стимулируя продукцию кожного сала; способствует дегрануляции тучных клеток, результатом чего становится выход гистамина и других медиаторов воспаления: ИЛ-1, ИЛ-2, ФНО-α, VEGF (Vascular Endothelial Growth Factor) в межклеточное пространство, приводя к развитию воспалительной реакции, таким образом вызывая обострение или утяжеление акне [37–39].
В последние десятилетия в большом количестве зарубежных исследований подтверждена связь между развитием и/или обострением акне и так называемой западной диетой, которая отличается высоким потреблением коровьего молока и молочных продуктов, калорийной пищи с высоким гликемическим индексом, сладостей, большого количества жиров и мяса. Западная диета также характеризуется нарушением соотношения между омега-6- и омега-3-жирными кислотами в пользу омега-6-жирных кислот (в пищевом рационе их содержится в 10 раз больше).
Патологический механизм реализуется по следующим путям:
1. Молоко (молочные продукты) увеличивают уровни инсулина и инсулиноподобного фактора роста 1 (ИФР-1), в результате чего происходит активация двух киназ, вызывающих фосфорилирование FOXO1, ко-супрессора АР. FoxO1 покидает ядро андрогензависимых клеток, открывая АР. ДГТ связывается с АР. Этот процесс называется «сигнальный путь инсулина/ИФР-1» [19].
2. ИФР-1 стимулирует липогенез в сальных железах, индуцируя факторы подсемейства SREBP (sterol regulatory element-bilding protein), что приводит к увеличению выработки кожного сала и повышает содержание мононенасыщенных жирных кислот и создает благоприятные условия для колонизации С. acnes [40].
3. Активация комплекса mTORC1 – mammalian target of rapamycin (нутриент-чувствительная киназа механической мишени рапамицина), ключевого регулятора клеточного роста. mTORC1 активируется углеводами, аминокислотами. При активации mTORC1 анаболические процессы преобладают над катаболическими, в результате происходят усиление клеточной пролиферации, активация себоцитов, воспаление и обострение акне [41].
4. Продукты с высоким гликемическим индексом приводят к повышению уровня инсулина, который подавляет синтез ПССГ, соответственно, увеличивая концентрацию свободного тестостерона в сыворотке крови, что приводит к образованию акне [8, 19].
Кроме того, в молочной промышленности 75–90% сырья для производства молока берется от беременных коров, оно содержит в 3,4 раза больше андростендиона, в 1,3 раза больше тестостерона, в 1,2 раза больше ДГЭА, чем молоко небеременных коров [42].
В многоцентровых исследованиях по типу случай-контроль, проведенных как в Европе, так и в Азии на
3 тыс. пациентов мужского и женского пола с различными формами акне (предподростковые акне, аcne vulgaris, acne tarda) в возрасте от 10 до 30 лет с различной степенью тяжести заболевания (в большинстве случаев папуло-пустулезные акне средней/среднетяжелой степени тяжести), было выявлено, что употребление молока более трех раз в неделю или более двух стаканов в день увеличивает риск развития тяжелых и среднетяжелых форм дерматоза. В малазийском исследовании, опубликованном в 2012 г., были получены сходные данные. Всего исследовали 88 пациентов обоего пола (основная/контрольная группа) в возрасте от 18 до 30 лет. У 81,8% пациентов основной группы семейный анамнез по акне был отягощен. При анализе результатов обнаружено, что употребление молока и мороженого более одного раза в неделю увеличивает проявления акне в
4 раза по сравнению с теми, кто употребляет эти продукты менее одного раза в неделю [43–46].
В ряде исследований отмечено, что частое употребление шоколада связано с высоким риском появления акне и утяжеления клинической картины заболевания, а сочетанное употребление молочных продуктов и шоколада оказывает комбинированное отрицательное влияние на дерматоз и способствует ухудшению клинической картины заболевания [47, 48].
В турецком исследовании, проведенном в 2019 г. на 106 добровольцах (53 пациента с акне и 53 человека без акне), были проанализированы рацион и возможность продуктов питания провоцировать/утяжелять акне. Средний возраст испытуемых составил около 25 лет.
В отношении массы тела, роста, индекса массы тела между группами не было отмечено статистически значимой разницы. При статистическом сравнении групп оказалось, что употребление сыра было выше в группе пациентов с акне, при этом в отношении употребления молока, йогурта, мороженого, кефира такой закономерности зафиксировано не было. Также установлено, что тяжесть акне усиливается по мере увеличения потребления углеводов в группе пациентов с акне; но не увеличивается по мере увеличения потребления жиров [49].
В ряде зарубежных исследований отмечено, что высокое потребление рыбы снижает риск развития акне, однако потребление морепродуктов может быть связано с повышенным риском развития дерматоза. Употребление достаточного количества фруктов и овощей также может нивелировать проявления заболевания. Эти наблюдаемые защитные эффекты могут быть связаны с жирными кислотами омега-3, содержащимися в рыбе, и высоким содержанием клетчатки во фруктах и овощах, которые могут снижать уровень ИФР-1, тем самым уменьшая проявления акне [50, 51].
Курение вызывает особый тип акне – atypical post-adolescent acne (APAA), которое характеризуется преобладанием открытых и закрытых комедонов (невоспалительное акне) с локализацией в области лица (рис. 3). Известно, что курильщики подвержены более высокому риску невоспалительных акне по сравнению с некурящими, а количество выкуренных сигарет не влияет на тяжесть высыпаний. Никотин провоцирует продукцию кожного сала через активацию нейрональных (никотиновых) ацетилхолиновых рецепторов, что приводит к усилению кератинизации в фолликулярном инфундибулуме, снижает концентрацию витамина Е – природного антиоксиданта, транспортируемого себумом на поверхность кожи, который способен нивелировать негативное воздействие никотина. Это и является причиной усугубления течения угревой сыпи и развития ретенционных поражений. Кроме того, сигаретный дым содержит большое количество арахидоновой кислоты и полициклических ароматических углеводородов, которые могут стимулировать зависимый от фосфолипазы А2 путь воспаления и усугублять течение акне [52, 53].
Таким образом, несомненна роль экзогенных и эндогенных триггеров, оказывающих влияние на проявление, течение и степень тяжести акне. Потенциальными факторами, которые с наибольшей вероятностью могут повлиять на течение заболевания, являются генетический фактор, гормонально-эндокринные нарушения, стресс, а также образ жизни пациента. При курации пациентов с акне необходимо учитывать внутренние и внешние факторы, негативно воздействующие на дерматоз, и по возможности нивелировать их.
Конфликт интересов. Автор заявляет об отсутствии конфликта интересов.
Conflict of interests. The author declares that there is not conflict of interests.
Каиль-Горячкина Мария Владимировна – канд. мед. наук, врач-дерматолог Клиники кожных и венерических болезней,
ФГАОУ ВО «Первый МГМУ им. И.М. Сеченова» (Сеченовский Университет). E-mail: ultra1147@mail.ru; ORCID: 0000-0002-1023-4279
Mariya V. Kail-Goryachkina – Сand. Sci. (Med.), Sechenov First Moscow State Medical University (Sechenov University).
E-mail: ultra1147@mail.ru; ORCID: 0000-0002-1023-4279
Поступила в редакцию / Received: 20.03.2023
Поступила после рецензирования / Revised: 22.03.2023
Принята к публикации / Accepted: 23.03.2023
15 мая 2023
Количество просмотров: 1293
